Diabetic Nephropathy - Sweet Kidney Trouble
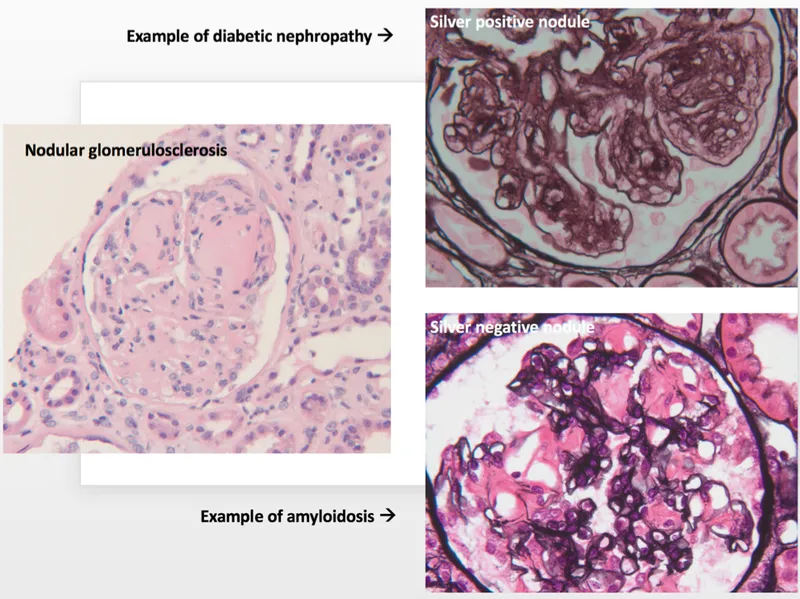
- Patho: Non-enzymatic glycation → hyaline arteriolosclerosis (efferent > afferent) → initial hyperfiltration (↑ GFR). Progresses to glomerular basement membrane (GBM) thickening & mesangial expansion.
- Hallmark: Kimmelstiel-Wilson (KW) nodules (PAS-positive, nodular glomerulosclerosis).
- Clinical: Earliest sign is microalbuminuria (Urine Albumin-to-Creatinine Ratio 30-300 mg/g). Often co-exists with retinopathy.
- Management: Strict glucose (HbA1c <7%) & BP control (<130/80 mmHg).
- First-line: ACE inhibitors or ARBs.
- Add-on: SGLT2 inhibitors (e.g., -gliflozins) for renoprotection.
⭐ ACE inhibitors are first-line to slow nephropathy progression, even in normotensive patients with microalbuminuria, by reducing intraglomerular pressure.
Lupus Nephritis - Wolf in the Filters
- Pathogenesis: Type III hypersensitivity. DNA/anti-dsDNA immune complex deposition in glomeruli.
- Presentation: Varies from asymptomatic hematuria/proteinuria to overt nephritic or nephrotic syndrome.
- Diagnosis: Renal biopsy is the gold standard for staging. Key serologies: ↑ ANA, ↑ anti-dsDNA, ↓ C3/C4.
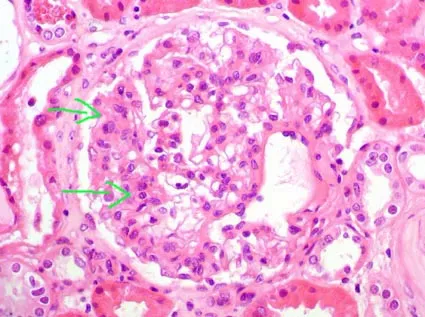
- ISN/RPS Classification & Treatment:
- Class III/IV (Focal/Diffuse Proliferative): Most common & severe. Aggressive therapy with steroids + Mycophenolate Mofetil (MMF) or Cyclophosphamide.
- Class V (Membranous): Presents with nephrotic syndrome. Treat with steroids + MMF.
⭐ Full House Immunofluorescence: On biopsy, staining is positive for IgG, IgA, IgM, C3, and C1q-a classic finding for lupus nephritis.
Amyloid & Paraproteins - Misfolded Mess
- Pathophysiology: Extracellular deposition of insoluble, misfolded fibrillar proteins (β-pleated sheets).
- Amyloidosis:
- AL (Primary): Monoclonal light chain deposition from plasma cell dyscrasias.
- AA (Secondary): Serum Amyloid A deposition from chronic inflammation (e.g., RA, IBD).
- Diagnosis: Congo Red stain shows classic apple-green birefringence under polarized light.
- Presentation: Nephrotic syndrome, enlarged kidneys.
- Light Chain Cast Nephropathy (Myeloma Kidney):
- Filtered monoclonal light chains (Bence-Jones proteins) are directly toxic to tubules, forming obstructing casts.
⭐ Bence-Jones proteins in urine are not detected by standard urine dipstick, which primarily detects albumin. Suspect this in patients with high total protein but negative/trace dipstick protein.

Vasculitis & Infections - Inflammatory Attack
- ANCA-Associated Vasculitis (Pauci-Immune GN): Rapidly progressive GN.
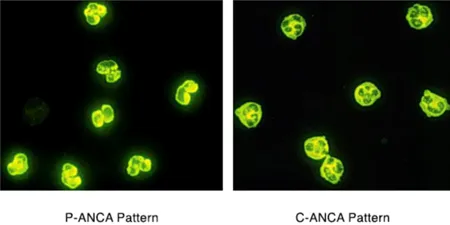
- Granulomatosis with Polyangiitis (GPA): c-ANCA (anti-PR3). Affects sinuses, lungs, kidneys. 📌 C-disease: C-ANCA.
- Microscopic Polyangiitis (MPA): p-ANCA (anti-MPO). Affects lungs, kidneys; no granulomas.
- EGPA (Churg-Strauss): p-ANCA, eosinophilia, asthma.
- Immune Complex GN:
- IgA Vasculitis (HSP): Follows URI. Palpable purpura, arthralgia, abdominal pain.
- Infection-Related GN: Post-strep (PSGN), endocarditis. Features ↓ C3.
⭐ GPA classically presents with a triad: 1) upper respiratory tract disease (sinusitis), 2) lower respiratory tract disease (hemoptysis), and 3) glomerulonephritis.
- Diabetic nephropathy is the leading cause of ESRD; Kimmelstiel-Wilson nodules are pathognomonic.
- Lupus nephritis is characterized by immune complex deposition and a “full-house” immunofluorescence pattern.
- Amyloidosis shows apple-green birefringence with a Congo red stain under polarized light.
- Goodpasture syndrome features anti-GBM antibodies against type IV collagen, creating a linear IF pattern.
- GPA (Wegener’s) is a pauci-immune GN strongly associated with c-ANCA (anti-PR3).
- IgA vasculitis (HSP) typically presents with palpable purpura, arthralgias, and renal involvement.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

