Trauma/Emergencies — MCQs

On this page
A 52-year-old woman is brought to the emergency department by fire and rescue after being involved in a motor vehicle accident. The paramedics report that the patient’s car slipped off the road during a rainstorm and rolled into a ditch. The patient was restrained and the airbags deployed during the crash. The patient has a past medical history of hypertension, hyperlipidemia, hypothyroidism, and gout. Her home medications include hydrochlorothiazide, simvastatin, levothyroxine, and allopurinol. The patient is alert on the examination table. Her temperature is 98.2°F (36.8°C), blood pressure is 83/62 mmHg, pulse is 131/min, respirations are 14/min, and SpO2 is 96%. She has equal breath sounds in all fields bilaterally. Her skin is cool with diffuse bruising over her abdomen and superficial lacerations, and her abdomen is diffusely tender to palpation. She is moving all four extremities equally. The patient’s FAST exam is equivocal. She is given several liters of intravenous fluid during her trauma evaluation but her blood pressure does not improve. Which of the following is the best next step?
A 27-year-old man comes to the physician because of pain and swelling in his right knee that began 3 days ago when he fell during football practice. He fell on his flexed right knee as he dove to complete a pass. He felt some mild knee pain but continued to practice. Over the next 2 days, the pain worsened and the knee began to swell. Today, the patient has an antalgic gait. Examination shows a swollen and tender right knee; flexion is limited by pain. The right knee is flexed and pressure is applied to proximal tibia; 8 mm of backward translation of the foreleg is observed. Which of the following is most likely injured?
A 24-year-old woman presents to her primary care physician for unilateral breast pain. The patient states that she has been breastfeeding her son but has been experiencing worsening pain recently. Her pain is severe enough that she is now struggling to breastfeed her son with her left breast. The patient's past medical history is notable for gestational diabetes which was controlled with diet and exercise. Her temperature is 101°F (38.3°C), blood pressure is 137/69 mmHg, pulse is 100/min, respirations are 13/min, and oxygen saturation is 97% on room air. Physical exam reveals an erythematous breast with a 3-cm tender and fluctuant mass of the left breast. Which of the following is the best next step in management?
A 40-year-old woman who works as a secretary presents to your office complaining of new pain and numbness in both of her hands. For the past few weeks, the sensation has occurred after long days of typing, but it now occasionally wakes her up from sleep. You do not note any deformities of her wrists or hands, but you are able to reproduce pain and numbness in the first three and a half digits by tapping the wrist. What is the best initial treatment for this patient's complaint?
A 32-year-old man is brought to the emergency department 15 minutes after falling 7 feet onto a flat-top wooden post. On arrival, he is in severe pain and breathing rapidly. His pulse is 135/min, respirations are 30/min, and blood pressure is 80/40 mm Hg. There is an impact wound in the left fourth intercostal space at the midaxillary line. Auscultation shows tracheal deviation to the right and absent breath sounds over the left lung. There is dullness to percussion over the left chest. Neck veins are flat. Cardiac examination shows no abnormalities. Two large-bore intravenous catheters are placed and intravenous fluid resuscitation is begun. Which of the following is the most likely diagnosis?
A 35-year-old man is brought into the emergency department by emergency medical services with his right hand wrapped in bloody bandages. The patient states that he is a carpenter and was cutting some wood for a home renovation project when he looked away and injured one of his digits with a circular table saw. He states that his index finger was sliced off and is being brought in by his wife. On exam, his vitals are within normal limits and stable, and he is missing part of his second digit on his right hand distal to the proximal interphalangeal joint. How should the digit be transported to the hospital for the best outcome?
A 35-year-old man is brought to the emergency department 20 minutes after being involved in a motor vehicle collision in which he was a restrained passenger. The patient is confused. His pulse is 140/min and blood pressure is 85/60 mm Hg. Examination shows a hand-sized hematoma on the anterior chest wall. An ECG shows sinus tachycardia. Which of the following structures is most likely injured in this patient?
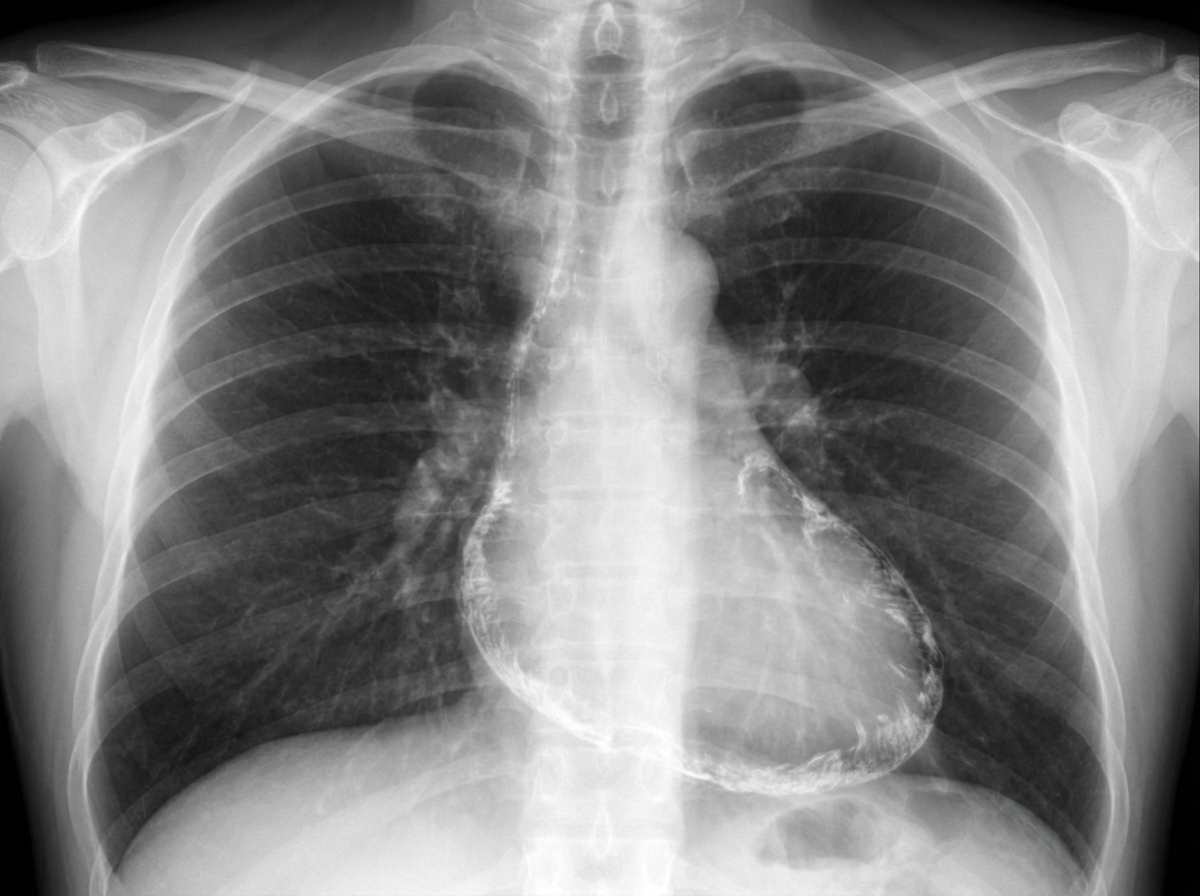
A 52-year-old man presents to the emergency department because of fatigue, abdominal distension, and swelling of both legs for the last 3 weeks. His wife says that he lost some weight recently. He has had type 2 diabetes mellitus for 12 years, for which he takes metformin and sitagliptin. He has a history of Hodgkin’s lymphoma which was successfully treated with mediastinal radiation 20 years ago. He does not smoke or drink alcohol. He has a family history of type 2 diabetes in his father and elder sister. Vital signs include a blood pressure of 100/70 mm Hg, a temperature of 36.9°C (98.4°F), and a regular radial pulse of 90/min. On physical examination, there is jugular venous distension, most prominently when the patient inhales. Bilateral ankle pitting edema is present, and his abdomen is distended with shifting dullness on percussion. An early diastolic knocking sound is audible on the chest. His chest X-ray is shown in the exhibit. Which of the following is the best treatment for this patient?
A previously healthy 64-year-old man comes to the physician 3 days after noticing a lump in his right groin while he was bathing. He has no history of trauma to the region. He has hypercholesterolemia and hypertension treated with atorvastatin and labetalol. He has smoked 2 packs of cigarettes daily for 35 years. His vital signs are within normal limits. Examination shows a 4-cm (1.6-in), nontender, pulsatile mass with a palpable thrill at the right midinguinal point. On auscultation, a harsh continuous murmur is heard over the mass. Femoral and pedal pulses are palpable bilaterally. The remainder of the examination shows no abnormalities. Which of the following is the most likely diagnosis?
A 62-year-old man presents to the emergency department with sudden onset of severe left leg pain accompanied by numbness and weakness. His medical history is remarkable for hypertension and hyperlipidemia. His vital signs include a blood pressure of 155/92 mm Hg, a temperature of 37.1°C (98.7°F), and an irregular pulse of 92/min. Physical examination reveals absent left popliteal and posterior tibial pulses. His left leg is noticeably cold and pale. There is no significant tissue compromise, nerve damage, or sensory loss. Which of the following will most likely be required for this patient's condition?
Practice by Chapter
Chest trauma management
Practice Questions
Head trauma management
Practice Questions
Spinal trauma
Practice Questions
Blunt abdominal trauma
Practice Questions
Penetrating abdominal trauma
Practice Questions
Pelvic fractures and hemorrhage
Practice Questions
Extremity trauma and vascular injuries
Practice Questions
Burns assessment and management
Practice Questions
Traumatic shock management
Practice Questions
Resuscitative thoracotomy
Practice Questions
Focused Assessment with Sonography in Trauma (FAST)
Practice Questions
Trauma in pregnancy
Practice Questions
Pediatric trauma considerations
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
