Insulin Types & Action - Sweet Regulator
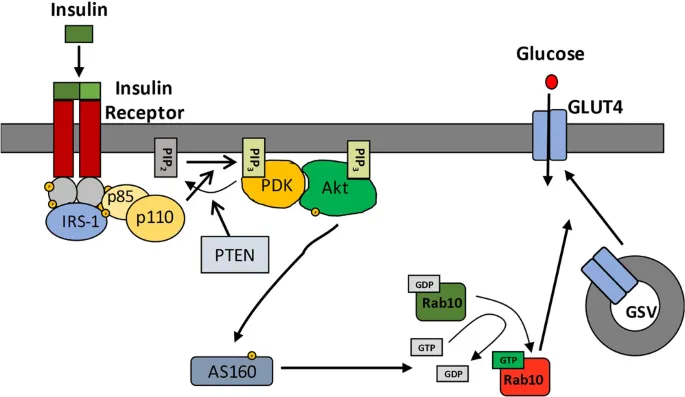
- Mechanism: Binds tyrosine kinase receptor → GLUT4 translocation (muscle, fat) → ↑ glucose uptake.
- Effects: ↑ Glycogenesis, ↑ protein synthesis, ↑ lipogenesis; ↓ Gluconeogenesis, ↓ glycogenolysis.
| Type | Examples | Onset (min) | Peak (hr) | Duration (hr) | Note |
|---|---|---|---|---|---|
| Rapid | Lispro, Aspart, Glulisine (📌 LAG) | 5-15 | 1-2 | 3-5 | Meal-time |
| Short (R) | Regular | 30-60 | 2-4 | 6-8 | IV use (DKA) |
| Intermediate | NPH | 60-120 | 4-8 | 10-18 | Basal |
| Long | Glargine, Detemir | 60-120 | Flat | ~24 | Basal, less hypo |
| Ultra-Long | Degludec, Glargine U300 | 30-90 | Flat | >24 | Stable basal |
Insulin Therapy & Risks - Prickly Points
- Risks:
- Hypoglycemia (<70 mg/dL): Common. Adrenergic/neuroglycopenic signs. Rule of 15.
- Lipodystrophy: Rotate injection sites.
- Weight gain, edema.
- Pearls:
- Somogyi (rebound) vs. Dawn (GH surge): Check 3 AM glucose.
- Injection: SC. Rotate sites (abdomen, thigh, arm, buttock).
- Storage: Unopened refrigerated; open vial room temp ≤28 days.
⭐ Severe hypoglycemia (<40 mg/dL): IV Dextrose or Glucagon.

Secretagogues & Metformin - Oral Workhorses
- Secretagogues: ↑Insulin secretion.
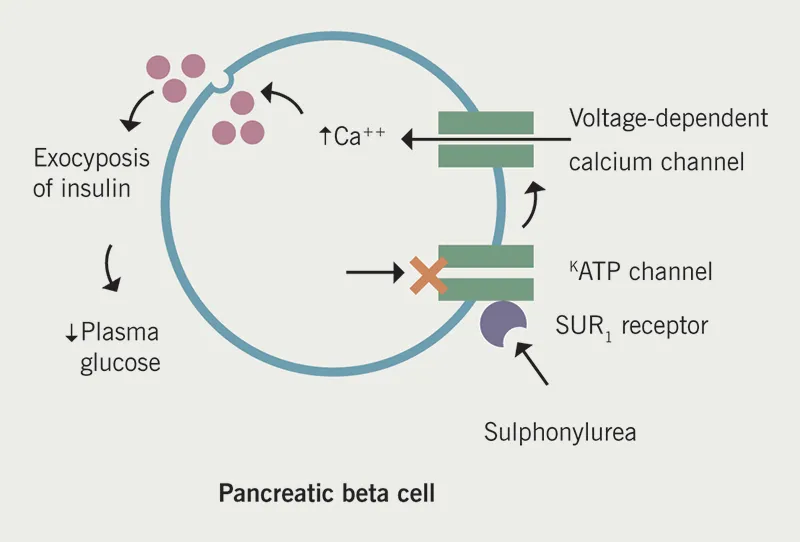
- Sulfonylureas (SUs): Close K-ATP channels on β-cells.
- 1st Gen: Chlorpropamide (SIADH).
- 2nd Gen: Glipizide (shortest), Glibenclamide (↑hypoglycemia), Glimepiride.
- SE: Hypoglycemia, weight gain.
- Meglitinides (Glinides): Repaglinide, Nateglinide. Rapid onset, short duration. For postprandial spikes.
- Sulfonylureas (SUs): Close K-ATP channels on β-cells.
- Metformin (Biguanide): First-line T2DM.
- MoA: ↓Hepatic gluconeogenesis, ↑Peripheral glucose uptake (AMPK activation).
- Benefits: Euglycemic, weight neutral/loss, ↓CV risk.
- SE: GI upset (most common), lactic acidosis (rare, ⚠️ eGFR < 30 mL/min/1.73m²), B12 deficiency.
⭐ Metformin: first-line T2DM, typically no hypoglycemia when used as monotherapy.
Glitazones & Glucosidase Blockers - Cellular & Gut Tactics
- Glitazones (TZDs): e.g., Pioglitazone
- Mechanism: PPAR-γ agonists → ↑ insulin sensitivity (muscle, fat). Slow onset (weeks).
- Side Effects: Weight gain, edema (⚠️ CHF exacerbation), hepatotoxicity, ↑ fracture risk. Pioglitazone: ?Bladder Ca risk.
- Benefits: ↓ TGs, ↑ HDL (Pioglitazone).

- α-Glucosidase Inhibitors: e.g., Acarbose, Voglibose
- Mechanism: Inhibit intestinal α-glucosidase → delay carbohydrate digestion/absorption → ↓ postprandial glucose.
- Side Effects: GI distress (flatulence, diarrhea). Take with first bite of meal.
⭐ If hypoglycemia occurs (with combination therapy), treat with glucose (dextrose), not sucrose.
Incretins, Gliptins & Flozins - New Wave Agents
- Incretin Mimetics (GLP-1 Agonists): E.g., Liraglutide, Semaglutide.
- MOA: ↑ Insulin, ↓ Glucagon, ↓ Gastric emptying, ↑ Satiety.
- Benefits: Weight ↓, CV protection. Injectable.
- SE: GI upset, pancreatitis risk.
- Gliptins (DPP-4 Inhibitors): E.g., Sitagliptin, Linagliptin.
- MOA: Inhibit DPP-4 → ↑ GLP-1/GIP. Oral.
- Benefits: Weight neutral. 📌 "Gliptins keep GLP-1 intact."
- SE: Nasopharyngitis, rare pancreatitis.
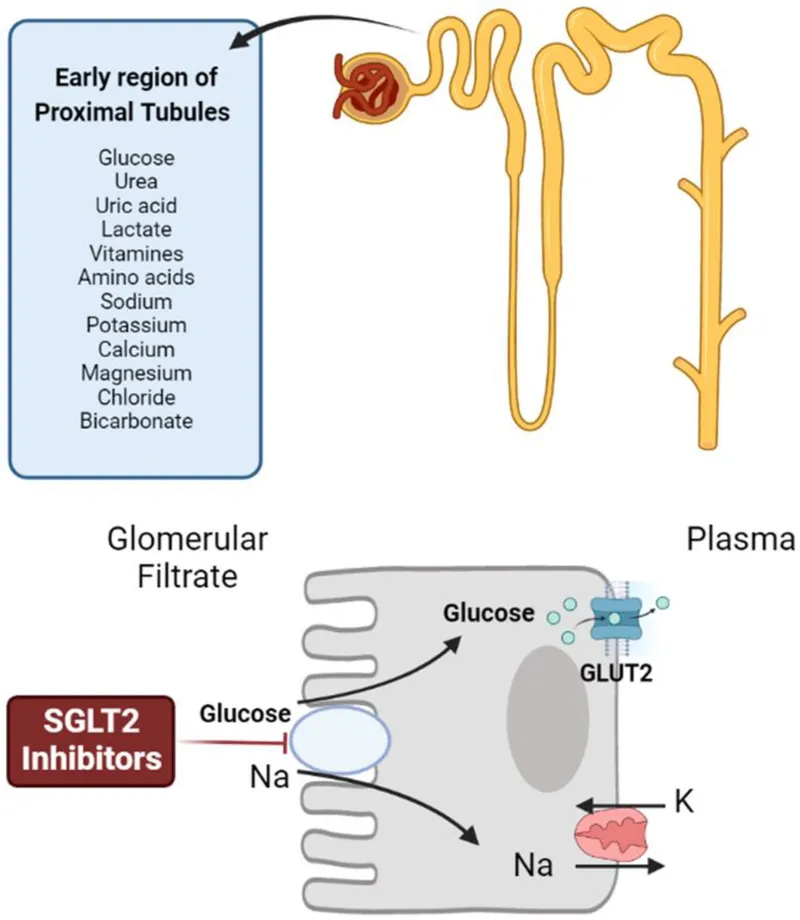
- Flozins (SGLT2 Inhibitors): E.g., Dapagliflozin, Empagliflozin.
- MOA: Block SGLT2 in kidney → Glucosuria. Oral.
- Benefits: Weight ↓, BP ↓.
- SE: UTIs, genital infections, euglycemic DKA risk.
⭐ SGLT2 inhibitors demonstrate significant cardiovascular and renal protective benefits.
High‑Yield Points - ⚡ Biggest Takeaways
- Rapid-acting insulins (lispro, aspart) for prandial; long-acting (glargine, detemir) for basal.
- Metformin: first-line T2DM, ↓ hepatic gluconeogenesis; risk: lactic acidosis.
- Sulfonylureas (glimepiride): ↑ insulin secretion; risk: hypoglycemia, weight gain.
- SGLT2 inhibitors (empagliflozin): glucosuria, CV benefit, weight loss; risk: UTIs, euglycemic DKA.
- GLP-1 agonists (liraglutide): ↑ insulin, ↓ glucagon, promote weight loss.
- DPP-4 inhibitors (sitagliptin): ↑ incretin levels, weight neutral.
- Thiazolidinediones (pioglitazone): PPAR-γ agonist, ↑ insulin sensitivity; risk: edema, HF, fractures.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

