Back
How to Solve Clinical Case Scenarios for NEET-PG and USMLE: A Complete Strategy Guide
Master clinical case scenarios with the proven MASTER framework used by top NEET-PG and USMLE scorers. Learn systematic approaches, time management, and advanced reasoning techniques for 90%+ accuracy.

How to Solve Clinical Case Scenarios for NEET-PG and USMLE: A Complete Strategy Guide
Clinical case scenarios represent 60-70% of questions in NEET-PG and form the backbone of USMLE Step 2 CK. Yet most medical students approach these questions reactively, reading through vignettes without a systematic strategy. Master diagnosticians follow proven frameworks that transform complex patient presentations into clear diagnostic pathways.
This guide reveals the exact methodologies used by top scorers to achieve 90%+ accuracy in clinical scenarios, backed by cognitive science research and proven exam strategies.
Why Clinical Case Scenarios Matter in Medical Exams
Clinical case scenarios test your ability to integrate knowledge, recognize patterns, and make diagnostic decisions under pressure. Unlike straightforward factual questions, these vignettes simulate real clinical encounters where you must:
Analyze patient presentations with incomplete information
Generate differential diagnoses based on available data
Prioritize investigations and treatment approaches
Apply clinical reasoning under time constraints
Exam Weightage and Impact
Exam | Clinical Scenario Percentage | Total Questions | Average Time Per Question |
|---|---|---|---|
NEET-PG | 65-70% | 200 | 90 seconds |
USMLE Step 2 CK | 80-85% | 318 | 90 seconds |
INI-CET | 60-65% | 200 | 90 seconds |
The high weightage means mastering clinical scenarios can single-handedly determine your exam outcome. Students who excel at case analysis typically score in the 95th percentile or higher.
The MASTER Framework: A Systematic Approach to Clinical Cases
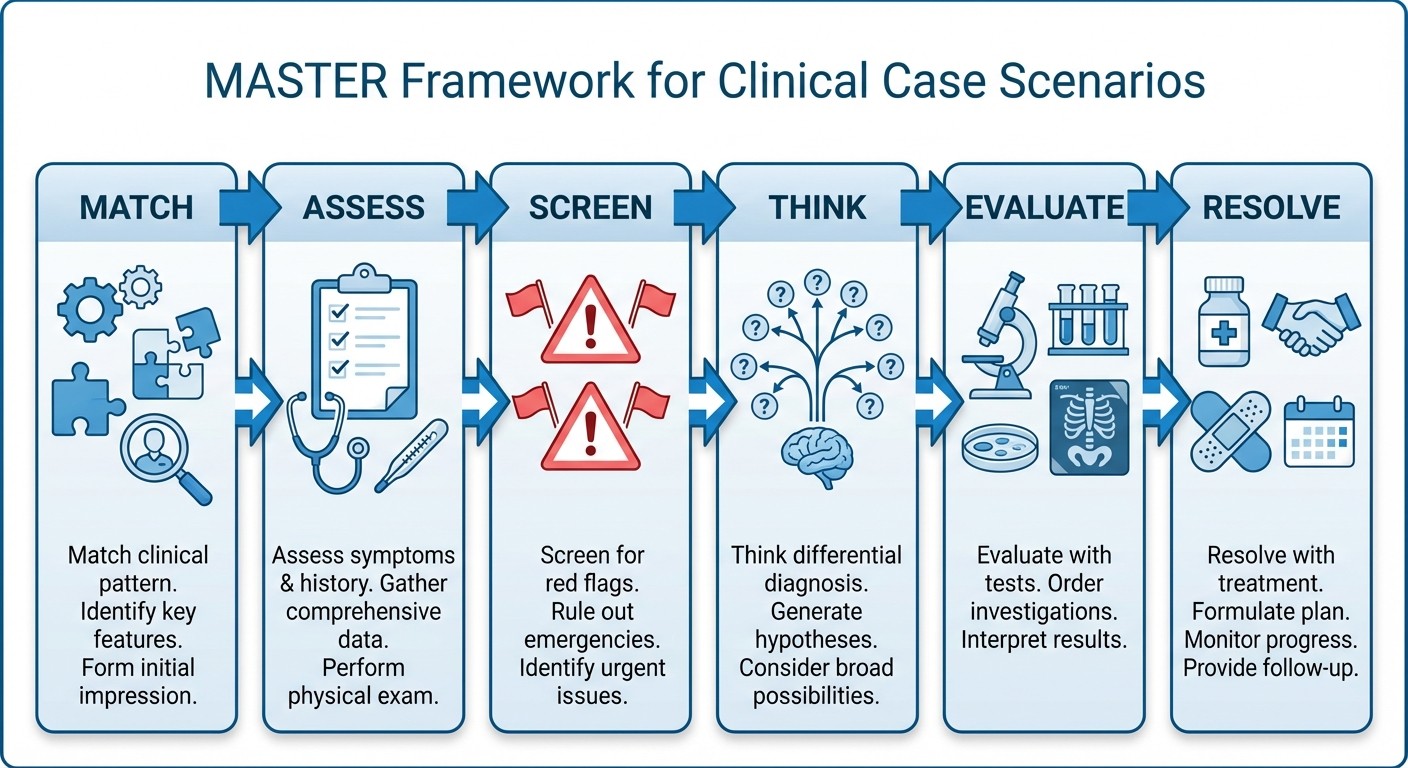
After analyzing thousands of high-yield clinical scenarios, successful candidates consistently apply the MASTER framework:
Match the clinical picture
Assess key symptoms and signs
Screen for red flags
Think differentials systematically
Evaluate with targeted investigations
Resolve with appropriate management
Step 1: Match the Clinical Picture (15-20 seconds)
Before diving into details, quickly identify the clinical pattern. Expert clinicians recognize presentations within 3 seconds through pattern recognition developed over years of practice.
Pattern Recognition Categories:
Acute presentations: Chest pain, dyspnea, altered mental status
Chronic conditions: Progressive weakness, weight loss, recurring symptoms
Emergency scenarios: Trauma, cardiac arrest, shock states
Pediatric patterns: Age-specific presentations and developmental considerations
Step 2: Assess Key Symptoms and Signs (20-25 seconds)
Systematically extract and categorize information from the vignette. Focus on high-yield discriminating features that narrow your differential diagnosis.
Assessment Hierarchy: 1. Chief complaint and duration 2. Associated symptoms (timing, quality, severity) 3. Physical examination findings 4. Vital signs and basic parameters 5. Past medical history and medications Pro Tip: Underline or mentally note qualifying words like "sudden," "gradual," "cramping," "burning," or "radiating" - these often point directly to the correct diagnosis.
Step 3: Screen for Red Flags (10-15 seconds)
Immediately identify life-threatening conditions that require urgent intervention. This step prevents you from getting distracted by less critical differentials.
Universal Red Flags:
Cardiovascular: Chest pain with diaphoresis, ECG changes
Respiratory: Severe dyspnea, oxygen desaturation
Neurological: Altered consciousness, focal deficits
Gastrointestinal: Severe abdominal pain, hematemesis
Infectious: High fever with altered mental status
Step 4: Think Differentials Systematically (25-30 seconds)
Generate 3-5 most likely diagnoses using systematic approaches. The key is organized thinking, not exhaustive lists.
Differential Generation Strategies:
1. Anatomical approach: Consider each organ system
2. Pathophysiological approach: Infectious, inflammatory, neoplastic, metabolic
3. Frequency-based approach: Common conditions first, then rare causes
4. Age-specific approach: Consider typical conditions for the patient's age group
Example - Chest Pain Differentials:
Cardiac: MI, angina, pericarditis
Pulmonary: PE, pneumothorax, pneumonia
Gastrointestinal: GERD, esophageal spasm
Musculoskeletal: Costochondritis, rib fracture
Advanced Clinical Reasoning Techniques
Bayesian Diagnostic Reasoning
Expert clinicians unconsciously apply Bayesian probability to update their diagnostic confidence as new information emerges. You can develop this skill systematically.
Bayesian Process: 1. Prior probability: Start with pre-test probability based on demographics and chief complaint 2. Likelihood ratios: Update probability based on symptoms, signs, and test results 3. Posterior probability: Final diagnostic confidence after integrating all evidence
OnCourse's clinical reasoning lessons provide interactive training in probabilistic thinking and diagnostic calibration.
Pattern Recognition Development
Research shows expert diagnosticians maintain 500-1000 illness scripts per specialty. Build your pattern library through deliberate practice:
Pattern Building Strategy:
Study classic presentations for each major condition
Learn discriminating features that distinguish similar conditions
Practice with varied presentations of the same disease
Build exception awareness for atypical presentations
Cognitive Bias Awareness
Diagnostic errors often result from cognitive biases rather than knowledge gaps. Common biases in clinical reasoning include:
Anchoring bias: Fixating on initial impressions
Availability heuristic: Overweighting recent or memorable cases
Confirmation bias: Seeking only confirming evidence
Premature closure: Stopping investigation too early
Learn more about avoiding these pitfalls in OnCourse's cognitive biases in clinical reasoning module.
Exam-Specific Strategies
NEET-PG Clinical Case Approach
NEET-PG emphasizes rapid pattern recognition with Indian clinical contexts. Focus on:
High-Yield NEET-PG Patterns:
Infectious diseases: TB, malaria, dengue, typhoid
Nutritional disorders: Anemia, vitamin deficiencies
Tropical medicine: Region-specific presentations
Public health scenarios: Vaccination, epidemiology
Time Management:
Spend maximum 90 seconds per case scenario
If unsure after 60 seconds, make educated guess and move on
Save difficult cases for review if time permits
Explore OnCourse's NEET-PG preparation resources for targeted practice and high-yield content review.
USMLE Step 2 CK Clinical Approach
USMLE emphasizes systematic clinical reasoning and evidence-based management. Key strategies:
USMLE-Specific Focus:
Next best step: Understand workflow and priority setting
Management decisions: Know guidelines and standard protocols
Ethics and communication: Patient-centered care principles
Quality improvement: Cost-effectiveness and population health
Question Types:
Diagnostic questions (35%): What is the most likely diagnosis?
Management questions (40%): What is the next best step?
Prognostic questions (15%): What is the expected outcome?
Prevention questions (10%): What preventive measure is indicated?
Access comprehensive USMLE preparation through OnCourse's USMLE Clinical Rounds for AI-powered case practice.
Common Clinical Case Question Types
Diagnostic Questions
Approach Strategy:
1. Identify the most discriminating symptoms
2. Match with classic disease patterns
3. Rule out life-threatening conditions first
4. Choose the most likely diagnosis based on epidemiology
Example Framework:
"A 45-year-old male presents with..." → Consider age-appropriate conditions
Key symptoms → Match to illness scripts
Physical findings → Confirm or refute hypothesis
Choose best fit diagnosis
Management Questions
Decision-Making Hierarchy: 1. Stabilize the patient (ABCs - Airway, Breathing, Circulation) 2. Confirm the diagnosis if unclear 3. Initiate appropriate treatment based on guidelines 4. Monitor and follow-up as indicated Common Management Stems:
"What is the next best step?" → Immediate priority
"What is the most appropriate treatment?" → Standard therapy
"What should be done first?" → Triage decision
Prognostic Questions
Focus on natural history, complications, and expected outcomes based on evidence-based medicine.
Key Considerations:
Disease severity and staging
Patient comorbidities and risk factors
Treatment response and complications
Long-term outcomes and quality of life
Practice Strategies for Clinical Case Mastery
Deliberate Practice Methodology
Research demonstrates that deliberate practice with immediate feedback accelerates expertise development. Follow these principles:
Effective Practice Structure: 1. Timed practice sessions: Simulate exam conditions 2. Immediate feedback: Review explanations after each question 3. Error analysis: Identify reasoning mistakes, not just wrong answers 4. Spaced repetition: Return to challenging cases after intervals
Case-Based Learning Tools
Recommended Resources:
1. OnCourse Clinical Rounds: AI-powered virtual patients with personalized feedback and gamified learning experience
2. Question banks: High-yield cases with detailed explanations
3. Textbook cases: Classic presentations from standard references
4. Online simulators: Interactive case-solving platforms
OnCourse's Clinical Rounds game provides unlimited practice with virtual patients, offering personalized feedback and progress tracking to accelerate your clinical reasoning development.
Study Group Strategies
Collaborative case analysis enhances learning through diverse perspectives:
Group Practice Format:
Case presentation: One member presents the scenario
Group differential: Brainstorm possible diagnoses
Evidence review: Systematically evaluate each possibility
Consensus decision: Agree on most likely diagnosis and management
Time Management and Exam Day Strategy
Optimal Time Allocation
Per Question Breakdown (90 seconds total):
Reading and understanding: 20-25 seconds
Analysis and differential: 35-40 seconds
Decision making: 15-20 seconds
Review and confirmation: 10-15 seconds
Guessing Strategy
When unsure, apply these evidence-based guessing techniques:
Smart Guessing Rules: 1. Common conditions are more likely than rare diseases 2. Simple treatments are usually preferred over complex interventions 3. Conservative management is often correct before invasive procedures 4. Age-appropriate conditions match demographic patterns
Managing Test Anxiety
Clinical scenarios can be overwhelming due to their complexity. Combat anxiety with:
Anxiety Management Techniques:
Systematic approach: Follow your framework consistently
Breathing control: Take deep breaths between difficult cases
Positive self-talk: Remind yourself of successful practice sessions
Time awareness: Don't panic if behind schedule - maintain pace
Building Long-Term Clinical Reasoning Skills
Beyond Exam Success
The clinical reasoning skills developed for exam success translate directly to clinical practice. Focus on:
Transferable Skills:
Systematic thinking: Approach every patient encounter methodically
Evidence integration: Combine clinical findings with research evidence
Uncertainty tolerance: Make decisions with incomplete information
Continuous learning: Update knowledge based on new evidence
Career Development
Strong clinical reasoning abilities distinguish exceptional physicians. Continue developing these skills through:
Ongoing Development:
Case conferences: Participate actively in multidisciplinary discussions
Journal clubs: Stay current with clinical research
Mentorship: Learn from experienced clinicians
Reflective practice: Analyze your decision-making process regularly

Frequently Asked Questions
How many clinical cases should I practice daily?
For optimal skill development, practice 20-30 clinical scenarios daily during intense preparation phases. Focus on quality analysis rather than quantity - spending 5 minutes reviewing explanations is more valuable than rushing through additional cases.
What if I can't identify the pattern within 20 seconds?
Don't panic. Move systematically through the MASTER framework even if pattern recognition fails. Many cases are designed to test analytical reasoning rather than immediate pattern matching.
How do I improve my speed without sacrificing accuracy?
Develop automatic responses to common patterns through spaced repetition. Practice with time pressure regularly, and learn to recognize when detailed analysis is necessary versus when quick pattern matching suffices.
Should I memorize specific case presentations?
Focus on understanding underlying principles rather than memorizing specific cases. Disease patterns vary, but pathophysiological principles remain consistent. Build flexible knowledge that adapts to novel presentations.
How important are rare diseases in clinical scenarios?
Rare diseases typically comprise 5-10% of clinical scenarios. Focus 80% of your study time on common conditions, but maintain awareness of zebra diagnoses that present with common symptoms.
Conclusion: Master Clinical Reasoning for Exam Success
Clinical case scenarios separate good medical students from exceptional ones. Success requires more than medical knowledge - it demands systematic thinking, pattern recognition, and decision-making under pressure.
The MASTER framework provides a reproducible approach to clinical reasoning that works across different exam formats and clinical contexts. Combined with deliberate practice using high-quality resources like OnCourse's AI-powered clinical rounds, you can achieve the 90%+ accuracy that distinguishes top performers.
Remember that clinical reasoning skills extend far beyond exam success. The systematic thinking, evidence integration, and decision-making abilities you develop will serve you throughout your medical career, making you a more effective and confident physician.
Start practicing with structured approaches today. Your patients - and your exam scores - will thank you.
Ready to master clinical reasoning? Explore OnCourse's comprehensive clinical reasoning curriculum and start practicing with AI-powered Clinical Rounds for personalized feedback and unlimited case scenarios.