Trauma/Emergencies — MCQs

On this page
A 76-year-old hypertensive man who used to smoke 20 cigarettes a day for 40 years but quit 5 years ago presents to his family physician with a painless ulcer on the sole of his left foot, located at the base of his 1st toe. He has a history of pain in his left leg that awakens him at night and is relieved by dangling his foot off the side of the bed. His wife discovered the ulcer last week while doing his usual monthly toenail trimming. On physical exam, palpation of the patient’s pulses reveals the following: Right foot Femoral 4+ Popliteal 3+ Dorsalis Pedis 2+ Posterior Tibial 1+ Left foot Femoral 4+ Popliteal 2+ Dorsalis Pedis 0 Posterior Tibial 0 Pulse detection by Doppler ultrasound revealed decreased flow in the left posterior tibial artery, but no flow could be detected in the dorsalis pedis. What is the most likely principal cause of this patient’s ulcer?
A trauma 'huddle' is called. Morphine is administered for pain. Low-flow oxygen is begun. A traumatic diaphragmatic rupture is suspected. Infusion of 0.9% saline is begun. Which of the following is the most appropriate next step in management?
A 66-year-old woman is brought to the emergency department 4 hours after falling and hitting her head while skiing. Initially, she refused treatment, but an hour ago she began to develop a severe headache, nausea, and right leg weakness. She has osteopenia. Her only medication is a daily multivitamin. She has no visual changes and is oriented to person, time, and place. Her temperature is 37.2°C (99°F), pulse is 72/min, respirations are 18/min and regular, and blood pressure is 128/75 mm Hg. Examination shows a 5-cm bruise on the left side of her skull. The pupils are equal, round, and reactive to light and accommodation. Muscle strength is 0/5 in her right knee and foot. Which of the following is the most likely cause of this patient's symptoms?
A previously healthy 27-year-old man is brought to the emergency department 35 minutes after being involved in a high-speed motor vehicle collision in which he was an unrestrained passenger. He was ambulatory at the accident scene, with stable vital signs and no major external injuries except abrasions to both upper extremities. On arrival, he is alert and oriented. His temperature is 37.3°C (99.1°F), pulse is 88/min, respirations are 14/min, and blood pressure is 128/74 mm Hg. Abdominal examination shows ecchymosis over the upper abdomen, with tenderness to palpation over the left upper quadrant. There is no guarding or rigidity. Rectal examination is unremarkable. A CT scan of the abdomen with intravenous contrast shows a subcapsular splenic hematoma comprising 8% of the surface area, with no contrast extravasation and minimal blood in the peritoneal cavity. Which of the following is the next best step in management?
A 79-year-old man is brought to the emergency department after he noted the abrupt onset of weakness accompanied by decreased sensation on his left side. His symptoms developed rapidly, peaked within 1 minute, and began to spontaneously resolve 10 minutes later. Upon arrival in the emergency room 40 minutes after the initial onset of symptoms, they had largely resolved. The patient has essential hypertension, type 2 diabetes mellitus, chronic obstructive pulmonary disease, and a 50 pack-year smoking history. He also had an ST-elevation myocardial infarction 3 years ago. His brain CT scan without contrast is reported as normal. Carotid duplex ultrasonography reveals 90% stenosis of the right internal carotid. His transthoracic echocardiogram does not reveal any intracardiac abnormalities. Which of the following interventions is most appropriate for this patient's condition?
An unconscious middle-aged man is brought to the emergency department. He is actively bleeding from the rectum. He has no past medical history. At the hospital, his pulse is 110/min, the blood pressure is 90/60 mm Hg, the respirations are 26/min, and the oxygen saturation is 96% at room air. His extremities are cold. Resuscitation is started with IV fluids and cross-matched blood arranged. His vitals are stabilized after resuscitation and blood transfusion. His hemoglobin is 7.6 g/dL, hematocrit is 30%, BUN is 33 mg/dL, and PT/aPTT is within normal limits. A nasogastric tube is inserted, which drains bile without blood. Rectal examination and proctoscopy reveal massive active bleeding, without any obvious hemorrhoids or fissure. The physician estimates the rate of bleeding at 2-3 mL/min. What is the most appropriate next step in diagnosis?
A 25-year-old man comes to the emergency department with right knee pain. He was playing soccer when an opposing player tackled him from the side and they both fell down. He immediately heard a popping sound and felt severe pain in his right knee that prevented him from standing or walking. On physical examination, his right knee is swollen and there is local tenderness, mostly at the medial aspect. External rotation of the right knee elicits a significant sharp pain with a locking sensation. Which of the following structures is most likely injured?
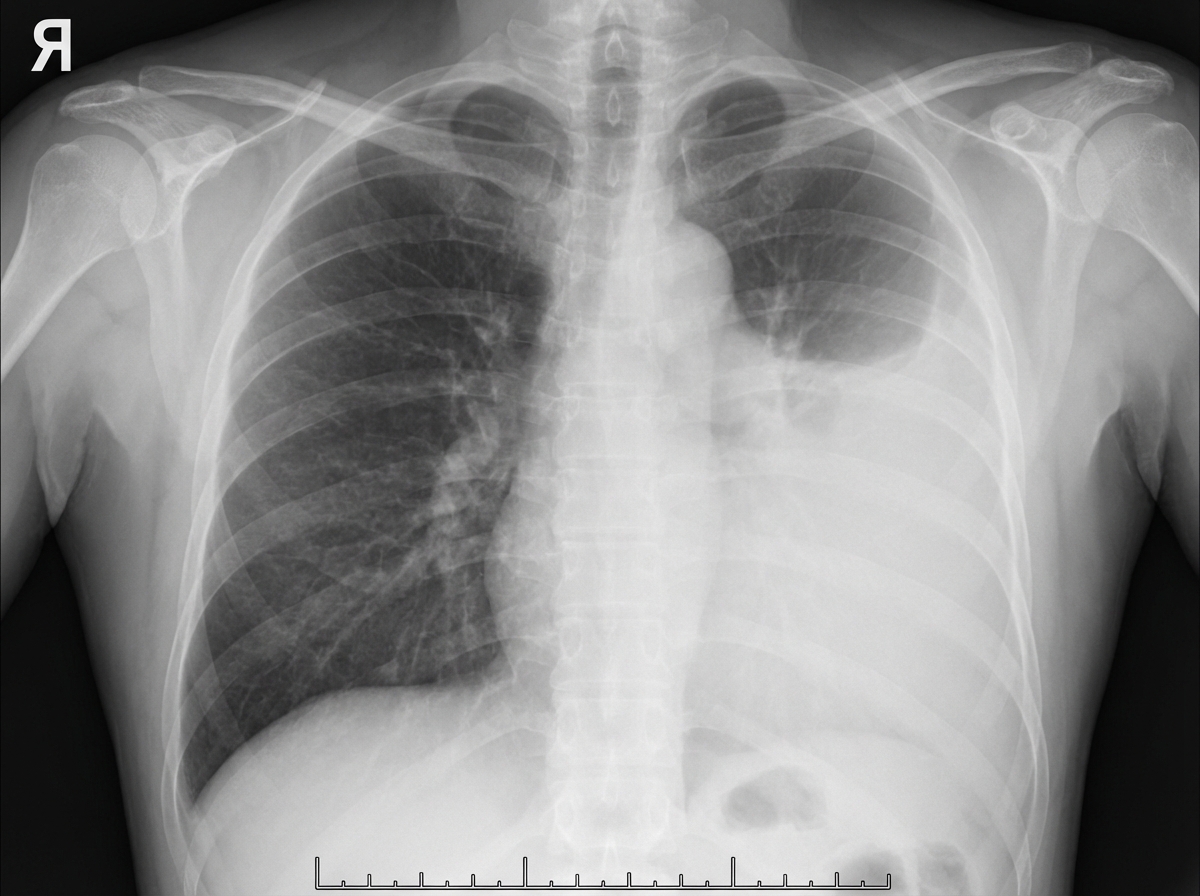
A 45-year-old man in respiratory distress presents to the emergency department. He sustained a stab to his left chest and was escorted to the nearest hospital. The patient appears pale and has moderate difficulty with breathing. His O2 saturation is 94%. The left lung is dull to percussion. CXRs are ordered and confirm the likely diagnosis. His blood pressure is 95/57 mm Hg, the respirations are 22/min, the pulse is 87/min, and the temperature is 36.7°C (98.0°F). His chest X-ray is shown. Which of the following is the next best step in management for this patient?
A 22-year-old man presents to the emergency department after being tackled in a game of football. The patient was hit from behind and fell to the ground. After the event, he complained of severe pain in his knee. The patient has a past medical history of anabolic steroid use. His current medications include whey protein supplements, multivitamins, and fish oil. His temperature is 99.5°F (37.5°C), blood pressure is 137/68 mmHg, pulse is 100/min, respirations are 17/min, and oxygen saturation is 98% on room air. On physical exam, you see a muscular young man clutching his knee in pain. The knee is inflamed and erythematous. When valgus stress is applied to the leg, there is some laxity when compared to the contralateral leg. The patient is requesting surgery for his injury. Arthrocentesis is performed and demonstrates no abnormalities of the synovial fluid. Which of the following physical exam findings is most likely to be seen in this patient?
A 40-year-old sailor is brought to a military treatment facility 20 minutes after being involved in a navy ship collision. He appears ill. He reports a sensation that he needs to urinate but is unable to void. His pulse is 140/min, respirations are 28/min, and blood pressure is 104/70 mm Hg. Pelvic examination shows ecchymoses over the scrotum and perineum. There is tenderness over the suprapubic region and blood at the urethral meatus. Digital rectal examination shows a high-riding prostate. Abdominal ultrasound shows a moderately distended bladder. X-rays of the pelvis show fractures of all four pubic rami. Which of the following is the most likely cause of this patient's symptoms?
Practice by Chapter
Chest trauma management
Practice Questions
Head trauma management
Practice Questions
Spinal trauma
Practice Questions
Blunt abdominal trauma
Practice Questions
Penetrating abdominal trauma
Practice Questions
Pelvic fractures and hemorrhage
Practice Questions
Extremity trauma and vascular injuries
Practice Questions
Burns assessment and management
Practice Questions
Traumatic shock management
Practice Questions
Resuscitative thoracotomy
Practice Questions
Focused Assessment with Sonography in Trauma (FAST)
Practice Questions
Trauma in pregnancy
Practice Questions
Pediatric trauma considerations
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
