Post-op care — MCQs

On this page
A 56-year-old woman comes to the physician because she palpated a mass in her right breast during self-examination a week ago. Menarche was at the age of 14, and her last menstrual period was at the age of 51. Vital signs are within normal limits. Examination shows a nontender, firm and hard mass in the upper outer quadrant of the right breast. Mammography shows large, dense breasts, with a 1.7-cm mass in the right upper outer quadrant. The patient undergoes right upper outer quadrant lumpectomy with subsequent sentinel node biopsy, which reveals moderately differentiated invasive ductal carcinoma and micrometastasis to one axillary lymph node. There is no evidence of extranodal metastasis. The tumor tests positive for both estrogen and progesterone receptors and does not show human epidermal growth factor receptor 2 (HER2) over-expression. Flow-cytometry reveals aneuploid tumor cells. Which of the following factors has the greatest effect on this patient's prognosis?
A 59-year-old woman presents to her primary care provider with a 6-month history of progressive left-arm swelling. Two years ago she had a partial mastectomy and axillary lymph node dissection for left breast cancer. She was also treated with radiotherapy at the time. Upon further questioning, she denies fever, pain, or skin changes, but reports difficulty with daily tasks because her hand feels heavy and weak. She is bothered by the appearance of her enlarged extremity and has stopped playing tennis. On physical examination, nonpitting edema of the left arm is noted with hyperkeratosis, papillomatosis, and induration of the skin. Limb elevation, exercise, and static compression bandaging are started. If the patient has no improvement, which of the following will be the best next step?
A 23-year-old woman presents to the physician with complaints of pain and paresthesias in her left hand, particularly her thumb, index, and middle fingers. She notes that the pain is worse at night, though she still feels significant discomfort during the day. The patient insists that she would like urgent relief of her symptoms, as the pain is keeping her from carrying out her daily activities. On physical examination, pain and paresthesias are elicited when the physician percusses the patient’s wrist as well as when the patient is asked to flex both of her palms at the wrist. Which of the following is the most appropriate initial step in the management of this patient’s condition?
A 56-year-old woman is one week status post abdominal hysterectomy when she develops a fever of 101.4°F (38.6°C). Her past medical history is significant for type II diabetes mellitus and a prior history of alcohol abuse. The operative report and intraoperative cystoscopy indicate that the surgery was uncomplicated. The nurse reports that since the surgery, the patient has also complained of worsening lower abdominal pain. She has given the patient the appropriate pain medications with little improvement. The patient has tolerated an oral diet well and denies nausea, vomiting, or abdominal distension. Her blood pressure is 110/62 mmHg, pulse is 122/min, and respirations are 14/min. Since being given 1000 mL of intravenous fluids yesterday, the patient has excreted 800 mL of urine. On physical exam, she is uncomfortable, shivering, and sweating. The surgical site is intact, but the surrounding skin appears red. No drainage is appreciated. The abdominal examination reveals tenderness to palpation and hypoactive bowel sounds. Labs and a clean catch urine specimen are obtained as shown below: Leukocyte count and differential: Leukocyte count: 18,000/mm^3 Segmented neutrophils: 80% Bands: 10% Eosinophils: 1% Basophils: < 1% Lymphocytes: 5% Monocytes: 4% Platelet count: 300,000/mm^3 Hemoglobin: 12.5 g/dL Hematocrit: 42% Urine: Epithelial cells: 15/hpf Glucose: positive RBC: 1/hpf WBC: 2/hpf Bacteria: 50 cfu/mL Ketones: none Nitrites: negative Leukocyte esterase: negative Which of the following is most likely the cause of this patient’s symptoms?
Eight hours after undergoing an open right hemicolectomy and a colostomy for colon cancer, a 52-year-old man has wet and bloody surgical dressings. He has had episodes of blood in his stools during the past 6 months, which led to the detection of colon cancer. He has hypertension and ischemic heart disease. His younger brother died of a bleeding disorder at the age of 16. The patient has smoked one pack of cigarettes daily for 36 years and drinks three to four beers daily. Prior to admission, his medications included aspirin, metoprolol, enalapril, and simvastatin. Aspirin was stopped 7 days prior to the scheduled surgery. He appears uncomfortable. His temperature is 36°C (96.8°F), pulse is 98/min, respirations are 14/min, and blood pressure is 118/72 mm Hg. Examination shows a soft abdomen with a 14-cm midline incision that has severe oozing of blood from its margins. The colostomy bag has some blood collected within. Laboratory studies show: Hemoglobin 12.3 g/dL Leukocyte count 11,200/mm3 Platelet count 210,000/mm3 Bleeding time 4 minutes Prothrombin time 15 seconds (INR=1.1) Activated partial thromboplastin time 36 seconds Serum Urea nitrogen 30 mg/dL Glucose 96 mg/dL Creatinine 1.1 mg/dL AST 48 U/L ALT 34 U/L γ-Glutamyltransferase 70 U/L (N= 5–50 U/L) Which of the following is the most likely cause of this patient's bleeding?
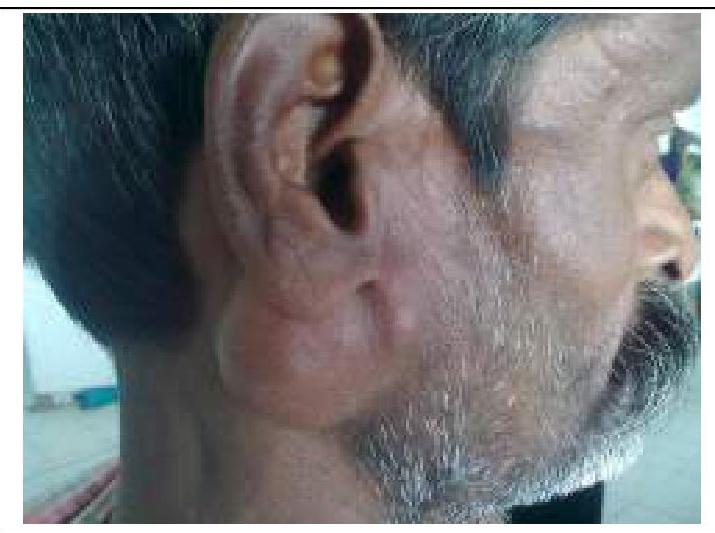
A 26-year-old woman presents to the medicine clinic with swelling around the right side of her chin and neck (Image A). She reports pain when moving her jaw and chewing. Her symptoms developed two days after receiving an uncomplicated tonsillectomy. She has been followed by a general medical physician since birth and has received all of her standard health maintenance procedures. Vital signs are stable with the exception of a temperature of 38.4 degrees Celcius. The area in question on the right side is exquisitely tender. The remainder of her exam is benign. What is the most likely diagnosis?
A 68-year-old woman comes to the physician because of a 3-month history of an oozing, red area above the left ankle. She does not recall any trauma to the lower extremity. She has type 2 diabetes mellitus, hypertension, atrial fibrillation, and ulcerative colitis. She had a myocardial infarction 2 years ago and a stroke 7 years ago. She has smoked 2 packs of cigarettes daily for 48 years and drinks 2 alcoholic beverages daily. Current medications include warfarin, metformin, aspirin, atorvastatin, carvedilol, and mesalamine. She is 165 cm (5 ft 4 in) tall and weighs 67 kg (148 lb); BMI is 24.6 kg/m2. Her temperature is 36.7°C (98°F), pulse is 90/min, respirations are 12/min, and blood pressure is 135/90 mm Hg. Examination shows yellow-brown spots and dilated tortuous veins over the lower extremities. The feet and the left calf are edematous. Femoral, popliteal, and pedal pulses are palpable bilaterally. There is a 3-cm (1.2-in) painless, shallow, exudative ulcer surrounded by granulation tissue above the medial left ankle. There is slight drooping of the right side of the face. Which of the following is the most likely cause of this patient's ulcer?
A 27-year-old man comes to the physician because of intermittent right shoulder pain for the past 2 weeks. The pain awakens him at night and is worse when he lies on the right shoulder. He does not have any paresthesia or numbness in the right arm. He is a painter, and these episodes of pain have not allowed him to work efficiently. He appears healthy. Vital signs are within normal limits. Examination shows painful abduction of the arm above the shoulder. There is severe pain when the elbow is flexed and the right shoulder is internally rotated. Elevation of the internally rotated and outstretched arm causes pain over the anterior lateral aspect of the shoulder. An x-ray of the shoulder shows no abnormalities. Injection of 5 mL of 1% lidocaine into the right subacromial space relieves the pain and increases the range of motion of the right arm. Which of the following is the most appropriate next step in management?
A 43-year-old woman comes to the physician because of a 3-month history of a painless ulcer on the sole of her right foot. There is no history of trauma. She has been dressing the ulcer once daily at home with gauze. She has a 15-year history of poorly-controlled type 1 diabetes mellitus and hypertension. Current medications include insulin and lisinopril. Vital signs are within normal limits. Examination shows a 2 x 2-cm ulcer on the plantar aspect of the base of the great toe with whitish, loose tissue on the floor of the ulcer and a calloused margin. A blunt metal probe reaches the deep plantar space. Sensation to vibration and light touch is decreased over both feet. Pedal pulses are intact. An x-ray of the right foot shows no abnormalities. Which of the following is the most appropriate initial step in management?
A 47-year-old woman comes to the physician for a mass in her left breast she noticed 2 days ago during breast self-examination. She has hypothyroidism treated with levothyroxine. There is no family history of breast cancer. Examination shows large, moderately ptotic breasts. The mass in her left breast is small (approximately 1 cm x 0.5 cm), firm, mobile, and painless. It is located 4 cm from her nipple-areolar complex at the 7 o'clock position. There are no changes in the skin or nipple, and there is no palpable axillary adenopathy. No masses are palpable in her right breast. A urine pregnancy test is negative. Mammogram showed a soft tissue mass with poorly defined margins. Core needle biopsy confirms a low-grade infiltrating ductal carcinoma. The pathological specimen is positive for estrogen receptors and negative for progesterone and human epidermal growth factor receptor 2 (HER2) receptors. Staging shows no distant metastatic disease. Which of the following is the most appropriate next step in management?
Practice by Chapter
Immediate post-anesthesia care
Practice Questions
Postoperative pain management
Practice Questions
Fluid and electrolyte management
Practice Questions
Nutrition support in surgical patients
Practice Questions
Wound care principles
Practice Questions
Drain management
Practice Questions
Early mobilization protocols
Practice Questions
Postoperative fever evaluation
Practice Questions
Recognition and management of SSIs
Practice Questions
DVT prophylaxis
Practice Questions
Enhanced recovery after surgery (ERAS)
Practice Questions
Postoperative respiratory care
Practice Questions
Transition of care planning
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
