Trauma/Emergencies — MCQs

On this page
A 27-year-old man is brought to the emergency department by ambulance following a motor vehicle accident 1 hour prior. He appears agitated. His blood pressure is 85/60 mm Hg, the pulse is 110/min, and the respiratory rate is 19/min. Physical examination shows bruising of the left flank and fracture of the left lower thoracic bones. Strict bed rest and monitoring with intravenous fluids is initiated. Urinalysis shows numerous RBCs. A contrast-enhanced CT scan shows normal enhancement of the right kidney. The left renal artery is only visible in the proximal section with a small amount of extravasated blood around the left kidney. The left kidney shows no enhancement. Imaging of the spleen shows no abnormalities. Which of the following is the most appropriate next step in management?
A 25-year-old man comes to the physician because of left-sided knee pain for 2 weeks. The pain started while playing basketball after suddenly hearing a popping sound. He has been unable to run since this incident. He has asthma, allergic rhinitis, and had a progressive bilateral sensorineural hearing impairment at birth treated with cochlear implants. His only medication is a salbutamol inhaler. The patient appears healthy and well-nourished. His temperature is 37°C (98.6°F), pulse is 67/min, and blood pressure is 120/80 mm Hg. Examination of the left knee shows medial joint line tenderness. Total knee extension is not possible and a clicking sound is heard when the knee is extended. An x-ray of the left knee shows no abnormalities. Which of the following is the most appropriate next step in the management of this patient?
An 81-year-old woman presents to her physician complaining of occasional right-sided weakness in her arm and leg. She reports 3 such episodes over the last 6 months, each lasting only 1 hour and not significantly affecting her daily functioning. The patient denies numbness and tingling, pain, weakness in her left side, and changes in her speech. She has a past medical history of hypertension and coronary artery disease with stable angina, and her medications include 81 mg aspirin, 20 mg lisinopril, 5 mg amlodipine, and 20 mg atorvastatin daily. The patient reports a 40-pack-year smoking history and occasional alcohol intake. At this visit, her temperature is 98.5°F (36.9°C), blood pressure is 142/87 mmHg, pulse is 70/min, and respirations are 14/min. She has a grade II systolic ejection murmur best heard at the right upper sternal border, and there is a carotid bruit on the left side. Her lungs are clear. Neurologic exam reveals intact cranial nerve function, 1+ deep tendon reflexes in bilateral patellae and biceps, as well as 5/5 strength and intact pinprick sensation in all extremities. Carotid ultrasound is performed and identifies 52% stenosis on the right side and 88% on the left. Which of the following is the best next step in management?
A 65-year-old woman comes to the physician because of a 2-month history of persistent pain in her right shoulder. The pain is localized to the top of the shoulder and is worse with movement. She has stiffness in the right shoulder that is worse in the morning and usually lasts 20 minutes. The patient reports that she is unable to brush her hair and has stopped going to her regular tennis lessons because of the pain. She does not recall any fall or trauma. When her right arm is passively abducted in an arc, there is pain between 60 and 120 degrees of abduction. When asked to lower the right arm slowly from 90 degrees of abduction, she is unable to hold her arm up and it drops to her side. Passive range of motion is normal. Injection of 5 mL of 1% lidocaine into the right subacromial space does not relieve the pain or improve active range of motion of the right arm. Which of the following is the most likely diagnosis?
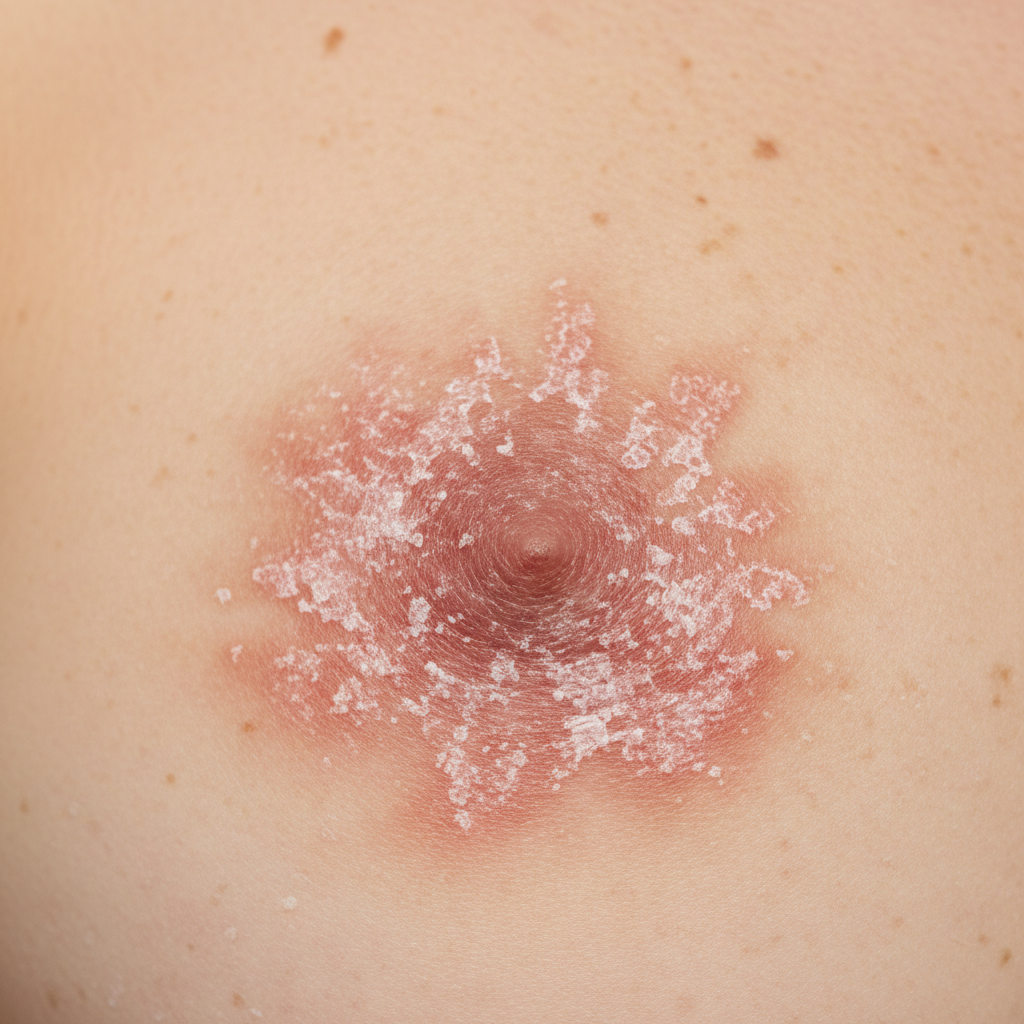
A 43-year-old woman presents to the physician because of a persistent rash on her right nipple for 1 month. The rash has persisted despite topical medication. She has no personal or family history of any serious illnesses. Other medications include oral contraceptive pills. She is single and has never had any children. Vital signs are within normal limits. An image of the right breast and nipple is shown. Palpation of the right breast shows a 2 x 2 cm mass under the areola. Lymphadenopathy is palpated in the right axilla. The remainder of the physical examination shows no abnormalities. A mammogram shows subareolar microcalcifications. Which of the following types of breast cancer is most likely to be found in this patient?
A 22-year-old man is brought to the emergency department 30 minutes after being involved in a high-speed motor vehicle collision in which he was the unrestrained driver. After extrication, he had severe neck pain and was unable to move his arms and legs. On arrival, he is lethargic and cannot provide a history. Hospital records show that eight months ago, he underwent an open reduction and internal fixation of the right humerus. His neck is immobilized in a cervical collar. Intravenous fluids are being administered. His pulse is 64/min, respirations are 8/min and irregular, and blood pressure is 104/64 mm Hg. Examination shows multiple bruises over the chest, abdomen, and extremities. There is flaccid paralysis and absent reflexes in all extremities. Sensory examination shows decreased sensation below the shoulders. Cardiopulmonary examination shows no abnormalities. The abdomen is soft. There is swelling of the right ankle and right knee. Squeezing of the glans penis does not produce anal sphincter contraction. A focused assessment with sonography for trauma shows no abnormalities. He is intubated and mechanically ventilated. Which of the following is the most appropriate next step in management?
A 49-year-old woman presents with a mass in her left breast. She says she discovered the mass during a monthly self-examination 3 months ago and has been 'watching it' since that time. She believes the mass has enlarged since she first discovered it. The patient denies any ulceration, weight loss, fatigue, night sweats, or nipple discharge. Her past medical history is significant for mild osteoporosis, managed with alendronate. The patient is afebrile, and her vital signs are within normal limits. On physical examination, there is a 4-cm-diameter left breast mass that is firm and non-tender on palpation. A mammogram of the left breast is performed but fails to display the mass. Which of the following is the best next step in the management of this patient?
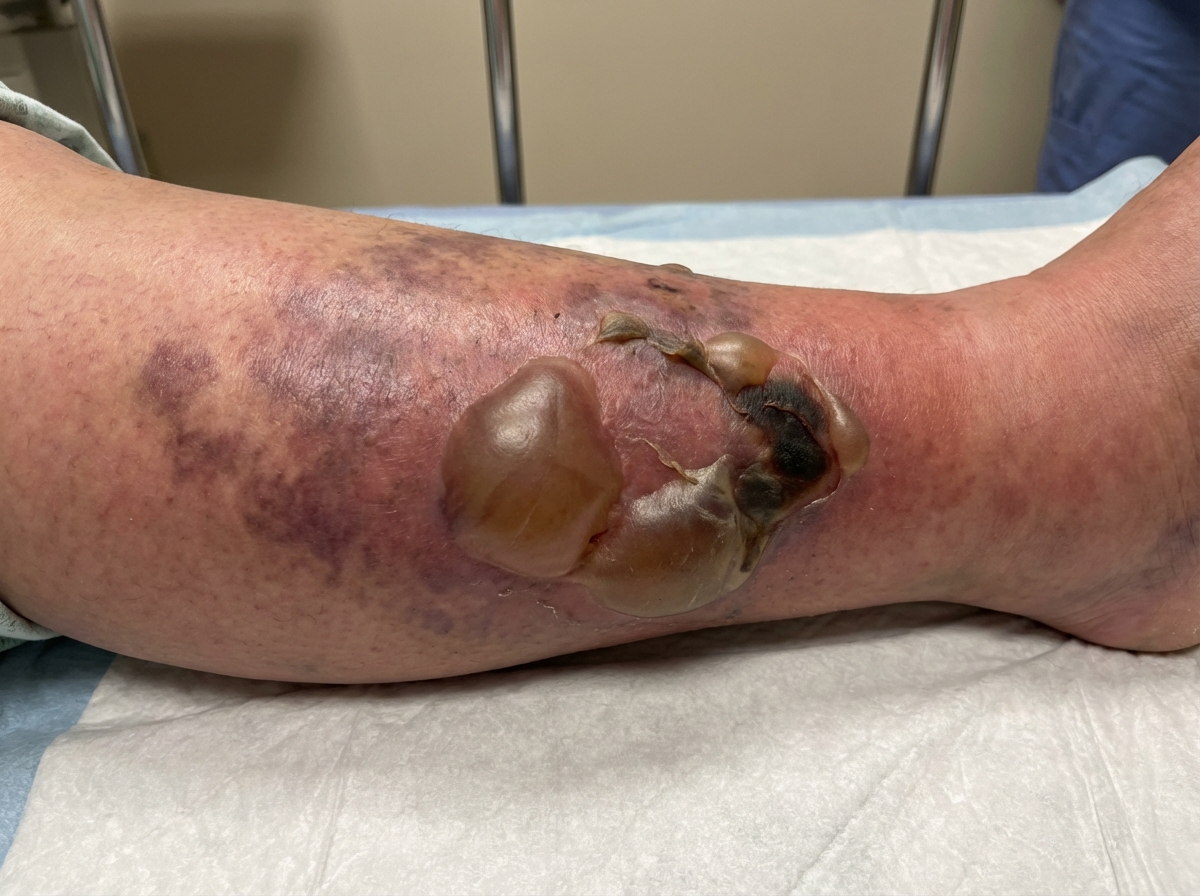
A 43-year-old man is brought to the emergency department with skin changes on his leg as shown in the image that manifested over the past 24 hours. He accidentally stabbed himself in the leg 4 days earlier with a knife that was in his pocket. He has a 10-year history of diabetes mellitus. His medications include metformin. He appears confused. His blood pressure is 90/70 mm Hg, the pulse is 115/min, the respirations are 21/min, and his temperature is 39.5℃ (103.1℉). The cardiopulmonary examination shows no other abnormalities. The serum creatinine level is 2.5 mg/dL. Which of the following is the most appropriate step in establishing a definitive diagnosis?
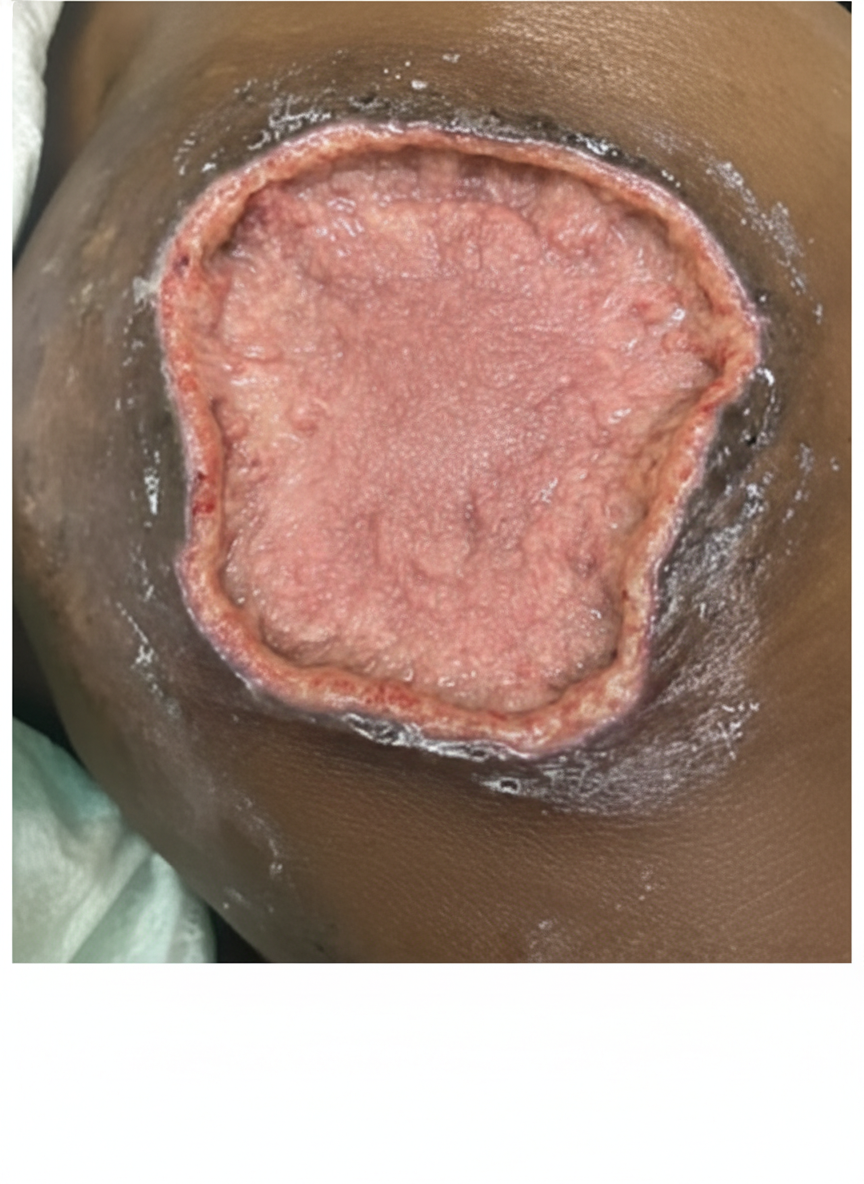
A 16-year-old boy is brought to the physician for a follow-up of a wound on his ankle. He had a pedestrian accident 3 days ago which caused a skin defect on the dorsal side of his left ankle. The lesion was cleaned, debrided, and observed over the past 3 days. He has no history of serious illness and takes no medications. His vital signs are within normal limits. Physical examination shows no signs of local infection. A photograph of the lesion is shown. Which of the following is the most appropriate surgical management?
A 67-year-old man is brought to the emergency room after being involved in a traffic accident. He currently complains of bilateral hip pain. His vital signs are within the normal range, and he is hemodynamically stable. The pelvic compression test is positive. External genitalia appears normal, except there is blood at the urethral meatus and a contusion at the base of the scrotum. Digital rectal examination (DRE) shows a high-riding ballotable prostate. An X-ray reveals the presence of a pelvic fracture. Which of the following initial actions is the most appropriate for this patient?
Practice by Chapter
Chest trauma management
Practice Questions
Head trauma management
Practice Questions
Spinal trauma
Practice Questions
Blunt abdominal trauma
Practice Questions
Penetrating abdominal trauma
Practice Questions
Pelvic fractures and hemorrhage
Practice Questions
Extremity trauma and vascular injuries
Practice Questions
Burns assessment and management
Practice Questions
Traumatic shock management
Practice Questions
Resuscitative thoracotomy
Practice Questions
Focused Assessment with Sonography in Trauma (FAST)
Practice Questions
Trauma in pregnancy
Practice Questions
Pediatric trauma considerations
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
