Immunosuppression principles — MCQs

A 56-year-old man comes to the emergency department because of progressively worsening shortness of breath and fever for 2 days. He also has a nonproductive cough. He does not have chest pain or headache. He has chronic myeloid leukemia and had a bone marrow transplant 3 months ago. His current medications include busulfan, mycophenolate mofetil, tacrolimus, and methylprednisolone. His temperature is 38.1°C (100.6°F), pulse is 103/min, respirations are 26/min, and blood pressure is 130/70 mm Hg. Pulse oximetry on room air shows an oxygen saturation of 93%. Pulmonary examination shows diffuse crackles. The spleen tip is palpated 4 cm below the left costal margin. Laboratory studies show: Hemoglobin 10.3 g/dL Leukocyte count 4,400/mm3 Platelet count 160,000/mm3 Serum Glucose 78 mg/dL Creatinine 2.1 mg/dL D-dimer 96 ng/mL (N < 250) pp65 antigen positive Galactomannan antigen negative Urinalysis is normal. An x-ray of the chest shows diffuse bilateral interstitial infiltrates. An ECG shows sinus tachycardia. Which of the following is the most appropriate pharmacotherapy?
A 37-year-old man who had undergone liver transplantation 7 years ago, presents to the physician because of yellowish discoloration of the skin, sclera, and urine. He is on regular immunosuppressive therapy and is well-adherent to the treatment. He has no comorbidities and is not taking any other medication. He provides a history of similar episodes of yellowish skin discoloration 6–7 times since he underwent liver transplantation. Physical examination shows clinical jaundice. Laboratory studies show: While blood cell (WBC) count 4,400/mm3 Hemoglobin 11.1 g/dL Serum creatinine 0.9 mg/dL Serum bilirubin (total) 44 mg/dL Aspartate transaminase (AST) 1,111 U/L Alanine transaminase (ALT) 671 U/L Serum gamma-glutamyl transpeptidase 777 U/L Alkaline phosphatase 888 U/L Prothrombin time 17 seconds A Doppler ultrasound shows significantly reduced blood flow into the transplanted liver. A biopsy of the transplanted liver is likely to show which of the following histological features?
A 43-year-old woman comes to the office with a 5-day history of a rash. She's had a rash across her neck, shoulders, and the palms of her hands for the past five days. She's also had large-volume watery diarrhea for the same period of time. Past medical history is notable for acute myeloid leukemia, for which she received a stem cell transplant from a donor about two months prior. Physical exam reveals a faint red maculopapular rash across her neck, shoulders, and hands, as well as an enlarged liver and spleen. Labs are notable for a total bilirubin of 10. Which of the following is the mechanism of this patient's pathology?
A 14-year-old boy has undergone kidney transplantation due to stage V chronic kidney disease. A pre-transplantation serologic assessment showed that he is negative for past or present HIV infection, viral hepatitis, EBV, and CMV infection. He has a known allergy for macrolides. The patient has no complaints 1 day after transplantation. His vital signs include: blood pressure 120/70 mm Hg, heart rate 89/min, respiratory rate 17/min, and temperature 37.0°C (98.6°F). On physical examination, the patient appears to be pale, his lungs are clear on auscultation, heart sounds are normal, and his abdomen is non-tender on palpation. His creatinine is 0.65 mg/dL (57.5 µmol/L), GFR is 71.3 mL/min/1.73 m2, and urine output is 0.9 mL/kg/h. Which of the following drugs should be used in the immunosuppressive regimen in this patient?
A 29-year-old female presents to her gynecologist complaining of a painful rash around her genitals. She has multiple sexual partners and uses condoms intermittently. Her last STD screen one year ago was negative. On examination, she has bilateral erosive vesicles on her labia majora and painful inguinal lymphadenopathy. She is started on an oral medication that requires a specific thymidine kinase for activation. Which of the following adverse effects is associated with this drug?
Fourteen days after a laparoscopic cholecystectomy for cholelithiasis, a 45-year-old woman comes to the emergency department because of persistent episodic epigastric pain for 3 days. The pain radiates to her back, occurs randomly throughout the day, and is associated with nausea and vomiting. Each episode lasts 30 minutes to one hour. Antacids do not improve her symptoms. She has hypertension and fibromyalgia. She has smoked 1–2 packs of cigarettes daily for the past 10 years and drinks 4 cans of beer every week. She takes lisinopril and pregabalin. She appears uncomfortable. Her temperature is 37°C (98.6° F), pulse is 84/min, respirations are 14/min, and blood pressure is 127/85 mm Hg. Abdominal examination shows tenderness to palpation in the upper quadrants without rebound or guarding. Bowel sounds are normal. The incisions are clean, dry, and intact. Serum studies show: AST 80 U/L ALT 95 U/L Alkaline phosphatase 213 U/L Bilirubin, total 1.3 mg/dL Direct 0.7 mg/dL Amylase 52 U/L Abdominal ultrasonography shows dilation of the common bile duct and no gallstones. Which of the following is the most appropriate next step in management?
A 31 year-old-man presents to an urgent care clinic with symptoms of lower abdominal pain, bloating, bloody diarrhea, and fullness, all of which have become more frequent over the last 3 months. Rectal examination reveals a small amount of bright red blood. His vital signs include: temperature 36.7°C (98.0°F), blood pressure 126/74 mm Hg, heart rate 74/min, and respiratory rate 14/min. Colonoscopy is performed, showing extensive mucosal erythema, induration, and pseudopolyps extending from the rectum to the splenic flexure. Given the following options, what is the most appropriate treatment to induce remission in this patient?
Five days after undergoing right knee arthroplasty for osteoarthritis, a 68-year-old man has severe pain in his right knee preventing him from participating in physical therapy. On the third postoperative day when the dressing was changed, the surgical wound appeared to be intact, slightly swollen, and had a clear secretion. He has a history of diabetes, hyperlipidemia, and hypertension. Current medications include metformin, enalapril, and simvastatin. His temperature is 37.3°C (99.1°F), pulse is 94/min, and blood pressure is 130/88 mm Hg. His right knee is swollen, erythematous, and tender to palpation. There is pain on movement of the joint. The medial parapatellar skin incision appears superficially opened in its proximal and distal part with yellow-green discharge. There is blackening of the skin on both sides of the incision. Which of the following is the next best step in the management of this patient?
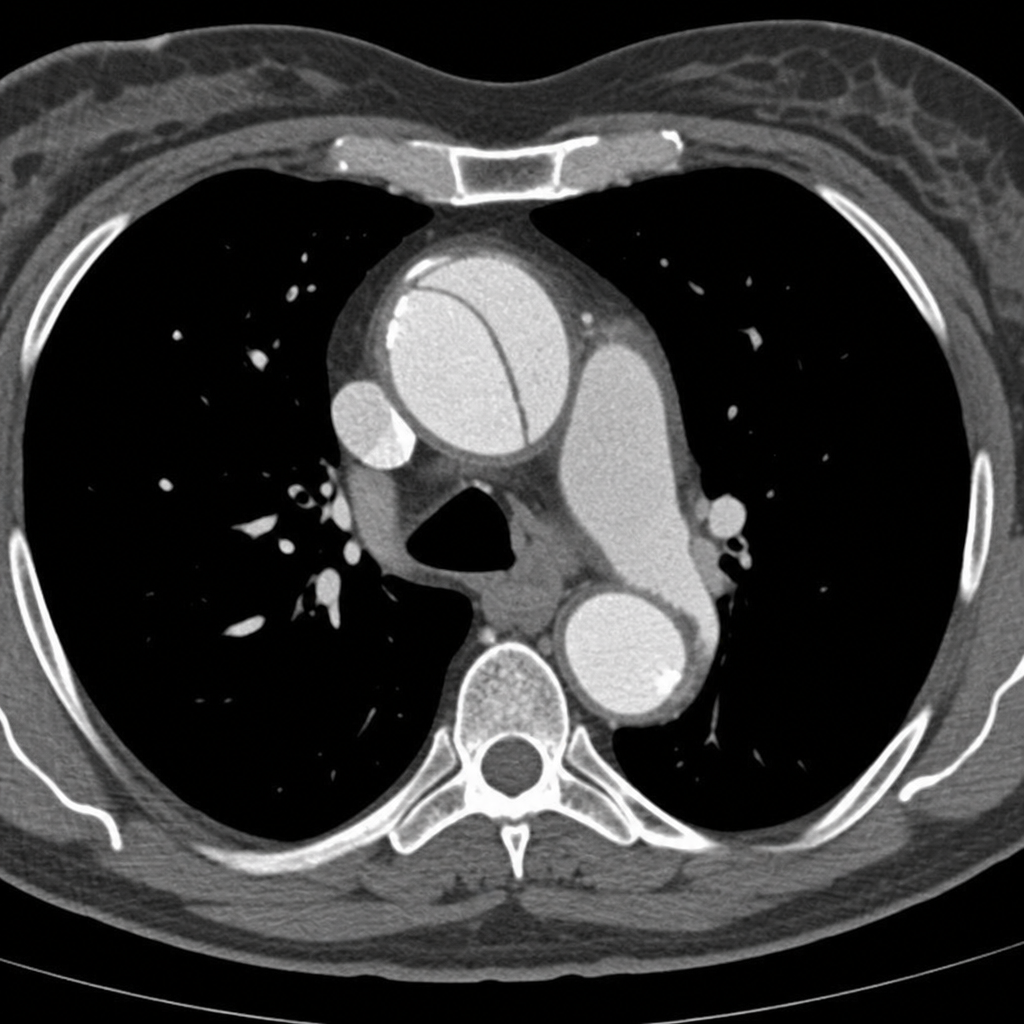
A 45-year-old woman presents to the emergency department with sudden-onset severe tearing chest pain radiating to the interscapular region. Her blood pressure is 178/96 mmHg in the right arm and 142/80 mmHg in the left arm. She is diaphoretic and in moderate distress. A CT angiogram of the chest is obtained and demonstrates an intimal flap involving the ascending aorta, consistent with a Stanford Type A aortic dissection. Based on the imaging findings, which of the following is the most appropriate next step in management?
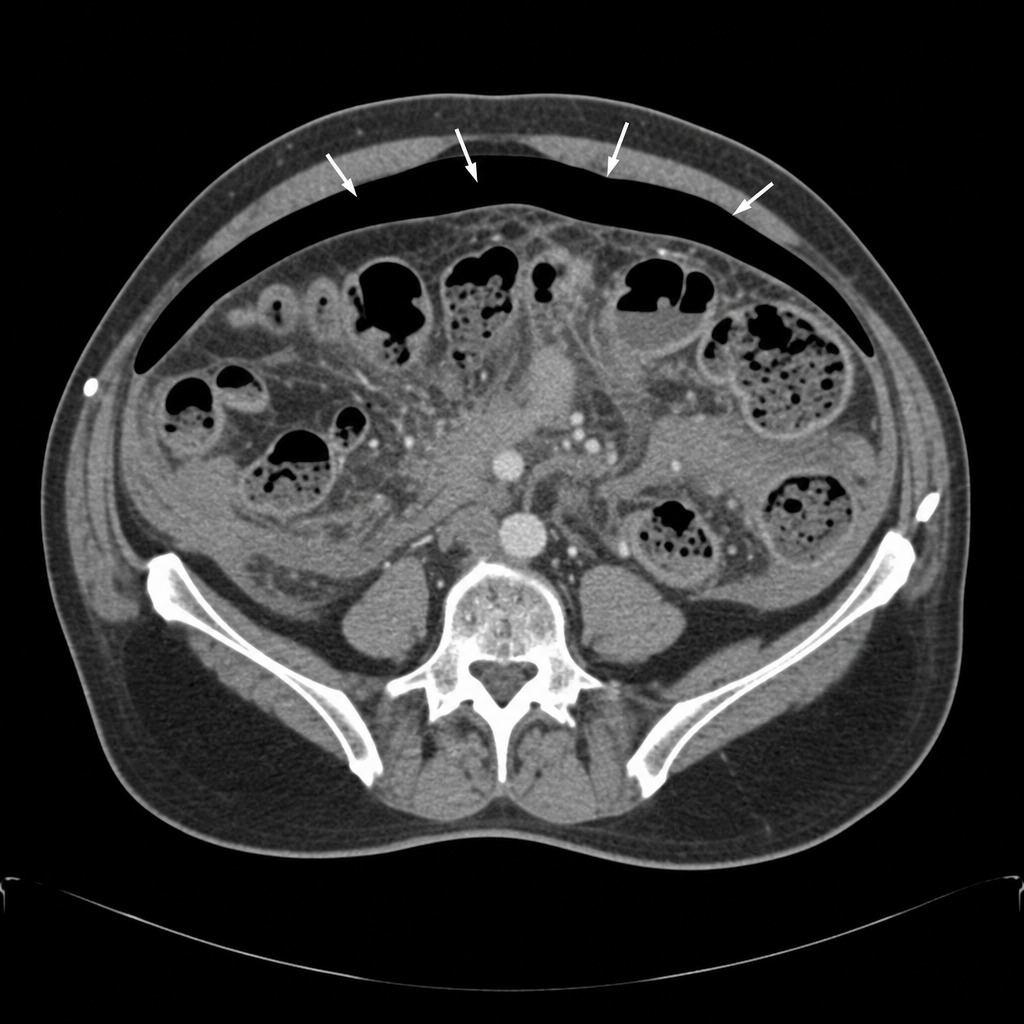
A 58-year-old woman undergoes an elective sigmoid colectomy for recurrent diverticulitis. On postoperative day 6, she develops a temperature of 38.9°C, HR of 118 bpm, and BP of 88/54 mmHg despite 2L of IV fluid resuscitation. She complains of worsening lower abdominal pain. Her abdomen is diffusely tender with guarding and rigidity. WBC is 19,500/µL. A CT scan of the abdomen and pelvis with contrast demonstrates free intraperitoneal air and diffuse pelvic fluid consistent with an uncontained anastomotic leak. Based on the CT findings, what is the most appropriate next step in management?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
