Congenital diaphragmatic hernia — MCQs

A 42-year-old woman presents to the emergency department in active labor. She has had no prenatal care and is unsure of the gestational age. Labor progresses rapidly and spontaneous vaginal delivery of a baby boy occurs 3 hours after presentation. On initial exam, the child is 1.9 kg (4.2 lb) with a small head and jaw. A sac-like structure containing intestine, as can be seen in the picture, protrudes from the abdominal wall. What complication is closely associated with this presentation?
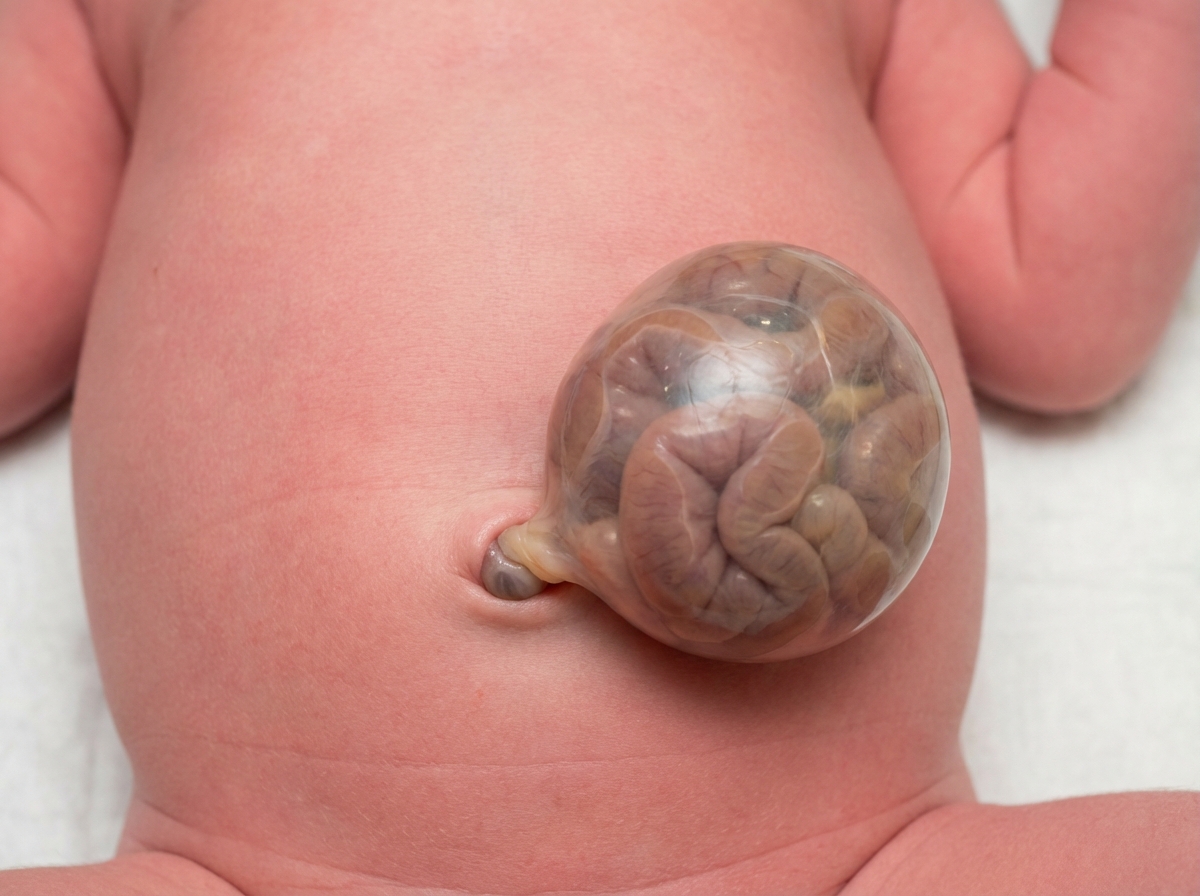
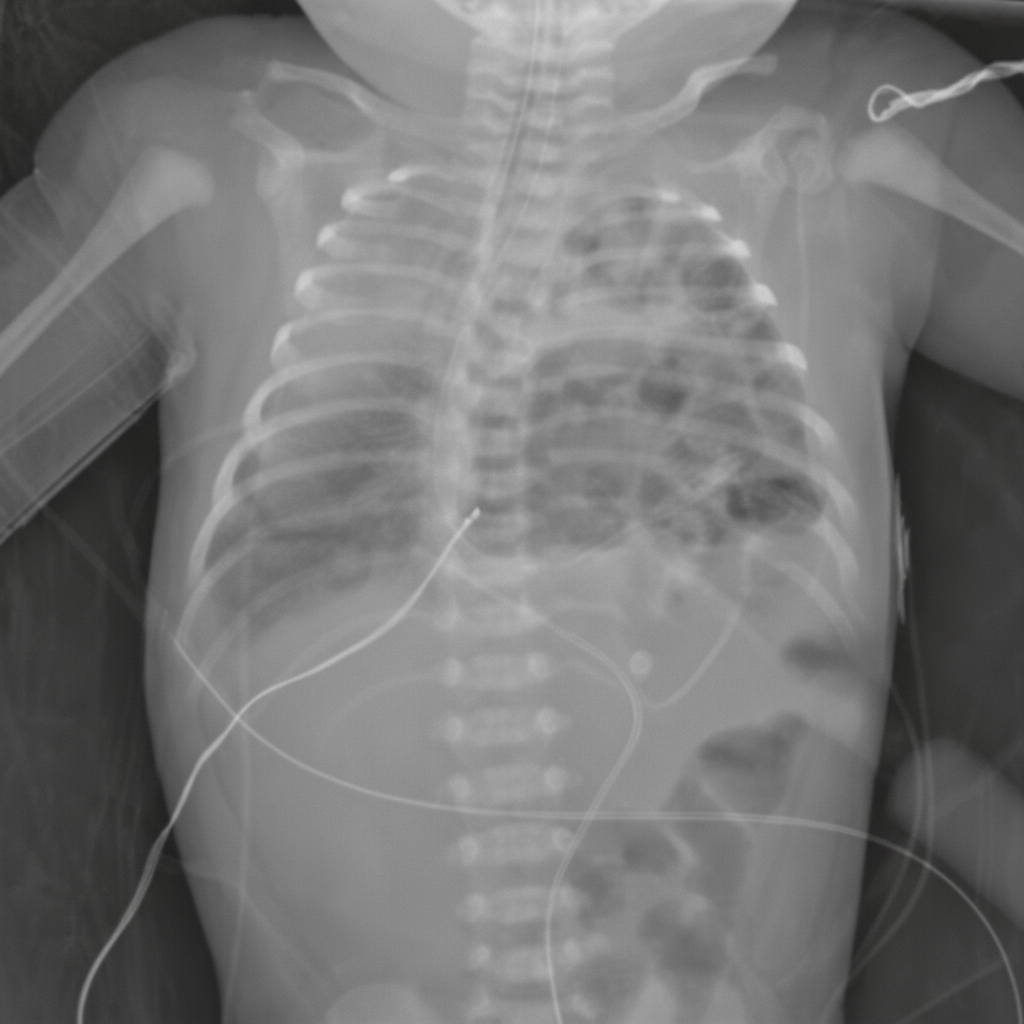
A 3900-g (8.6-lb) newborn is delivered at 38 weeks' gestation to a 27-year-old woman, gravida 3, para 2, via spontaneous vaginal delivery. Immediately after delivery, he spontaneously cries, grimaces, and moves all four extremities. Over the next five minutes, he becomes cyanotic, dyspneic, and tachypneic. Mask ventilation with 100% oxygen is begun, but ten minutes after delivery the baby continues to appear cyanotic. His temperature is 37.2°C (99.0°F), pulse is 155/min, respirations are 65/min, and blood pressure is 90/60 mm Hg. Pulse oximetry on 100% oxygen mask ventilation shows an oxygen saturation of 83%. Breath sounds are normal on the right and absent on the left. Heart sounds are best heard in the right midclavicular line. The abdomen appears concave. An x-ray of the chest is shown below. Which of the following is the most appropriate initial step in the management of this patient?
An 8-year-old girl is brought to the emergency department by her parents with severe difficulty in breathing for an hour. She is struggling to breathe. She was playing outside with her friends, when she suddenly fell to the ground, out of breath. She was diagnosed with asthma one year before and has since been on treatment for it. At present, she is sitting leaning forward with severe retractions of the intercostal muscles. She is unable to lie down. Her parents mentioned that she has already taken several puffs of her inhaler since this episode began but without response. On physical examination, her lungs are hyperresonant to percussion and there is decreased air entry in both of her lungs. Her vital signs show: blood pressure 110/60 mm Hg, pulse 110/min, respirations 22/min, and a peak expiratory flow rate (PEFR) of 50%. She is having difficulty in communicating with the physician. Her blood is sent for evaluation and a chest X-ray is ordered. Her arterial blood gas reports are as follows: PaO2 50 mm Hg pH 7.38 PaCO2 47 mm Hg HCO3 27 mEq/L Which of the following is the most appropriate next step in management?
A 4-week-old infant is brought to the emergency department by his parents with violent vomiting. It started about 3 days ago and has slowly gotten worse. He vomits after most feedings but seems to keep some formula down. His mother notes that he is eager to feed between episodes and seems to be putting on weight. Other than an uncomplicated course of chlamydia conjunctivitis, the infant has been healthy. He was born at 39 weeks gestation via spontaneous vaginal delivery. He is up to date on all vaccines and is meeting all developmental milestones. The physical exam is significant for a palpable mass in the right upper quadrant. What is the first-line confirmatory diagnostic test and associated finding?
A two-month-old female presents to the emergency department for difficulty feeding. The patient was born at 38 weeks gestation to a 29-year-old primigravid via vaginal delivery. The newborn period has thus far been uncomplicated. The patient has been exclusively breastfed since birth. Her parents report that feeding had previously seemed to be going well, and the patient has been gaining weight appropriately. Over the past several days, the patient’s mother has noticed that the patient seems to tire out before the end of the feeding. She has also noticed that the patient begins to appear short of breath and has a bluish discoloration of her lips. The patient’s height and weight were in the 20th and 10th percentile at birth, respectively. Her current height and weight are in the 20th and 15th percentiles, respectively. Her temperature is 98.0°F (36.7°C), blood pressure is 60/48 mmHg, pulse is 143/min, and respirations are 40/min. On physical exam, the patient is in no acute distress and appears well developed. A systolic crescendo-decrescendo murmur can be heard at the left upper sternal border. Her abdomen is soft, non-tender, and non-distended. During the abdominal exam, the patient begins crying and develops cyanosis of the perioral region. Which of the following is the best initial test to diagnose this patient’s condition?
A 3580-g (7-lb 14-oz) male newborn is delivered at 36 weeks' gestation to a 26-year-old woman, gravida 2, para 1 after an uncomplicated pregnancy. His temperature is 36.7°C (98.1°F), heart rate is 96/min, and respirations are 55/min and irregular. Pulse oximetry on room air shows an oxygen saturation of 65% measured in the right hand. He sneezes and grimaces during suction of secretions from his mouth. There is some flexion movement. The trunk is pink and the extremities are blue. The cord is clamped and the newborn is dried and wrapped in a prewarmed towel. Which of the following is the most appropriate next best step in management?
A baby is born after the 32nd gestational week by cesarean delivery. The mother suffered from gestational diabetes; however, she had no other pregnancy-related diseases and was otherwise healthy. The baby has a blood pressure of 100/58 mm Hg, heart rate of 104/min, and oxygen saturation of 88%. The child has tachypnea, subcostal and intercostal retractions, nasal flaring, and cyanosis. The cyanosis is responding well to initial administration of oxygen. The nasogastric tube was positioned without problems. Which of the following is the most likely diagnosis?
A P2G1 diabetic woman is at risk of delivering at 29 weeks gestation. Her obstetrician counsels her that there is a risk the baby could have significant pulmonary distress after it is born. However, she states she will give the mother corticosteroids, which will help prevent this from occurring. Additionally, the obstetrician states she will perform a test on the amniotic fluid which will indicate the likelihood of the infant being affected by this syndrome. Which of the following ratios would be most predictive of the infant having pulmonary distress?
A 79-year-old man is admitted to the intensive care unit for hospital acquired pneumonia, a COPD flare, and acute heart failure requiring intubation and mechanical ventilation. On his first night in the intensive care unit, his temperature is 99.7°F (37.6°C), blood pressure is 107/58 mm Hg, and pulse is 150/min which is a sudden change from his previous vitals. Physical exam is notable for jugular venous distension and a rapid heart rate. The ventilator is checked and is functioning normally. Which of the following is the best next step in management for the most likely diagnosis?
A 27-year-old man presents to the emergency department with severe dyspnea and sharp chest pain that suddenly started an hour ago after he finished exercising. He has a history of asthma as a child, and he achieves good control of his acute attacks with Ventolin. On examination, his right lung field is hyperresonant along with diminished lung sounds. Chest wall motion during respiration is asymmetrical. His blood pressure is 105/67 mm Hg, respirations are 22/min, pulse is 78/min, and temperature is 36.7°C (98.0°F). The patient is supported with oxygen, given corticosteroids, and has had analgesic medications via a nebulizer. Considering the likely condition affecting this patient, what is the best step in management?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
