HIPAA: key rules, patient privacy and common violations
Ah, HIPAA! The "Health Insurance Portability and Accountability Act" of 1996. It’s basically the "Vegas Rule" of medicine—what happens in the clinic stays in the clinic (mostly). For the USMLE, understanding the nuances of patient privacy isn't just about being a good person; it's high-yield for those ethics questions!
Let me pull up some specific lessons on this so you have the best study material handy.
📚 HIPAA & Ethics Lessons
HIPAA is built on a few core pillars that every med student needs to know. It’s not just about keeping secrets; it’s about standardized protection of Protected Health Information (PHI).
1. The Key Rules
- The Privacy Rule: This is the big one. It sets the standards for who can look at and receive a patient's health info. It applies to "Covered Entities" (doctors, hospitals, insurance companies).
- The Security Rule: This focuses specifically on electronic PHI (ePHI). It ensures that hospitals have the right "locks" on their digital doors (encryption, passwords, etc.).
- The Breach Notification Rule: If PHI is compromised, the entity must notify the affected individuals and, in some cases, the Department of Health and Human Services (HHS).
2. Patient Privacy Rights
Patients have more power than they might realize! Under HIPAA, they have the right to:
- Inspect and copy their medical records.
- Request corrections if they think something is wrong.
- Get an accounting of disclosures (basically a list of who else has seen their info).
- Request restricted communication (e.g., "Don't call my house, only my cell").
3. Common Violations (The "Don'ts")
These are the classic scenarios you'll see in ethics questions:
- Snooping: Looking at the records of a celebrity, a neighbor, or even your own family members without a clinical reason. ==Even if you have access to the system, you don't have the right to look unless you're on the care team.==
- Improper Disposal: Throwing un-shredded patient charts in the regular trash.
- Lost/Stolen Devices: Leaving an unencrypted laptop or thumb drive in a car.
- Social Media Blunders: Posting a "cool X-ray" even if the name is cropped out—if the patient could still be identified (rare condition, specific date/location), it's a violation.
High-Yield Tip: HIPAA doesn't just apply to names. It includes 18 identifiers, including dates (birth, admission), geographic subdivisions smaller than a state, and even full-face photos!
I'm going to find a quick visual summary of these rules to help you visualize how they overlap.
Here's a breakdown of the specific safeguards that healthcare organizations must have in place to stay compliant. It's a great way to see how the "Security Rule" actually works in practice!
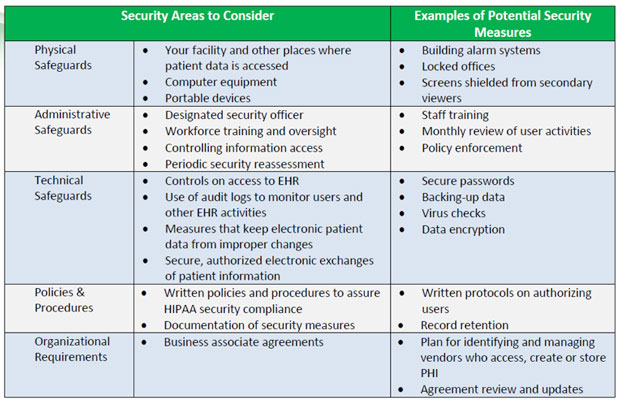
That table really highlights how HIPAA isn't just about "not talking in the elevator"—it's a massive system of administrative, physical, and technical safeguards.
For your exams, keep these "Trick Scenarios" in mind:
- The Family Member: If a patient's spouse calls for results, you cannot give them unless the patient has explicitly authorized it.
- The Police: Generally, you need a warrant or a specific court order to release PHI to law enforcement (there are exceptions for emergencies or specific crimes, but "just asking" isn't enough).
- The "Good Samaritan": If you see a car accident and help out, HIPAA doesn't apply to you as a bystander. But once you're in the hospital as their doctor, the rules are in full effect.
If you're feeling confident, we could try a quick quiz on these ethics scenarios, or I can find some flashcards to help you memorize those 18 identifiers! What do you think?
Setting up chat...