🌊 Why Reroute the Flow?
Urinary diversion creates a new path for urine to exit when the bladder is removed or non-functional. This is necessary to prevent renal damage from obstruction or reflux.
- Bladder Removal (Cystectomy):
- Muscle-invasive bladder cancer (MIBC).
- Refractory non-muscle invasive disease or carcinoma in situ.
- Bladder Dysfunction:
- Neurogenic bladder (e.g., spinal cord injury, spina bifida).
- Severe, intractable incontinence.
- Trauma/Obstruction:
- Pelvic trauma damaging bladder/urethra.
- Irreparable fistulas or strictures.
⭐ The most common indication for urinary diversion in adults is radical cystectomy for muscle-invasive bladder cancer.
🛠️ Anatomy - Building New Plumbing
Urinary diversion re-routes urine flow after cystectomy. The choice of procedure balances surgical complexity with patient quality of life, dexterity, and oncologic goals.
| Procedure Type | Bowel Segment | Continence & Stoma | Key Features & Complications |
|---|---|---|---|
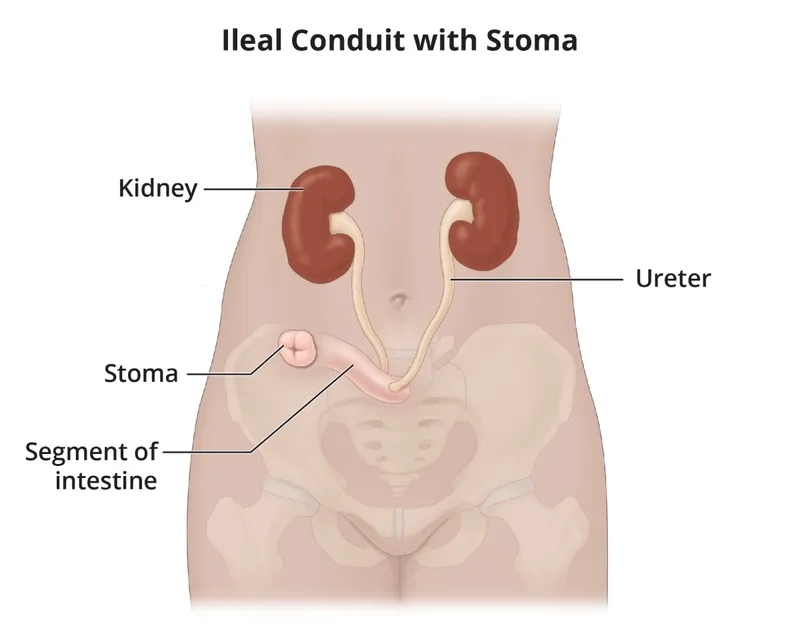
| Ileal Conduit (Bricker) | Distal Ileum | Incontinent; requires external ostomy bag. | Simplest, fastest. Low pressure system. ⚠️ High risk of uretero-ileal stricture, parastomal hernia, pyelonephritis. |
| Indiana Pouch | R. Colon & Terminal Ileum | Continent; self-catheterization via abdominal stoma. | Internal reservoir, no bag. Higher surgical complexity. ⚠️ Risk of stone formation, mucus plugging, difficult catheterization. |
| Orthotopic Neobladder (Studer) | Ileum | Continent; voids via native urethra. | Most "natural" urination. Requires intact urethral sphincter & patient motivation. ⚠️ Risk of nocturnal incontinence, hypercontinence (retention). |
⭐ Metabolic Complications: Using bowel segments for diversion leads to reabsorption of urinary solutes. The most common finding is a non-anion gap, hyperchloremic metabolic acidosis due to intestinal chloride absorption in exchange for bicarbonate.
📌 ACIDosis from Absorption of Chloride and Ileal/colonic Diversion.
⚠️ Complications - When Pipes Go Wrong
-
General Complications:
- Early (<30 days): Infection (UTI, pyelonephritis), anastomotic leak, prolonged ileus, DVT/PE.
- Late (>30 days): Stomal stenosis/hernia, uretero-enteric stricture → hydronephrosis, urolithiasis (struvite, calcium oxalate), vitamin B12 deficiency (if >50 cm of terminal ileum resected).
-
Metabolic Complications (High-Yield):
⭐ The bowel segment used determines the specific metabolic derangement due to reabsorption of urinary solutes.
- Ileum or Colon (Most Common):
- Mechanism: Bowel reabsorbs urinary ammonium ($NH_4^+$) and chloride ($Cl^-$) while secreting bicarbonate ($HCO_3^-$).
- Result: Hyperchloremic, hypokalemic, normal anion gap metabolic acidosis.
- Jejunum (Rarely Used):
- Mechanism: High osmotic load from urine in the jejunal loop causes fluid and electrolyte shifts.
- Result: Hyponatremic, hypochloremic, hyperkalemic metabolic acidosis. 📌 Mnemonic: "J" for "Jumpin' K⁺".
- Ileum or Colon (Most Common):
⚙️ Management - Keeping Systems Go
- Post-Op Monitoring:
- Urine output >0.5 mL/kg/hr.
- Stoma viability: Should be pink and moist.
- Catheters/stents: Ensure patency; typically removed in 2-3 weeks.
- Common Complications:
- Early: UTI, urine leak, ileus.
- Late: Uretero-intestinal stricture, stones, parastomal hernia.
⭐ High-Yield: Ileal conduits can cause a hyperchloremic, non-anion gap metabolic acidosis due to Cl⁻ absorption and HCO₃⁻ secretion by the intestinal mucosa.
- Troubleshooting Low Output:
⚡ Biggest Takeaways
- Radical cystectomy for muscle-invasive bladder cancer is the primary indication for urinary diversion.
- Ileal conduit is the most common incontinent diversion, requiring an external ostomy appliance.
- Orthotopic neobladder is a continent diversion allowing urethral voiding; risks include incontinence and retention.
- Hyperchloremic, non-anion gap metabolic acidosis is a key complication from using bowel segments.
- This occurs via Cl⁻ absorption and HCO₃⁻ secretion by the intestinal mucosa.
- Long-term risks include uretero-intestinal strictures, recurrent UTIs, and vitamin B12 deficiency.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

