Clinical Manifestations and Presentation of Diseases Indian Medical PG Practice Questions and MCQs
Practice Indian Medical PG questions for Clinical Manifestations and Presentation of Diseases. These multiple choice questions (MCQs) cover important concepts and help you prepare for your exams.
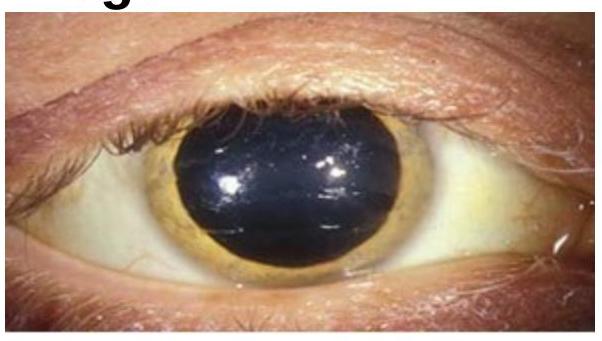
Clinical Manifestations and Presentation of Diseases Indian Medical PG Question 1: Choose the best method of diagnosis for the clinical sign represented in the image.
- A. Serum copper
- B. Serum ceruloplasmin (Correct Answer)
- C. Karyotyping
- D. PCR
Clinical Manifestations and Presentation of Diseases Explanation: ***Serum ceruloplasmin***
- The image shows a **Kayser-Fleischer ring**, a greenish-brown discoloration in the periphery of the cornea, which is pathognomonic for **Wilson's disease**.
- **Wilson's disease** is a genetic disorder of copper metabolism characterized by **low serum ceruloplasmin** levels (the primary copper-carrying protein in the blood) and increased copper deposition in various tissues.
*Serum copper*
- While Wilson's disease involves copper accumulation, **total serum copper** can be normal or even elevated due to widespread tissue damage releasing copper into the circulation, making it an unreliable diagnostic marker on its own.
- A low serum copper level can be seen, but it is not as specific as low ceruloplasmin, as much of the copper in serum is bound to ceruloplasmin.
*Karyotyping*
- **Karyotyping** is used to analyze the number and structure of chromosomes and is primarily indicated for diagnosing chromosomal abnormalities, such as Down syndrome or Turner syndrome.
- It is not relevant for diagnosing metabolic disorders like Wilson's disease, which is caused by a mutation in a single gene (ATP7B), not a chromosomal aberration.
*PCR*
- **PCR (Polymerase Chain Reaction)** is a technique used to amplify DNA sequences and can be used for genetic testing to identify specific mutations.
- While genetic testing for the **ATP7B gene** mutation is a confirmatory test for Wilson's disease, it is not the primary or best method for initial diagnosis, especially when classic clinical signs and biochemical markers (like low ceruloplasmin) are present.
Clinical Manifestations and Presentation of Diseases Indian Medical PG Question 2: You have diagnosed a patient clinically as having SLE and ordered 6 tests out of which 4 tests have come positive and 2 are negative. Which of the following values are required to determine the probability of SLE at this point?
- A. Relative risk of SLE in the patient
- B. Incidence and prevalence of SLE
- C. Prior probability of SLE, sensitivity and specificity of each test (Correct Answer)
- D. Incidence of SLE and the predictive value of each test
Clinical Manifestations and Presentation of Diseases Explanation: ***Prior probability of SLE, sensitivity and specificity of each test***
- To determine the **post-test probability** of a disease like SLE, you need the **prior probability** (pre-test probability) of the disease in the patient.
- Additionally, the **sensitivity** (true positive rate) and **specificity** (true negative rate) of *each* diagnostic test are crucial for calculating how much each positive or negative test result alters that prior probability, often using **Bayes' theorem**.
*Relative risk of SLE in the patient*
- **Relative risk** is a measure of association between exposure and disease, typically used in **epidemiological studies** to compare risk in exposed vs. unexposed groups.
- It does not directly help determine an individual patient's post-test probability of SLE based on their specific test results.
*Incidence and prevalence of SLE*
- **Incidence** refers to the rate of new cases in a population over a specific period, while **prevalence** refers to the proportion of individuals in a population who have the disease at a specific time.
- While prevalence can contribute to the **prior probability** for a general population, it's not sufficient on its own, nor does it incorporate the results of individual diagnostic tests.
*Incidence of SLE and the predictive value of each test*
- Although **predictive values (positive and negative)** are important for interpreting test results, they are *derived from* sensitivity, specificity, and prevalence.
- To *determine* the probability of SLE using multiple tests, you need the fundamental properties of the tests (sensitivity and specificity) and the prior probability, rather than just the incidence and already-calculated predictive values.
Clinical Manifestations and Presentation of Diseases Indian Medical PG Question 3: Which of the following is NOT a feature of Systemic Inflammatory Response Syndrome?
- A. Hypothermia (less than 36°C)
- B. Hyperthermia (more than 38°C)
- C. Bradycardia (Correct Answer)
- D. Leucocytosis
Clinical Manifestations and Presentation of Diseases Explanation: ***Bradycardia***
- **Bradycardia** (a slow heart rate) is **not** a typical diagnostic criterion for **Systemic Inflammatory Response Syndrome (SIRS)**.
- SIRS is usually associated with **tachycardia** (heart rate >90 beats/min) due to the body's increased metabolic demand and stress response [2].
*Hypothermia (less than 36°C)*
- **Hypothermia** (<36°C) is a recognized diagnostic criterion for **SIRS**, indicating a dysregulated thermoregulatory response.
- It often suggests a more severe or decompensated inflammatory state.
*Hyperthermia (more than 38°C)*
- **Hyperthermia** (>38°C) is a common and primary diagnostic criterion for **SIRS**, reflecting the body's inflammatory response to infection or injury [2], [3].
- This elevated core temperature is part of the systemic response to pathogens or tissue damage.
*Leucocytosis*
- **Leucocytosis** (white blood cell count >12,000 cells/mm³) is a key diagnostic criterion for **SIRS**, indicating a robust innate immune response [1], [2].
- A WBC count <4,000 cells/mm³ (leucopenia) or >10% immature neutrophils ("bands") also fulfills this criterion.
Clinical Manifestations and Presentation of Diseases Indian Medical PG Question 4: Which of the following factors is labelled as cytokine in the pathogenesis of Systemic Inflammatory Response Syndrome (SIRS)?
- A. Leukotrienes
- B. Nitric oxide
- C. Complements
- D. Tumor necrosis factor (Correct Answer)
Clinical Manifestations and Presentation of Diseases Explanation: ***Tumor necrosis factor***
- **Tumor necrosis factor (TNF-α)** is a prominent pro-inflammatory cytokine and a key mediator in the pathogenesis of **Systemic Inflammatory Response Syndrome (SIRS)** [1].
- It plays a crucial role in initiating and amplifying the inflammatory cascade, leading to systemic effects like fever, increased vascular permeability, and tissue damage [1].
*Leukotrienes*
- **Leukotrienes** are lipid mediators derived from arachidonic acid, involved in inflammation and allergic reactions [1].
- They are not classified as **cytokines**, which are protein signaling molecules [1].
*Nitric oxide*
- **Nitric oxide (NO)** is a gaseous signaling molecule with various physiological roles, including vasodilation and neurotransmission.
- While it contributes to the pathophysiology of SIRS, particularly in regulating vascular tone, it is not a **cytokine**.
*Complements*
- **Complements** are a system of plasma proteins that are part of the innate immune response, helping to clear pathogens [1].
- They participate in inflammation but are distinct from **cytokines**, which are regulatory proteins [1].
**References:**
[1] Kumar V, Abbas AK, et al.. Robbins and Cotran Pathologic Basis of Disease. 9th ed. Inflammation and Repair, pp. 93-101.
Clinical Manifestations and Presentation of Diseases Indian Medical PG Question 5: Match the following drugs in Column A with their contraindications in Column B.
| Column A | Column B |
| :-- | :-- |
| 1. Morphine | 1. QT prolongation |
| 2. Amiodarone | 2. Thromboembolism |
| 3. Vigabatrin | 3. Pregnancy |
| 4. Estrogen preparations | 4. Head injury |
- A. A-1, B-3, C-2, D-4
- B. A-4, B-1, C-3, D-2 (Correct Answer)
- C. A-3, B-2, C-4, D-1
- D. A-2, B-4, C-1, D-3
Clinical Manifestations and Presentation of Diseases Explanation: ***A-4, B-1, C-3, D-2***
- **Morphine** is contraindicated in **head injury** as it can increase intracranial pressure and mask neurological symptoms.
- **Amiodarone** is contraindicated in patients with **QT prolongation** due to its risk of inducing more severe arrhythmias like Torsades de Pointes.
- **Vigabatrin** is contraindicated during **pregnancy** due to its potential for teratogenicity and adverse effects on fetal development.
- **Estrogen preparations** are contraindicated in patients with a history of **thromboembolism** due to their increased risk of blood clot formation.
*A-1, B-3, C-2, D-4*
- This option incorrectly matches **Morphine** with QT prolongation and **Estrogen preparations** with head injury, which are not their primary contraindications.
- It also incorrectly links **Vigabatrin** with thromboembolism and **Amiodarone** with pregnancy.
*A-3, B-2, C-4, D-1*
- This choice incorrectly associates **Morphine** with pregnancy and **Vigabatrin** with head injury, which are not the most critical or direct contraindications.
- It also misaligns **Amiodarone** with thromboembolism and **Estrogen preparations** with QT prolongation.
*A-2, B-4, C-1, D-3*
- This option incorrectly matches **Morphine** with thromboembolism and **Amiodarone** with head injury, which are not their most significant contraindications.
- It also incorrectly links **Vigabatrin** with QT prolongation and **Estrogen preparations** with pregnancy.
More Clinical Manifestations and Presentation of Diseases Indian Medical PG questions available in the OnCourse app. Practice MCQs, flashcards, and get detailed explanations.