Glycogen storage diseases: types, enzyme defects and clinical features
Glycogen Storage Diseases (GSDs) are a fascinating but complex group of inherited metabolic disorders where the body can't properly store or break down glycogen. This usually leads to an accumulation of glycogen in the liver, muscles, or both, depending on which enzyme is missing.
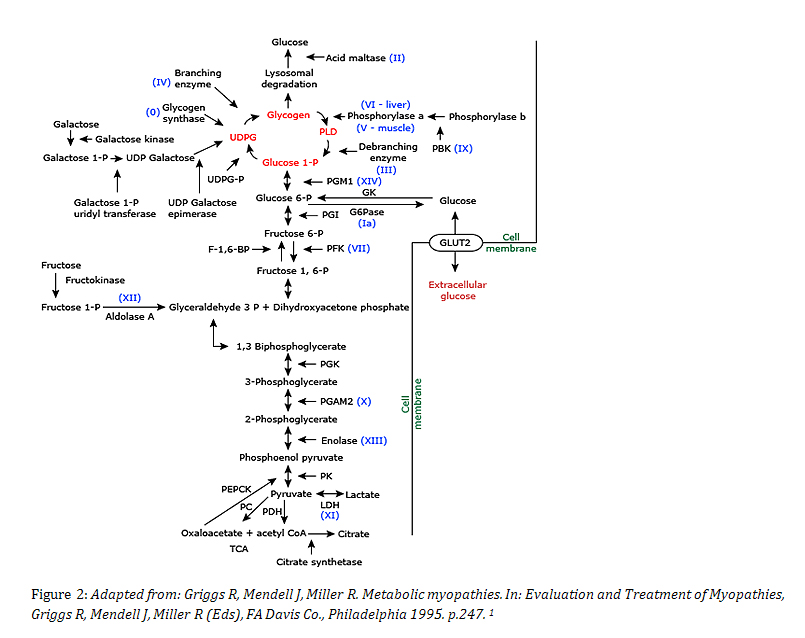
To help you visualize where these enzyme defects occur in the metabolic pathway, let me find a helpful diagram for you.
That diagram gives a great bird's-eye view of how these enzymes fit into the bigger picture of carbohydrate metabolism.
Now, let's break down the most high-yield types you'll need to know for your exams. I've put together a table that summarizes the enzyme defects and the classic clinical "vibe" for each one.
| Type | Name | Enzyme Defect | Key Clinical Features |
|---|---|---|---|
| Type I | Von Gierke | Glucose-6-phosphatase | Severe fasting hypoglycemia, increased blood lactate, hepatomegaly, "doll-like" face, hyperuricemia (gout). |
| Type II | Pompe | Lysosomal $\alpha$-1,4-glucosidase (Acid maltase) | Cardiomegaly, hypertrophic cardiomyopathy, exercise intolerance, and systemic findings leading to early death. "Pompe trashes the Pump (heart)." |
| Type III | Cori | Debranching enzyme ($\alpha$-1,6-glucosidase) | Milder form of Type I with normal lactate levels. Gluconeogenesis is intact. Accumulation of limit dextrin-like structures. |
| Type IV | Andersen | Branching enzyme | Infantile liver cirrhosis, failure to thrive, and hepatosplenomegaly. Often fatal in early childhood. |
| Type V | McArdle | Skeletal muscle glycogen phosphorylase | Muscle cramps, myoglobinuria (red urine) after strenuous exercise, "second-wind" phenomenon. Blood glucose levels are normal. |
| Type VI | Hers | Hepatic glycogen phosphorylase | Similar to Type I but much milder. Hepatomegaly and mild hypoglycemia. |
That table covers the big ones! A quick tip for your exams: Von Gierke (Type I) is the most severe because it blocks the final step of both glycogenolysis and gluconeogenesis, which is why the hypoglycemia is so intense.
To help you lock these in, I've pulled up some detailed lessons and a set of flashcards for you to review.
📚 GSD Lessons
Those resources should give you a solid foundation! Remember, the key to GSDs is often distinguishing between the ones that affect the liver (causing hypoglycemia) and the ones that affect the muscle (causing exercise intolerance).
If you're feeling confident, we could do a quick round of Synapses to see if you can group these diseases by their clinical features. Just let me know!
Setting up chat...