Breast imaging: mammography, BIRADS classification and screening guidelines
Breast imaging is a cornerstone of radiology, especially when it comes to early detection of breast cancer. It’s a topic that’s high-yield for exams and incredibly important in clinical practice.
Let's break this down into the three main areas you mentioned: the screening guidelines, the technical side of mammography, and how we actually report those findings using the BI-RADS system.
1. Screening Guidelines
While different organizations (like the ACR, ACS, and USPSTF) have slightly different takes, the general consensus for an average-risk woman is:
- Start Age: Usually
40-45 years. - Frequency: Annually or biennially (every 2 years).
- Stop Age: Around
75 years, or when life expectancy is < 10 years.
2. Mammography Basics
Mammography uses low-dose X-rays. The two standard views taken for each breast are:
- Craniocaudal (CC): Viewed from above.
- Mediolateral Oblique (MLO): Viewed from the side at an angle (this view captures the most breast tissue, including the "axillary tail of Spence").
3. BI-RADS Classification
The Breast Imaging-Reporting and Data System (BI-RADS) is the universal language radiologists use to communicate risk and management.
I've put together a table for you that simplifies the BI-RADS categories, what they mean, and what the next step should be for the patient.
| BI-RADS Category | Assessment | Management Recommendation | Risk of Malignancy |
|---|---|---|---|
| 0 | Incomplete | Need additional imaging (Ultrasound/Spot views) | N/A |
| 1 | Negative | Routine screening | ~0% |
| 2 | Benign | Routine screening | ~0% |
| 3 | Probably Benign | Short-interval follow-up (6 months) | < 2% |
| 4 | Suspicious | Biopsy should be considered | 2% - 95% |
| 5 | Highly Suggestive of Malignancy | Appropriate action (Biopsy/Surgery) | > 95% |
| 6 | Known Biopsy-Proven Malignancy | Surgical excision when clinically appropriate | 100% |
That table is a lifesaver for exams—especially remembering that BI-RADS 3 requires a 6-month follow-up, while BI-RADS 4 and 5 require tissue diagnosis (biopsy).
To help you visualize what we're looking for on a mammogram, I'll find an image showing the standard views and some common findings like calcifications or masses.
Here is a great example of the standard CC and MLO views. Notice how the MLO view captures more of the tissue toward the chest wall.
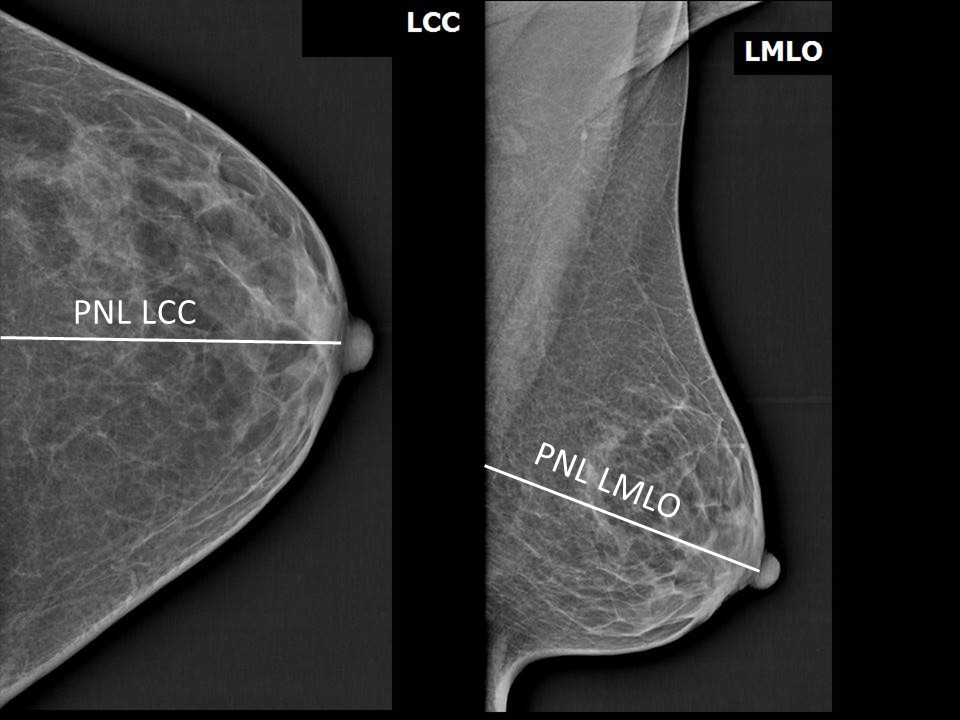
These images show the mix of radiodense (white) fibroglandular tissue and radiolucent (darker) fatty tissue. The Posterior Nipple Line (PNL) is a key landmark used to ensure enough tissue has been captured for a high-quality screen.
To wrap this up, I'll pull some high-yield lessons and flashcards so you can lock in these BI-RADS categories and screening ages!
🗂️ Breast Imaging Flashcards
Tap to study 10 flashcards in the Oncourse app
📚 Breast Imaging Lessons
I've pulled up some high-yield lessons and flashcards to help you master these concepts. The lessons on Cancer Screening Recommendations and Breast Cancer Diagnosis are particularly useful for understanding how imaging fits into the bigger clinical picture.
One final tip: if you see "pleomorphic microcalcifications" or a "spiculated mass" on a mammogram, those are major red flags for malignancy (usually BI-RADS 4 or 5).
Let me know if you'd like to dive deeper into any of these, or if you're ready to test your knowledge with a quick quiz!
Setting up chat...