Neuro-Ophthalmology — Flashcards

On this page
_____ is a condition of abnormal myelination of the nerve fibers of the retina, where myelination continues beyond lamina cribrosa and spreads into the retina beyond the optic disc.
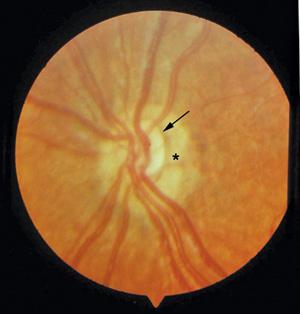
_____ sign is seen in optic nerve hypoplasia
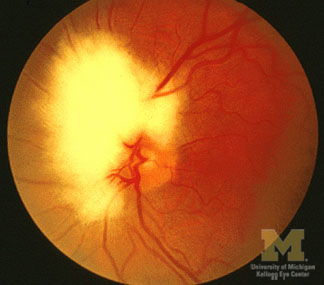
Hyperemic optic disc with telangiectatic (non-leaky on FFA) capillaries is suggestive of _____.
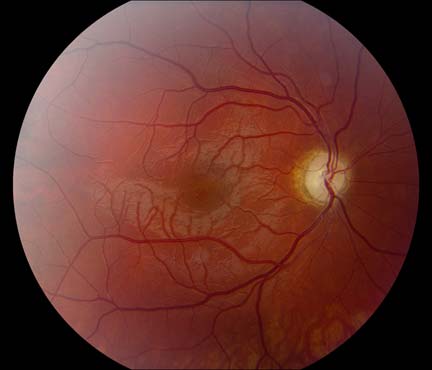
_____ pupil is tested with the 'swinging flashlight' test
Papilledema leads to blockage of _____, axonal swelling and collection of extracellular fluid
Early stage of papilledema is characterised by obscuration of disc margins (_____ margin first), and absence of spontaneous venous pulsations of the disc
Established papilledema may lead to a _____ or dome-shaped disc, and appearance of a macular fan
Lesions to the optic nerve result in _____-ocular and ipsi-lateral deficits in vision
Optic neuritis is of 3 types-_____-Neuroretinitis-Retrobulbar neuritis
Weakness of _____, mainly seen when the eye is adducted, is seen with superior oblique palsy
Study by Chapter
Anatomy of Visual Pathways
Flashcards
Pupillary Disorders
Flashcards
Optic Neuritis
Flashcards
Ischemic Optic Neuropathies
Flashcards
Other Optic Neuropathies
Flashcards
Papilledema
Flashcards
Cranial Nerve Palsies
Flashcards
Nystagmus
Flashcards
Visual Field Defects
Flashcards
Neuro-ophthalmic Manifestations of Intracranial Lesions
Flashcards
Functional Visual Disorders
Flashcards
Migraine and the Eye
Flashcards
About Neuro-Ophthalmology Flashcards for NEET-PG
These Neuro-Ophthalmology flashcards are designed for NEET-PG Ophthalmology preparation, using active recall to help you retain high-yield concepts, clinical correlations, and commonly tested facts. Each card prompts you to retrieve information from memory rather than passively reviewing notes, which research shows leads to significantly better exam performance.
The 86 cards in this deck cover the most important topics in Neuro-Ophthalmology, including key mechanisms, diagnostic criteria, treatment protocols, and clinical pearls that frequently appear in NEET-PG examinations. Cards are organised by chapter so you can focus on specific areas or work through the entire topic systematically.
For personalised spaced repetition scheduling that adapts to your performance, unlimited flashcards, and detailed progress analytics, download the Oncourse app.
Frequently Asked Questions
Are Neuro-Ophthalmology flashcards free on Oncourse?
How do flashcards help with NEET-PG preparation?
How many Neuro-Ophthalmology flashcards are available?
Can I study Neuro-Ophthalmology flashcards by chapter?
What topics do these Ophthalmology flashcards cover?
Want unlimited flashcards?
Get full access to all flashcards, spaced repetition, and progress tracking.
Start For Free