Post-transplant infections — MCQs

A 26-year-old man comes to the physician for a follow-up examination. He was diagnosed with HIV infection 2 weeks ago. His CD4+ T-lymphocyte count is 162/mm3 (N ≥ 500). An interferon-gamma release assay is negative. Prophylactic treatment against which of the following pathogens is most appropriate at this time?
A 55-year-old woman recently underwent kidney transplantation for end-stage renal disease. Her early postoperative period was uneventful, and her serum creatinine is lowered from 4.3 mg/dL (preoperative) to 2.5 mg/dL. She is immediately started on immunosuppressive therapy. On postoperative day 7, she presents to the emergency department (ED) because of nausea, fever, abdominal pain at the transplant site, malaise, and pedal edema. The vital signs include: pulse 106/min, blood pressure 167/96 mm Hg, respirations 26/min, and temperature 40.0°C (104.0°F). The surgical site shows no signs of infection. Her urine output is 250 mL over the past 24 hours. Laboratory studies show: Hematocrit 33% White blood cell (WBC) count 6700/mm3 Blood urea 44 mg/dL Serum creatinine 3.3 mg/dL Serum sodium 136 mEq/L Serum potassium 5.6 mEq/L An ultrasound of the abdomen shows collection of fluid around the transplanted kidney with moderate hydronephrosis. Which of the following initial actions is the most appropriate?
An investigator is conducting a study to identify potential risk factors for post-transplant hypertension. The investigator selects post-transplant patients with hypertension and gathers detailed information regarding their age, gender, preoperative blood pressure readings, and current medications. The results of the study reveal that some of the patients had been treated with cyclosporine. This study is best described as which of the following?
A 56-year-old man comes to the emergency department because of progressively worsening shortness of breath and fever for 2 days. He also has a nonproductive cough. He does not have chest pain or headache. He has chronic myeloid leukemia and had a bone marrow transplant 3 months ago. His current medications include busulfan, mycophenolate mofetil, tacrolimus, and methylprednisolone. His temperature is 38.1°C (100.6°F), pulse is 103/min, respirations are 26/min, and blood pressure is 130/70 mm Hg. Pulse oximetry on room air shows an oxygen saturation of 93%. Pulmonary examination shows diffuse crackles. The spleen tip is palpated 4 cm below the left costal margin. Laboratory studies show: Hemoglobin 10.3 g/dL Leukocyte count 4,400/mm3 Platelet count 160,000/mm3 Serum Glucose 78 mg/dL Creatinine 2.1 mg/dL D-dimer 96 ng/mL (N < 250) pp65 antigen positive Galactomannan antigen negative Urinalysis is normal. An x-ray of the chest shows diffuse bilateral interstitial infiltrates. An ECG shows sinus tachycardia. Which of the following is the most appropriate pharmacotherapy?
A 33-year-old HIV-positive male is seen in clinic for follow-up care. When asked if he has been adhering to his HIV medications, the patient exclaims that he has been depressed, thus causing him to not take his medication for six months. His CD4+ count is now 33 cells/mm3. What medication(s) should he take in addition to his anti-retroviral therapy?
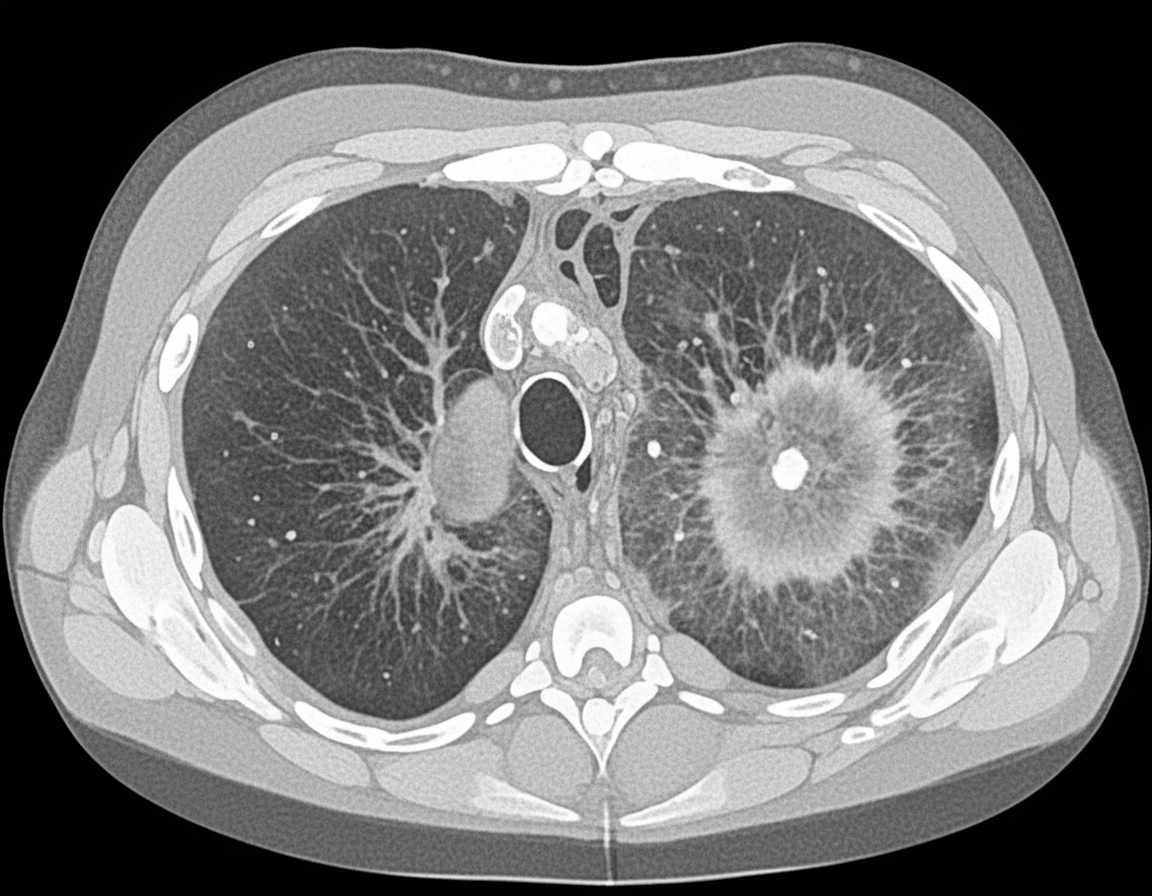
A 26-year-old man is undergoing a bone marrow transplantation for treatment of a non-Hodgkin lymphoma that has been refractory to several rounds of chemotherapy and radiation over the past 2 years. He has been undergoing a regimen of cyclophosphamide and total body irradiation for the past several weeks in anticipation of his future transplant. This morning, he reports developing a productive cough and is concerned because he noted some blood in his sputum this morning. The patient also reports pain with inspiration. His temperature is 101°F (38.3°C), blood pressure is 115/74 mmHg, pulse is 120/min, respirations are 19/min, and oxygen saturation is 98% on room air. A chest radiograph and CT are obtained and shown in Figures A and B respectively. Which of the following is the most likely diagnosis?
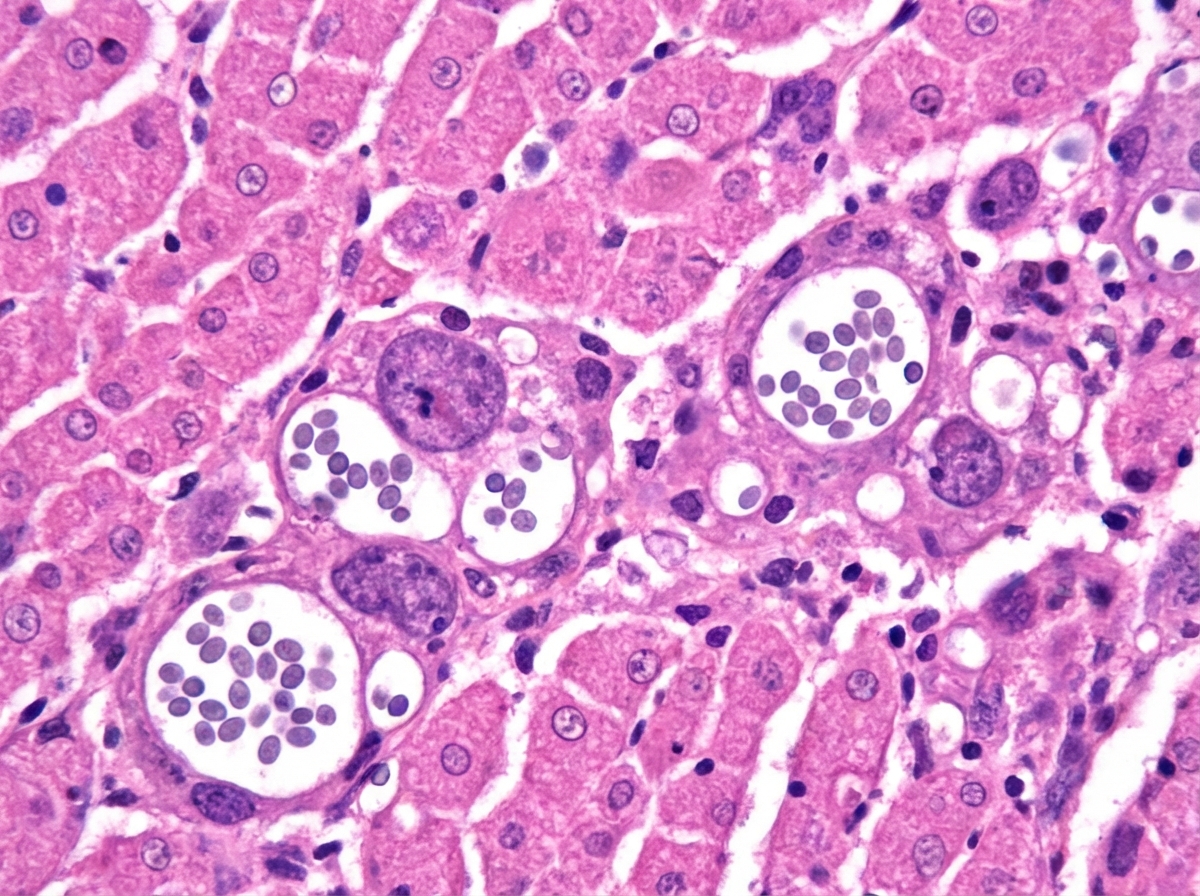
A 55-year-old man comes to the physician because of fever, fatigue, dry cough, headache, and myalgia over the past week. Two days ago, he developed several painful oral lesions and difficulty swallowing. He underwent kidney transplantation 3 years ago. His temperature is 38.2°C (100.7°F). Physical examination shows bilateral rales, hepatosplenomegaly, and multiple 1–2 cm ulcerative lesions with raised borders in the oral mucosa. A photomicrograph of a liver biopsy specimen is shown. Which of the following is the most likely causal pathogen?
A 14-year-old boy has undergone kidney transplantation due to stage V chronic kidney disease. A pre-transplantation serologic assessment showed that he is negative for past or present HIV infection, viral hepatitis, EBV, and CMV infection. He has a known allergy for macrolides. The patient has no complaints 1 day after transplantation. His vital signs include: blood pressure 120/70 mm Hg, heart rate 89/min, respiratory rate 17/min, and temperature 37.0°C (98.6°F). On physical examination, the patient appears to be pale, his lungs are clear on auscultation, heart sounds are normal, and his abdomen is non-tender on palpation. His creatinine is 0.65 mg/dL (57.5 µmol/L), GFR is 71.3 mL/min/1.73 m2, and urine output is 0.9 mL/kg/h. Which of the following drugs should be used in the immunosuppressive regimen in this patient?
A 66-year-old man is transferred from another hospital after 3 days of progressively severe headache, vomiting, low-grade fever, and confusion. According to his partner, the patient has been dealing with some memory loss and complaining about headaches for the past 2 weeks. He has a history of interstitial pulmonary disease that required lung transplantation 2 years ago. Upon admission, he is found with a blood pressure of 160/100 mm Hg, a pulse of 58/min, a respiratory rate of 15/min, and a body temperature of 36°C (97°F). During the examination, he is found with oral thrush and symmetric and reactive pupils; there are no focal neurological signs or papilledema. A lumbar puncture is performed. Which of the following features would be expected to be found in this case?
A 24-year-old man is brought to the emergency department 30 minutes after being involved in a high-speed motor vehicle collision in which he was a restrained driver. On arrival, he is alert and oriented. His pulse is 112/min, respirations are 29/min, and blood pressure is 100/60 mm Hg. The pupils are equal and reactive to light. There is a 3-cm laceration over the forehead and multiple bruises over the trunk. The lungs are clear to auscultation. Cardiac examination shows no abnormalities. The abdomen is soft and nontender. The right knee is swollen and tender; range of motion is limited by pain. Infusion of 0.9% saline is begun and intravenous acetaminophen is administered. Two hours later, blood-tinged fluid spontaneously drains from both nostrils, and is made worse by leaning forward. On a piece of gauze, it shows up as a rapidly-expanding clear ring of fluid surrounding blood. Further evaluation of this patient is most likely to show which of the following?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
