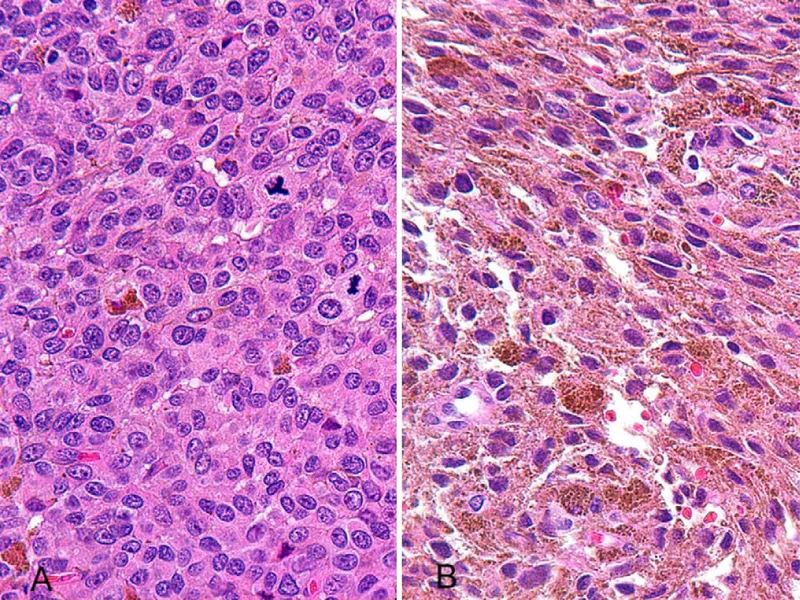
Nevi of Ota and Ito Indian Medical PG Practice Questions and MCQs
Practice Indian Medical PG questions for Nevi of Ota and Ito. These multiple choice questions (MCQs) cover important concepts and help you prepare for your exams.
Nevi of Ota and Ito Indian Medical PG Question 1: A 7-year old boy presents with a right-sided hemangioma and left-sided focal seizures. The most likely diagnosis is:
- A. Incontinentia pigmenti
- B. Sturge-Weber disease (Correct Answer)
- C. Neurofibromatosis
- D. Hypermelanosis of Ito
Nevi of Ota and Ito Explanation: ***Sturge-Weber disease***
- The classic presentation of a **facial hemangioma** (port-wine stain) and **focal seizures** on the contralateral side is highly characteristic of Sturge-Weber disease.
- This neurocutaneous syndrome involves a **leptomeningeal angioma** on the same side as the facial hemangioma, leading to neurological symptoms.
*Incontinentia pigmenti*
- This X-linked dominant disorder primarily affects females and presents with **skin lesions** that evolve through vesicular, verrucous, and hyperpigmented stages, often in a **linear pattern**.
- While it can cause neurological symptoms, a unilateral hemangioma and contralateral focal seizures are not typical.
*Neurofibromatosis*
- Neurofibromatosis Type 1 (NF1) is characterized by **café-au-lait spots**, **axillary/inguinal freckling**, and **neurofibromas**.
- While seizures can occur, the combination of a unilateral hemangioma and contralateral focal seizures is not the hallmark presentation of neurofibromatosis.
*Hypermelanosis of Ito*
- This condition is characterized by **streaky or whorled hyperpigmentation** patterns on the skin, often following Blaschko's lines.
- While neurological abnormalities can be associated, the primary cutaneous manifestation is diffuse hyperpigmentation, not a focal hemangioma.
Nevi of Ota and Ito Indian Medical PG Question 2: What is the most likely diagnosis for a 15 mm hyperpigmented lesion on the shoulder that is enlarging and has hair growing from it?
- A. Melanocytic nevus
- B. Becker nevus (Correct Answer)
- C. Sebaceous nevus
- D. Comedo nevus
Nevi of Ota and Ito Explanation: ***Correct: Becker nevus***
This diagnosis is supported by the description of a **hyperpigmented lesion** that is **enlarging** and has **hair growing from it**, typically appearing during adolescence or young adulthood.
**Becker nevus** often presents as an **irregular, hyperpigmented patch**, usually on the shoulder or upper trunk, and is characteristically associated with **hypertrichosis** (increased terminal hair growth).
The combination of location (shoulder), enlargement, and hair growth in a 15 mm lesion is classic for Becker nevus.
*Incorrect: Melanocytic nevus*
While **melanocytic nevi** are hyperpigmented, they typically do not continue to **enlarge significantly** after childhood and generally do not develop new onset **hypertrichosis** as a primary feature.
The size (15 mm) and progressive growth combined with hair development are more characteristic of a Becker nevus than a common melanocytic nevus.
*Incorrect: Sebaceous nevus*
**Sebaceous nevi** are typically **yellow-orange to tan, waxy plaques**, often on the scalp or face, with a cobblestone or papillomatous texture.
They are not primarily characterized by **hyperpigmentation** and terminal hair growth, but rather by sebaceous gland proliferation.
*Incorrect: Comedo nevus*
A **comedo nevus** presents as a linear or unilateral group of **dilated follicular openings** filled with keratinous material, resembling blackheads.
It is not characterized by diffuse **hyperpigmentation** or the increased terminal hair growth described in this case.
Nevi of Ota and Ito Indian Medical PG Question 3: "Isomorphic response" can be a feature of the following except
- A. Tinea (Correct Answer)
- B. Warts
- C. Molluscum contagiosum
- D. Psoriasis
Nevi of Ota and Ito Explanation: ***Tinea***
- The **isomorphic response (Koebner phenomenon)** refers to the development of new skin lesions in areas of trauma due to an immunological process.
- This phenomenon is **not typically seen in tinea** (fungal infections).
- While tinea can spread to new areas, this occurs through **direct fungal inoculation and contact spread**, not through the true Koebner mechanism.
*Warts*
- **Warts** caused by human papillomavirus (HPV) can exhibit the **isomorphic response**.
- Trauma to the skin can lead to **viral inoculation** in that area, resulting in new wart formation along lines of trauma.
- This is a well-recognized example of Koebner phenomenon in viral infections.
*Molluscum contagiosum*
- **Molluscum contagiosum** (poxvirus infection) can demonstrate the **isomorphic response**.
- **Scratching or rubbing** can spread the virus to new areas through autoinoculation.
- New lesions develop along the lines of trauma, consistent with Koebner phenomenon.
*Psoriasis*
- **Psoriasis** is the **classic and most well-known** condition exhibiting the isomorphic response or Koebner phenomenon.
- New psoriatic plaques appear in areas of **skin injury** (scratches, cuts, burns, surgical incisions, friction).
- Seen in approximately **25-50%** of psoriasis patients.
Nevi of Ota and Ito Indian Medical PG Question 4: Identify the type of skin lesion shown in the image.
- A. Papule
- B. Patch
- C. Nodule
- D. Macule (Correct Answer)
Nevi of Ota and Ito Explanation: ***Macule***
- The lesion shown is a **macule**, characterized by being **flat and circumscribed** with no elevation above the skin surface.
- A macule is defined as a **skin discoloration less than 1 cm in diameter** without any palpable change in texture or thickness.
- Classic examples include **freckles, flat nevi, and café-au-lait spots**.
- The image demonstrates the typical appearance with clear borders and no vertical component.
*Papule*
- A papule is an **elevated, solid lesion less than 1 cm** in diameter.
- Unlike the lesion shown, papules have a **palpable raised component** above the skin surface.
- Examples include acne, warts, and lichen planus.
*Patch*
- A patch is similar to a macule but is **larger than 1 cm in diameter**.
- While also flat, the size criterion differentiates it from a macule.
- Examples include vitiligo patches and large birthmarks.
*Nodule*
- A nodule is a **solid, elevated lesion greater than 1 cm** that extends into deeper skin layers.
- It has both elevation and depth, unlike the flat lesion shown.
- Examples include dermatofibromas, lipomas, and some cysts.
Nevi of Ota and Ito Indian Medical PG Question 5: A child presents with grouped vesicles on the lips. What is the bedside investigation that you would like to do?
- A. Wood's lamp
- B. Slit skin smear
- C. Tzanck smear (Correct Answer)
- D. KOH
Nevi of Ota and Ito Explanation: ***Tzanck smear***
- A **Tzanck smear** is a rapid bedside test that can identify **multinucleated giant cells**, which are seen in herpes simplex virus infections.
- The presence of **grouped vesicles on the lips** is highly suggestive of **herpes labialis** (HSV-1), which is primarily a **clinical diagnosis**.
- Among the options provided, Tzanck smear is the only relevant bedside investigation, though it has **limited sensitivity and specificity** and **cannot distinguish between HSV and VZV**.
- In modern practice, **PCR or direct immunofluorescence** are preferred when laboratory confirmation is needed, but Tzanck smear remains a low-cost option in resource-limited settings.
*Wood's lamp*
- A Wood's lamp uses **ultraviolet light** to detect certain fungal or bacterial infections by revealing characteristic fluorescence.
- It is useful for conditions like **tinea capitis** (green fluorescence) and **erythrasma** (coral-red fluorescence), but has no role in diagnosing viral vesicular lesions.
*Slit skin smear*
- A **slit skin smear** is used to detect **acid-fast bacilli** in the diagnosis of **leprosy**.
- It is not indicated for vesicular lesions and is irrelevant to herpes simplex infection.
*KOH*
- A **KOH (potassium hydroxide) mount** is used to diagnose **fungal infections** by dissolving keratinocytes and revealing fungal hyphae or spores.
- It has no utility in diagnosing viral infections such as herpes simplex.
Nevi of Ota and Ito Indian Medical PG Question 6: What is the most common association with Acanthosis nigricans?
- A. Hypertension
- B. Diabetes Mellitus
- C. Obesity (Correct Answer)
- D. Hypothyroidism
Nevi of Ota and Ito Explanation: **Explanation:**
**Acanthosis Nigricans (AN)** is a common dermatological condition characterized by hyperpigmented, velvety plaques, typically found in intertriginous areas like the axilla and neck.
**Why Obesity is the Correct Answer:**
Obesity is the **most common** association and cause of Acanthosis Nigricans (Pseudo-acanthosis nigricans). The underlying mechanism is **Insulin Resistance**. In obese individuals, high levels of circulating insulin bind to **Insulin-like Growth Factor-1 (IGF-1) receptors** on keratinocytes and fibroblasts. This stimulates excessive proliferation of these cells, leading to the characteristic epidermal thickening and hyperpigmentation.
**Analysis of Incorrect Options:**
* **Diabetes Mellitus (B):** While AN is a strong cutaneous marker for Type 2 Diabetes, it usually precedes the clinical onset of diabetes. Obesity remains the primary driver and more frequent association.
* **Hypertension (A) & Hypothyroidism (D):** These are often part of the "Metabolic Syndrome" or associated endocrinopathies (like PCOS), but they are not the primary or most common cause of the skin changes seen in AN.
**High-Yield Clinical Pearls for NEET-PG:**
* **Malignant Acanthosis Nigricans:** If AN appears suddenly, is very extensive, or involves the palms (**Tripe Palms**) and oral mucosa, it is highly suggestive of internal malignancy, most commonly **Gastric Adenocarcinoma**.
* **Histopathology:** Shows hyperkeratosis and papillomatosis. Note that "acanthosis" (thickening of the stratum spinosum) is actually minimal despite the name.
* **Common Sites:** Neck (most common), axilla, groins, and knuckles.
* **Drug-induced AN:** Can be caused by Nicotinic acid, systemic corticosteroids, and OCPs.
Nevi of Ota and Ito Indian Medical PG Question 7: An increased incidence of vitiligo is found in association with which of the following conditions?
- A. Psoriasis
- B. Nutritional deficiency
- C. Old age
- D. Diabetes mellitus (Correct Answer)
Nevi of Ota and Ito Explanation: **Explanation:**
**Vitiligo** is a chronic autoimmune skin disorder characterized by the destruction of melanocytes. The key medical concept to understand for NEET-PG is that vitiligo is frequently associated with other **organ-specific autoimmune disorders**.
**1. Why Diabetes Mellitus is correct:**
Vitiligo is part of a spectrum of autoimmune polyendocrine syndromes. There is a statistically significant association between vitiligo and **Type 1 Diabetes Mellitus** (and occasionally Type 2) due to shared genetic susceptibility and autoimmune pathways. Other common associations include:
* **Thyroid disorders** (most common association, especially Hashimoto’s thyroiditis).
* Pernicious anemia.
* Addison’s disease.
* Alopecia areata.
**2. Why the other options are incorrect:**
* **Psoriasis (A):** While both are T-cell mediated inflammatory skin diseases, psoriasis is not classically associated with the systemic autoimmune cluster seen in vitiligo.
* **Nutritional deficiency (B):** Vitiligo is an autoimmune process, not a nutritional one. While some studies suggest low Vitamin B12 or Vitamin D levels in vitiligo patients, deficiency is not a causative or strongly associated factor.
* **Old age (C):** Vitiligo typically has an early onset; 50% of cases begin before age 20. It is not a degenerative condition of aging.
**High-Yield Clinical Pearls for NEET-PG:**
* **Most common association:** Thyroid dysfunction (check TSH in vitiligo patients).
* **Koebner Phenomenon:** Vitiligo shows positivity (depigmentation at sites of trauma).
* **Vogt-Koyanagi-Harada Syndrome:** Vitiligo associated with uveitis, meningitis, and auditory symptoms.
* **Treatment of choice:** Narrowband UVB (NB-UVB) is the gold standard for generalized vitiligo.
Nevi of Ota and Ito Indian Medical PG Question 8: A 'silver tattoo' is due to deposition of which substance in the oral mucosa?
- A. Silver amalgam in mucosa (Correct Answer)
- B. Silver amalgam in bone
- C. Silver amalgam in dentin
- D. Silver amalgam in enamel
Nevi of Ota and Ito Explanation: **Explanation:**
The correct answer is **A. Silver amalgam in mucosa.**
An **amalgam tattoo** (often referred to as a "silver tattoo") is a common iatrogenic lesion caused by the accidental implantation of dental restorative material into the oral soft tissues. This typically occurs during the placement or removal of silver amalgam fillings, or during endodontic procedures (like an apicoectomy).
**Why Option A is correct:**
The "tattoo" effect occurs when silver particles from the amalgam are embedded into the **lamina propria** of the oral mucosa. Once in the tissue, the silver salts stain the reticulin fibers of the basement membrane and blood vessel walls, resulting in a localized, asymptomatic, slate-grey to bluish-black macule.
**Why other options are incorrect:**
* **Options B, C, and D:** While amalgam is used to restore dentin and enamel, and may occasionally come into contact with bone during surgery, the clinical term "silver tattoo" specifically refers to the visible **mucosal pigmentation**. Pigmentation within the hard tissues (bone, dentin, enamel) does not manifest as a "tattoo" because these tissues are not superficial or translucent enough to show the characteristic localized blue-grey discoloration seen on the surface of the gums or cheeks.
**High-Yield Clinical Pearls for NEET-PG:**
* **Most Common Site:** The gingiva and alveolar mucosa are the most frequent sites.
* **Radiology:** On a periapical X-ray, radiopaque (white) speckles may be visible at the site of the tattoo if the fragments are large enough.
* **Differential Diagnosis:** It is crucial to differentiate an amalgam tattoo from a **malignant melanoma**. If the lesion is expanding or lacks a history of dental work, a biopsy is mandatory.
* **Histology:** Characterized by black, granular deposits along collagen fibers and around small blood vessels.
Nevi of Ota and Ito Indian Medical PG Question 9: Fine reticular pigmentation with palmar pits is seen in which of the following conditions?
- A. Dowling-Degos disease (Correct Answer)
- B. Rothmund-Thomson syndrome
- C. Cockayne syndrome
- D. Bloom syndrome
Nevi of Ota and Ito Explanation: **Explanation:**
**Dowling-Degos Disease (DDD)** is an autosomal dominant genodermatosis characterized by a defect in the **KRT5 gene** (Keratin 5). The hallmark clinical presentation is **fine, reticulate (lace-like) hyperpigmentation** that typically begins in the axillae and groin and later spreads to other flexures. A diagnostic clinical clue for DDD is the presence of **pitted perioral scars** and **comedo-like lesions** (dark keratinous plugs) on the neck and back, along with **palmar pits**. Histologically, it shows "antler-like" or "filiform" downward extensions of the epidermis with hyperpigmentation of the tips.
**Why the other options are incorrect:**
* **Rothmund-Thomson Syndrome:** Characterized by **poikiloderma** (atrophy, telangiectasia, and mottled pigmentation) starting on the cheeks, associated with juvenile cataracts and skeletal abnormalities.
* **Cockayne Syndrome:** A DNA repair defect presenting with **cachectic dwarfism**, "bird-like" facies, and extreme photosensitivity, but lacks reticulate pigmentation or palmar pits.
* **Bloom Syndrome:** Features a characteristic **malar "butterfly" rash** (photosensitive telangiectatic erythema) and proportional short stature due to chromosomal instability (BLM gene).
**High-Yield Clinical Pearls for NEET-PG:**
* **Reticulate Pigmentation Spectrum:** If the question mentions reticulate pigmentation *plus* hypopigmented macules and nail dystrophy, think of **Dyskeratosis Congenita**.
* **Kitamura Reticulate Acropigmentation:** Similar to DDD but involves the **dorsum of hands and feet** (acral distribution) and is associated with the *ADAM10* gene.
* **Palmar Pits Triad:** Always remember the three major causes of palmar pits: **Dowling-Degos Disease**, **Gorlin Syndrome** (Basal Cell Nevus Syndrome), and **Darier Disease**.
Nevi of Ota and Ito Indian Medical PG Question 10: A child presents with a 2x2 cm depigmented macule with irregular margins over the forehead and glabella. There is a white forelock over the forehead since birth. What is the most likely diagnosis?
- A. Piebaldism (Correct Answer)
- B. Dermatitis
- C. Vitiligo
- D. Nevus of Ito
Nevi of Ota and Ito Explanation: **Explanation:**
The clinical presentation of a **congenital depigmented macule** associated with a **white forelock (poliosis)** is the classic hallmark of **Piebaldism**.
**1. Why Piebaldism is Correct:**
Piebaldism is an autosomal dominant disorder caused by a mutation in the **KIT proto-oncogene**, which leads to defective migration and differentiation of melanoblasts from the neural crest to the skin during embryogenesis. Key features include:
* **Congenital presence:** Present since birth (unlike vitiligo).
* **White Forelock:** Occurs in 80-90% of cases, typically in a triangular or diamond shape.
* **Distribution:** Depigmented patches usually involve the central forehead, trunk, and extremities, often with "islands" of normal pigmentation within the patches.
**2. Why Other Options are Incorrect:**
* **Dermatitis:** This is an inflammatory skin condition characterized by erythema, scaling, and itching. While post-inflammatory hypopigmentation can occur, it is not congenital and does not present with a white forelock.
* **Vitiligo:** This is an acquired autoimmune destruction of melanocytes. It typically appears later in life, is progressive, and lacks the stable, congenital pattern seen here.
* **Nevus of Ito:** This is a dermal melanocytosis presenting as a **bluish-gray hyperpigmented** patch (not depigmented) along the distribution of the posterior supraclavicular and lateral cutaneous brachial nerves.
**Clinical Pearls for NEET-PG:**
* **Differential Diagnosis:** Always differentiate Piebaldism from **Waardenburg Syndrome**, which also features a white forelock but includes systemic findings like sensorineural deafness and heterochromia iridis.
* **Stability:** Unlike Vitiligo, the patches in Piebaldism are stable and do not change significantly in size throughout life.
* **Histopathology:** Shows a complete absence of melanocytes in the depigmented areas.
More Nevi of Ota and Ito Indian Medical PG questions available in the OnCourse app. Practice MCQs, flashcards, and get detailed explanations.
 and Nevus of Ito (shoulder/neck) showing characteristic blue-gray pigmentation) G
and Nevus of Ito (shoulder/neck) showing characteristic blue-gray pigmentation) G