Trauma/Emergencies — MCQs

On this page
A 35-year-old man is referred to a physical therapist due to limitation of movement in the wrist and fingers of his left hand. He cannot hold objects or perform daily activities with his left hand. He broke his left arm at the humerus one month ago. The break was simple and treatment involved a cast for one month. Then he lost his health insurance and could not return for follow up. Only after removing the cast did he notice the movement issues in his left hand and wrist. His past medical history is otherwise insignificant, and vital signs are within normal limits. On examination, the patient’s left hand is pale and flexed in a claw-like position. It is firm and tender to palpation. Right radial pulse is 2+ and left radial pulse is 1+. The patient is unable to actively extend his fingers and wrist, and passive extension is difficult and painful. Which of the following is a proper treatment for the presented patient?
A 20-year-old man presents to the family medicine clinic with left knee pain. He is the star running back for his college football team with a promising future in the sport. He states he injured his knee 2 days ago during the final game of the season while making a cutting move, where his foot was planted and rotated outward and his knee buckled inward. He admits to feeling a ‘pop’ and having immediate pain. He denies any locking, clicking, or giving way since the event. Physical examination reveals an antalgic gait with avoidance of active knee extension. His left knee demonstrates moderate, diffuse swelling and is very tender to palpation along the joint line. Which of the following structures is most likely damaged in this patient?
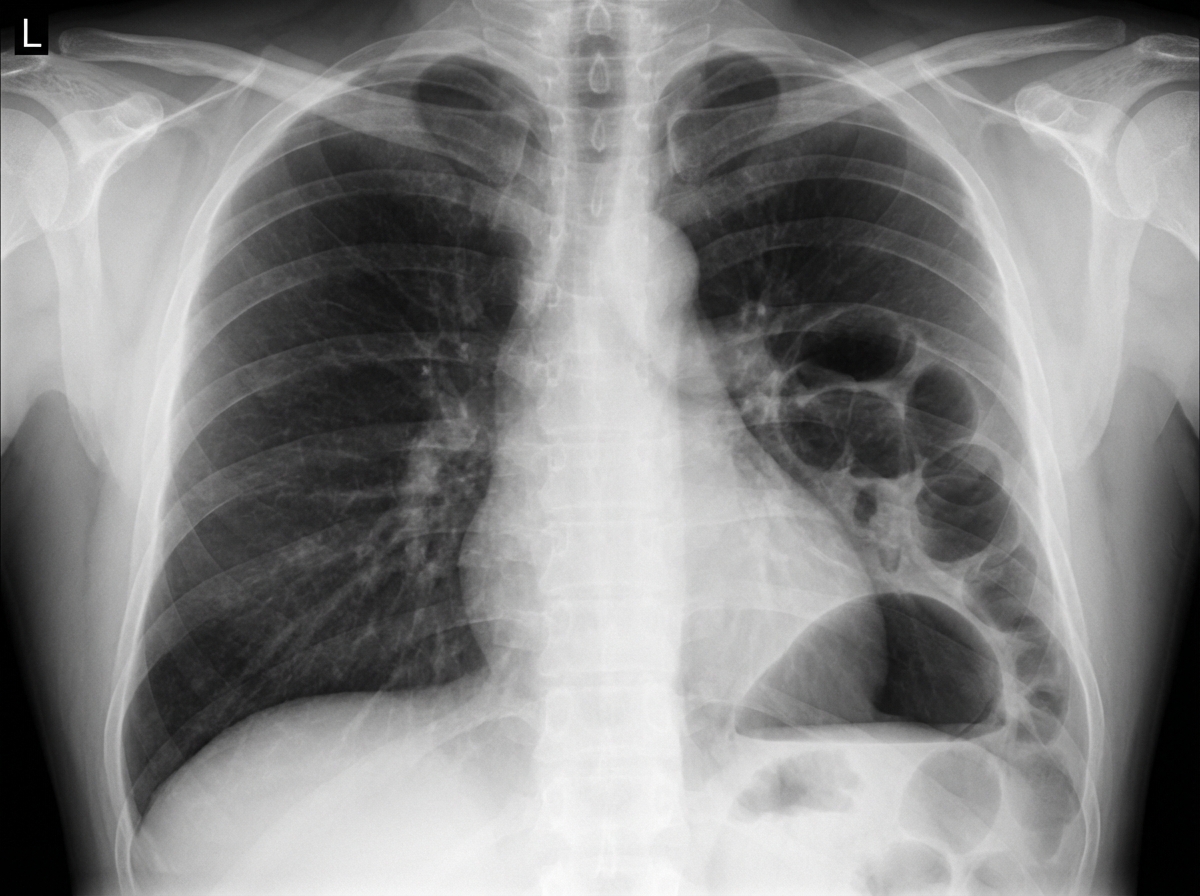
A 28-year-old man is brought to the emergency department with shortness of breath and chest pain, 35 minutes after he was involved in a high-speed motor vehicle collision. He was the helmeted driver of a scooter hit by a truck. On arrival, he is alert and oriented with a Glasgow Coma Scale rating of 14. His temperature is 37.3°C (99.1°F), pulse is 103/min, respirations are 33/min and blood pressure is 132/88 mm Hg. Pulse oximetry on room air shows an oxygen saturation of 94%. Examination shows multiple abrasions over his abdomen and extremities. There is a 2.5-cm (1-in) laceration on the left side of the chest. There are decreased breath sounds over the left base. Cardiac examination shows no abnormalities. The abdomen is soft and there is tenderness to palpation over the left upper quadrant. Bowel sounds are normal. His hemoglobin concentration is 13.6 g/dL, leukocyte count is 9,110/mm3, and platelet count is 190,000/mm3. A chest x-ray is shown. Which of the following is the most likely diagnosis?
An 8-year-old boy and his 26-year-old babysitter are brought into the emergency department with severe injuries caused by a motor vehicle accident. The child is wheeled to the pediatric intensive care unit with a severe injury to his right arm, as well as other external and internal injuries. He is hemorrhaging and found to be hemodynamically unstable. He subsequently requires transfusion and surgery, and he is currently unconscious. The pediatric trauma surgeon evaluates the child’s arm and realizes it will need to be amputated at the elbow. Which of the following is the most appropriate course of action to take with regards to the amputation?
A 37-year-old man is brought to the emergency department by a friend after he was found lying unconscious outside his front door. The friend reports that they were “pretty drunk” the previous night, and she had dropped her friend off at his home and driven off. When she came back in the morning, she found him passed out on the ground next to the doorstep. On arrival, he is conscious and cooperative. He reports feeling cold, with severe pain in his hands and face. He remembers having lost his gloves last night. His rectal temperature is 35.2°C (95.3°F), pulse is 86/min, respirations are 17/min, and blood pressure is 124/58 mm Hg. Examination shows decreased sensations over the distal fingers, which are cold to touch. The skin over the distal phalanges is cyanotic, hard, waxy, and tender, with surrounding edema. Laboratory studies are within the reference range. An x-ray of the chest and ECG show no abnormalities. Which of the following is the most appropriate next step in management?
A 35-year-old man is brought to the emergency department 40 minutes after spilling hot oil over himself in a kitchen accident. Examination shows multiple tense blisters over the abdomen, anterior chest, and right upper extremity. On deroofing the blisters, the skin over the right upper extremity is tender, pink, and blanches with pressure. The skin over the abdomen and anterior chest is tender, mottled, and does not blanch with pressure. The left thigh shows erythema only, is tender, and shows quick capillary refill after blanching with pressure. Which of the following most closely approximates the body surface area affected by 2nd-degree burns in this patient?
A 24-year-old man is brought to the emergency department 30 minutes after being involved in a high-speed motor vehicle collision in which he was a restrained driver. On arrival, he is alert and oriented. His pulse is 112/min, respirations are 29/min, and blood pressure is 100/60 mm Hg. The pupils are equal and reactive to light. There is a 3-cm laceration over the forehead and multiple bruises over the trunk. The lungs are clear to auscultation. Cardiac examination shows no abnormalities. The abdomen is soft and nontender. The right knee is swollen and tender; range of motion is limited by pain. Infusion of 0.9% saline is begun and intravenous acetaminophen is administered. Two hours later, blood-tinged fluid spontaneously drains from both nostrils, and is made worse by leaning forward. On a piece of gauze, it shows up as a rapidly-expanding clear ring of fluid surrounding blood. Further evaluation of this patient is most likely to show which of the following?
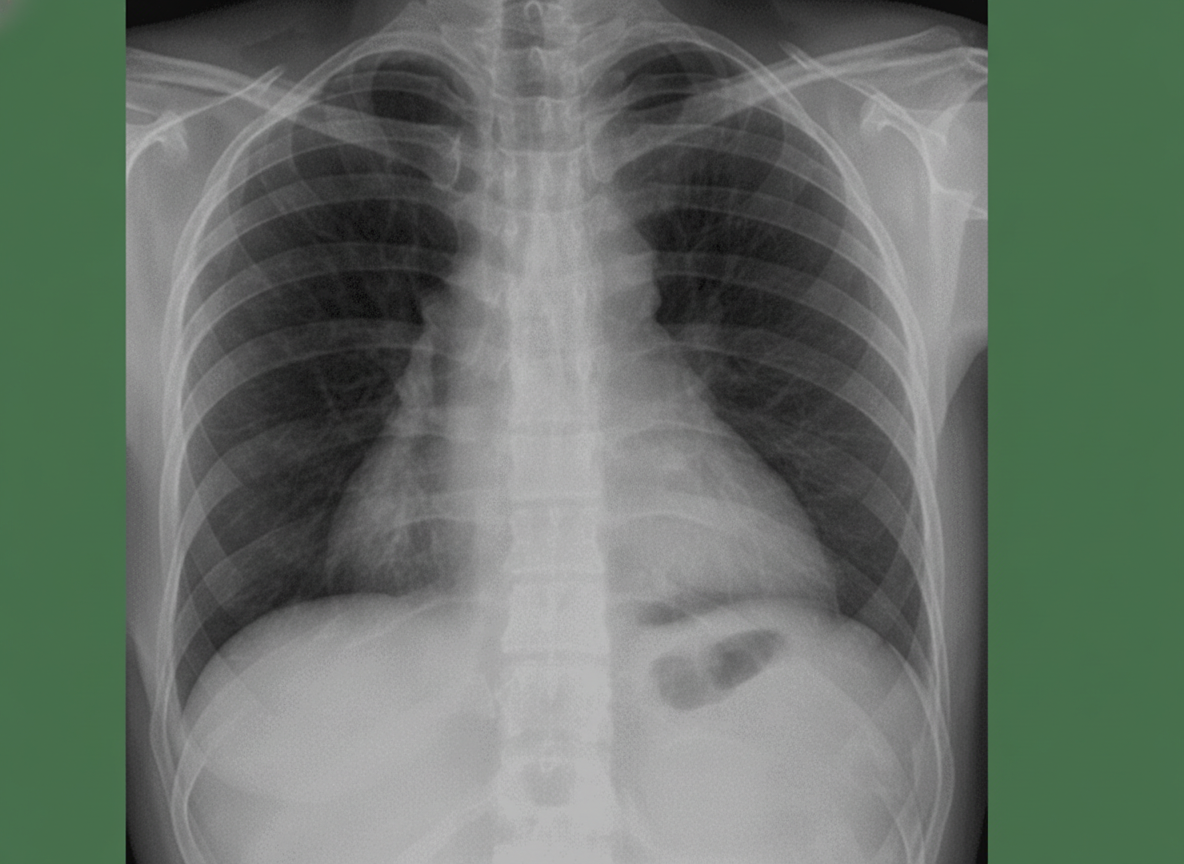
A 50-year-old man presents with severe chest pain for a week. His pain increases with breathing and is localized to the right. He has tried over-the-counter medications at home, but they did not help. The patient has a 20-pack-year smoking history and currently smokes 2 packs of cigarettes daily, and he drinks 3 to 4 cans of beer daily before dinner. His temperature is 39.1°C (102.3°F), blood pressure is 127/85 mm Hg, pulse is 109/min, and respirations are 20/min. Respiratory examination shows dullness to percussion from the 7th rib inferiorly at the right midaxillary line, decreased vocal tactile fremitus, and diminished breath sounds in the same area. Chest radiograph is shown in the image. The patient is prepared for thoracocentesis. Which of the following locations would be the most appropriate for insertion of a chest tube?
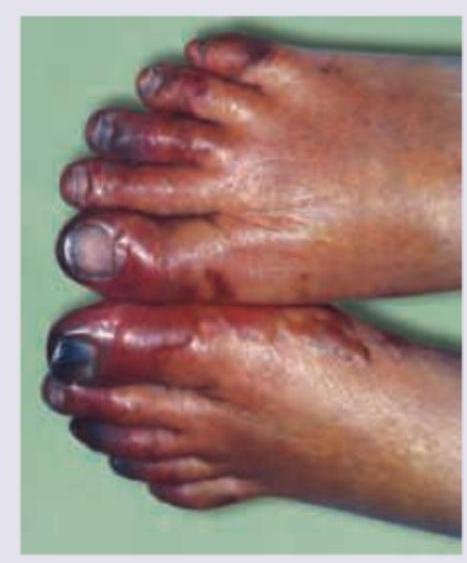
A 75-year-old man presents to the emergency department because of pain in his left thigh and left calf for the past 3 months. The pain occurs at rest, increases with walking, and is mildly improved by hanging the foot off the bed. He has had hypertension for 25 years and type 2 diabetes mellitus for 30 years. He has smoked 30–40 cigarettes per day for the past 45 years. On examination, femoral, popliteal, and dorsalis pedis pulses are faint on both sides. The patient’s foot is shown in the image. Resting ankle-brachial index (ABI) is found to be 0.30. Antiplatelet therapy and aggressive risk factors modifications are initiated. Which of the following is the best next step for this patient?
A 27-year-old man presents to the emergency department after being hit by a car while riding his bike. The patient was brought in with his airway intact, vitals stable, and with a C-collar on. Physical exam is notable for bruising over the patient’s head and a confused man with a Glasgow coma scale of 11. It is noticed that the patient has a very irregular pattern of breathing. Repeat vitals demonstrate his temperature is 97.5°F (36.4°C), blood pressure is 172/102 mmHg, pulse is 55/min, respirations are 22/min and irregular, and oxygen saturation is 94% on room air. Which of the following interventions are most likely to improve this patient's vital signs?
Practice by Chapter
Chest trauma management
Practice Questions
Head trauma management
Practice Questions
Spinal trauma
Practice Questions
Blunt abdominal trauma
Practice Questions
Penetrating abdominal trauma
Practice Questions
Pelvic fractures and hemorrhage
Practice Questions
Extremity trauma and vascular injuries
Practice Questions
Burns assessment and management
Practice Questions
Traumatic shock management
Practice Questions
Resuscitative thoracotomy
Practice Questions
Focused Assessment with Sonography in Trauma (FAST)
Practice Questions
Trauma in pregnancy
Practice Questions
Pediatric trauma considerations
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
