Informed consent: requirements, exceptions and clinical scenarios
Ah, informed consent! This is a classic "bread and butter" ethics topic for the USMLE. It’s not just about getting a signature on a piece of paper; it’s a process to ensure the patient is making an autonomous, well-informed decision about their care.
To make sure you have the best resources at your fingertips, let me pull up some high-yield lessons on this topic for you.
📚 Informed Consent Lessons
Those lessons cover the core theory, but let's break down the "must-know" components for your exam. For a consent to be valid, it generally needs to meet these four criteria:
- Disclosure: You must explain the diagnosis, the proposed treatment, the risks and benefits, and any alternatives (including doing nothing!).
- Capacity: The patient must have the mental ability to understand the information and make a reasoned decision.
- Voluntariness: The decision must be made without coercion or manipulation.
- Comprehension: The patient actually has to understand what you just said (using a "teach-back" method is a great clinical tip here).
Now, the USMLE loves to test the exceptions—those rare times when you don't need to get full informed consent before acting. I've put together a quick reference table for you.
| Exception | Description | Clinical Scenario Example |
|---|---|---|
| Waiver | Patient explicitly requests not to be informed. | "Doctor, just do what you think is best, I don't want to know the details." |
| Legally Incapacitated | Patient lacks decision-making capacity. | A patient with advanced dementia or someone who is currently unconscious. |
| Emergency | Immediate action is needed to prevent serious harm or death. | An unconscious trauma patient in the ER needing immediate surgery. |
| Therapeutic Privilege | Disclosure would cause severe psychological harm (rarely the right answer on USMLE!). | Withholding a diagnosis because the patient is acutely suicidal and the news might trigger an attempt. |
That table covers the big ones, but the USMLE really loves to throw minors at you. Generally, parents or legal guardians give consent for minors, but there are two major exceptions you must know:
1. The Emancipated Minor
An emancipated minor can consent to all medical procedures as if they were an adult. They are usually:
- Married
- Self-supporting (living on their own)
- In the military
- Parents themselves (in many states)
2. The "Sex, Drugs, and Rock & Roll" Rule
Even if they aren't emancipated, minors can often consent to specific types of care without parental involvement:
- Sexually transmitted infections (testing and treatment)
- Contraception (but not necessarily abortion—that varies by state)
- Pregnancy care (prenatal care)
- Substance abuse treatment
Key Point: If a 16-year-old comes in for an STI test, you do not need to call their parents. In fact, doing so might even be a HIPAA violation!
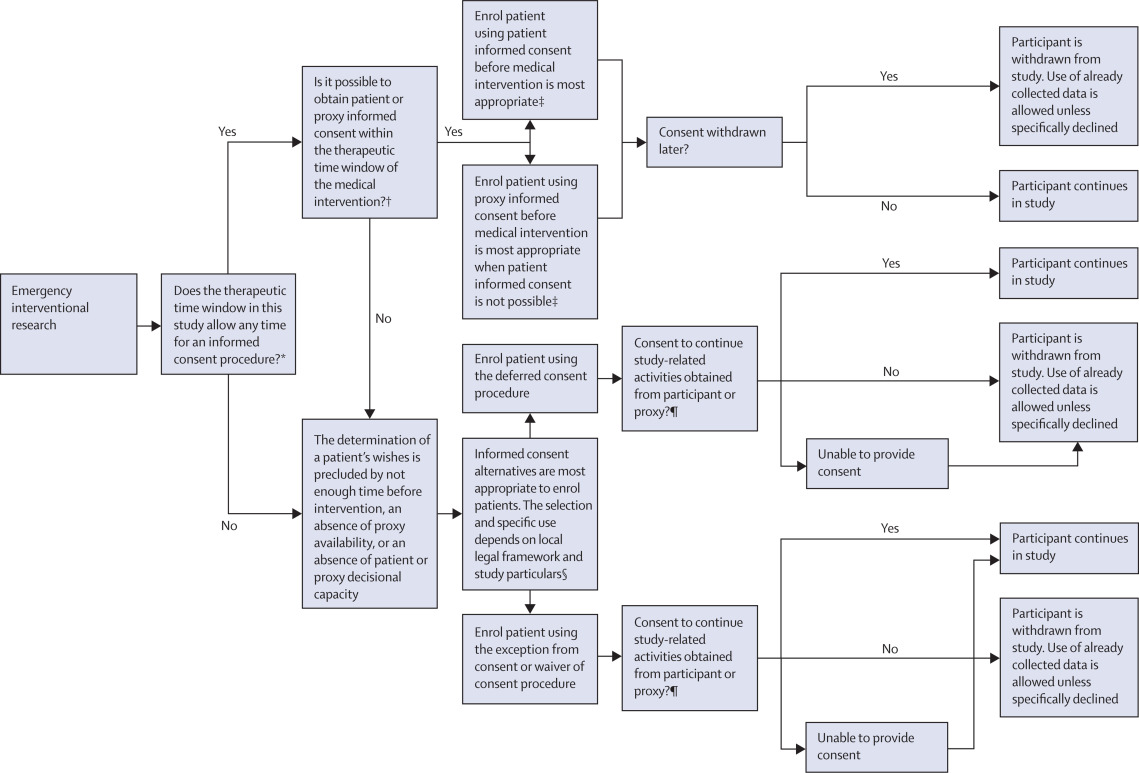
Let me see if I can find a helpful flowchart to help you visualize the decision-making process for consent.
That flowchart is a great way to visualize the decision-making process, especially in those tricky emergency or research situations.
To wrap this up, let's look at a quick clinical scenario:
Scenario: A 17-year-old male comes to the clinic alone asking for a prescription for birth control for his girlfriend. He also mentions he's been feeling depressed.
- Can he consent to his own care? Yes, for the depression (mental health) and potentially for STI screening.
- Can he consent for his girlfriend? No! She must consent for her own care.
- Do you call his parents? No, not without his permission, unless he is an immediate danger to himself or others.
==Remember: Informed consent is about the patient's right to self-determination.==
If you're feeling confident, I can set up a quick quiz to see how you handle some of these ethics board-style questions!
Setting up chat...