Lung transplantation — MCQs

A 48-year-old Caucasian male suffering from ischemic heart disease is placed on a heart transplant list. Months later, he receives a heart from a matched donor. During an endomyocardial biopsy performed 3 weeks later, there is damage consistent with acute graft rejection. What is most likely evident on the endomyocardial biopsy?
A 31-year-old female receives a kidney transplant for autosomal dominant polycystic kidney disease (ADPKD). Three weeks later, the patient experiences acute, T-cell mediated rejection of the allograft and is given sirolimus. Which of the following are side effects of this medication?
A 40-year-old male with a history of chronic alcoholism recently received a liver transplant. Two weeks following the transplant, the patient presents with a skin rash and frequent episodes of bloody diarrhea. A colonoscopy is performed and biopsy reveals apoptosis of colonic epithelial cells. What is most likely mediating these symptoms?
A 24-year-old male with cystic fibrosis is brought to the emergency room by his mother after he had difficulty breathing. He previously received a lung transplant 6 months ago and was able to recover quickly from the operation. He is compliant with all of his medications and had been doing well with no major complaints until 2 weeks ago when he began to experience shortness of breath. Exam reveals a decreased FEV1/FVC ratio and biopsy reveals lymphocytic infiltration. Which of the following components is present in the airway zone characteristically affected by the most likely cause of this patient's symptoms?
An investigator studying immune-mediated pulmonary damage performs an autopsy on a bilateral lung transplant recipient who died of hypercapnic respiratory failure. The patient underwent lung transplantation for idiopathic pulmonary fibrosis. Microscopic examination of the lung shows diffuse eosinophilic scarring of the terminal and respiratory bronchioles and near-complete luminal obliteration by polypoidal plugs of granulation tissue. Examination of the skin shows no abnormalities. The findings in this patient are most consistent with which of the following conditions?
In which of the following pathological states would the oxygen content of the trachea resemble the oxygen content in the affected alveoli?
A 58-year-old man is brought to the emergency department because of confusion, weight loss, and anuria. He has chronic kidney disease, hypertension, and type 2 diabetes mellitus. He was diagnosed with acute lymphoblastic leukemia at the age of 8 years and was treated with an allogeneic stem cell transplantation. He is HIV-positive and has active hepatitis C virus infection. He drinks around 8 cans of beer every week. His current medications include tenofovir, emtricitabine, atazanavir, daclatasvir, sofosbuvir, insulin, amlodipine, and enalapril. He appears lethargic. His temperature is 36°C (96.8°F), pulse is 130/min, respirations are 26/min, and blood pressure is 145/90 mm Hg. Examination shows severe edema in his legs and generalized muscular weakness. Auscultation of the lung shows crepitant rales. Laboratory studies show positive HCV antibody and positive HCV RNA. His HIV viral load is undetectable and his CD4+ T-lymphocyte count is 589/μL. Six months ago, his CD4+ T-lymphocyte count was 618/μL. An ECG of the heart shows arrhythmia with frequent premature ventricular contractions. Arterial blood gas analysis on room air shows: pH 7.23 PCO2 31 mm Hg HCO3- 13 mEq/L Base excess -12 mEq/L The patient states he would like to donate organs or tissues in the case of his death. Which of the following is an absolute contraindication for organ donation in this patient?
A 45-year-old man with a 5-year history of worsening shortness of breath and cough comes to the physician for a follow-up examination. He has never smoked. His pulse is 75/min, blood pressure is 130/65 mm Hg, and respirations are 25/min. Examination shows an increased anteroposterior diameter of the chest. Diminished breath sounds and wheezing are heard on auscultation of the chest. An x-ray of the chest shows widened intercostal spaces, a flattened diaphragm, and basilar-predominant bullous changes of the lungs. This patient is at increased risk for which of the following complications?
A 66-year-old man is transferred from another hospital after 3 days of progressively severe headache, vomiting, low-grade fever, and confusion. According to his partner, the patient has been dealing with some memory loss and complaining about headaches for the past 2 weeks. He has a history of interstitial pulmonary disease that required lung transplantation 2 years ago. Upon admission, he is found with a blood pressure of 160/100 mm Hg, a pulse of 58/min, a respiratory rate of 15/min, and a body temperature of 36°C (97°F). During the examination, he is found with oral thrush and symmetric and reactive pupils; there are no focal neurological signs or papilledema. A lumbar puncture is performed. Which of the following features would be expected to be found in this case?
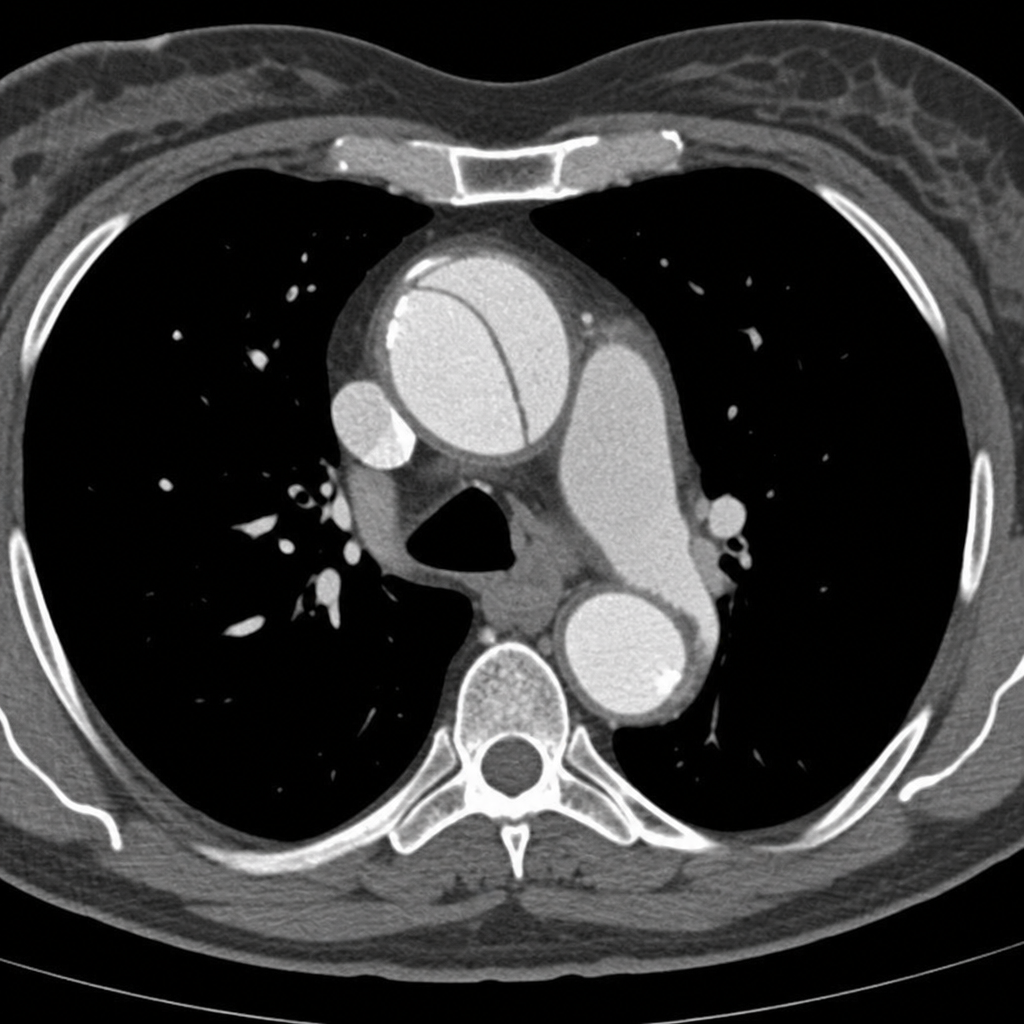
A 45-year-old woman presents to the emergency department with sudden-onset severe tearing chest pain radiating to the interscapular region. Her blood pressure is 178/96 mmHg in the right arm and 142/80 mmHg in the left arm. She is diaphoretic and in moderate distress. A CT angiogram of the chest is obtained and demonstrates an intimal flap involving the ascending aorta, consistent with a Stanford Type A aortic dissection. Based on the imaging findings, which of the following is the most appropriate next step in management?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
