Back
How to Study Ophthalmology for NEET PG 2026: High-Yield Topics, Image-Based Questions and Exam Strategy
Complete ophthalmology study guide for NEET PG 2026. Master image-based questions, high-yield topics like diabetic retinopathy and glaucoma, plus proven exam strategies for maximum scores.

How to Study Ophthalmology for NEET PG 2026: High-Yield Topics, Image-Based Questions and Exam Strategy
Youre staring at another ophthalmology question with a fundus photograph, and you have no idea if thats diabetic retinopathy or hypertensive retinopathy. Sound familiar?
Ophthalmology carries 12-15 questions in NEET PG, making up about 6% of your total score. That translates to roughly 72-90 marks - enough to make or break your rank. The catch? Most of these questions are image-based, testing pattern recognition rather than rote memorization.
Heres the reality: ophthalmology questions have shifted dramatically toward clinical images in the past 3 years. You cant just memorize classification lists anymore. You need to recognize fundus photographs, slit-lamp findings, and external eye appearances instantly. The good news? Once you master the visual patterns, ophthalmology becomes one of the most predictable subjects in NEET PG.
This guide breaks down exactly how to study ophthalmology for NEET PG 2026, focusing on high-yield topics that appear repeatedly and the specific image recognition skills youll need on exam day.
Understanding NEET PG Ophthalmology Question Pattern
NEET PG ophthalmology has evolved into a heavily image-dependent subject. Heres what you can expect:
12-15 questions total (6% weightage)
70% image-based questions (fundus photos, slit-lamp images, external eye photos)
30% theoretical questions (medical management, surgical indications, anatomy)
High repeatability - same image types appear every year with slight variations
Question Distribution by Topic:
Retinal disorders: 4-5 questions
Glaucoma: 2-3 questions
Cataract and lens disorders: 2 questions
Corneal and external eye diseases: 2-3 questions
Optic nerve disorders: 1-2 questions
Ocular manifestations of systemic diseases: 2 questions
The key insight? Focus your image recognition practice on retinal disorders and glaucoma - they dominate the question paper.
High-Yield Ophthalmology Topics for NEET PG 2026
1. Diabetic Retinopathy (Must-Know Topic)
This appears in 2-3 questions every year, always with fundus photographs.
Essential Recognition Points:
Non-proliferative DR: Hard exudates, soft exudates, microaneurysms, flame-shaped hemorrhages
Proliferative DR: Neovascularization, vitreous hemorrhage, tractional retinal detachment
Diabetic maculopathy: Hard exudates in macula, macular edema
High-Yield Facts:
First sign: microaneurysms
Most common cause of blindness in diabetics: macular edema
Indication for panretinal photocoagulation: neovascularization
Cotton wool spots = nerve fiber layer infarcts
Use Oncourses ophthalmology flashcards to drill fundus image recognition - the spaced repetition helps you distinguish between different stages of DR within seconds.
2. Glaucoma (High-Yield Image Topic)
Expect 2-3 questions, split between acute angle closure and chronic open angle glaucoma.
Visual Recognition Keys:
Acute angle closure: Corneal edema, shallow anterior chamber, mid-dilated pupil
Chronic open angle: Cupped disc with increased cup-disc ratio (>0.6), nasal displacement of vessels
Normal tension glaucoma: Cupping without raised IOP
Clinical Correlations:
Acute angle closure: IOP >40 mmHg, halos around lights, severe pain
POAG: Gradual visual field loss, starting with paracentral scotomas
Treatment: Prostaglandin analogs (latanoprost) first line for POAG
Memory Hook: "ACUTE" for angle closure - Anterior chamber shallow, Corneal edema, Unilateral pain, Tension high, Emergency
3. Age-Related Macular Degeneration (AMD)
Always appears with characteristic fundus images.
Pattern Recognition:
Dry AMD: Drusen (yellow deposits), geographic atrophy
Wet AMD: Subretinal hemorrhage, hard exudates, pigment epithelial detachment
Disciform scar: End-stage wet AMD
Clinical Points:
Dry AMD: More common (90%), slower progression
Wet AMD: Rapid vision loss, needs urgent anti-VEGF therapy
Amsler grid testing: Metamorphopsia in wet AMD
4. Hypertensive Retinopathy
Classic fundus findings that repeat yearly.
Grade Recognition:
Grade I: Arterial narrowing, increased light reflex
Grade II: AV nicking, copper wire arteries
Grade III: Flame hemorrhages, cotton wool spots
Grade IV: Papilledema, hard exudates, silver wire arteries
Key Associations:
Cotton wool spots: Nerve fiber layer infarcts
Hard exudates: Lipid deposits
AV nicking: Arteriovenous crossing changes
The Synapses mnemonic game has excellent visual mnemonics for remembering hypertensive retinopathy grades - much more effective than rote memorization.
5. Cataract Classification and Surgery
Visual Types (Image-Based):
Nuclear cataract: Yellow-brown nucleus
Cortical cataract: Spoke-wheel appearance
Posterior subcapsular: Central opacity, affects near vision most
Mature cataract: Completely opaque lens
Surgical Indications:
Visual acuity <6/60 or functional visual impairment
Phacoemulsification: Gold standard technique
IOL power calculation: SRK-T formula most accurate
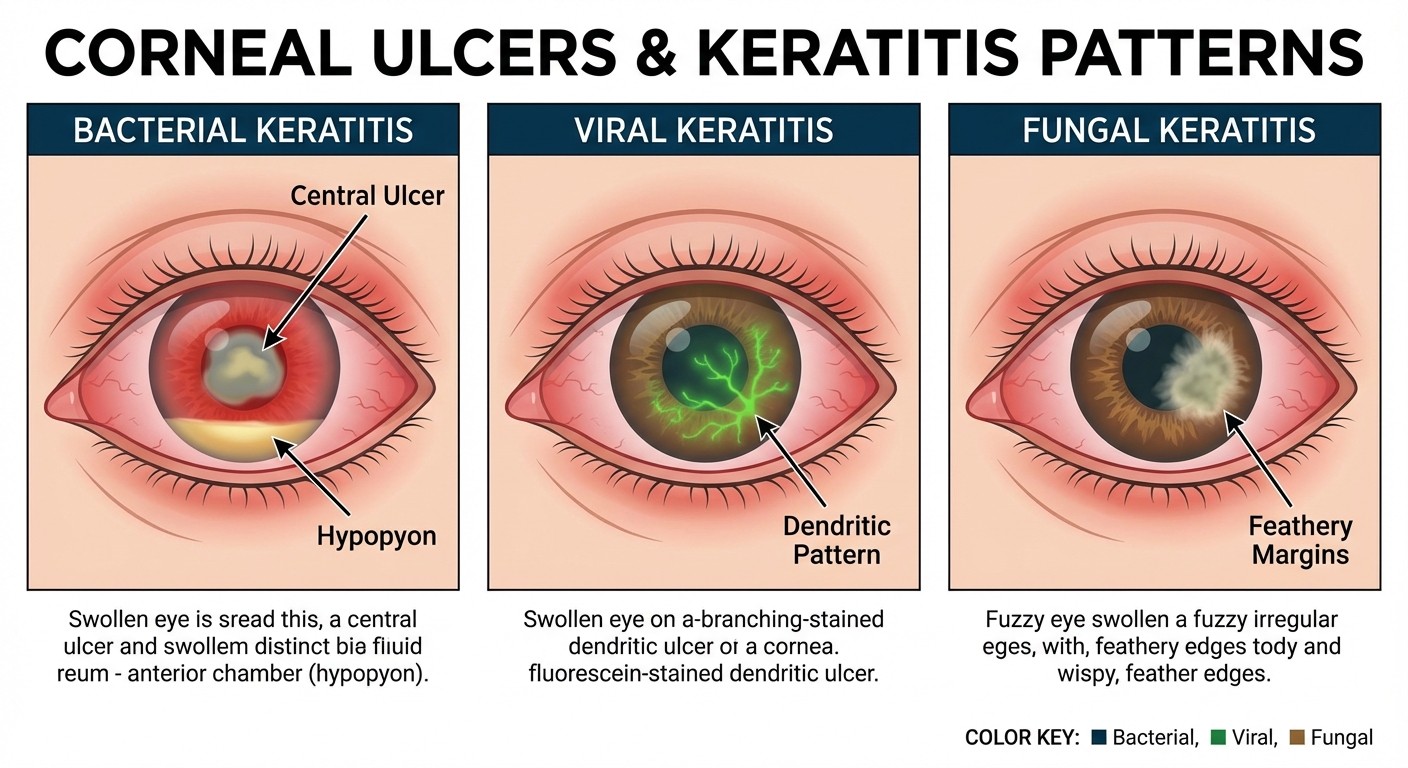
6. Corneal Disorders (Image Recognition Focus)
High-Yield Conditions:
Bacterial keratitis: Central ulcer with hypopyon
Viral keratitis: Dendritic ulcers (HSV), geographic ulcers (HZV)
Fungal keratitis: Feathery margins, satellite lesions
Pterygium: Triangular fibrovascular growth, nasal side more common
Treatment Pearls:
Bacterial keratitis: Fortified antibiotics
HSV keratitis: Topical acyclovir
Fungal keratitis: Topical antifungals (natamycin for filamentary)
Mastering Image-Based Questions
Image recognition is where most students struggle in ophthalmology. Heres your systematic approach:
Step 1: Learn the Normal First
Before jumping into pathology, spend 2 days understanding normal fundus anatomy:
Optic disc: Pink, well-demarcated margins
Macula: Avascular zone, foveal reflex
Blood vessels: Arteries (bright red), veins (dark red), A:V ratio 2:3
Background: Uniform orange-red reflex
Step 2: Pattern-Based Learning
Group similar-looking conditions and learn differentiating features:
Cotton Wool Spots Differential:
Diabetic retinopathy: Multiple, scattered
Hypertensive retinopathy: Few, peripapillary
HIV retinopathy: Multiple, no other diabetic changes
CRVO: Extensive, with hemorrhages
Disc Swelling Differential:
Papilledema: Bilateral, obscured margins, no visual loss initially
Papillitis: Unilateral, central scotoma, painful eye movements
AION: Altitudinal field defect, pale swelling
Step 3: Systematic Image Analysis
Develop a consistent approach for every fundus photograph:
1. Disc: Size, color, margins, cup-disc ratio
2. Vessels: Caliber, AV ratio, abnormal vessels
3. Macula: Exudates, edema, hemorrhages
4. Periphery: Hemorrhages, exudates, new vessels
5. Background: Color, uniformity, abnormal pigmentation
Practice this sequence with every image until it becomes automatic. The Probe game tests your pattern recognition speed - aim for <10 seconds per fundus image identification.
Strategic Study Plan for Ophthalmology
Phase 1: Foundation (Days 1-5)
Day 1-2: Basic anatomy and normal fundus
Day 3-4: Optics and refraction basics
Day 5: Examination techniques and instruments
Phase 2: High-Yield Pathology (Days 6-12)
Day 6-7: Diabetic retinopathy (all stages)
Day 8-9: Glaucoma (acute and chronic)
Day 10: AMD and other macular disorders
Day 11: Hypertensive and vascular retinopathies
Day 12: CRVO, CRAO, and optic nerve disorders
Phase 3: Image Mastery (Days 13-15)
Day 13: Corneal and external eye conditions
Day 14: Cataract types and lens disorders
Day 15: Mixed image practice and rapid recognition
Study from Oncourses comprehensive ophthalmology lessons - they integrate theory with image banks, so youre learning recognition alongside concepts.
Essential Memory Techniques
Visual Mnemonics for Retinal Disorders
"4 H's of Diabetic Retinopathy":
Hard exudates
Hemorrhages (dot-blot)
Hemorrhages (flame-shaped)
Hyperplasia (neovascularization)
"CALM" for Glaucoma Management:
Carbonic anhydrase inhibitors
Alpha agonists
Latanoprost (prostaglandin analogs)
Miotics (pilocarpine)
Number-Based Facts
High-yield numbers that appear repeatedly:
Normal IOP: 12-20 mmHg
Cup-disc ratio >0.6: Suspicious for glaucoma
Visual acuity <6/60: Cataract surgery indication
AMD prevalence: 10% in >65 years
Diabetic retinopathy: Leading cause of blindness in 20-65 years
Rezzy AI can help you create personalized mnemonics for these number associations - just ask it to generate memory hooks for specific ophthalmology facts youre struggling with.
Common Mistakes to Avoid
1. Confusing Similar-Looking Conditions
Hard Exudates vs Soft Exudates:
Hard exudates: Yellow, well-demarcated, lipid deposits
Soft exudates: Gray-white, fluffy, cotton wool spots (nerve fiber infarcts)
Papilledema vs Papillitis:
Papilledema: Bilateral, no early visual symptoms
Papillitis: Unilateral, immediate central vision loss
2. Overlooking Clinical Correlations
Dont just memorize images - connect them to symptoms:
Central scotoma → Macular pathology
Peripheral field loss → Glaucoma or retinal detachment
Altitudinal field defect → AION
Metamorphopsia → Wet AMD or macular hole
3. Ignoring Treatment Priorities
NEET PG loves treatment-based questions:
Acute angle closure: Immediate IOP reduction (mannitol, acetazolamide)
Wet AMD: Anti-VEGF injection within days
Central retinal artery occlusion: Ocular massage, hyperbaric oxygen within hours
Endophthalmitis: Immediate vitrectomy and antibiotics
Practice Strategy for Maximum Retention
Daily Practice Schedule
Week 1: 20 images/day (10 minutes) Week 2: 30 images/day (15 minutes) Week 3: 50 images/day (20 minutes)
Focus on speed and accuracy. If you cant identify a condition within 10 seconds of seeing the image, you need more practice with that pattern.
Question Bank Strategy
Use Oncourses ophthalmology question bank for targeted practice:
Start with topic-wise questions to build confidence
Move to mixed practice once you hit 80% accuracy per topic
Focus extra time on your weak areas (most students struggle with corneal conditions)
Practice explanation reading - NEET PG explanations often contain high-yield teaching points
Image Bank Resources
Create your own image collection from multiple sources:
Standard textbook images (Khurana, Parson's)
Online ophthalmology atlases
Previous year NEET PG questions
Clinical photographs from journals
Review your image collection daily - active recall works better than passive recognition.
Exam Day Strategy
Time Management
Allocate 45-60 seconds per ophthalmology question
Image-based questions: 30 seconds for recognition, 15 seconds for options
Theory questions: 45 seconds maximum
Image Analysis Under Pressure
1. Quick overall scan (3 seconds)
2. Focus on most obvious abnormality (5 seconds)
3. Confirm with systematic analysis (10 seconds)
4. Choose answer (2 seconds)
Elimination Techniques
When unsure between two options:
Choose the more common condition
Pick the option that matches the demographic (elderly = AMD, young diabetic = DR)
Trust your first instinct on image recognition
Frequently Asked Questions
How many ophthalmology questions can I expect in NEET PG 2026?
You can expect 12-15 ophthalmology questions, representing about 6% of the total paper. This translates to roughly 72-90 marks, making it a significant scoring opportunity.
Are ophthalmology questions mostly image-based?
Yes, approximately 70% of ophthalmology questions now include clinical images, particularly fundus photographs, slit-lamp findings, and external eye conditions. The remaining 30% test theoretical knowledge about management and surgical indications.
Which ophthalmology topics have the highest weightage?
Retinal disorders (especially diabetic retinopathy) and glaucoma together account for 6-8 questions. These should be your primary focus, followed by AMD, hypertensive retinopathy, and cataract classification.
How can I improve my fundus image recognition speed?
Practice systematic analysis: disc → vessels → macula → periphery → background. Start with 20 images daily and gradually increase to 50 images. Use spaced repetition tools and aim for <10 seconds recognition time.
Is it worth studying rare ophthalmology conditions?
No, focus on high-yield conditions that repeat yearly. Spend 80% of your time on the top 10 conditions rather than trying to cover everything. Rare conditions occasionally appear but shouldnt be your priority.
How should I balance theory vs image practice in ophthalmology?
Spend 60% time on image recognition and 40% on theory. However, integrate them - learn pathophysiology while studying images, so you understand why certain findings appear together.
---
Prepare smarter with Oncourse AI — adaptive MCQs, spaced repetition, and AI explanations built for NEET PG. Download free on Android and iOS.