Acute limb ischaemia: 6 Ps, investigations and revascularisation options
Acute limb ischaemia (ALI) is a true "stop everything and call the vascular registrar" emergency. It's essentially a heart attack of the limb, where a sudden decrease in blood flow threatens its viability.
Since you're prepping for the UKMLA AKT, remember that time is tissue—you've usually got a 6-hour window before irreversible nerve and muscle damage sets in. Let me find a visual to show you what this looks like clinically.
I've found a clinical image that shows the severe end of the spectrum—ischemia leading to necrosis. In the early stages of ALI, the limb might just look very pale or mottled.
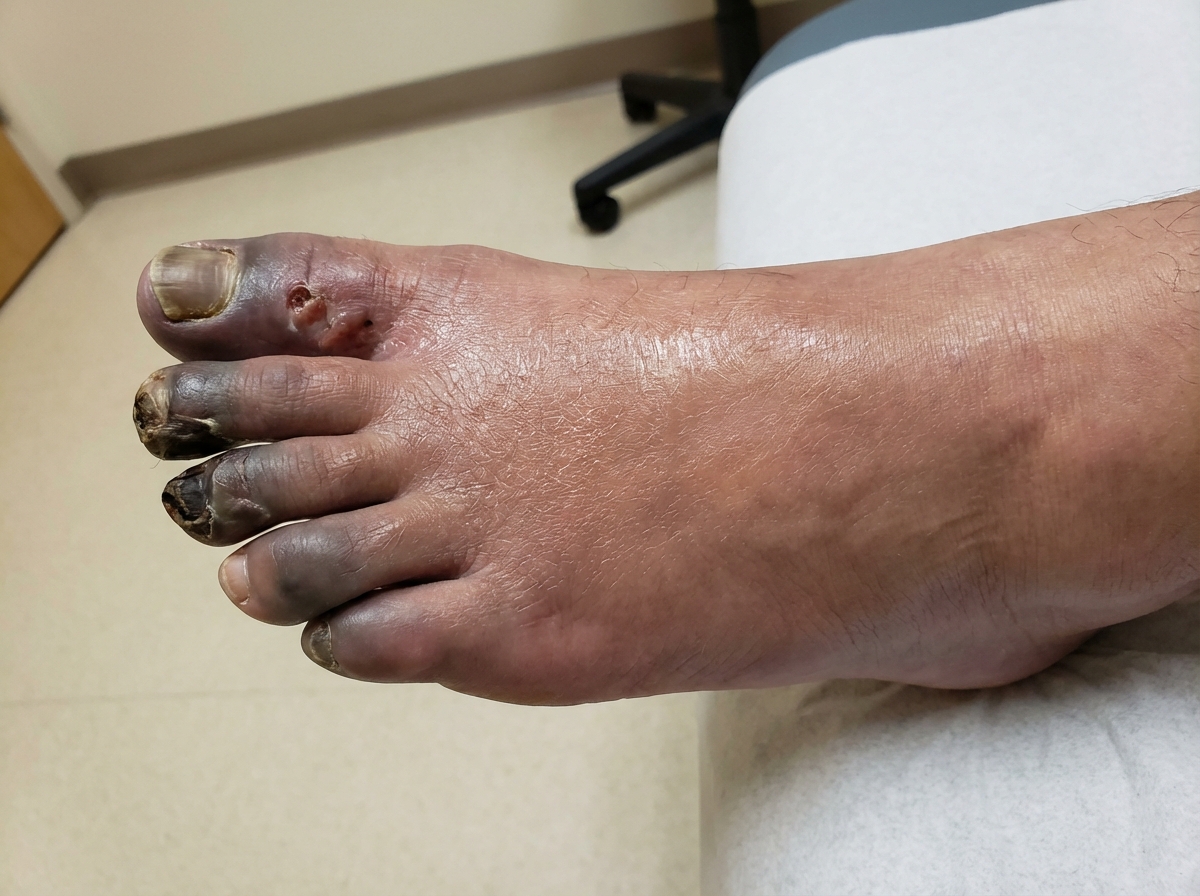
This image shows the progression of ischemia to necrosis. In acute limb ischaemia, the goal is to intervene before it reaches this stage.
The classic clinical presentation is summarized by the 6 Ps. It's vital to recognize that Paresthesia and Paralysis are late signs indicating a "threatened" limb that needs immediate surgical intervention to avoid amputation.
| Feature | Description |
|---|---|
| Pain | Usually sudden, severe, and "out of proportion" to findings initially. |
| Pallor | The limb looks pale, white, or mottled (marble-like). |
| Pulselessness | No palpable pulses. Use a Doppler to check for signals. |
| Paresthesia | Numbness or "pins and needles" (indicates nerve ischemia). |
| Paralysis | Inability to move the limb (indicates muscle ischemia). |
| Perishingly Cold | Also called poikilothermia; the limb matches the room temperature. |
When you suspect ALI, the diagnosis is primarily clinical, but you need to confirm it and plan the surgery quickly.
Investigations
- Bedside:
- Handheld Doppler: To check for arterial and venous signals.
- ECG: Look for Atrial Fibrillation (the most common cause of an embolic ALI).
- Bloods:
- Group and Save/Crossmatch (they're going to theatre!).
- Lactate and CK: To assess for muscle breakdown (rhabdomyolysis) and metabolic acidosis.
- Imaging:
- CT Angiogram (CTA): The gold standard for identifying the site of occlusion and planning revascularisation.
Let me pull up some lessons that cover the diagnostic pathway and the Rutherford classification, which is often tested in the AKT.
Revascularisation Options
Management starts with immediate anticoagulation (usually a bolus of IV Unfractionated Heparin) to prevent the clot from propagating. The definitive treatment depends on whether the cause is an embolus (e.g., from AF) or a thrombus (e.g., on top of pre-existing peripheral arterial disease).
-
Surgical Options:
- Embolectomy: Using a Fogarty catheter to pull the clot out. This is usually the go-to for embolic causes.
- Bypass Surgery: If the vessel is too diseased for a simple embolectomy (thrombotic cause).
- Fasciotomy: Often required after revascularisation to prevent Compartment Syndrome (reperfusion injury).
-
Endovascular Options:
- Intra-arterial Thrombolysis: Infusing "clot-busting" drugs like Alteplase directly into the clot via a catheter. This is usually for "viable" limbs where you have time (Rutherford I or IIa).
- Angioplasty/Stenting: To fix the underlying narrowing after the clot is cleared.
-
Amputation:
- Reserved for Rutherford III (Irreversible) cases where the limb is dead, there is no sensation/movement, and revascularising would cause a fatal systemic "washout" of toxins (potassium, lactate, myoglobin).
Always remember the ABCDE approach first—these patients are often elderly with significant cardiovascular comorbidities!
Setting up chat...