Trauma/Emergencies — MCQs

On this page
A 32-year-old man is brought to the emergency department 10 minutes after he sustained a stab wound to the left chest just below the clavicle. On arrival, he is hypotensive with rapid and shallow breathing and appears anxious and agitated. He is intubated and mechanically ventilated. Infusion of 0.9% saline is begun. Five minutes later, his pulse is 137/min and blood pressure is 84/47 mm Hg. Examination shows a 3-cm single stab wound to the left chest at the 4th intercostal space at the midclavicular line without active external bleeding. Cardiovascular examination shows muffled heart sounds and jugular venous distention. Breath sounds are normal bilaterally. Further evaluation of this patient is most likely to show which of the following findings?
A 37-year-old man presents to the emergency department after he cut his hand while working on his car. The patient has a past medical history of antisocial personality disorder and has been incarcerated multiple times. His vitals are within normal limits. Physical exam is notable for a man covered in tattoos with many bruises over his face and torso. Inspection of the patient's right hand reveals 2 deep lacerations on the dorsal aspects of the second and third metacarpophalangeal (MCP) joints. The patient is given a tetanus vaccination, and the wound is irrigated. Which of the following is appropriate management for this patient?
A 45-year-old man presents to an urgent care clinic because he coughed up blood this morning. Although he had a persistent cough for the past 3 weeks, he had never coughed up blood until now. His voice is hoarse and admits that it has been like that for the past few months. Both his past medical history and family history are insignificant. He has smoked a pack of cigarettes a day since the age of 20 and drinks wine every night before bed. His vitals are: heart rate of 78/min, respiratory rate of 14/min, temperature of 36.5°C (97.8°F), blood pressure of 140/88 mm Hg. An indirect laryngoscopy reveals a rough vegetating lesion on the free border of the right vocal cord. Which of the following is the most likely diagnosis?
A 22-year-old soldier sustains a stab wound to his chest during a military attack in Mali. He is brought to the combat medic by his unit for a primary survey. The soldier reports shortness of breath. He is alert and oriented to time, place, and person. His pulse is 99/min, respirations are 32/min, and blood pressure is 112/72 mm Hg. Examination shows a 2-cm wound at the left fourth intercostal space at the midclavicular line. Bubbling of blood is seen with each respiration at the wound site. There is no jugular venous distention. There is hyperresonance to percussion and decreased breath sounds on the left side. The trachea is at the midline. Which of the following is the most appropriate next step in management?
A 65-year-old man with a past medical history of anterior myocardial infarction, peripheral arterial disease, and known patent foramen ovale presents to the emergency department after being found down from a fall on the sidewalk in the middle of winter. He states that his right leg feels numb and painful at the same time. He insists that he did not slip on ice or snow, yet fell suddenly. He is taking aspirin, simvastatin, and cilastazol. Vital signs show T 98.0 F, BP 100/60, HR 100, RR 18. His pulse is irregularly irregular. His right leg appears pale with no dorsalis pedis and posterior tibial pulses compared to 2+ pulses on the left. He cannot discern soft or sharp touch in his right leg. Which intervention will most likely improve the viability of this patient's right leg?
A 60-year-old man is brought to the emergency department 25 minutes after falling and hitting his left flank on a concrete block. He has severe left-sided chest pain and mild shortness of breath. He underwent a right knee replacement surgery 2 years ago. He has type 2 diabetes mellitus. He has smoked one pack of cigarettes daily for 42 years. Current medications include metformin, sitagliptin, and a multivitamin. He appears uncomfortable. His temperature is 37.5°C (99.5°F), pulse is 102/min, respirations are 17/min, and blood pressure is 132/90 mm Hg. Pulse oximetry on room air shows an oxygen saturation of 96%. Examination shows multiple abrasions on his left flank and trunk. The upper left chest wall is tender to palpation and bony crepitus is present. There are decreased breath sounds over both lung bases. Cardiac examination shows no murmurs, rubs, or gallops. The abdomen is soft and nontender. Focused assessment with sonography for trauma is negative. An x-ray of the chest shows nondisplaced fractures of the left 4th and 5th ribs, with clear lung fields bilaterally. Which of the following is the most appropriate next step in management?
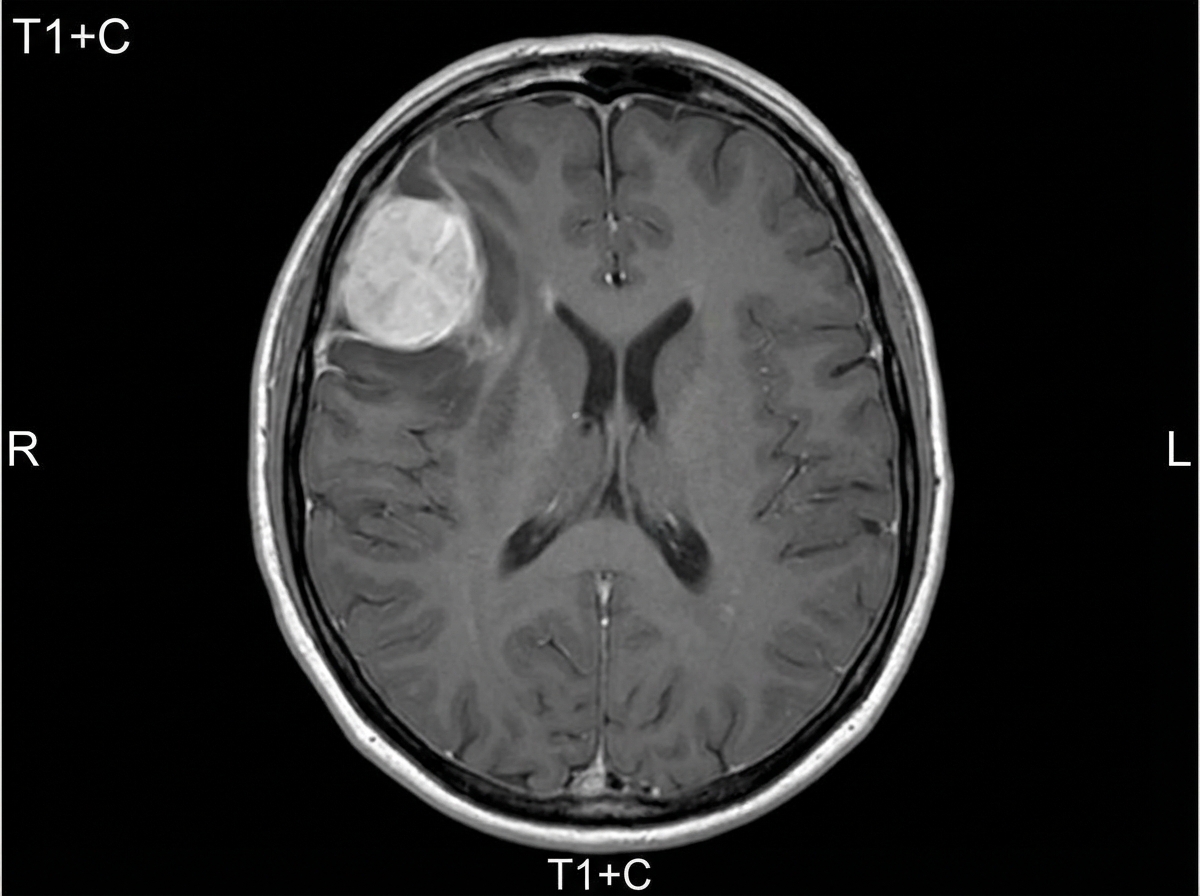
A 54-year-old woman comes to the physician because of paresthesias and weakness in her left leg for one year. Her symptoms have become progressively worse during this period and have led to some difficulty walking for the past month. She has had frequent headaches for the past 4 months. She has a history of hypertension and hypothyroidism. Current medications include amlodipine and levothyroxine. Her temperature is 37.3°C (99.1°F), pulse is 97/min, and blood pressure is 110/80 mm Hg. Neurologic examination shows decreased muscle strength in the left lower extremity. Deep tendon reflexes of the lower extremity are 4+ on the left and 2+ on the right side. The remainder of the examination shows no abnormalities. A complete blood count and serum concentrations of electrolytes, glucose, creatinine, and calcium are within the reference ranges. An MRI of the brain is shown. Which of the following is the most appropriate next step in management?
A 23-year-old man is brought to the emergency department because of severe right shoulder pain and inability to move the shoulder for the past 30 minutes. The pain began after being tackled while playing football. He has nausea but has not vomited. He is in no apparent distress. Examination shows the right upper extremity externally rotated and slightly abducted. Palpation of the right shoulder joint shows tenderness and an empty glenoid fossa. The right humeral head is palpated below the coracoid process. The left upper extremity is unremarkable. The radial pulses are palpable bilaterally. Which of the following is the most appropriate next step in management?
A 35-year-old man is brought to the emergency department 30 minutes after being involved in a motor vehicle collision. The patient was on his way to work before he lost control of his car and crashed into a tree. On arrival, the patient appears weak and lethargic. He has pain in his abdomen. His temperature is 37°C (98.6°F), pulse is 121/min, respirations are 22/min, and blood pressure is 85/60 mm Hg. He is oriented to person but not to place or time. The lungs are clear to auscultation. Cardiac examination shows tachycardia but no murmurs, rubs, or gallops. Abdominal examination shows several bruises above the umbilicus; there is diffuse abdominal tenderness. Focused assessment with sonography in trauma (FAST) is performed but the results are inconclusive. In addition to intravenous fluid resuscitation, which of the following is the most appropriate next step in management of this patient?
A 17-year-old male presents to the emergency department after a knife fight. He initially refused to come to the hospital, but one of his wounds overlying the right antecubital fossa would not stop bleeding. Vitals include: BP 90/65, HR 115, and RR 24. He reports that he is light-headed and having visual changes. You hold direct pressure over the wound on his right arm while the rest of the team resuscitates him with crystalloid and pRBCs. After his vitals signs normalize, you note that his right arm is cool and you are unable to palpate a radial pulse. The vascular surgery team explores his right arm, finding and repairing a lacerated brachial artery. Two hours post-operatively he is complaining of 10/10 pain in his right forearm and screams out loud when you passively move his fingers. What is the most appropriate next step in management?
Practice by Chapter
Chest trauma management
Practice Questions
Head trauma management
Practice Questions
Spinal trauma
Practice Questions
Blunt abdominal trauma
Practice Questions
Penetrating abdominal trauma
Practice Questions
Pelvic fractures and hemorrhage
Practice Questions
Extremity trauma and vascular injuries
Practice Questions
Burns assessment and management
Practice Questions
Traumatic shock management
Practice Questions
Resuscitative thoracotomy
Practice Questions
Focused Assessment with Sonography in Trauma (FAST)
Practice Questions
Trauma in pregnancy
Practice Questions
Pediatric trauma considerations
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
