Prenatal care: routine screening tests, schedule and high-risk monitoring
Prenatal care is such a huge part of OB/GYN, and getting the timing right for all these screenings is key for both the boards and clinical practice! It's basically a timeline of keeping both mom and baby safe.
I'll break this down into the routine schedule, the specific tests by trimester, and how we pivot when things get high-risk.
1. Routine Prenatal Visit Schedule
For a standard, uncomplicated pregnancy, the visit frequency usually follows this pattern:
- Weeks 4–28: Every 4 weeks (once a month)
- Weeks 28–36: Every 2 weeks (twice a month)
- Weeks 36–Birth: Every week
2. Routine Screening Timeline
We can divide the screenings into trimesters to make them easier to memorize:
First Trimester (Weeks 1–12)
- Initial Visit: Confirm pregnancy, ultrasound for dating (most accurate in 1st trimester), and a full lab panel (CBC, Blood type/Rh, Rubella immunity, HIV, Syphilis, Hepatitis B, and Urinalysis/Culture).
- Aneuploidy Screening: Options include Cell-free DNA (cfDNA) (after 10 weeks) or the Combined Test (Nuchal translucency ultrasound + PAPP-A + hCG).
Second Trimester (Weeks 13–27)
- Anatomy Scan: A detailed ultrasound performed between weeks 18–22 to check fetal structures.
- Quad Screen: (If cfDNA wasn't done) Checks AFP, hCG, Estriol, and Inhibin A.
- Glucose Challenge Test: Usually done between weeks 24–28 to screen for Gestational Diabetes.
Third Trimester (Weeks 28–Birth)
- Rhogam: Administered at 28 weeks if the mother is Rh-negative.
- Group B Strep (GBS): Rectovaginal swab performed at weeks 36–37.
- Repeat Labs: Check for anemia (CBC) and sometimes repeat STI screening if high risk.
3. High-Risk Monitoring
When a pregnancy is flagged as high-risk (due to preeclampsia, gestational diabetes, or multiples), we step up the surveillance:
- Non-Stress Test (NST): Monitoring the fetal heart rate for accelerations.
- Biophysical Profile (BPP): An ultrasound evaluating fetal movement, tone, breathing, and amniotic fluid volume.
- Umbilical Artery Doppler: Used specifically in cases of Fetal Growth Restriction (FGR).
To help you visualize the flow of these screenings, let me pull up a clinical flowchart for prenatal management.
That table is a perfect summary of the aneuploidy screening markers—definitely something that shows up on exams!
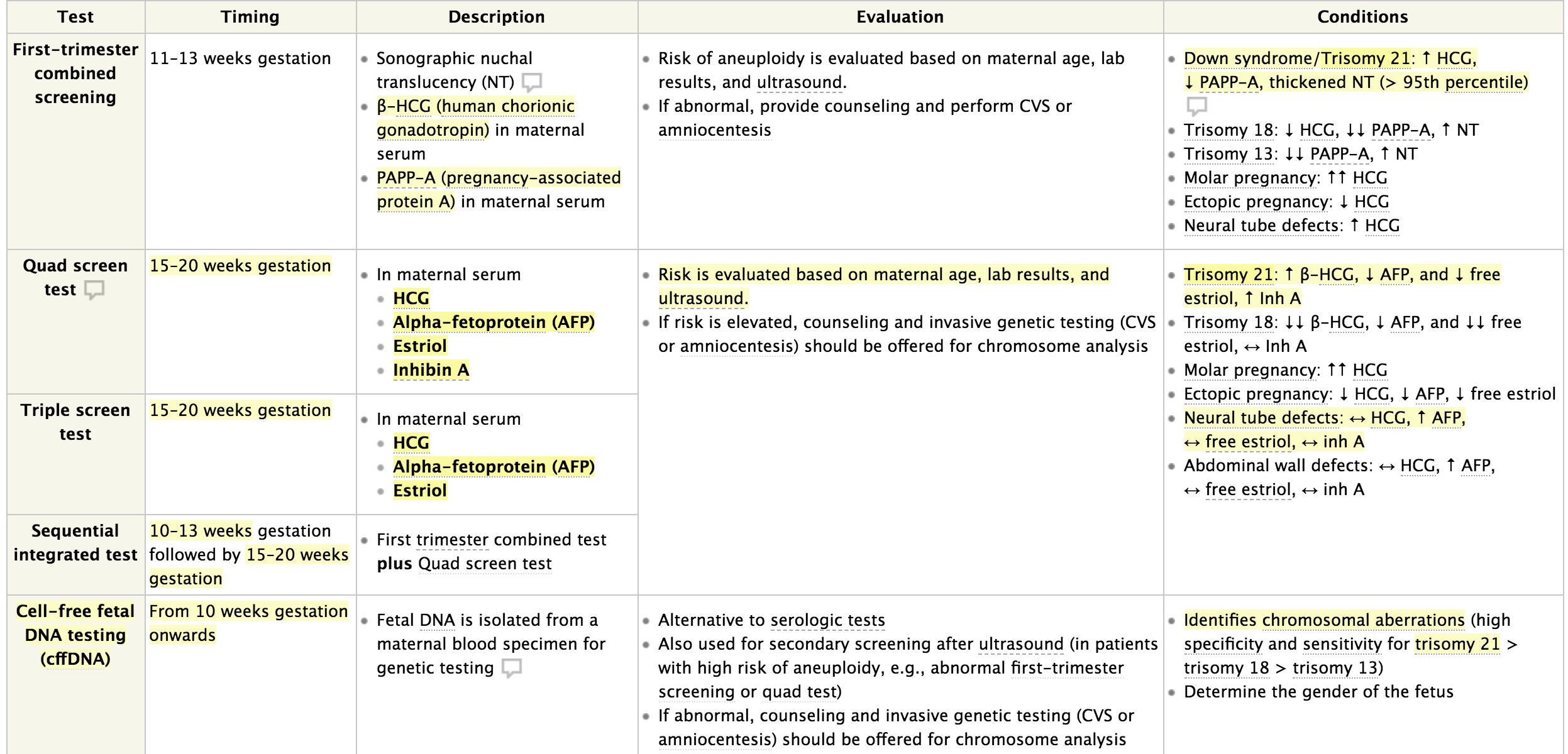
This table compares the different screening tests for chromosomal abnormalities, showing which markers (like hCG, AFP, and PAPP-A) are increased or decreased in conditions like Down Syndrome (Trisomy 21) and Edwards Syndrome (Trisomy 18).
To help you lock this in, I've got some great lessons and flashcards that go deeper into the specific management of high-risk conditions like preeclampsia and gestational diabetes.
📚 Prenatal Care Lessons
Those lessons cover everything from the routine checkups to the red flags that move a patient into the high-risk category.
To really cement the timing of these tests (like when to do the GBS swab or the glucose challenge), let's pull up some flashcards for quick review.
🗂️ Prenatal Screening Flashcards
Tap to study 18 flashcards in the Oncourse app
Those flashcards highlight some really high-yield "exceptions" to the rules—like when you don't need to screen for GBS because the patient already qualifies for antibiotics based on their history.
If you're feeling confident about the timeline, we could jump into a quick quiz to see how you'd handle these scenarios in a clinical case format. Or, if you want to see how we manage a specific high-risk condition like preeclampsia, just let me know!
Setting up chat...