Trauma/Emergencies — MCQs

On this page
A 27-year-old woman presents to her family physician with pain on the front of her right knee. The pain started 2 months ago after she began training for a marathon, and it was gradual in onset and has slowly worsened. The pain increases with prolonged sitting and climbing stairs. She denies significant knee trauma. Her only medication is diclofenac sodium as needed for pain. Medical history is unremarkable. The vital signs include: temperature 36.9°C (98.4°F), blood pressure 100/70 mm Hg, and heart rate 78/min. Her body mass index is 26 kg/m2. The pain is reproduced by applying direct pressure to the right patella, and there is increased patellar laxity with medial and lateral displacement. The remainder of the examination is otherwise unremarkable. Which of the following is the most likely diagnosis?
A 27-year-old man presents to the emergency department after he was assaulted and shot during a robbery. The patient was beaten with a baseball bat and has a bullet entry wound in his neck. He is currently complaining of diffuse pains but is able to speak. His voice sounds muffled, and he is requesting pain medications. An initial resuscitation is begun in the trauma bay. The patient's general appearance reveals ecchymosis throughout his body and minor scrapes and cuts, and possible multiple facial bone fractures. There is another bullet wound found in the left side of his back without an exit wound. Which of the following is the best next step in management?
A 36-year-old man was sent to the Emergency Department after a stray baseball hit him in the left eye during a game. Paramedics on sight could not perform the necessary testing and encouraged the patient to visit an ED for further testing and imaging. At the Emergency Department, the patient complains of slight pain in the orbital region and minimal diplopia that mildly increases with upward gaze. The patient’s blood pressure is 110/60 mm Hg, heart rate is 53/min, respiratory rate is 13/min, and temperature 36.6℃ (97.9℉). On physical examination, the patient is alert and responsive. There is an ecchymosis involving the lower lid and infraorbital area on the left side, with a slight downward deviation of the left globe, and conjunctival injection of the left eye. An upward gaze is limited on the left side. The visual acuity is 5/20 bilaterally. A head and neck CT shows a small (0.4 cm), nondisplaced, linear fracture of the left orbital floor. Which of the following statements about the condition the patient presents with is the most accurate?
A 28-year-old woman is brought to the emergency department 30 minutes after being involved in a high-speed motor vehicle collision in which she was the unrestrained driver. On arrival, she is semiconscious and incoherent. She has shortness of breath and is cyanotic. Her pulse is 112/min, respirations are 59/min, and blood pressure is 128/89 mm Hg. Examination shows a 3-cm (1.2-in) laceration on the forehead and multiple abrasions over the thorax and abdomen. There is crepitation on palpation of the thorax on the right. Auscultation of the lung shows decreased breath sounds on the right side. A crunching sound synchronous with the heartbeat is heard best over the precordium. There is dullness on percussion of the right hemithorax. The lips and tongue have a bluish discoloration. There is an open femur fracture on the left. The remainder of the examination shows no abnormalities. Arterial blood gas analysis on room air shows: pH 7.31 PCO2 55 mm Hg PO2 42 mm Hg HCO3- 22 mEq/L O2 saturation 76% The patient is intubated and mechanically ventilated. Infusion of 0.9% saline is begun. Which of the following is the most likely diagnosis?
A 27-year-old soldier stationed in Libya sustains a shrapnel injury during an attack, causing a traumatic above-elbow amputation. The resulting arterial bleed is managed with a tourniquet prior to transport to the military treatment facility. On arrival, he is alert and oriented to person, place, and time. His armor and clothing are removed. His pulse is 145/min, respirations are 28/min, and blood pressure is 95/52 mm Hg. Pulmonary examination shows symmetric chest rise. The lungs are clear to auscultation. Abdominal examination shows no abnormalities. There are multiple shrapnel wounds over the upper and lower extremities. A tourniquet is in place around the right upper extremity; the right proximal forearm has been amputated. One large-bore intravenous catheter is placed in the left antecubital fossa. Despite multiple attempts, medical staff is unable to establish additional intravenous access. Which of the following is the most appropriate next step in management?
A 31-year-old man presents to the Emergency Department with severe left leg pain and paresthesias 4 hours after his leg got trapped by the closing door of a bus. Initially, he had a mild pain which gradually increased to unbearable levels. Past medical history is noncontributory. In the Emergency Department, his blood pressure is 130/80 mm Hg, heart rate is 87/min, respiratory rate is 14/min, and temperature is 36.8℃ (98.2℉). On physical exam, his left calf is firm and severely tender on palpation. The patient cannot actively dorsiflex his left foot, and passive dorsiflexion is limited. Posterior tibial and dorsalis pedis pulses are 2+ in the right leg and 1+ in the left leg. Axial load does not increase the pain. Which of the following is the best next step in the management of this patient?
A 72-year-old man comes to the physician for a 5-month history of hoarseness, exertional dyspnea, and fatigue. He does not smoke or drink alcohol. His pulse is 98/min and irregular. His voice is coarse in quality. Physical examination shows a liver span of 16 cm and a soft diastolic murmur heard best at the apex. Which of the following is the most likely cause of this patient's hoarseness?
A 33-year-old man presents to his primary care physician with shoulder pain. He states that he can't remember a specific instance when the injury occurred. He is a weight lifter and competes in martial arts. The patient has no past medical history and is currently taking a multivitamin. Physical exam demonstrates pain with abduction of the patient's right shoulder and with external rotation of the right arm. There is subacromial tenderness with palpation. His left arm demonstrates 10/10 strength with abduction as compared to 4/10 strength with abduction of the right arm. Which of the following best confirms the underlying diagnosis?
A 17-year-old boy is brought to the emergency department by his parents 6 hours after he suddenly began to experience dyspnea and pleuritic chest pain at home. He has a remote history of asthma in childhood but has not required any treatment since the age of four. His temperature is 98.4°F (36.9°C), blood pressure is 100/76 mmHg, pulse is 125/min, respirations are 24/min. On exam, he has decreased lung sounds and hyperresonance in the left upper lung field. A chest radiograph shows a slight tracheal shift to the right. What is the best next step in management?
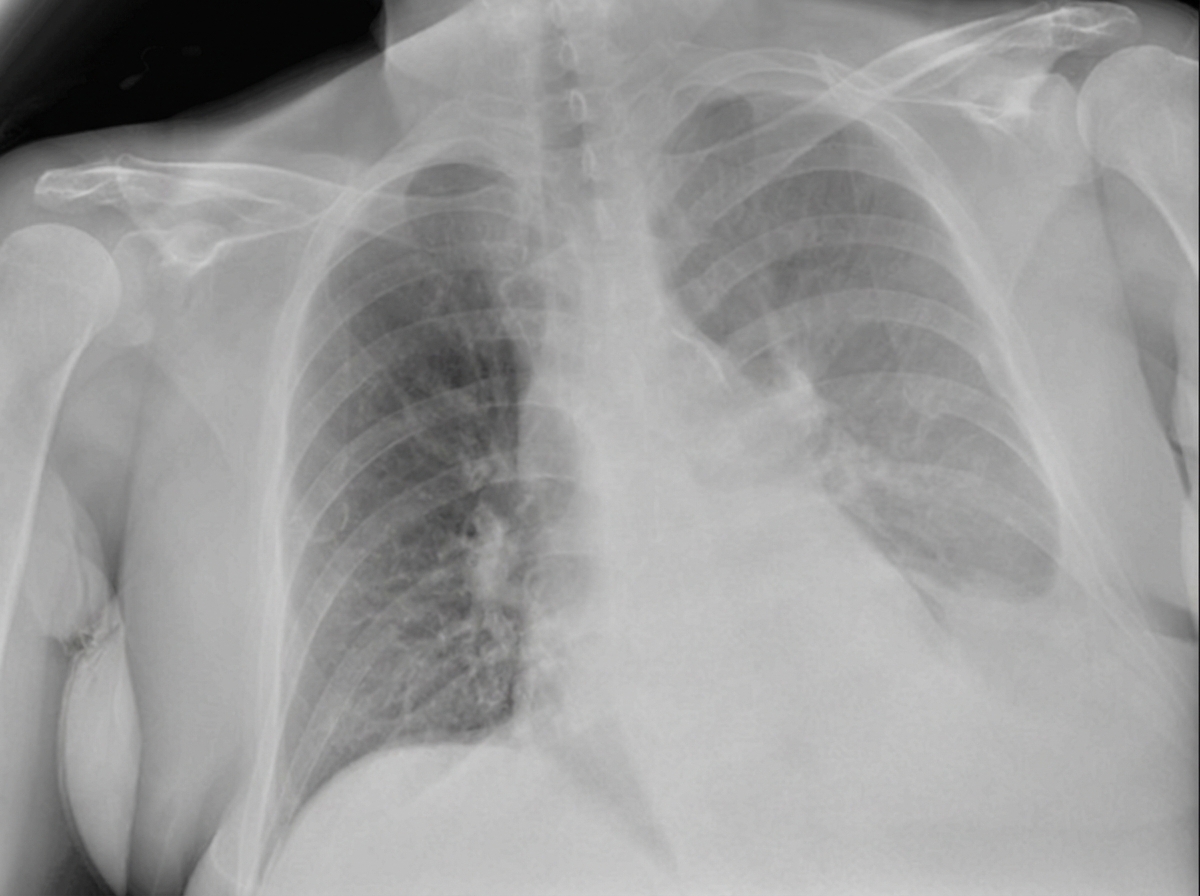
A 27-year-old soldier is brought to the emergency department of a military hospital 20 minutes after being involved in a motor vehicle accident during a training exercise. He was an unrestrained passenger. On arrival, he has shortness of breath and chest pain. He appears pale and anxious. His temperature is 37°C (98.6°F), pulse is 110/min, respirations are 20/min, and blood pressure is 100/65 mm Hg. He is alert and oriented to person, place, and time. Examination shows pale conjunctivae and mucous membranes. There is bruising on the chest, extremities, and abdomen. The lungs are clear to auscultation. He has normal heart sounds and flat neck veins. The abdomen is flat, soft, and mildly tender. The remainder of the physical examination shows no abnormalities. High-flow oxygen is applied, and intravenous fluid resuscitation is begun. A chest x-ray is obtained. Which of the following is the most appropriate next step in management?
Practice by Chapter
Chest trauma management
Practice Questions
Head trauma management
Practice Questions
Spinal trauma
Practice Questions
Blunt abdominal trauma
Practice Questions
Penetrating abdominal trauma
Practice Questions
Pelvic fractures and hemorrhage
Practice Questions
Extremity trauma and vascular injuries
Practice Questions
Burns assessment and management
Practice Questions
Traumatic shock management
Practice Questions
Resuscitative thoracotomy
Practice Questions
Focused Assessment with Sonography in Trauma (FAST)
Practice Questions
Trauma in pregnancy
Practice Questions
Pediatric trauma considerations
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
