Lipid metabolism: beta-oxidation, ketogenesis and dyslipidemias
Lipid metabolism is a massive topic, but it's essentially the body's way of managing its long-term energy bank. We're going to look at how we "withdraw" energy via beta-oxidation, what happens when the system gets overwhelmed (ketogenesis), and what happens when the transport system breaks down (dyslipidemias).
1. Beta-Oxidation: Burning the Fuel
Beta-oxidation is the process of breaking down fatty acids into Acetyl-CoA to enter the TCA cycle. This happens in the mitochondrial matrix.
- The Activation Step: Fatty acids are converted to Fatty Acyl-CoA in the cytosol.
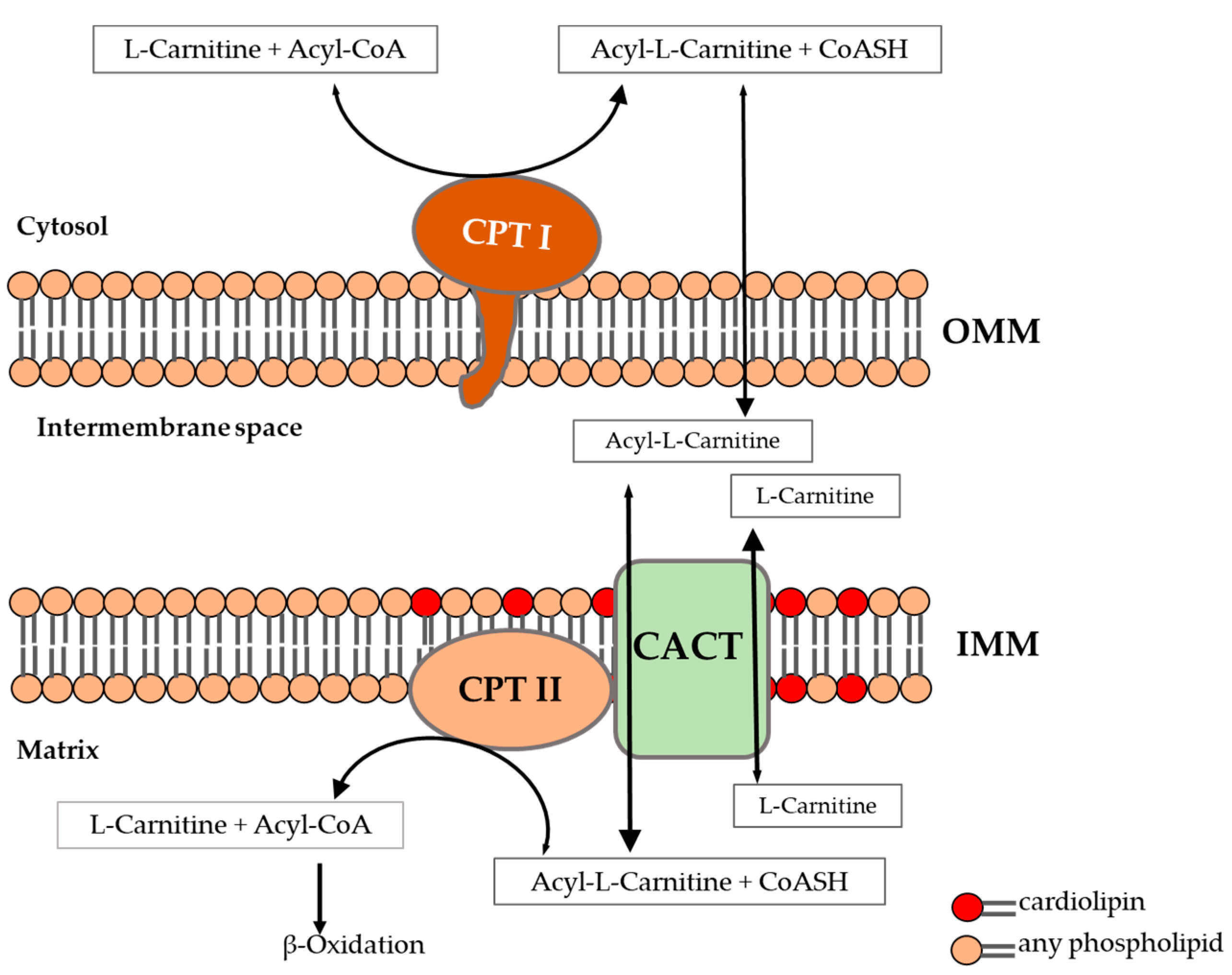
- The Carnitine Shuttle: This is the rate-limiting step! Long-chain fatty acids can't just walk into the mitochondria; they need the Carnitine shuttle (CPT-1 and CPT-2) to get across the inner membrane.
- The Yield: Each cycle of beta-oxidation removes two carbons and produces
1 FADH2,1 NADH, and1 Acetyl-CoA.
Let me find a good visual of that carnitine shuttle for you, as it's a favorite for exam questions.
That diagram perfectly captures the "shuttle" mechanism. Notice how CPT-1 is the gatekeeper on the outer membrane—it's inhibited by Malonyl-CoA, which prevents the body from burning fat while it's trying to synthesize it!
2. Ketogenesis: The Backup Plan
When the liver is flooded with Acetyl-CoA (from massive beta-oxidation during fasting or starvation) and the TCA cycle is maxed out, the liver converts that excess Acetyl-CoA into ketone bodies.
- The Three Ketones: Acetoacetate, 3-hydroxybutyrate, and Acetone (the one that causes "fruity breath").
- The Key Enzyme: HMG-CoA synthase is the rate-limiting enzyme for ketogenesis.
- Clinical Pearl: The liver makes ketones but cannot use them because it lacks the enzyme thiophorase. This ensures ketones are sent out to the brain and muscles during starvation.
3. Dyslipidemias: The Transport Troubles
Dyslipidemias are usually classified by which lipoprotein is elevated. This is high-yield for Step 1 and Step 2.
I've put together a quick comparison table of the primary Familial Dyslipidemias to help you keep them straight:
| Type | Name | Elevated Lipoprotein | Major Finding |
|---|---|---|---|
| I | Hyperchylomicronemia | Chylomicrons | Pancreatitis, Xanthomas, no increased risk for atherosclerosis |
| IIa | Familial Hypercholesterolemia | LDL | Early MI (often <20 yrs), Achilles tendon xanthomas |
| III | Dysbetalipoproteinemia | IDL (Remnants) | Palmar xanthomas, premature atherosclerosis |
| IV | Hypertriglyceridemia | VLDL | Acute pancreatitis, associated with insulin resistance |
That table covers the "big four" you'll see in clinical vignettes. Remember: Type I is about Chylomicrons (think "milky" blood), while Type IIa is the one that leads to very early heart attacks.
To help you lock this in, I've pulled up some high-yield lessons and flashcards on these specific pathways.
📚 Lipid Metabolism Lessons
Those lessons will give you the deep dive on the biochemistry. To make sure you don't forget the key enzymes and clinical findings, here are some flashcards for a quick review session.
🗂️ Lipid Metabolism Flashcards
Tap to study 24 flashcards in the Oncourse app
Those flashcards are perfect for drilling the rate-limiting steps. Remember: HMG-CoA Synthase is for Ketogenesis, while HMG-CoA Reductase is for Cholesterol synthesis—don't let the exam catch you mixing those up!
If you're feeling confident, we could try a quick quiz or even a clinical case to see how these dyslipidemias present in a real patient. What do you think?
Setting up chat...