Back
How to Study Neurology for USMLE Step 2 CK 2026: High-Yield Topics, Clinical Vignette Strategy and Exam Checklist
Master USMLE Step 2 CK neurology with high-yield topics, clinical vignette strategies, and a comprehensive exam checklist. Cover stroke, epilepsy, MS, headaches, and movement disorders efficiently.

How to Study Neurology for USMLE Step 2 CK 2026: High-Yield Topics, Clinical Vignette Strategy and Exam Checklist
You probably opened this thinking neurology is the hardest Step 2 CK specialty to crack. Here's the thing: Step 2 CK neurology has 35-40 questions, representing 12% of your exam. That's roughly one question every 7 minutes dedicated to stroke presentations, seizure management, and movement disorders.
Most students treat neurology like a black box – memorizing symptoms without understanding the clinical decision trees that Step 2 CK actually tests. The exam doesnt care if you know every rare syndrome. It cares whether you can recognize a middle cerebral artery stroke in a 67-year-old diabetic, choose the right antiepileptic drug for a pregnant woman with focal seizures, or distinguish Parkinson disease from multiple system atrophy in a clinical vignette.
This guide breaks down exactly how USMLE Step 2 CK tests neurology, which topics yield the most questions, and a systematic approach to clinical vignettes that turns pattern recognition into points. By December 2026, you'll have a clear roadmap from high-yield concepts to exam-day execution.
USMLE Step 2 CK Neurology Blueprint Breakdown
Step 2 CK neurology questions cluster around 7 core domains that mirror real clinical encounters:
High-Yield Topic Distribution
Stroke and Cerebrovascular Disease: 25% of neurology questions
Seizures and Epilepsy: 20% of neurology questions
Headache Disorders: 15% of neurology questions
Multiple Sclerosis and Demyelinating Disease: 10% of neurology questions
Movement Disorders: 10% of neurology questions
Peripheral Neuropathy: 10% of neurology questions
Dementia and Cognitive Disorders: 10% of neurology questions
These percentages matter because they guide your study time allocation. Spending 3 weeks on rare metabolic disorders while skipping stroke management is exactly backwards for Step 2 CK success.
The Oncourse high-yield topic cards organize neurology into bite-sized concepts mapped to Step 2 CK blueprints, linking each topic directly to practice questions so you move from concept to clinical vignette in one tap.
Stroke and Cerebrovascular Disease: 9-10 Questions
Step 2 CK stroke questions test clinical decision-making, not anatomy memorization. You need to recognize stroke syndromes, choose appropriate acute management, and understand secondary prevention.
Acute Ischemic Stroke Management
The exam loves testing tPA eligibility and contraindications. Key decision points:
Time windows: IV tPA within 4.5 hours, mechanical thrombectomy within 24 hours for large vessel occlusion
Absolute contraindications: Active bleeding, recent surgery, hemorrhagic stroke history
Blood pressure management: Hold antihypertensives unless >220/120 mmHg
Stroke Syndromes to Recognize
Middle Cerebral Artery: Contralateral hemiparesis, hemisensory loss, aphasia (dominant hemisphere)
Anterior Cerebral Artery: Leg weakness greater than arm, personality changes
Posterior Cerebral Artery: Homonymous hemianopia, memory deficits
Basilar Artery: Cranial nerve palsies, ataxia, altered consciousness
TIA vs Stroke Differentiation
Clinical vignettes often present transient symptoms. Key differentiators:
TIA: Symptoms resolve completely within 24 hours, no acute infarct on imaging
Stroke: Persistent deficits or positive imaging regardless of symptom duration
Practice stroke recognition with focused neurology questions that mirror Step 2 CK clinical presentations. The adaptive algorithms identify whether you struggle more with acute management decisions or syndrome recognition.
Seizures and Epilepsy: 7-8 Questions
Step 2 CK seizure questions focus on seizure classification, antiepileptic drug (AED) selection, and status epilepticus management rather than EEG interpretation.
Seizure Classification
Focal seizures: Previously "partial seizures" - can be aware or with impaired awareness
Generalized seizures: Tonic-clonic, absence, myoclonic, atonic
Unknown onset: When seizure beginning isnt witnessed
First-Line AED Selection
The exam tests drug selection based on seizure type and patient factors:
Seizure Type | First-Line AEDs | Avoid |
|---|---|---|
Focal seizures | Levetiracetam, lamotrigine | Carbamazepine in pregnancy |
Generalized tonic-clonic | Valproate, lamotrigine | Valproate in pregnancy |
Absence seizures | Ethosuximide, valproate | Carbamazepine, phenytoin |
Status Epilepticus Protocol
Step 2 CK tests the sequential approach:
1. 0-5 minutes: Lorazepam 0.1 mg/kg IV 2. 5-20 minutes: Phenytoin 20 mg/kg IV or fosphenytoin 3. 20-40 minutes: Repeat phenytoin or alternative (levetiracetam, valproate) 4. 40+ minutes: Anesthetic agents (propofol, midazolam) Epilepsy practice questions help solidify these protocols through repetitive clinical scenarios. Look for questions that test AED selection in pregnancy – a frequent Step 2 CK favorite.
Headache Disorders: 5-6 Questions
Step 2 CK headache questions emphasize red flags, medication overuse patterns, and treatment approaches rather than detailed diagnostic criteria.
Primary Headache Recognition
Migraine: Unilateral, throbbing, with nausea/photophobia, 4-72 hours
Tension-type: Bilateral, pressing/tightening, no nausea, 30 minutes to 7 days
Cluster: Unilateral, severe, with autonomic symptoms, 15-180 minutes
Red Flags Requiring Immediate Evaluation
Sudden onset "thunderclap" headache
Headache with fever and neck stiffness
New headache in patient >50 years
Headache with focal neurologic signs
Progressive headache with papilledema
Migraine Management
Acute treatment: Triptans (avoid in cardiovascular disease), NSAIDs, antiemetics Prophylaxis (≥4 headache days/month): Propranolol, topiramate, valproate
The exam often tests medication overuse headache – suspect when headaches worsen despite increased acute medication use.
Multiple Sclerosis and Demyelinating Disease: 4 Questions
Step 2 CK MS questions focus on diagnostic criteria, disease-modifying therapy selection, and acute relapse management.
MS Diagnostic Criteria (2017 McDonald Criteria)
Requires dissemination in time and space plus exclusion of alternative diagnoses:
Clinical relapses separated by ≥30 days involving different CNS regions
MRI findings: Gadolinium-enhancing and non-enhancing lesions
CSF analysis: Oligoclonal bands (supportive but not required)
Disease-Modifying Therapy Selection
First-line: Interferon-β, glatiramer acetate, teriflunomide
High-efficacy: Natalizumab, ocrelizumab, alemtuzumab (for active disease)
Pregnancy considerations: Glatiramer acetate and certain interferons are safer options
Acute Relapse Management
High-dose IV methylprednisolone (1g daily × 3-5 days) for functionally significant relapses. Plasma exchange reserved for severe relapses unresponsive to steroids.
Oncourse's movement disorders flashcards include MS-related mobility issues alongside Parkinson disease and essential tremor, helping you differentiate these commonly confused conditions.
Movement Disorders: 4 Questions
Step 2 CK movement disorder questions cluster around Parkinson disease diagnosis, treatment complications, and essential tremor differentiation.
Parkinson Disease Clinical Features
Motor symptoms (asymmetric onset):
Bradykinesia (required for diagnosis)
Rest tremor (4-6 Hz)
Rigidity
Postural instability
Non-motor symptoms: Depression, constipation, sleep disorders, cognitive changes
Parkinson Disease Treatment
Initial therapy: Levodopa/carbidopa (best symptomatic control) or dopamine agonists (younger patients)
Motor complications: Wearing-off phenomenon, dyskinesias
Advanced therapies: Deep brain stimulation for medication-refractory symptoms
Essential Tremor vs Parkinson Tremor
Feature | Essential Tremor | Parkinson Tremor |
|---|---|---|
Frequency | 4-12 Hz | 4-6 Hz |
Position | Action/postural | Rest |
Distribution | Bilateral, symmetric | Unilateral onset |
Treatment | Propranolol, primidone | Dopaminergic agents |
Peripheral Neuropathy: 4 Questions
Step 2 CK peripheral neuropathy questions focus on diabetic neuropathy, carpal tunnel syndrome, and Guillain-Barré syndrome recognition.
Diabetic Peripheral Neuropathy
Pattern: Distal, symmetric, sensorimotor
Symptoms: Burning pain, numbness in stocking-glove distribution
Management: Glycemic control, gabapentin/pregabalin for neuropathic pain
Carpal Tunnel Syndrome
Clinical features: Thenar weakness, positive Tinel/Phalen signs
Electrodiagnostic findings: Prolonged median nerve distal latency
Treatment: Wrist splints, corticosteroid injection, surgery for severe cases
Guillain-Barré Syndrome
Presentation: Ascending weakness following infection
CSF findings: Elevated protein (>45 mg/dL), normal cell count
Treatment: Plasma exchange or IVIG (equally effective)
Dementia and Cognitive Disorders: 4 Questions
Step 2 CK dementia questions emphasize Alzheimer disease diagnosis, vascular dementia patterns, and behavioral management.
Alzheimer Disease Features
Cognitive pattern: Memory loss, executive dysfunction, language problems
Imaging: Medial temporal lobe atrophy on MRI
Treatment: Cholinesterase inhibitors (donepezil, rivastigmine, galantamine)
Vascular Dementia Recognition
Pattern: Stepwise cognitive decline following strokes
Risk factors: Hypertension, diabetes, smoking
Prevention: Vascular risk factor management
Performance analytics in Oncourse's dashboard break down your performance by specialty and subtopic, showing whether you need more work on dementia drug mechanisms or clinical differentiation between dementia types.
Clinical Vignette Strategy for USMLE Step 2 CK Neurology
Step 2 CK neurology vignettes follow predictable patterns. Master these approaches to convert clinical scenarios into correct answers systematically.
The 4-Step Vignette Analysis Method
Step 1: Extract Key Clinical Data
Patient demographics (age, sex)
Chief complaint and timeline
Past medical history
Physical examination findings
Diagnostic test results
Step 2: Identify the Clinical Syndrome
Ask: "What neurological syndrome does this constellation of findings suggest?"
Stroke syndrome (vascular territory)
Seizure type (focal vs generalized)
Movement disorder (tremor characteristics)
Headache pattern (primary vs secondary)
Step 3: Apply Step 2 CK Clinical Reasoning
Step 2 CK tests management decisions, not just diagnosis:
What's the next best step in management?
Which treatment is most appropriate?
What diagnostic test would confirm the diagnosis?
How should complications be managed?
Step 4: Eliminate Wrong Answers Using Clinical Logic
Rule out options that contradict the clinical presentation
Eliminate treatments inappropriate for the specific patient
Choose the most conservative appropriate option when multiple could work
Pattern Recognition Shortcuts
Stroke Vignettes:
Look for vascular risk factors + acute onset + focal deficits
Time since onset determines treatment options
Contraindications eliminate tPA choices
Seizure Vignettes:
Focus on seizure description and patient factors (pregnancy, age)
AED selection depends on seizure type and contraindications
Status epilepticus = time-based protocol
MS Vignettes:
Young adult + relapsing symptoms + MRI lesions
Optic neuritis or internuclear ophthalmoplegia are classic presentations
Uhthoff phenomenon (symptoms worsen with heat)
USMLE Step 2 CK Neurology Exam Checklist
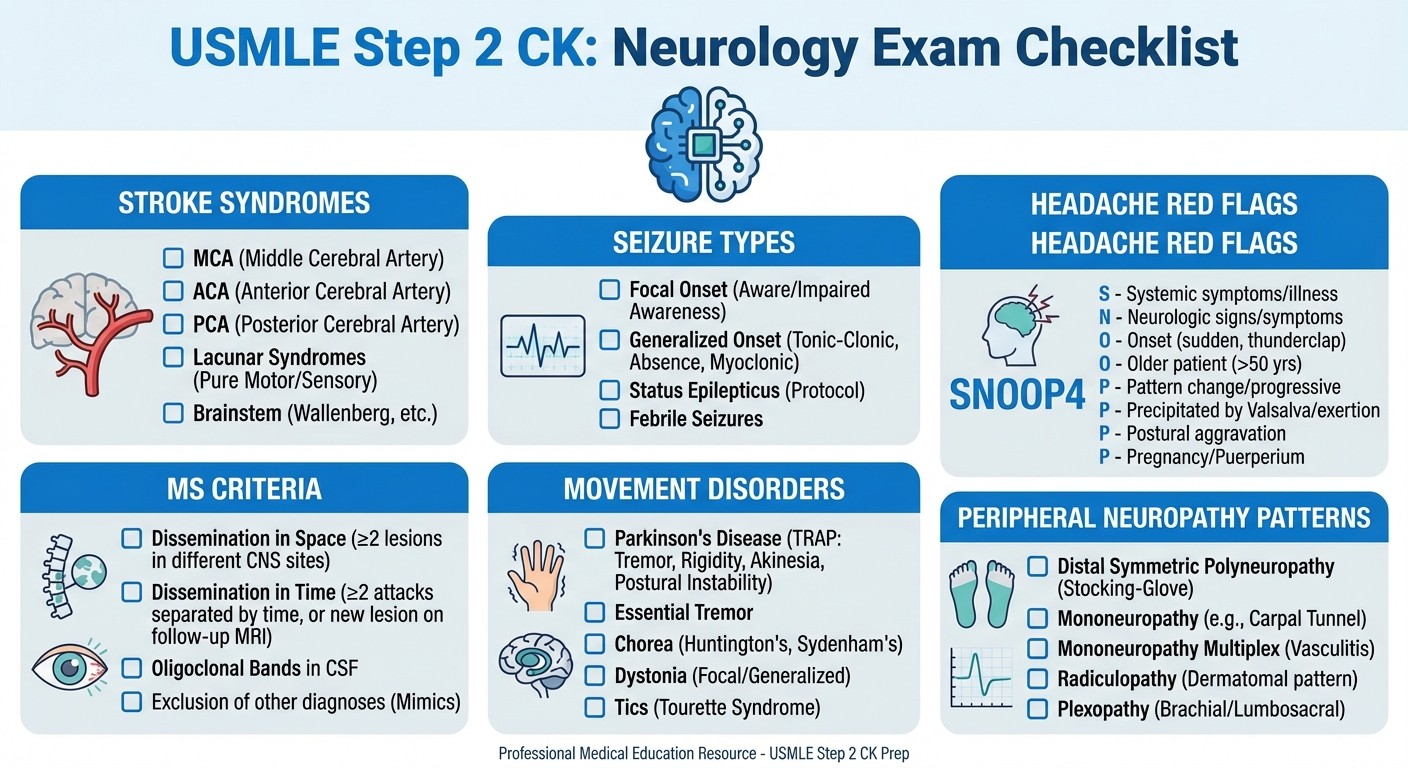
Use this checklist in your final weeks before Step 2 CK to ensure you've covered all high-yield neurology concepts:
Stroke and Cerebrovascular Disease ✓
[ ] tPA eligibility criteria and contraindications
[ ] Mechanical thrombectomy time window (24 hours)
[ ] Blood pressure management in acute stroke
[ ] MCA, ACA, PCA syndrome recognition
[ ] TIA vs stroke differentiation
[ ] Secondary stroke prevention (antiplatelet therapy, statins)
Seizures and Epilepsy ✓
[ ] Focal vs generalized seizure classification
[ ] First-line AED selection by seizure type
[ ] AED considerations in pregnancy
[ ] Status epilepticus management protocol
[ ] Breakthrough seizure management
[ ] Drug-resistant epilepsy criteria
Headache Disorders ✓
[ ] Migraine vs tension-type vs cluster headache features
[ ] Headache red flags requiring urgent evaluation
[ ] Migraine acute treatment options
[ ] Migraine prophylaxis indications and drugs
[ ] Medication overuse headache recognition
[ ] Thunderclap headache differential diagnosis
Multiple Sclerosis ✓
[ ] 2017 McDonald diagnostic criteria
[ ] Relapsing-remitting vs progressive MS patterns
[ ] Disease-modifying therapy selection
[ ] Acute relapse management with steroids
[ ] Pregnancy considerations in MS
[ ] Uhthoff phenomenon and heat sensitivity
Movement Disorders ✓
[ ] Parkinson disease motor and non-motor features
[ ] Levodopa vs dopamine agonist selection
[ ] Motor complications (wearing-off, dyskinesias)
[ ] Essential tremor vs Parkinson tremor differentiation
[ ] Deep brain stimulation indications
[ ] Huntington disease genetic patterns
Peripheral Neuropathy ✓
[ ] Diabetic peripheral neuropathy management
[ ] Carpal tunnel syndrome clinical features and treatment
[ ] Guillain-Barré syndrome presentation and management
[ ] Neuropathic pain treatment options
[ ] Mononeuropathy vs polyneuropathy patterns
[ ] Electrodiagnostic study indications
Dementia and Cognitive Disorders ✓
[ ] Alzheimer disease diagnostic criteria
[ ] Cholinesterase inhibitor indications and side effects
[ ] Vascular dementia vs Alzheimer differentiation
[ ] Mild cognitive impairment recognition
[ ] Dementia behavioral management strategies
[ ] Capacity assessment principles
Study Timeline: 8 Weeks to Step 2 CK Neurology Mastery
Weeks 1-2: Foundation Building
Complete high-yield topic review for stroke, seizures, and headaches
Begin systematic neurology question practice focusing on pattern recognition
Create syndrome summary cards for quick review
Weeks 3-4: Clinical Application
Focus on MS, movement disorders, and peripheral neuropathy
Practice timed question blocks mixing neurology with other specialties
Review incorrect answers to identify knowledge gaps
Weeks 5-6: Weakness Targeting
The adaptive question algorithms automatically surface your weak neurology subtopics during this phase, helping you spend time efficiently on areas that need the most work rather than reviewing concepts you've already mastered.
Weeks 7-8: Integration and Review
Complete full-length practice tests including neurology questions
Use the exam checklist for systematic review
Focus on high-yield facts and clinical decision trees
Common Step 2 CK Neurology Mistakes to Avoid
Overthinking Straightforward Presentations
Step 2 CK neurology isnt about rare diseases. If a vignette describes classic stroke symptoms in a diabetic patient, the answer involves standard stroke management, not exotic vasculitis.
Ignoring Contraindications
Many students know tPA treats stroke but miss absolute contraindications. Always check for recent surgery, bleeding history, or time limitations.
Confusing Similar Conditions
Practice differentiating:
Essential tremor vs Parkinson tremor
Migraine vs tension headache
MS vs other demyelinating diseases
Alzheimer vs vascular dementia
Forgetting Drug Interactions and Pregnancy
Step 2 CK loves testing AED selection in pregnant women and drug interactions in elderly patients with multiple comorbidities.
Frequently Asked Questions
How many neurology questions are on USMLE Step 2 CK?
USMLE Step 2 CK contains 35-40 neurology questions out of 318 total questions, representing approximately 12% of the exam. These questions are distributed across stroke (25%), seizures (20%), headaches (15%), MS (10%), movement disorders (10%), peripheral neuropathy (10%), and dementia (10%).
What are the highest yield neurology topics for Step 2 CK?
Stroke and cerebrovascular disease yield the most questions (9-10), followed by seizures and epilepsy (7-8), and headache disorders (5-6). Focus your study time on these three areas first, ensuring you know tPA criteria, AED selection, and headache red flags.
How should I approach neurology clinical vignettes on Step 2 CK?
Use a systematic 4-step approach: extract key clinical data, identify the neurological syndrome, apply Step 2 CK clinical reasoning (focus on management, not just diagnosis), and eliminate wrong answers using clinical logic. Remember that Step 2 CK tests practical decision-making.
Which antiepileptic drugs are safe in pregnancy for Step 2 CK?
Lamotrigine is the safest AED in pregnancy. Avoid valproate (teratogenic), carbamazepine (neural tube defects), and phenytoin (fetal hydantoin syndrome). Levetiracetam is increasingly used but has less pregnancy data than lamotrigine.
What imaging findings suggest multiple sclerosis on Step 2 CK?
Look for T2 hyperintense lesions that are periventricular, juxtacortical, infratentorial, or in the spinal cord. Gadolinium-enhancing lesions indicate active inflammation. The 2017 McDonald criteria require dissemination in time and space.
How do I differentiate stroke types in Step 2 CK vignettes?
Focus on vascular territory patterns: MCA stroke causes contralateral hemiparesis with aphasia (if dominant hemisphere), ACA stroke causes leg weakness greater than arm with personality changes, and PCA stroke causes homonymous hemianopia with memory deficits.
Prepare smarter with Oncourse AI — adaptive MCQs, spaced repetition, and AI explanations built for USMLE Step 2 CK. Download free on Android and iOS.