Trauma/Emergencies — MCQs

On this page
A 23-year-old patient presents to the emergency department after a motor vehicle accident. The patient was an unrestrained driver involved in a head-on collision. The patient is heavily intoxicated on what he claims is only alcohol. An initial trauma assessment is performed, and is notable for significant bruising of the right forearm. The patient is in the trauma bay, and complains of severe pain in his right forearm. A physical exam is performed and is notable for pallor, decreased sensation, and cool temperature of the skin of the right forearm. Pain is elicited upon passive movement of the right forearm and digits. A thready radial pulse is palpable. A FAST exam is performed, and is negative for signs of internal bleeding. The patient's temperature is 99.5°F (37.5°C), pulse is 100/min, blood pressure is 110/70 mmHg, respirations are 12/min, and oxygen saturation is 98% on room air. Radiography of the right forearm is ordered. The patient is still heavily intoxicated. Which of the following is the best next step in management?
A 3-year-old boy is brought to a respiratory specialist. The family physician referred the child because of recurrent respiratory infections over the past 2 years. Chest X-rays showed a lesion of < 2 cm that includes glands and cysts in the upper lobe of the right lung. Diseases affecting the immune system were investigated and ruled out. No family history of any pulmonary disease or congenital malformations exists. He was born at full term via a normal vaginal delivery with an APGAR score of 10. Which of the following should be highly considered for effective management of this child’s condition?
A 23-year-old woman comes to the emergency department for the evaluation of mild retrosternal pain for the last 7 hours after several episodes of self-induced vomiting. The patient was diagnosed with bulimia nervosa 9 months ago. Her only medication is citalopram. She is 170 cm (5 ft 7 in) tall and weighs 62 kg (136.6 lb); BMI is 21.5 kg/m2. She appears pale. Her temperature is 37°C (98.6°F), pulse is 75/min, respirations are 21/min, and blood pressure is 110/75 mm Hg. The lungs are clear to auscultation. Cardiac examinations shows no murmurs, rubs, or gallops. The abdomen is soft and nontender with no organomegaly. The remainder of the physical examination shows swelling of the salivary glands, dry skin, and brittle nails. An ECG and an x-ray of the chest show no abnormalities. Contrast esophagram with gastrografin shows mild leakage of contrast from the lower esophagus into the mediastinum without contrast extravasation into the pleural and peritoneal cavities. Which of the following is the most appropriate next step in the management?
A 41-year-old man is admitted to the emergency room after being struck in the abdomen by a large cement plate while transporting it. On initial assessment by paramedics at the scene, his blood pressure was 110/80 mm Hg, heart rate 85/min, with no signs of respiratory distress. On admission, the patient is alert but in distress. He complains of severe, diffuse, abdominal pain and severe weakness. Vital signs are now: blood pressure 90/50 mm Hg, heart rate 96/min, respiratory rate 19/min, temperature 37.4℃ (99.3℉), and oxygen saturation of 95% on room air. His lungs are clear on auscultation. The cardiac exam is significant for a narrow pulse pressure. Abdominal examination reveals a large bruise over the epigastric and periumbilical regions. The abdomen is distended and there is diffuse tenderness to palpation with rebound and guarding, worst in the epigastric region. There is hyperresonance to percussion in the epigastric region and absence of hepatic dullness in the right upper quadrant. Aspiration of the nasogastric tube reveals bloody contents. Focused assessment with sonography for trauma (FAST) shows free fluid in the pelvic region. Evaluation of the perisplenic and perihepatic regions is impossible due to the presence of free air. Aggressive intravenous fluid resuscitation is administered but fails to improve upon the patient’s hemodynamics. Which of the following is the next best step in management?
A 22-year-old soldier sustains a gunshot wound to the left side of the chest during a deployment in Syria. The soldier and her unit take cover from gunfire in a nearby farmhouse, and a combat medic conducts a primary survey of her injuries. She is breathing spontaneously. Two minutes after sustaining the injury, she develops severe respiratory distress. On examination, she is agitated and tachypneic. There is an entrance wound at the midclavicular line at the 2nd rib and an exit wound at the left axillary line at the 4th rib. There is crepitus on the left side of the chest wall. Which of the following is the most appropriate next step in management?
A 62-year-old man comes to the emergency department for severe, acute right leg pain. The patient's symptoms began suddenly 4 hours ago, while he was reading the newspaper. He has poorly-controlled hypertension and osteoarthritis. He has smoked one pack of cigarettes daily for 31 years. Current medications include lisinopril, metoprolol succinate, and ibuprofen. He appears to be in severe pain and is clutching his right leg. His temperature is 37.4°C (99.3°F), pulse is 102/min and irregularly irregular, respirations are 19/min, and blood pressure is 152/94 mm Hg. The right leg is cool to the touch, with decreased femoral, popliteal, posterior tibial, and dorsalis pedis pulses. There is moderate weakness and decreased sensation in the right leg. An ECG shows absent P waves and a variable R-R interval. Right leg Doppler study shows inaudible arterial signal and audible venous signal. Angiography shows 90% occlusion of the right common femoral artery. In addition to initiating heparin therapy, which of the following is the most appropriate next step in management?
A 40-year-old male visits a urologist and reports that for the past 2 weeks, his penis has been gradually curving to the right with associated pain during intercourse. He is able to have a normal erection and he does not recollect of any trauma to his penis. Although he is married, he admits to having unprotected sexual relationship with several females in the past year. His vitals are normal and physical examination is unremarkable except for a lesionless curved penis. It is painless to touch. Test results for sexually transmitted disease is pending. Which of the following is the most likely cause?
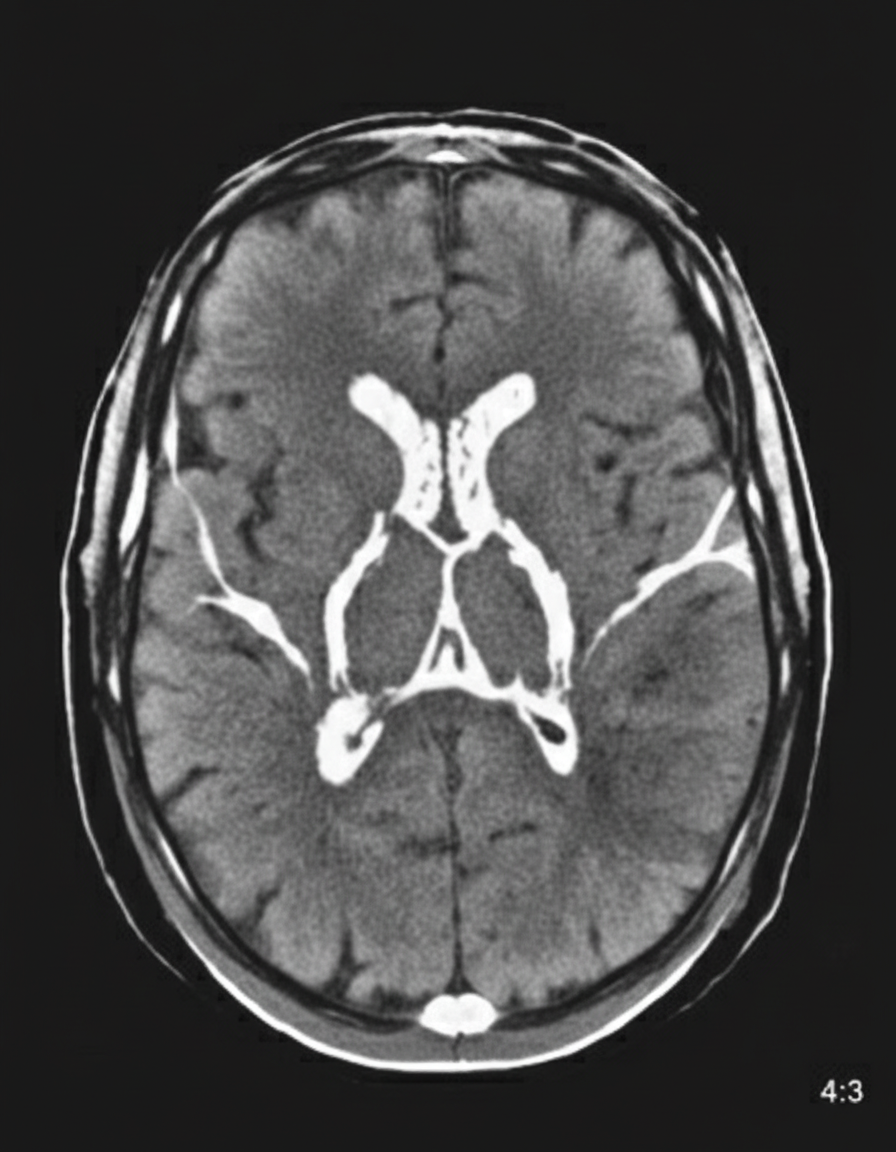
A 48-year-old woman is brought to the emergency department because of a 1-hour history of sudden-onset headache associated with nausea and vomiting. The patient reports she was sitting at her desk when the headache began. The headache is global and radiates to her neck. She has hypertension. She has smoked one pack of cigarettes daily for the last 10 years. She drinks alcohol occasionally. Her father had a stroke at the age 58 years. Current medications include hydrochlorothiazide. She is in severe distress. She is alert and oriented to person, place, and time. Her temperature is 38.2°C (100.8°F), pulse is 89/min, respirations are 19/min, and blood pressure is 150/90 mm Hg. Cardiopulmonary examination shows no abnormalities. Cranial nerves II–XII are intact. She has no focal motor or sensory deficits. She flexes her hips and knees when her neck is flexed while lying in a supine position. A CT scan of the head is shown. Which of the following is the most appropriate intervention?
A 23-year-old man comes to the emergency department with an open wound on his right hand. He states that he got into a bar fight about an hour ago. He appears heavily intoxicated and does not remember the whole situation, but he does recall lying on the ground in front of the bar after the fight. He does not recall any history of injuries but does remember a tetanus shot he received 6 years ago. His temperature is 37°C (98.6°F), pulse is 77/min, and blood pressure is 132/78 mm Hg. Examination shows a soft, nontender abdomen. His joints have no bony deformities and display full range of motion. There is a 4-cm (1.6-in) lesion on his hand with the skin attached only on the ulnar side. The wound, which appears to be partly covered with soil and dirt, is irrigated and debrided by the hospital staff. Minimal erythema and no purulence is observed in the area surrounding the wound. What is the most appropriate next step in management?
A 43-year-old man is brought to the emergency department 40 minutes after falling off a 10-foot ladder. He has severe pain and swelling of his right ankle and is unable to walk. He did not lose consciousness after the fall. He has no nausea. He appears uncomfortable. His temperature is 37°C (98.6°F), pulse is 98/min, respirations are 16/min, and blood pressure is 110/80 mm Hg. He is alert and oriented to person, place, and time. Examination shows multiple abrasions over both lower extremities. There is swelling and tenderness of the right ankle; range of motion is limited by pain. The remainder of the examination shows no abnormalities. An x-ray of the ankle shows an extra-articular calcaneal fracture. Intravenous analgesia is administered. Which of the following is the most appropriate next step in the management of this patient?
Practice by Chapter
Chest trauma management
Practice Questions
Head trauma management
Practice Questions
Spinal trauma
Practice Questions
Blunt abdominal trauma
Practice Questions
Penetrating abdominal trauma
Practice Questions
Pelvic fractures and hemorrhage
Practice Questions
Extremity trauma and vascular injuries
Practice Questions
Burns assessment and management
Practice Questions
Traumatic shock management
Practice Questions
Resuscitative thoracotomy
Practice Questions
Focused Assessment with Sonography in Trauma (FAST)
Practice Questions
Trauma in pregnancy
Practice Questions
Pediatric trauma considerations
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
