Vascular Surgery — MCQs

On this page
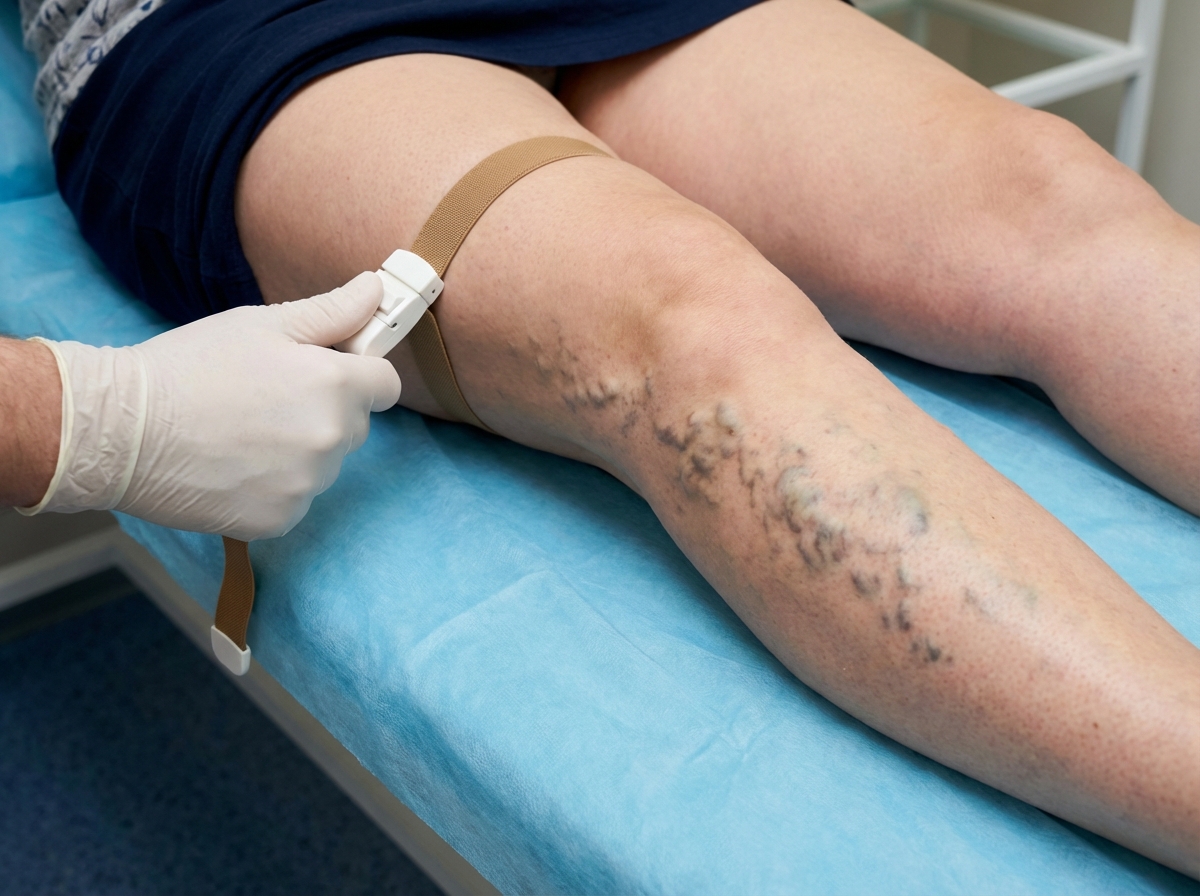
A patient complains of leg pain along with cramps and pruritus. On physical examination, visible limb veins are noticed. For further evaluation a test is conducted which is shown in the image. All are the possible sites for performing this test except:
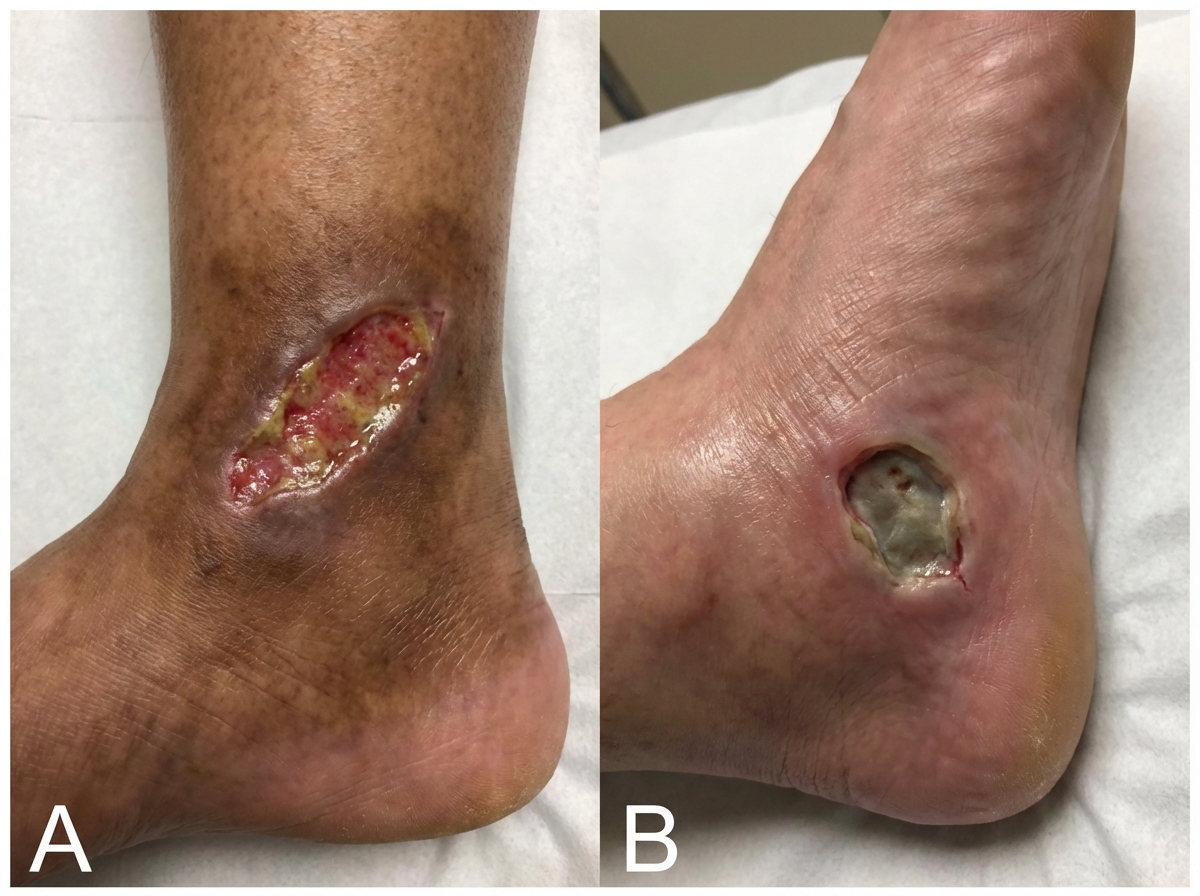
Identify the ulcer types shown in images A and B.
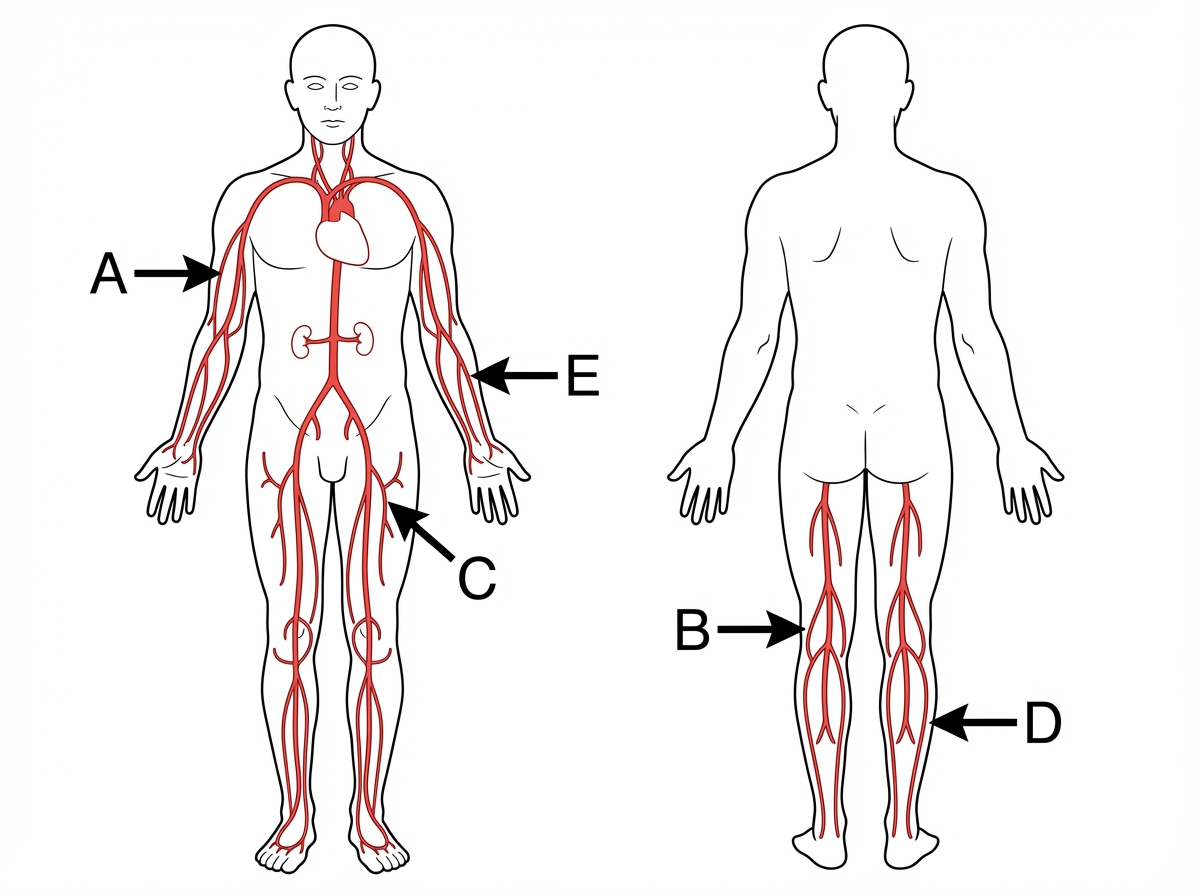
Which is the most common site of peripheral aneurysm?
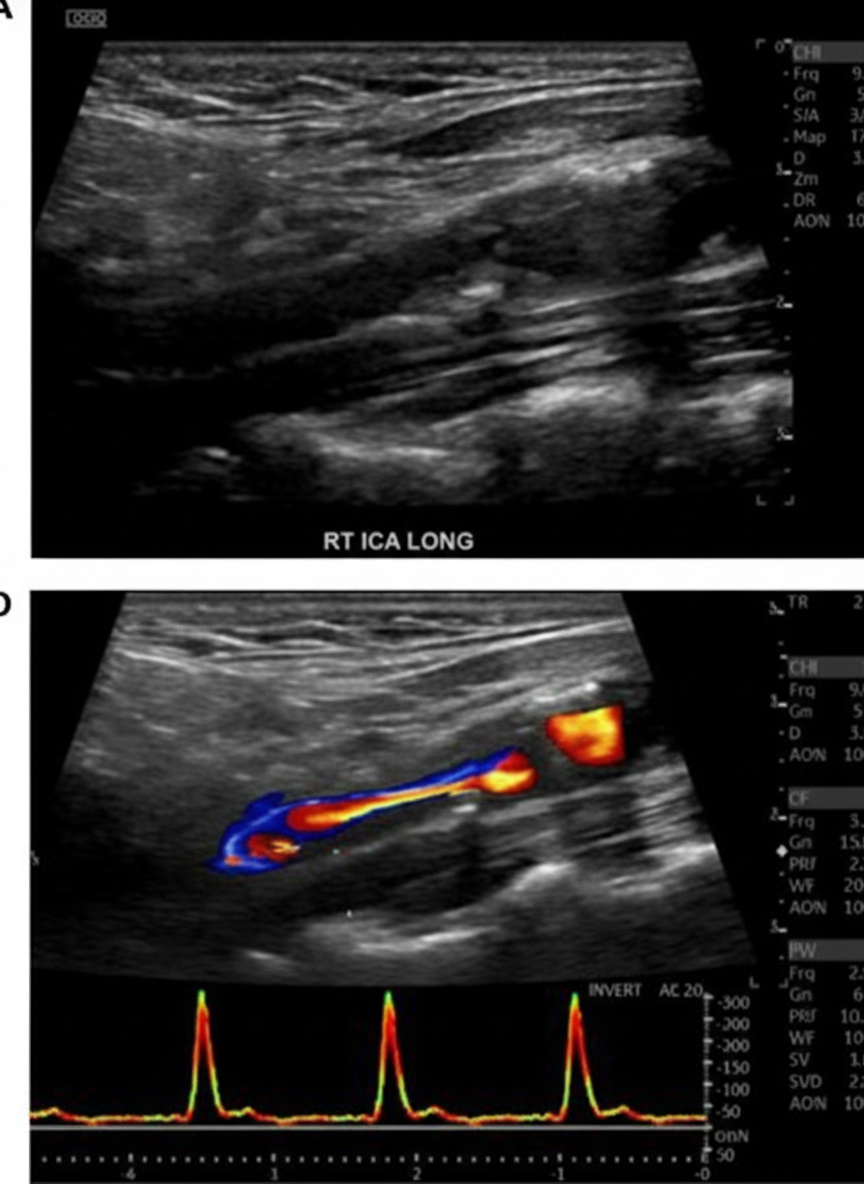
A patient has developed a disease shown below after receiving neck irradiation. Which is the best management for the patient?
Practice by Chapter
Abdominal aortic aneurysm repair
Practice Questions
Acute limb ischemia management
Practice Questions
Aortic dissection management
Practice Questions
Bypass grafting techniques and materials
Practice Questions
Carotid endarterectomy indications and technique
Practice Questions
Compartment syndrome diagnosis and fasciotomy
Practice Questions
Dialysis access procedures and complications
Practice Questions
Endovascular procedures overview
Practice Questions
Peripheral arterial disease diagnosis and management
Practice Questions
Thoracic aortic aneurysm management
Practice Questions
Thromboembolectomy procedures
Practice Questions
Vascular trauma management
Practice Questions
Venous insufficiency and varicose vein treatment
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
