Dietary Management - The Cornerstone Strategy
- Goal: Maintain euglycemia & prevent hypoglycemia.
- Uncooked Cornstarch (UCCS): Cornerstone for GSD I, III, IV, VI, IX.
- Provides slow, steady glucose release.
- Dose: 1.6-2.5 g/kg every 4-6 hours.
- Must be uncooked and mixed in cool water.
- Dietary Restrictions (GSD I):
- Strict avoidance of fructose, sucrose, galactose, & lactose.
- Prevents worsening of lactic acidosis & hyperlipidemia.
- Specific Modifications:
- GSD III: High-protein diet supports gluconeogenesis.
- GSD V (McArdle): Pre-exercise sucrose (~30g) can improve exercise tolerance.
⭐ Uncooked cornstarch (UCCS) therapy revolutionized GSD I management, dramatically improving survival and reducing reliance on continuous nocturnal feedings.
Pharmacotherapy & ERT - The Medical Arsenal
-
GSD I (von Gierke's Disease):
- Allopurinol: Manages hyperuricemia to prevent gout and nephropathy.
- Citrate supplements: Alkalinize urine, reducing risk of uric acid stones.
- Lipid-lowering agents: Statins or fibrates for severe hypertriglyceridemia.
- G-CSF (Filgrastim): For neutropenia and recurrent infections in GSD Ib.
-
GSD II (Pompe Disease):
- Enzyme Replacement Therapy (ERT): The cornerstone of treatment.
- Alglucosidase alfa (Myozyme®, Lumizyme®): A recombinant human acid α-glucosidase (GAA) administered via regular IV infusions.
-
GSD V (McArdle's Disease):
- Pre-exercise sucrose/glucose: Provides an alternative, readily available fuel source.
- Vitamin B6 (Pyridoxine): Cofactor for muscle glycogen phosphorylase; may offer some benefit.
⭐ In Pompe disease, ERT dramatically improves hypertrophic cardiomyopathy and survival in infants, but its efficacy on skeletal muscle function in late-onset disease is more variable.

Monitoring & Complications - The Long-Term View
- Routine Surveillance: Lifelong, multidisciplinary follow-up is key.
- Growth: Serial height/weight, bone age.
- Biochemical: Glucose, lactate, lipid panel, uric acid.
- Liver: Annual LFTs & ultrasound (from age 10 for GSD I).
- Renal: Annual urinalysis (microalbuminuria), creatinine, electrolytes.
- Cardiac: ECG/ECHO for GSD III, IV.
- Long-Term Complications:
- Hepatic: Hepatic adenomas (GSD I) → risk of hemorrhage or malignant transformation to HCC.
- Renal: Nephromegaly, progressive renal insufficiency, Fanconi syndrome.
- Bone: Osteopenia/osteoporosis.
- Hematologic: Anemia, platelet dysfunction.
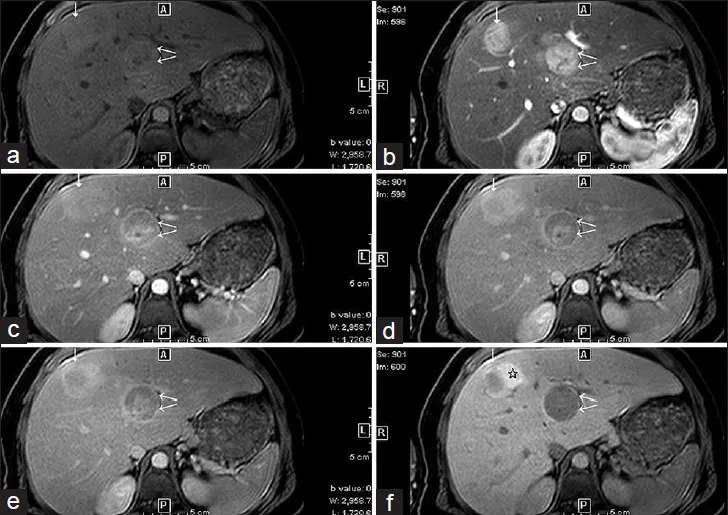
⭐ In GSD I, hepatic adenomas can regress with strict dietary therapy, but the risk of malignant transformation into hepatocellular carcinoma (HCC) remains a lifelong concern.
High‑Yield Points - ⚡ Biggest Takeaways
- The primary goal is to maintain euglycemia and prevent hypoglycemia.
- Management relies on dietary therapy, including frequent small meals and continuous nocturnal feeds.
- Uncooked cornstarch is a cornerstone, providing slow-release glucose, especially overnight.
- In GSD I (von Gierke), it's crucial to avoid fructose and galactose.
- Allopurinol is used to treat the hyperuricemia associated with GSD I.
- For GSD V (McArdle), management includes sucrose before exercise.
- GSD II (Pompe) is uniquely treated with enzyme replacement therapy (ERT).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

