Peritoneum & Cavity: Basics - Silky Smooth Sac
- Peritoneum: Largest serous membrane; single layer of mesothelial cells.
- Parietal layer: Lines abdominal wall; somatic innervation.
- Visceral layer: Covers organs; autonomic innervation.
- Peritoneal Cavity: Potential space between layers.
- Contains thin film of serous fluid (~50-100 mL).
- Functions: Lubrication, organ suspension, immune defense.

⭐ Parietal peritoneum (somatic innervation) is sensitive to localized pain, temperature, touch, and pressure; visceral peritoneum (autonomic innervation) is sensitive to stretch and chemical irritation, causing poorly localized pain.
Peritoneum & Cavity: Spaces - Cavity Capers
- Peritoneal Cavity: Potential space. Divided into:
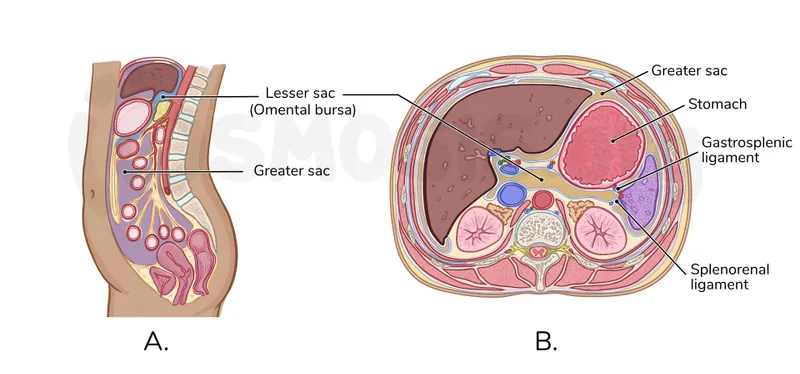
- Greater Sac: Main, larger portion.
- Lesser Sac (Omental Bursa): Smaller, posterior to stomach & lesser omentum.
- Communication: Via Epiploic Foramen (of Winslow).
- Boundaries:
- Ant: Hepatoduodenal ligament (free edge of lesser omentum containing portal triad).
- Post: IVC.
- Sup: Caudate lobe (liver).
- Inf: 1st part of duodenum.
- Boundaries:
⭐ The epiploic foramen (of Winslow) is the sole natural communication between the greater sac and the lesser sac (omental bursa); its boundaries are crucial for understanding potential sites of internal herniation.
 oka
oka
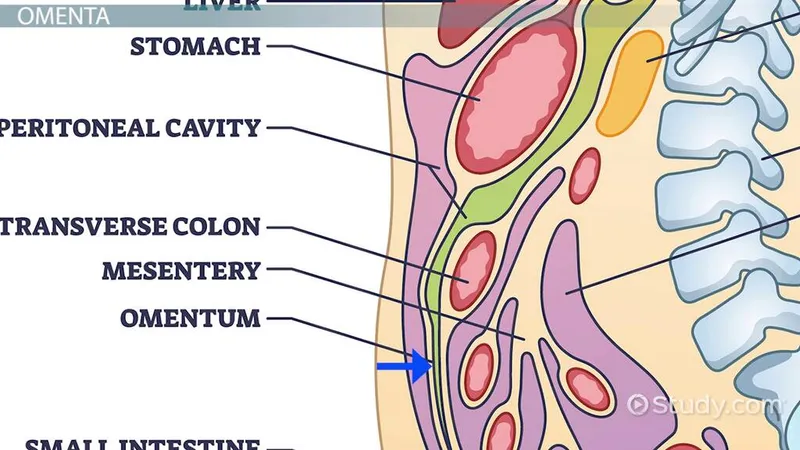
Peritoneum & Cavity: Folds - Abdominal Draperies
- Omenta: Double-layered folds.
- Greater Omentum: "Abdominal policeman"; from greater stomach curvature.
- Includes: Gastrocolic, gastrosplenic, gastrophrenic ligaments.
- Lesser Omentum: From lesser stomach curvature/duodenum to liver.
- Hepatogastric, hepatoduodenal (portal triad) ligaments.
- Greater Omentum: "Abdominal policeman"; from greater stomach curvature.
- Mesenteries: Suspend intestines from posterior wall; neurovascular pathway.
- Types: The Mesentery, transverse/sigmoid mesocolon, mesoappendix.
- Ligaments: Connect organs or to abdominal wall.
- Liver: Falciform, coronary, triangular.
- Spleen: Splenorenal, gastrosplenic.
⭐ The hepatoduodenal ligament, free edge of lesser omentum, contains portal triad: portal vein (posterior), hepatic artery proper (anterior/left), bile duct (anterior/right). 📌 Mnemonic: DAVE (Duct, Artery, Vein, anterior to posterior, simplified).
Peritoneum & Cavity: Compartments & Gutters - Fluid Flow Routes
- Peritoneal Compartmentalization:
- Supracolic Compartment: Superior to transverse mesocolon (liver, stomach, spleen).
- Infracolic Compartment: Inferior to transverse mesocolon (intestines, colon).
- Divided by small bowel mesentery into right/left infracolic spaces.
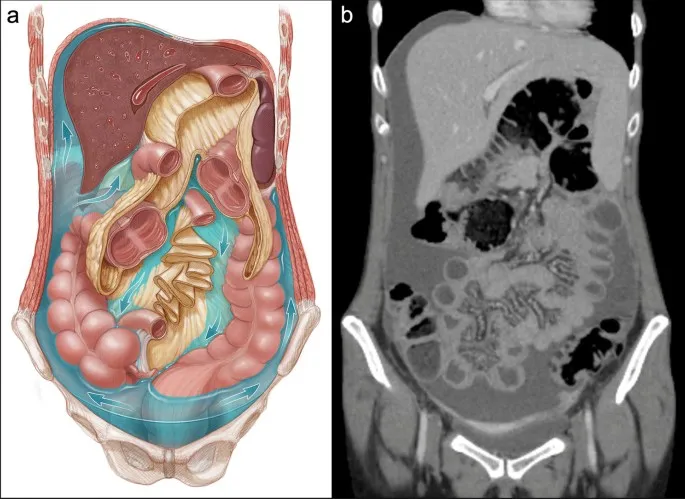
- Key Gutters & Fluid Pathways:
- Right Paracolic Gutter:
- Primary vertical channel for fluid movement.
- Connects RLQ (e.g., appendicitis) to Morison's pouch, subphrenic space, and pelvis.
- Left Paracolic Gutter:
- Lateral to descending colon.
- Superior flow limited by phrenicocolic ligament.
- Pelvic Cavity: Most dependent part; common site for fluid collection.
- Right Paracolic Gutter:
⭐ The right paracolic gutter provides a direct pathway for the spread of infected fluid from the supracolic compartment (e.g., perforated appendix) to the hepatorenal pouch (Morison's pouch) and the pelvis.
Peritoneum & Cavity: Clinical Correlations - Peritoneal Problems
- Peritonitis: Inflammation (infection/chemical). Signs: pain, guarding.
- Ascites: Fluid in cavity (cirrhosis, cancer). Paracentesis.
- Dependent collection: Morison's pouch (supine), Pelvic pouches (upright).
- Adhesions: Post-op/inflammation → obstruction.
- Peritoneal Dialysis: Therapeutic.
⭐ The rectouterine pouch (Pouch of Douglas) is the most dependent part of the peritoneal cavity in an upright female, making it a common site for fluid accumulation (e.g., pus, blood) and accessible for culdocentesis.
High‑Yield Points - ⚡ Biggest Takeaways
- Peritoneum: Serous membrane; parietal lines cavity, visceral covers organs.
- Peritoneal cavity: Potential space with serous fluid; divided into greater and lesser sacs.
- Lesser sac (omental bursa): Posterior to stomach; connects to greater sac via foramen of Winslow.
- Intraperitoneal organs (e.g., stomach) suspended by mesentery/omentum.
- Retroperitoneal organs (e.g., kidneys) lie posterior to peritoneum.
- Key sites for fluid collection: Morison's pouch, Pouch of Douglas. Ascites and peritonitis are crucial clinicals_
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

