Trauma/Emergencies — MCQs

On this page
A 33-year-old woman is brought to the emergency department 15 minutes after being stabbed in the chest with a screwdriver. Her pulse is 110/min, respirations are 22/min, and blood pressure is 90/65 mm Hg. Examination shows a 5-cm deep stab wound at the upper border of the 8th rib in the left midaxillary line. Which of the following structures is most likely to be injured in this patient?
A 65-year-old woman presents to her primary care provider for shoulder pain. She reports that she initially thought the pain was due to "sleeping funny" on the arm, but that the pain has now lasted for 4 weeks. She denies trauma to the joint and says that the pain is worse when reaching overhead to retrieve things from her kitchen cabinets. On physical exam, the patient's shoulders are symmetric, and the right lateral shoulder is tender to palpation. The shoulder has full passive and active range of motion, although pain is reproduced on active abduction of the right arm above 90 degrees. Pain is also reproduced on passively internally rotating and then lifting the shoulder. The patient is able to resist elbow flexion without pain, and she otherwise has 5/5 strength. Which of the following is the most likely diagnosis?
A 62-year-old man comes to the physician for the evaluation of nocturia and a weak urinary stream. These symptoms began 1 year ago, but have progressively worsened over the past 6 months. He now wakes up 3–5 times every night to urinate. He has hypertension treated with hydrochlorothiazide and lisinopril. The patient has smoked a half-pack of cigarettes daily for the past 30 years. He appears well. His temperature is 37.3°C (99.1°F), pulse is 77/min, and blood pressure is 128/77 mm Hg. Cardiopulmonary examination shows no abnormalities. His abdomen is soft and nontender. Digital rectal examination shows a diffusely enlarged prostate with a firm nodule in the right posterior lobe. Urinalysis is within normal limits. Prostate-specific antigen (PSA) level is 6.5 ng/mL (N = 0–4). Which of the following is the most appropriate next step in management?
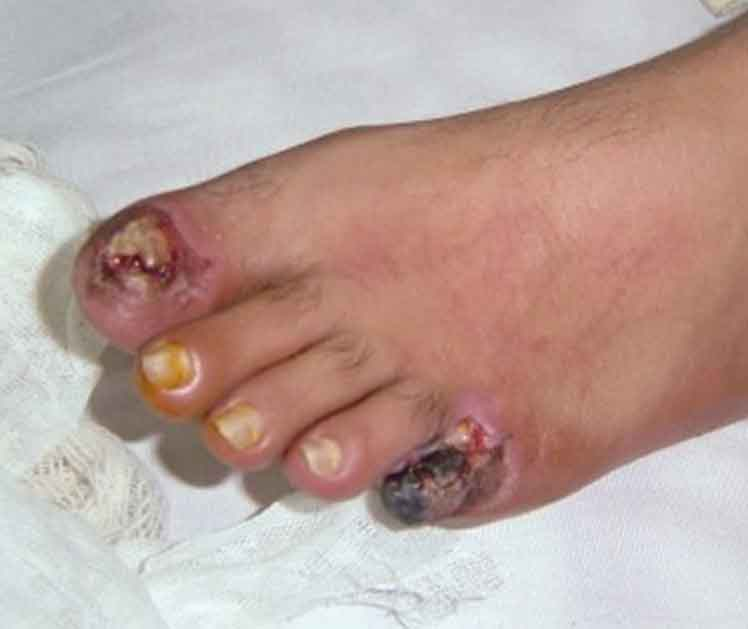
A 75-year-old man presents to the emergency department because of pain in his left thigh and left calf for the past 3 months. The pain occurs at rest, worsens with walking, and is slightly improved by hanging his foot off the bed. He has had hypertension for 25 years and type 2 diabetes mellitus for 30 years. He has smoked 30–40 cigarettes per day for the past 45 years. On examination, the femoral, popliteal, and dorsalis pedis pulses are diminished, but detectable on both sides. The patient’s foot is shown in the image. Which of the following is the most likely diagnosis?
A 67-year-old man comes to the physician for a follow-up examination. He has had lower back pain for several months. The pain radiates down the right leg to the foot. He has no history of any serious illness and takes no medications. His pain increases after activity. The straight leg test is positive on the right. The results of the laboratory studies show: Laboratory test Hemoglobin 14 g/d Leukocyte count 5,500/mm3 with a normal differential Platelet count 350,000/mm3 Serum Calcium 9.0 mg/dL Albumin 3.8 g/dL Urea nitrogen 14 mg/dL Creatinine 0.9 mg/dL Serum immunoelectrophoresis shows an immunoglobulin G (IgG) type monoclonal component of 40 g/L. Bone marrow plasma cells return at 20%. Skeletal survey shows no bone lesions. Magnetic resonance imaging (MRI) shows a herniated disc at the L5. Which of the following is the most appropriate next step?
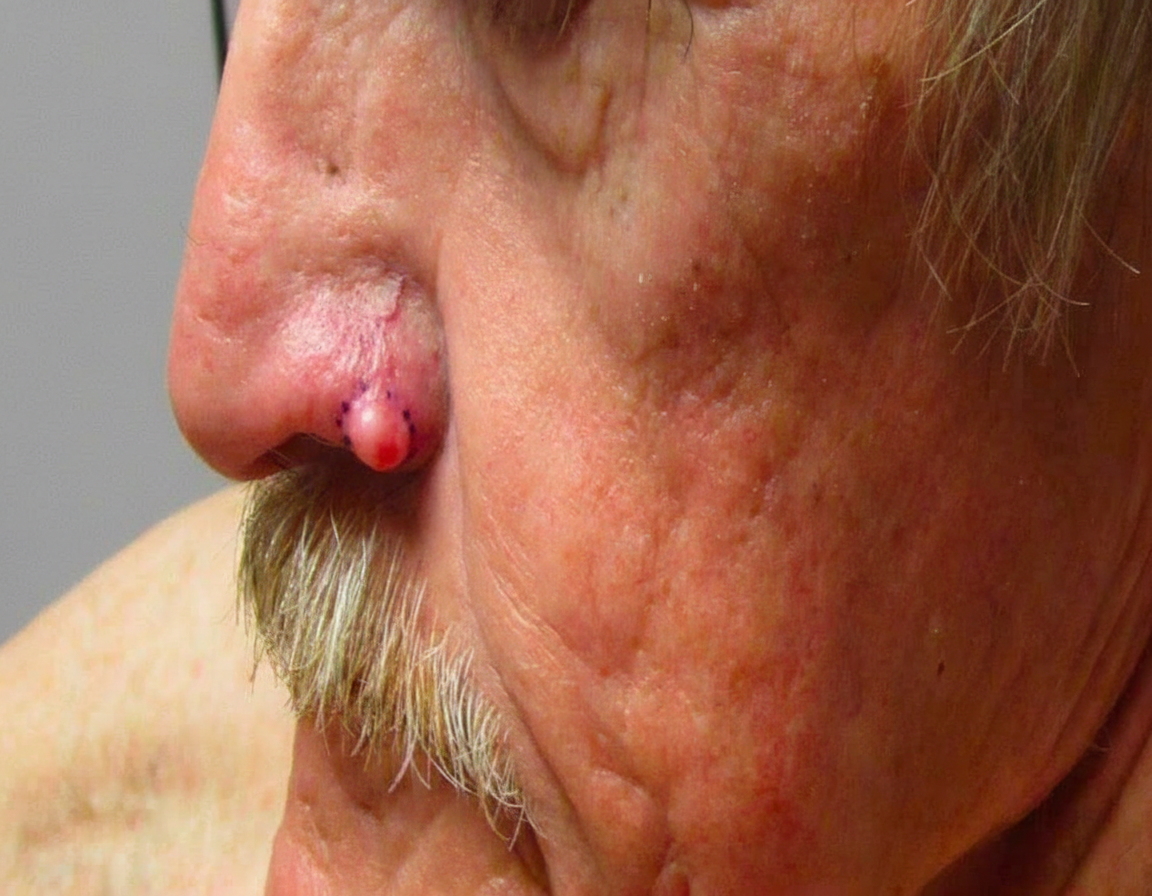
A 67-year-old man is referred to a dermatologist after a reddish mole appears on his nose. The mole’s size has changed over the last 2 years, and occasional bleeding is noted. The man’s medical history is unremarkable, and he does not take any medications. He retired from his construction job 15 years ago. Physical examination of his nose reveals a 2-cm pink papule with a pearly appearance and overlying telangiectasia on the ala of the nose (see image). Which of the following would be the best treatment modality if surgery is not an option?
A 57-year-old woman presents to an outpatient clinic with lower extremity weakness and lower back pain. The patient says that her symptoms began 2 weeks ago when she was working in her garden and have progressively worsened to the extent she currently is unable to walk on her own. She describes the pain as sharp, severe and descending bilaterally from her lower back to her lateral ankles along the posterior surface of her thighs and legs. She also states that she has had several episodes of urinary incontinence for the past couple of days. The patient denies having any similar pain or incontinence in the past. No other significant past medical history. Current medications are alendronate 5 mg orally daily and a daily multivitamin. Her temperature is 37.0℃ (98.6℉), the blood pressure is 110/70 mm Hg, the pulse is 72/min, the respiratory rate is 15/min, and oxygen saturation is 99% on room air. On physical examination, the patient appears to be in significant distress. Strength is ⅗ in her thighs bilaterally and ⅖ in the legs bilaterally left greater than right. Muscle tone is decreased in the lower extremities. The patellar reflex is 1+ bilaterally and plantar reflex is 0+ bilaterally. Fine touch and pain and temperature sensation are decreased in the lower extremities bilaterally, left greater than right. Saddle anesthesia is present. Which of the following is the next, best step in the management of this patient?
A 24-year-old woman is brought to the emergency department after being assaulted. The paramedics report that the patient was found conscious and reported being kicked many times in the torso. She is alert and able to respond to questions. She denies any head trauma. She has a past medical history of endometriosis and a tubo-ovarian abscess that was removed surgically two years ago. Her only home medication is oral contraceptive pills. Her temperature is 98.5°F (36.9°C), blood pressure is 82/51 mmHg, pulse is 136/min, respirations are 24/min, and SpO2 is 94%. She has superficial lacerations to the face and severe bruising over her chest and abdomen. Her lungs are clear to auscultation bilaterally and her abdomen is soft, distended, and diffusely tender to palpation. Her skin is cool and clammy. Her FAST exam reveals fluid in the perisplenic space. Which of the following is the next best step in management?
A 27-year-old man presents to the emergency department with severe dyspnea and sharp chest pain that suddenly started an hour ago after he finished exercising. He has a history of asthma as a child, and he achieves good control of his acute attacks with Ventolin. On examination, his right lung field is hyperresonant along with diminished lung sounds. Chest wall motion during respiration is asymmetrical. His blood pressure is 105/67 mm Hg, respirations are 22/min, pulse is 78/min, and temperature is 36.7°C (98.0°F). The patient is supported with oxygen, given corticosteroids, and has had analgesic medications via a nebulizer. Considering the likely condition affecting this patient, what is the best step in management?
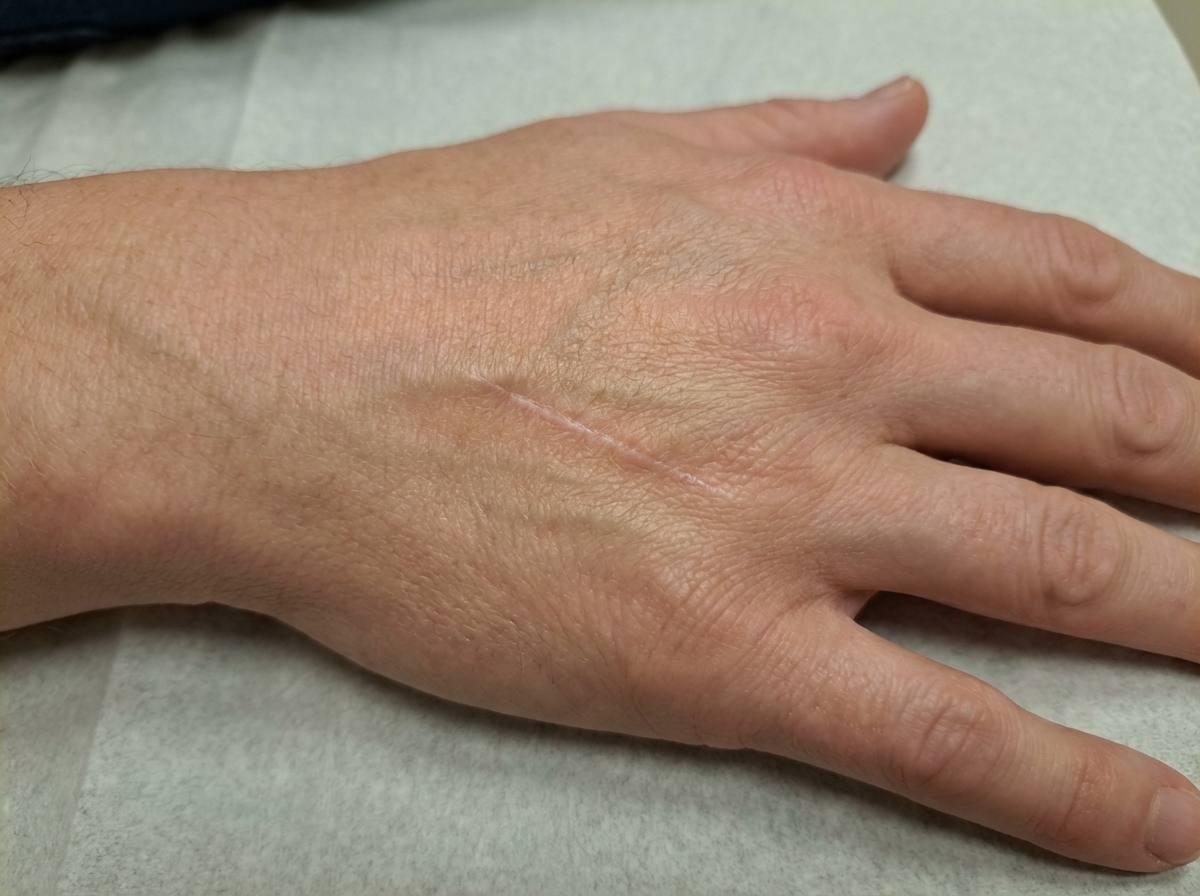
A 16-year-old boy presents to the emergency department after a skateboarding accident. He fell on a broken bottle and received a 4 cm wound on the dorsal aspect of his left hand. His vitals are stable and he was evaluated by the surgeon on call who determined that suturing was not required. After several weeks the wound has almost completely healed (see image). Which of the following is the correct description of this patient's wound before healing?
Practice by Chapter
Chest trauma management
Practice Questions
Head trauma management
Practice Questions
Spinal trauma
Practice Questions
Blunt abdominal trauma
Practice Questions
Penetrating abdominal trauma
Practice Questions
Pelvic fractures and hemorrhage
Practice Questions
Extremity trauma and vascular injuries
Practice Questions
Burns assessment and management
Practice Questions
Traumatic shock management
Practice Questions
Resuscitative thoracotomy
Practice Questions
Focused Assessment with Sonography in Trauma (FAST)
Practice Questions
Trauma in pregnancy
Practice Questions
Pediatric trauma considerations
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
