Trauma/Emergencies — MCQs

On this page
A 65-year-old man comes to his primary care physician with a 6-month history of bilateral calf pain. The pain usually occurs after walking his dog a few blocks and is more severe on the right side. He has coronary artery disease, essential hypertension, and type 2 diabetes mellitus. He has smoked two packs of cigarettes daily for 43 years and drinks two alcoholic beverages a day. Current medications include metformin, lisinopril, and aspirin. He is 183 cm (5 ft 11 in) tall and weighs 113 kg (250 lb); BMI is 34.9 kg/m2. His temperature is 37°C (98.6°F), pulse is 84/min, and blood pressure is 129/72 mm Hg. Cardiac examination shows a gallop without murmurs. The legs have shiny skin with reduced hair below the knee. Femoral and popliteal pulses are palpable bilaterally. Dorsal pedal pulses are 1+ on the left and absent on the right. Ankle-brachial index (ABI) is performed in the office. ABI is 0.5 in the right leg, and 0.6 in the left leg. Which of the following is the most appropriate initial step in management?
A 33-year-old man with a history of alcohol abuse and cirrhosis presents to the emergency department with profuse vomiting. The patient is aggressive, combative, emotionally labile, and has to be chemically restrained. The patient continues to vomit and blood is noted in the vomitus. His temperature is 99.2°F (37.3°C), blood pressure is 139/88 mmHg, pulse is 106/min, respirations are 17/min, and oxygen saturation is 100% on room air. The patient complains of sudden onset chest pain during his physical exam. A crunching and rasping sound is heard while auscultating the heart. Which of the following is the pathophysiology of the most likely diagnosis?
A 29-year-old man is brought to the emergency department 20 minutes after being stabbed in the left thigh. His pulse is 110/min, respirations are 20/min, and blood pressure is 110/70 mm Hg. Examination shows a 2-cm wound overlying a pulsatile mass on the left anterior thigh, 4 cm below the inguinal crease. A thrill is palpated, and a bruit is heard over this area. Peripheral pulses are normal bilaterally. The patient is at greatest risk for which of the following?
A 35-year-old man arrives at the emergency department within minutes after a head-on motor vehicle accident. He suffered from blunt abdominal trauma, several lacerations to his face as well as lacerations to his upper and lower extremities. The patient is afebrile, blood pressure is 45/25 mmHg and pulse is 160/minute. A CBC is obtained and is most likely to demonstrate which of the following?
A 30-year-old male presents with a testicular mass of unknown duration. The patient states he first noticed something unusual with his right testicle two weeks ago, but states he did not think it was urgent because it was not painful and believed it would resolve on its own. It has not changed since he first noticed the mass, and the patient still denies pain. On exam, the patient’s right testicle is non-tender, and a firm mass is felt. There is a negative transillumination test, and the mass is non-reducible. Which of the following is the best next step in management?
A 28-year-old soldier is brought back to a military treatment facility 45 minutes after sustaining injuries in a building fire from a mortar attack. He was trapped inside the building for around 20 minutes. On arrival, he is confused and appears uncomfortable. He has a Glasgow Coma Score of 13. His pulse is 113/min, respirations are 18/min, and blood pressure is 108/70 mm Hg. Pulse oximetry on room air shows an oxygen saturation of 96%. Examination shows multiple second-degree burns over the chest and bilateral upper extremities and third-degree burns over the face. There are black sediments seen within the nose and mouth. The lungs are clear to auscultation. Cardiac examination shows no abnormalities. The abdomen is soft and nontender. Intravenous fluid resuscitation is begun. Which of the following is the most appropriate next step in management?
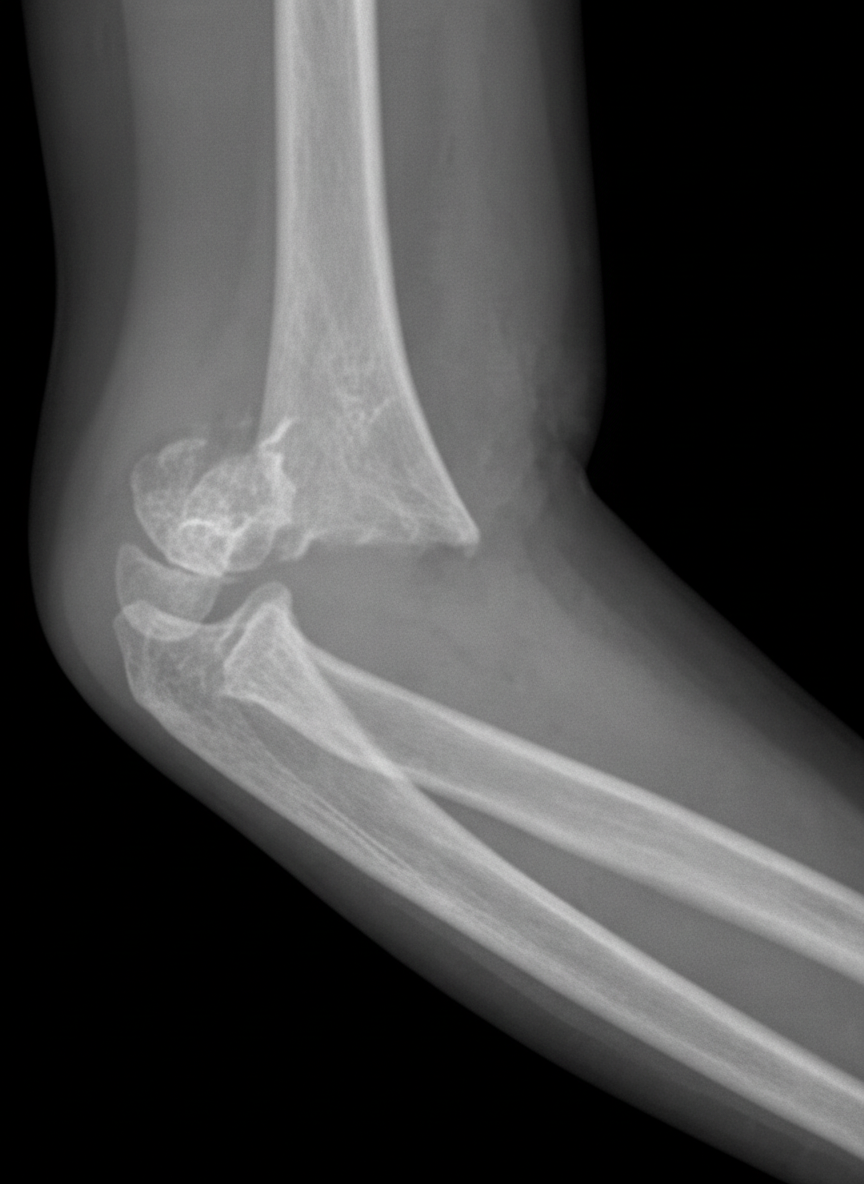
A 5-year-old boy is brought to the emergency department for right elbow swelling and pain 45 minutes after he fell while playing on the monkey bars during recess. He has been unable to move his right elbow since the fall. Examination shows ecchymosis, swelling, and tenderness of the right elbow; range of motion is limited by pain. The remainder of the examination shows no abnormalities. An x-ray of the right arm is shown. Which of the following is the most likely complication of this patient's injury?
A 54-year-old man comes to the physician because of a painful mass in his left thigh for 3 days. He underwent a left lower limb angiography for femoral artery stenosis and had a stent placed 2 weeks ago. He has peripheral artery disease, coronary artery disease, hypercholesterolemia and type 2 diabetes mellitus. He has smoked one pack of cigarettes daily for 34 years. Current medications include enalapril, aspirin, simvastatin, metformin, and sitagliptin. His temperature is 36.7°C (98°F), pulse is 88/min, and blood pressure is 116/72 mm Hg. Examination shows a 3-cm (1.2-in) tender, pulsatile mass in the left groin. The skin over the area of the mass shows no erythema and is cool to the touch. A loud bruit is heard on auscultation over this area. The remainder of the examination shows no abnormalities. Results of a complete blood count and serum electrolyte concentrations show no abnormalities. Duplex ultrasonography shows an echolucent sac connected to the common femoral artery, with pulsatile and turbulent blood flow between the artery and the sac. Which of the following is the most appropriate next best step in management?
A 45-year-old man is brought to the emergency department following a house fire. Following initial stabilization, the patient is transferred to the ICU for management of his third-degree burn injuries. On the second day of hospitalization, a routine laboratory panel is obtained, and the results are demonstrated below. Per the nurse, he remains stable compared to the day prior. His temperature is 99°F (37°C), blood pressure is 92/64 mmHg, pulse is 98/min, respirations are 14/min, and SpO2 is 98%. A physical examination demonstrates an unresponsive patient with extensive burn injuries throughout his torso and lower extremities. Hemoglobin: 13 g/dL Hematocrit: 36% Leukocyte count: 10,670/mm^3 with normal differential Platelet count: 180,000/mm^3 Serum: Na+: 135 mEq/L Cl-: 98 mEq/L K+: 4.7 mEq/L HCO3-: 25 mEq/L BUN: 10 mg/dL Glucose: 123 mg/dL Creatinine: 1.8 mg/dL Thyroid-stimulating hormone: 4.3 µU/mL Triiodothyronine: 48 ng/dL Thyroxine: 10 ug/dL Ca2+: 8.7 mg/dL AST: 89 U/L ALT: 135 U/L What is the best course of management for this patient?
A 22-year-old man comes to the physician because of a progressive swelling and pain in his right ring finger for the past 2 days. The pain began while playing football, when his finger got caught in the jersey of another player who forcefully pulled away. Examination shows that the right ring finger is extended. There is pain and swelling at the distal interphalangeal joint. When the patient is asked to make a fist, his right ring finger does not flex at the distal interphalangeal joint. There is no joint laxity. Which of the following is the most likely diagnosis?
Practice by Chapter
Chest trauma management
Practice Questions
Head trauma management
Practice Questions
Spinal trauma
Practice Questions
Blunt abdominal trauma
Practice Questions
Penetrating abdominal trauma
Practice Questions
Pelvic fractures and hemorrhage
Practice Questions
Extremity trauma and vascular injuries
Practice Questions
Burns assessment and management
Practice Questions
Traumatic shock management
Practice Questions
Resuscitative thoracotomy
Practice Questions
Focused Assessment with Sonography in Trauma (FAST)
Practice Questions
Trauma in pregnancy
Practice Questions
Pediatric trauma considerations
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
