Spinal Cord Overview - The Neural Highway
- Cylindrical CNS component in vertebral canal.
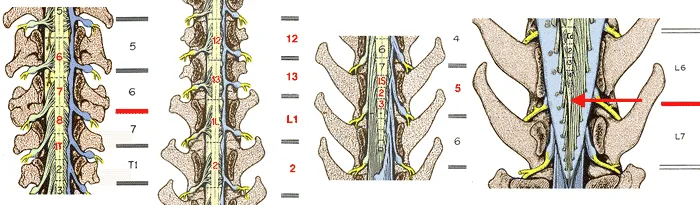
- Extends from foramen magnum (medulla) to L1 vertebra (adults).
⭐ Spinal cord terminates at L1/L2 in adults, but at L3 in neonates.
- Segments: 31 pairs of spinal nerves:
- 8 Cervical (C1-C8)
- 12 Thoracic (T1-T12)
- 5 Lumbar (L1-L5)
- 5 Sacral (S1-S5)
- 1 Coccygeal (Co1)
- Enlargements:
- Cervical (C5-T1): For upper limbs (brachial plexus).
- Lumbosacral (L1-S3): For lower limbs (lumbosacral plexus).
- Conus Medullaris: Tapered inferior end.
- Cauda Equina: "Horse's tail"; lumbosacral nerve roots.
- Filum Terminale: Pial extension from conus; anchors to coccyx.
Meningeal Layers - Protective Wrappings
- Three protective membranes (meninges) cover the spinal cord.
- 📌 Mnemonic: PAD (Pia, Arachnoid, Dura - from innermost to outermost).
- Pia Mater: Innermost, vascular, adheres to cord. Forms filum terminale internum, denticulate ligaments.
- Arachnoid Mater: Middle, avascular, web-like. Lines dural sac.
- Dura Mater: Outermost, tough. Forms dural sac (thecal sac), ends at S2 vertebra. Epidural space external.
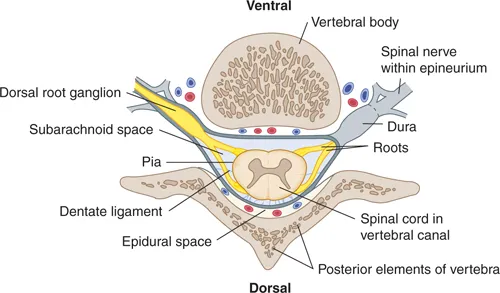
⭐ The subarachnoid space (between arachnoid and pia mater) contains Cerebrospinal Fluid (CSF) & major spinal vessels.
Internal Cord Structure - Cord's Inner Circuitry

- Grey Matter (Central H-shape): Neuron cell bodies, dendrites, unmyelinated axons, glial cells.
- Posterior Horn: Sensory nuclei (e.g., substantia gelatinosa for pain/temp). Receives sensory input.
- Anterior Horn: Motor nuclei (alpha for muscle contraction, gamma for muscle spindle tone). Sends motor output.
- Lateral Horn (Thoracolumbar T1-L2): Sympathetic preganglionic neurons.
- Intermediate Zone: Interneurons, Clarke's nucleus (proprioception to cerebellum).
- White Matter (Outer Region): Myelinated axons in funiculi (columns) containing tracts.
- Dorsal Funiculus: Ascending sensory (Fasciculus Gracilis - lower body, Cuneatus - upper body).
- Lateral Funiculus: Mixed (Lateral Corticospinal - motor; Lateral Spinothalamic - pain/temp).
- Anterior Funiculus: Mixed (Anterior Corticospinal - motor; Anterior Spinothalamic - crude touch/pressure).
⭐ The lateral corticospinal tract, controlling voluntary skilled limb movements, decussates (crosses over) at the pyramids of the medulla oblongata.
Spinal Cord Vasculature - Lifeline Arteries & Veins

- Arterial Supply:
- 1 Anterior Spinal Artery (ASA): From vertebral arteries; supplies anterior 2/3 of cord.
- 2 Posterior Spinal Arteries (PSAs): From vertebral arteries or PICA; supply posterior 1/3.
- Segmental/Radicular Arteries: Reinforce ASA & PSAs; includes Artery of Adamkiewicz.
- Venous Drainage:
- Anterior and Posterior Spinal Veins.
- Drain into Internal Vertebral Venous Plexus (Batson's plexus).
⭐ The Artery of Adamkiewicz (Great Anterior Radicular Artery of Luhska), typically arising from T9-T12 on the left, is crucial for thoracolumbar cord irrigation; its occlusion can lead to Anterior Spinal Artery Syndrome below the lesion level.
Clinical Correlations - Cord in Crisis
- Lumbar Puncture (LP):
- Site: Adults L3-L4 / L4-L5 interspace; Children L4-L5 / L5-S1.
⭐ Structures pierced (superficial to deep): Skin → Subcutaneous tissue → Supraspinous lig. → Interspinous lig. → Ligamentum flavum → Epidural space → Dura mater → Arachnoid mater → Subarachnoid space.
- Disc Herniation: Common sites: L4-L5, L5-S1. Can cause radiculopathy or cord compression.
- Spinal Cord Compression: Urgent MRI & management. Causes: trauma, tumor, disc, abscess.
- Cauda Equina Syndrome: ⚠️ Surgical emergency! Presents with saddle anesthesia, bowel/bladder dysfunction, leg weakness.
 oka
oka
High‑Yield Points - ⚡ Biggest Takeaways
- Spinal cord terminates at L1-L2 (adults), L3 (newborns).
- Dural sac and subarachnoid space (with CSF) end at S2 vertebra.
- Lumbar puncture safely performed at L3-L4 or L4-L5 interspace.
- Epidural space contains fat and the internal vertebral venous plexus.
- Pia mater forms denticulate ligaments (anchoring cord laterally) and filum terminale (anchoring inferiorly).
- Anterior Spinal Artery supplies anterior 2/3 of the spinal cord; two Posterior Spinal Arteries supply posterior 1/3.
- Artery of Adamkiewicz (major anterior segmental medullary artery) typically at T9-L2, crucial for lower cord perfusion.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

