Phases of wound healing — MCQs

A 30-year-old man comes to the physician for a follow-up examination 1 month after sustaining a chemical burn over the dorsum of his right hand and forearm. Physical examination shows hyperextension of the hand at the wrist. The skin over the dorsum of the wrist is tense and there is a thick, epithelialized scar. Range of motion of the right wrist is restricted. This patient's contracture is most likely due to activity of which of the following cells?
A 55-year-old African American female presents to her breast surgeon for a six-month follow-up visit after undergoing a modified radical mastectomy for invasive ductal carcinoma of the left breast. She reports that she feels well and her pain has been well controlled with ibuprofen. However, she is frustrated that her incisional scar is much larger than she expected. She denies any pain or pruritus associated with the scar. Her past medical history is notable for systemic lupus erythematosus and multiple dermatofibromas on her lower extremities. She has had no other surgeries. She currently takes hydroxychloroquine. On examination, a raised hyperpigmented rubbery scar is noted at the inferior border of the left breast. It appears to have extended beyond the boundaries of the initial incision. Left arm range of motion is limited due to pain at the incisional site. Abnormal deposition of which of the following molecules is most likely responsible for the appearance of this patient’s scar?
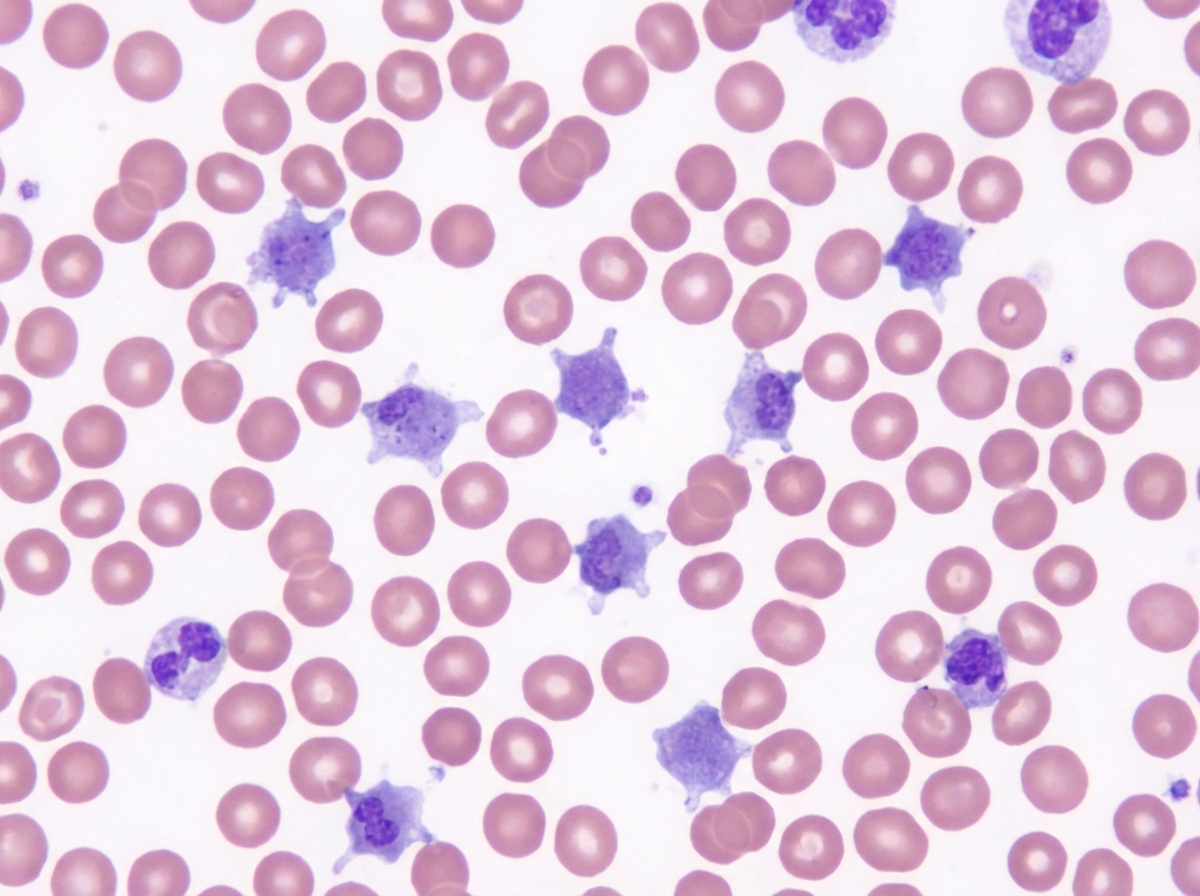
A 3-week-old boy is brought to the pediatrician by his parents for a circumcision. The circumcision was uncomplicated; however, after a few hours, the diaper contained blood, and the bleeding has not subsided. A complete blood count was ordered, which was significant for a platelet count of 70,000/mm3. On peripheral blood smear, the following was noted (figure A). The prothrombin time was 12 seconds, partial thromboplastin time was 32 seconds, and bleeding time was 13 minutes. On platelet aggregation studies, there was no response with ristocetin. This result was not corrected with the addition of normal plasma. There was a normal aggregation response with the addition of ADP. Which of the following is most likely true of this patient's underlying disease?
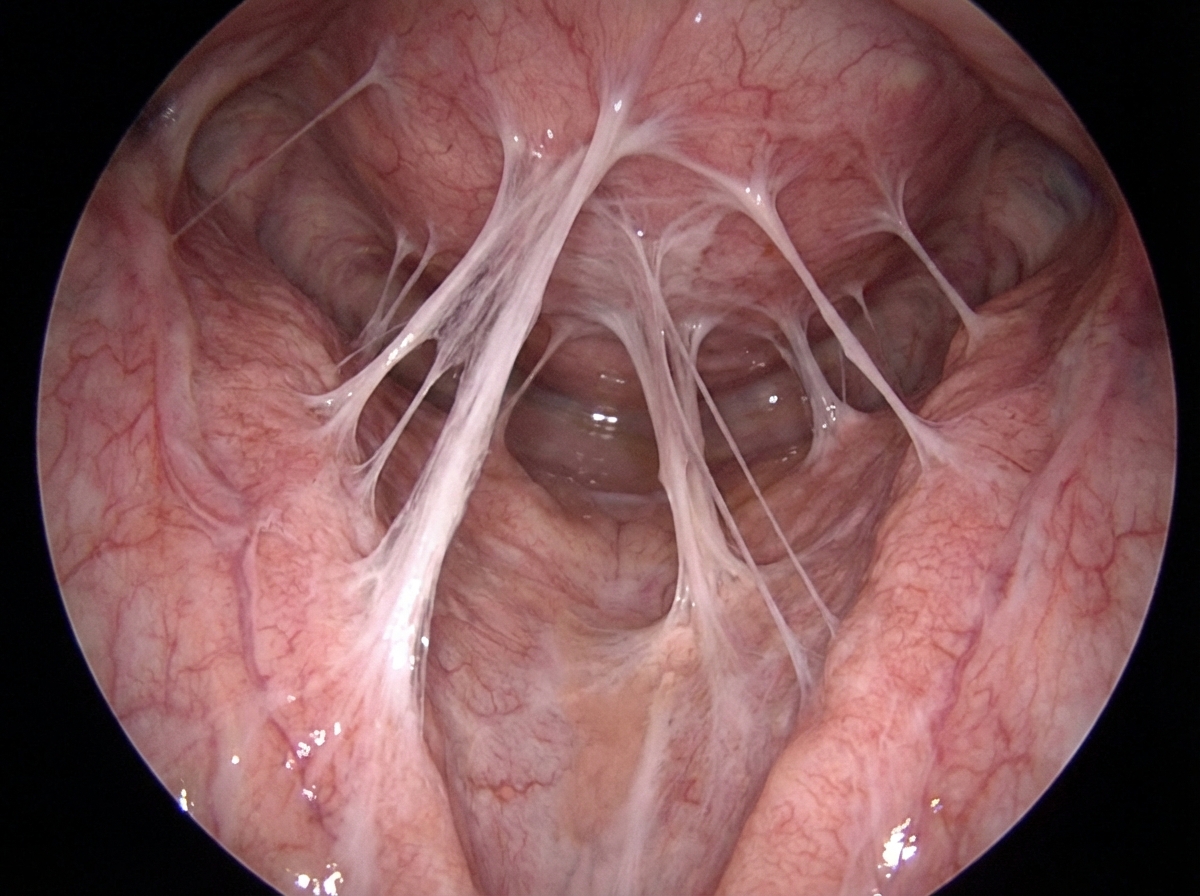
A 28-year-old woman and her husband are admitted to the office due to difficulties conceiving a child for the past year. Her menarche was at the age of 15 years, and her periods have been regular since then. Her medical history is positive for an abortion with curettage 5 years ago. A spermogram on the partner is performed, and it shows motile sperm cells. An ultrasound is performed on the patient and it is unremarkable. The laboratory results show that the FSH, LH, TSH, and prolactin levels are within normal ranges. A hysteroscopy is additionally performed and multiple adhesions are found in the uterus (refer to the image). Which of the following is the most likely composition of the scar tissue present in the uterus?
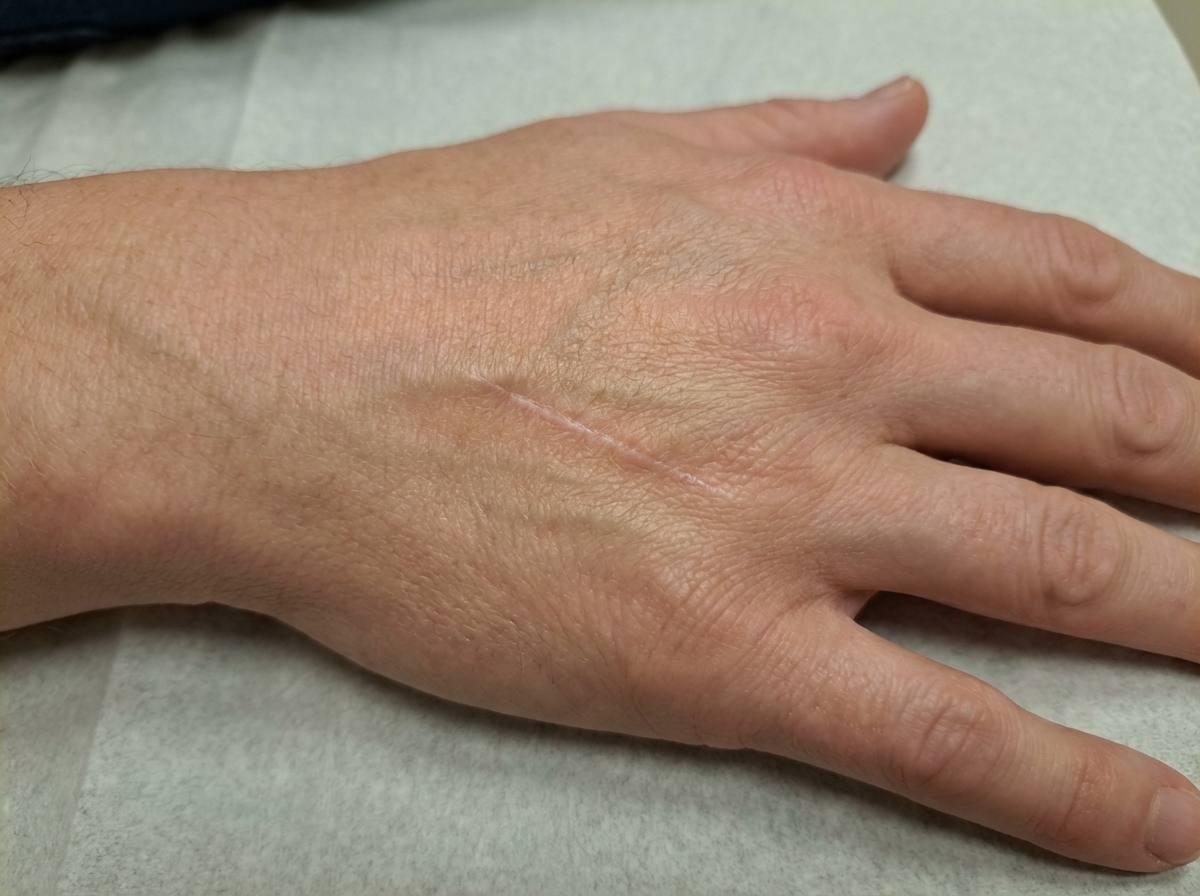
A 16-year-old boy presents to the emergency department after a skateboarding accident. He fell on a broken bottle and received a 4 cm wound on the dorsal aspect of his left hand. His vitals are stable and he was evaluated by the surgeon on call who determined that suturing was not required. After several weeks the wound has almost completely healed (see image). Which of the following is the correct description of this patient's wound before healing?
An investigator is studying the structural integrity of collagen. Human fibroblasts are cultured on a medium and different enzymes are applied. One of the cultures is supplemented with an enzyme that inhibits lysyl oxidase, preventing the formation of covalent cross-links between collagen α-chains. Which of the following processes is most likely to be impaired as a result?
A 16-year-old male presents to the emergency department with a hematoma after falling during gym class. He claims that he has a history of prolonged nosebleeds and bruising/bleeding after minor injuries. Physical exam is unrevealing other than the hematoma. Labs are obtained showing an increased bleeding time and an abnormal ristocetin cofactor assay. Coagulation assays reveal an increased partial thromboplastin time (PTT) but a normal prothrombin time (PT). The patient is given desmopressin and is asked to avoid aspirin. Which of the following findings is most likely directly involved in the etiology of this patient's presentation?
A 45-year-old man comes to his primary care provider for a routine visit. The patient mentions that while he was cooking 5 days ago, he accidentally cut himself with a meat cleaver and lost the skin at the tip of his finger. After applying pressure and ice, the bleeding stopped and he did not seek treatment. The patient is otherwise healthy and does not take any daily medications. The patient’s temperature is 98.2°F (36.8°C), blood pressure is 114/72 mmHg, pulse is 60/min, and respirations are 12/min. On exam, the patient demonstrates a 0.5 x 0.3 cm wound on the tip of his left third finger. No bone is involved, and the wound is red, soft, and painless. There are no signs of infection. Which of the following can be expected on histopathological examination of the wounded area?
A 38-year-old, working, first-time mother brings her 9-month-old male infant to the pediatrician for "wounds that simply won't heal" and bleeding gums. She exclaims, "I have been extra careful with him making sure to not let him get dirty, I boil his baby formula for 15 minutes each morning before I leave for work to give to the caregiver, and he has gotten all of his vaccinations." This infant is deficient in a molecule that is also an essential co-factor for which of the following reactions?
A previously healthy 5-year-old boy is brought to the emergency department 15 minutes after sustaining an injury to his right hand. His mother says that she was cleaning the bathroom when he accidentally knocked over the drain cleaner bottle and spilled the liquid onto his hand. On arrival, he is crying and holding his right hand in a flexed position. His temperature is 37.7°C (99.8°F), pulse is 105/min, respirations are 25/min, and blood pressure is 105/65 mm Hg. Examination of the right hand shows a 4 x 4 cm area of reddened, blistered skin. The area is very tender to light touch. His ability to flex and extend the right hand are diminished. Radial pulses are palpable. Capillary refill time is less than 3 seconds. Which of the following is the most appropriate next step in management?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
