Back
NEET PG Endocrine Pharmacology Glossary 2026: Insulin Types, Antidiabetics, Thyroid Drugs and Corticosteroids — High-Yield Drug Mechanisms, Side Effects and MCQ Mnemonics
Master NEET PG endocrine pharmacology with this comprehensive 2026 glossary covering insulin types, antidiabetics, thyroid drugs, and corticosteroids. Includes high-yield mechanisms, side effects, contraindications, and memory mnemonics for MCQ success.

NEET PG Endocrine Pharmacology Glossary 2026: Insulin Types, Antidiabetics, Thyroid Drugs and Corticosteroids — High-Yield Drug Mechanisms, Side Effects and MCQ Mnemonics
You're staring at another endocrine pharmacology MCQ, and your brain freezes. Was it metformin that causes lactic acidosis, or was that something else? Which insulin peaks at 2-4 hours again? And dont even get started on remembering whether carbimazole or methimazole is the first-line antithyroid drug.
NEET PG 2026 tests endocrine pharmacology heavily — about 8-12 questions per paper. These arent just recall questions anymore. The pattern has shifted to mechanism-based MCQs that test your understanding of drug actions, contraindications, and clinical scenarios. You need more than rote memorization.
This glossary breaks down the 47 highest-yield endocrine drugs into memorable chunks with mnemonics that actually stick. Each drug entry includes the mechanism, key side effects, contraindications, and the exact clinical scenarios NEET PG loves to test.
Insulin and Antidiabetic Drugs
Insulin Classifications and Mechanisms
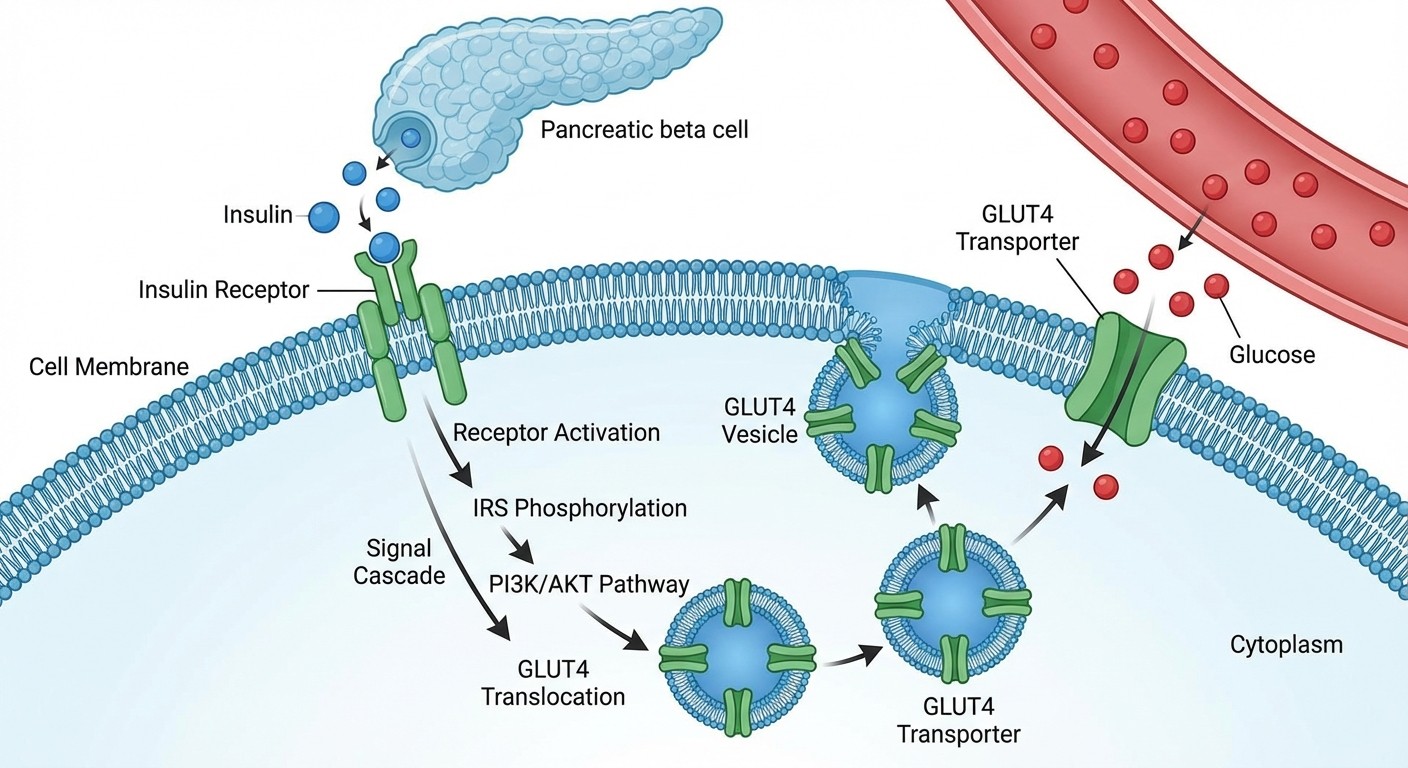
Insulin remains the cornerstone of diabetes management and a consistent NEET PG favorite. Understanding onset, peak, and duration patterns is crucial for clinical MCQs.
Rapid-Acting Insulins (Mnemonic: "LAG" - Lispro, Aspart, Glulisine)
Onset: 15 minutes
Peak: 1-3 hours
Duration: 3-5 hours
Clinical use: Pre-meal boluses, DKA management
NEET PG pearl: These are the only insulins safe for IV administration in DKA
Short-Acting Insulin (Regular)
Onset: 30 minutes
Peak: 2-4 hours
Duration: 6-8 hours
Mnemonic: "Regular = 2-4-6" (peak at 2-4, lasts 6-8)
Clinical note: Can be given IV or SC, traditional choice for sliding scale
Intermediate-Acting Insulin (NPH)
Onset: 1-2 hours
Peak: 4-8 hours
Duration: 12-18 hours
Mnemonic: "NPH = Night Protection for 12 Hours"
NEET PG trap: NPH causes dawn phenomenon if dose is too low
Long-Acting Insulins
Glargine: No peak, 24-hour duration ("Glargine = Gradual")
Detemir: 12-24 hours, weight-neutral
Degludec: Ultra-long 42-hour duration
Oral Antidiabetic Agents
Metformin (Biguanide)
Mechanism: Decreases hepatic glucose output, increases insulin sensitivity
Side effects: GI upset (30% patients), lactic acidosis (rare but fatal)
Contraindications: eGFR <30, contrast studies, severe illness
NEET PG favorite: First-line therapy, contraindicated in renal failure
Mnemonic: "Met-for-min = Meets minimum glucose by blocking liver output"
Our Indian Medical PG endocrine pharmacology lessons dive deeper into metformin's cellular mechanisms and the specific contraindication scenarios that appear in MCQs. Sulfonylureas (Mnemonic: "GLITTERING" - Glipizide, Glyburide, Gliclazide)
Mechanism: Block K-ATP channels → insulin release
Side effects: Hypoglycemia (major), weight gain, SIADH-like syndrome
Contraindications: Kidney/liver disease, elderly (glyburide)
NEET PG pearl: Cause prolonged hypoglycemia, especially glyburide in elderly
DPP-4 Inhibitors (Mnemonic: "SITAGLIPTIN = SIT A GLIP TIN")
Mechanism: Prevent GLP-1 degradation
Side effects: Upper respiratory infections, pancreatitis (rare)
Advantage: Weight neutral, low hypoglycemia risk
NEET PG note: Safe in elderly, renal dosing required
SGLT-2 Inhibitors (Mnemonic: "FLOZA drugs" - dapagliflozin, empagliflozin)
Mechanism: Block glucose reabsorption in kidney
Side effects: UTIs, genital infections, DKA (euglycemic)
Benefits: Weight loss, CV protection, HF benefits
NEET PG trap: Can cause euglycemic DKA even with normal glucose
Practice these drug mechanisms with targeted endocrine pharmacology MCQs that mirror the NEET PG question style.
Thyroid Pharmacology
Antithyroid Agents
Carbimazole/Methimazole
Mechanism: Inhibits thyroid peroxidase → blocks T3/T4 synthesis
Side effects: Agranulocytosis (0.3%), hepatotoxicity, skin rash
Monitoring: CBC every 2 weeks initially
NEET PG pearl: Carbimazole is prodrug of methimazole
Mnemonic: "Carb-imazole Carbs the thyroid (blocks synthesis)"
Propylthiouracil (PTU)
Mechanism: Blocks synthesis + peripheral conversion T4→T3
Preferred in: Pregnancy (1st trimester), thyroid storm
Side effects: Hepatotoxicity (black box warning), vasculitis
NEET PG scenario: Always choose PTU for pregnant hyperthyroid patients
Radioactive Iodine (I-131)
Mechanism: Beta radiation destroys thyroid follicles
Contraindications: Pregnancy, breastfeeding, ophthalmopathy
Side effects: Hypothyroidism (inevitable), worsening eye disease
NEET PG note: Treatment of choice for Graves disease in non-pregnant adults
Thyroid Hormone Replacement
Levothyroxine (T4)
Mechanism: Converted to active T3 in tissues
Dosing: 1.6 μg/kg ideal body weight
Monitoring: TSH every 6-8 weeks until stable
Drug interactions: Iron, calcium, PPI reduce absorption
Mnemonic: "Levo-T4 = Level out T4 slowly"
The thyroid drugs lessons include detailed drug interaction tables that frequently appear in NEET PG MCQs. Liothyronine (T3)
Use: Myxedema coma, T4→T3 conversion defects
Onset: Rapid (hours vs days for T4)
NEET PG scenario: Emergency hypothyroidism treatment
Corticosteroid Pharmacology
Glucocorticoid Classifications
Short-Acting (Mnemonic: "CHAMP" - Cortisone, Hydrocortisone, And Mother Pred)
Hydrocortisone: Duration 8-12 hours, high mineralocorticoid activity
Prednisolone: Duration 12-36 hours, intermediate anti-inflammatory
Clinical use: Replacement therapy (hydrocortisone), inflammation (prednisolone)
Intermediate-Acting
Methylprednisolone: 12-36 hours, minimal mineralocorticoid activity
Use: IV pulse therapy, organ transplant rejection
NEET PG pearl: Preferred for high-dose IV therapy
Long-Acting
Dexamethasone: 36-72 hours, potent anti-inflammatory
Betamethasone: 36-72 hours, crosses placenta
Clinical use: Cerebral edema, fetal lung maturation
Mnemonic: "Dexa = Deluxe steroid (most potent, longest)"
Corticosteroid Side Effects (High-Yield for MCQs)
Metabolic: Hyperglycemia, weight gain, buffalo hump, moon face Cardiovascular: Hypertension, fluid retention, hypokalemia Musculoskeletal: Osteoporosis, myopathy, growth retardation Immune: Increased infection risk, impaired wound healing Psychiatric: Mood changes, psychosis, insomnia Ocular: Cataracts, glaucoma Dermatologic: Skin atrophy, striae, delayed healing NEET PG mnemonic for steroid side effects: "CUSHINGOID"
Cataracts
Ulcers (peptic)
Skin atrophy
Hypertension
Infections
Necrosis (avascular)
Growth retardation
Osteoporosis
Insomnia/psychiatric
Diabetes
Our corticosteroid mechanisms lessons include the molecular pathways tested in mechanism-based MCQs.
Mineralocorticoids
Fludrocortisone
Mechanism: Aldosterone receptor agonist
Use: Addison disease, orthostatic hypotension
Side effects: Hypertension, hypokalemia, edema
Monitoring: Blood pressure, serum K+
NEET PG note: Only synthetic mineralocorticoid in clinical use
Advanced Antidiabetic Agents
GLP-1 Receptor Agonists
Exenatide, Liraglutide, Semaglutide
Mechanism: Mimic incretin hormone → glucose-dependent insulin release
Route: Subcutaneous injection
Side effects: Nausea (50%), pancreatitis, delayed gastric emptying
Benefits: Weight loss, CV protection
NEET PG pearl: Contraindicated in gastroparesis
Mnemonic: "GLP = Gut Loses Pounds (weight loss effect)"
Alpha-Glucosidase Inhibitors
Acarbose, Miglitol
Mechanism: Block intestinal α-glucosidases → delay carbohydrate absorption
Side effects: Flatulence, diarrhea, abdominal pain
Advantage: No hypoglycemia, no weight gain
NEET PG note: Treat hypoglycemia with glucose only (not sucrose)
High-Yield MCQ Scenarios and Mnemonics
Scenario 1: Diabetic Emergency Management
Question type: "A diabetic patient presents with DKA. Which insulin should be used?" Answer: Regular insulin IV (only regular and rapid-acting can be given IV) Mnemonic: "DKA = Don't Keep Asking, use Regular IV"
Scenario 2: Thyroid Storm Treatment
Question pattern: "Pregnant woman with thyroid storm needs urgent treatment" Answer: PTU (not carbimazole in pregnancy) Mnemonic: "PTU = Pregnancy Treatment Usually"
Scenario 3: Steroid Withdrawal
Clinical scenario: "Patient on chronic steroids needs surgery" Key point: Stress dose steroids needed to prevent crisis Mnemonic: "Stress = Steroid up the dose"
Scenario 4: Drug Interactions
Common MCQ: "Levothyroxine absorption is decreased by..." Answers: Iron, calcium, PPIs, coffee Mnemonic: "LICC up absorption" (Levo needs empty stomach - no Iron, Calcium, Coffee, Caffeine)
Test your understanding with comprehensive endocrine pharmacology flashcards that use spaced repetition to cement these high-yield facts.
Drug Dosing and Clinical Pearls
Insulin Dosing Calculations
Initial dose: 0.5-1 unit/kg/day
Basal:bolus ratio: 50:50
Correction factor: 1800 ÷ total daily dose
NEET PG formula: If total daily dose = 36 units, correction factor = 1800 ÷ 36 = 50 (1 unit drops glucose by 50 mg/dL)
Steroid Equivalency (Relative Potency)
Hydrocortisone: 1 (reference)
Prednisolone: 4x
Methylprednisolone: 5x
Dexamethasone: 25-30x
NEET PG calculation: 20mg prednisolone = 5mg hydrocortisone × 4 = 80mg hydrocortisone
Thyroid Hormone Conversion
T4 to T3 ratio: 4:1 by weight
TSH suppression: Goal <0.1 for thyroid cancer, 0.1-0.5 for benign disease
Replacement dose: 1.6 μg/kg lean body weight
Contraindications and Drug Safety
Metformin Contraindications (NEET PG High-Yield)
eGFR <30 mL/min/1.73m²
Contrast procedures (hold 48 hours)
Severe illness (shock, sepsis, MI)
Alcohol abuse
Mnemonic: "Met CRASHES" - Contrast, Renal failure, Alcohol, Shock, Heart failure, Elderly sick
Steroid Contraindications
Systemic fungal infections
Live vaccines (while on steroids)
Psychotic disorders (relative)
Peptic ulcer disease (relative)
Thyroid Drug Monitoring
Carbimazole: CBC (agranulocytosis), LFTs (hepatotoxicity)
PTU: LFTs mandatory (black box warning for hepatotoxicity)
Levothyroxine: TSH every 6-8 weeks, cardiac symptoms in elderly
Frequently Asked Questions
Which insulin can be given IV in DKA?
Only regular insulin and rapid-acting insulins (lispro, aspart, glulisine) can be administered intravenously. NPH and long-acting insulins are never given IV.
What's the first-line antithyroid drug in pregnancy?
PTU is preferred in the first trimester due to lower teratogenicity risk. Carbimazole can be used in second and third trimesters.
How long before surgery should metformin be stopped?
Hold metformin 48 hours before any contrast procedure or major surgery. Resume after confirming normal renal function.
Which steroid has the longest duration of action?
Dexamethasone has the longest half-life (36-72 hours) and is most potent. Its used for cerebral edema and fetal lung maturation.
Can SGLT-2 inhibitors cause DKA?
Yes, SGLT-2 inhibitors can cause euglycemic DKA (normal glucose levels but ketosis). This is a unique and dangerous side effect.
What's the mechanism of sulfonylurea-induced hypoglycemia?
Sulfonylureas block K-ATP channels on pancreatic beta cells, causing sustained insulin release regardless of glucose levels. This leads to prolonged hypoglycemia, especially in elderly patients.
Prepare smarter with Oncourse AI — adaptive MCQs, spaced repetition, and AI explanations built for NEET PG. Download free on Android and iOS.