Trauma/Emergencies — MCQs

On this page
A 40-year-old man presents with a painless firm mass in the right breast. Examination shows retraction of the nipple and the skin is fixed to the underlying mass. The axillary nodes are palpable. Which of the following statements is FALSE regarding the above condition?
A 34-year-old man presents to the emergency department by ambulance after being involved in a fight. On arrival, there is obvious trauma to his face and neck, and his mouth is full of blood. Seconds after suctioning the blood, his mouth rapidly fills up with blood again. As a result, he is unable to speak to you. An attempt at direct laryngoscopy fails as a result of his injuries. His vital signs are pulse 102/min, blood pressure 110/75 mmHg, and O2 saturation 97%. Which of the following is indicated at this time?
A 25-year-old man comes to the physician because of right wrist pain after a fall from a ladder. Physical examination shows decreased grip strength and tenderness between the tendons of extensor pollicis longus and extensor pollicis brevis. X-ray of the right wrist shows no abnormalities. This patient is at increased risk for which of the following complications?
A 17-year-old male presents to your office with right knee pain. He is the quarterback of his high school football team and developed the knee pain after being tackled in last night's game. He states he was running with the ball and was hit on the lateral aspect of his right knee while his right foot was planted. Now, he is tender to palpation over the medial knee and unable to bear full weight on the right lower extremity. A joint effusion is present and arthrocentesis yields 50 cc's of clear fluid. Which of the following exam maneuvers is most likely to demonstrate ligamentous laxity?
A previously healthy 5-year-old boy is brought to the emergency department 15 minutes after sustaining an injury to his right hand. His mother says that she was cleaning the bathroom when he accidentally knocked over the drain cleaner bottle and spilled the liquid onto his hand. On arrival, he is crying and holding his right hand in a flexed position. His temperature is 37.7°C (99.8°F), pulse is 105/min, respirations are 25/min, and blood pressure is 105/65 mm Hg. Examination of the right hand shows a 4 x 4 cm area of reddened, blistered skin. The area is very tender to light touch. His ability to flex and extend the right hand are diminished. Radial pulses are palpable. Capillary refill time is less than 3 seconds. Which of the following is the most appropriate next step in management?
A 47-year-old man is brought to the emergency room by his wife. She states that they were having dinner at a restaurant when the patient suddenly became out of breath. His past medical history is irrelevant but has a 20-year pack smoking history. On evaluation, the patient is alert and verbally responsive but in moderate respiratory distress. His temperature is 37°C (98.6°F), blood pressure is 85/56 mm Hg, pulse is 102/min, and respirations are 20/min. His oxygen saturation is 88% on 2L nasal cannula. An oropharyngeal examination is unremarkable. The trachea is deviated to the left. Cardiopulmonary examination reveals decreased breath sounds on the right lower lung field with nondistended neck veins. Which of the following is the next best step in the management of this patient?
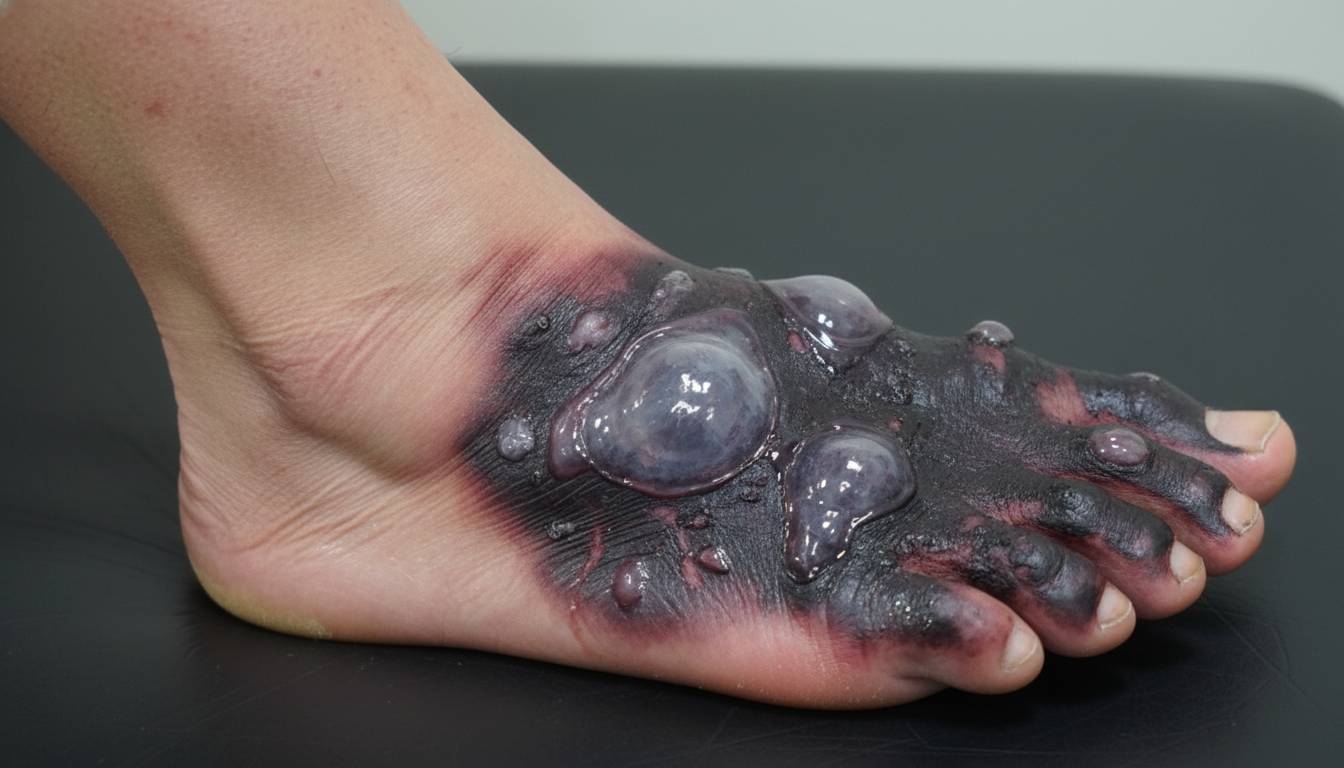
A 60-year-old man presents with pain, swelling, and a purulent discharge from his left foot. He says that the symptoms began 7 days ago with mild pain and swelling on the medial side of his left foot, but have progressively worsened. He states that there has been a foul-smelling discharge for the past 2 days. The medical history is significant for type 2 diabetes mellitus that was diagnosed 10 years ago and is poorly managed, and refractory peripheral artery disease that failed revascularization 6 months ago. The current medications include aspirin (81 mg orally daily) and metformin (500 mg orally twice daily). He has a 20-pack-year smoking history but quit 6 months ago. The family history is significant for type 2 diabetes mellitus in both parents and his father died of a myocardial infarction at 50 years of age. His temperature is 38.9°C (102°F); blood pressure 90/65 mm Hg; pulse 102/min; respiratory rate 22/min; and oxygen saturation 99% on room air. On physical examination, he appears ill and diaphoretic. The skin is flushed and moist. There is 2+ pitting edema of the left foot with blistering and black discoloration (see picture). The lower legs are hairless and the lower extremity peripheral pulses are 1+ bilaterally. Laboratory tests are pending. Blood cultures are positive for Staphylococcus aureus. Which of the following findings is the strongest indication for amputation of the left lower extremity in this patient?
A 32-year-old man is brought to the emergency department after a skiing accident. The patient had been skiing down the mountain when he collided with another skier who had stopped suddenly in front of him. He is alert but complaining of pain in his chest and abdomen. He has a past medical history of intravenous drug use and peptic ulcer disease. He is a current smoker. His temperature is 97.4°F (36.3°C), blood pressure is 77/53 mmHg, pulse is 127/min, and respirations are 13/min. He has a GCS of 15 and bilateral shallow breath sounds. His abdomen is soft and distended with bruising over the epigastrium. He is moving all four extremities and has scattered lacerations on his face. His skin is cool and delayed capillary refill is present. Two large-bore IVs are placed in his antecubital fossa, and he is given 2L of normal saline. His FAST exam reveals fluid in Morison's pouch. Following the 2L normal saline, his temperature is 97.5°F (36.4°C), blood pressure is 97/62 mmHg, pulse is 115/min, and respirations are 12/min. Which of the following is the best next step in management?
A 65-year-old man comes to the physician for evaluation of severe pain in his left shoulder for several days. He did not fall or injure his shoulder. He has a history of osteoarthritis of both knees that is well-controlled with indomethacin. He spends most of his time at a retirement facility and does not do any sports. There is no family history of serious illness. He has smoked one pack of cigarettes daily for 35 years. Vital signs are within normal limits. Physical examination shows tenderness of the greater tuberosity of the left humerus. There is no swelling or erythema. The patient is unable to slowly adduct his arm after it is passively abducted to 90 degrees. External rotation is limited by pain. Subacromial injection of lidocaine does not relieve his symptoms. An x-ray of the left shoulder shows sclerosis of the acromion and humeral head. Which of the following is the most appropriate next step in management?
A 34-year-old man is admitted to the emergency department after a motor vehicle accident in which he sustained blunt abdominal trauma. On admission, he is conscious, has a GCS score of 15, and has normal ventilation with no signs of airway obstruction. Vitals initially are blood pressure 95/65 mmHg, heart rate 87/min, respiratory rate 14/min, and oxygen saturation of 95% on room air. The physical exam is significant only for tenderness to palpation over the left flank. Noncontrast CT of the abdomen shows fractures of the 9th and 10th left ribs. Intravenous fluids are administered and the patient's blood pressure increases to 110/80 mm Hg. Three days later after admission, the patient suddenly complains of weakness and left upper quadrant (LUQ) pain. Vitals are blood pressure 80/50 mm Hg, heart rate 97/min, respiratory rate 18/min, temperature 36.2℃ (97.2℉) and oxygen saturation of 99% on room air. Prompt administration of 2L of IV fluids increases the blood pressure to 100/70 mm Hg. On physical exam, there is dullness to percussion and rebound tenderness with guarding in the LUQ. Bowel sounds are present. Raising the patient's left leg results in pain in his left shoulder. Stat hemoglobin level is 9.8 g/dL. Which of the following findings would be most likely seen if a CT scan were performed now?
Practice by Chapter
Chest trauma management
Practice Questions
Head trauma management
Practice Questions
Spinal trauma
Practice Questions
Blunt abdominal trauma
Practice Questions
Penetrating abdominal trauma
Practice Questions
Pelvic fractures and hemorrhage
Practice Questions
Extremity trauma and vascular injuries
Practice Questions
Burns assessment and management
Practice Questions
Traumatic shock management
Practice Questions
Resuscitative thoracotomy
Practice Questions
Focused Assessment with Sonography in Trauma (FAST)
Practice Questions
Trauma in pregnancy
Practice Questions
Pediatric trauma considerations
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
