Pediatric Surgery — MCQs

On this page
A 6-year-old baby is brought to the hospital by her parents complaining about right upper quadrant pain. On examination the baby is found to have jaundice and palpable abdominal mass. USG of the baby is shown below. What is the most likely cause?
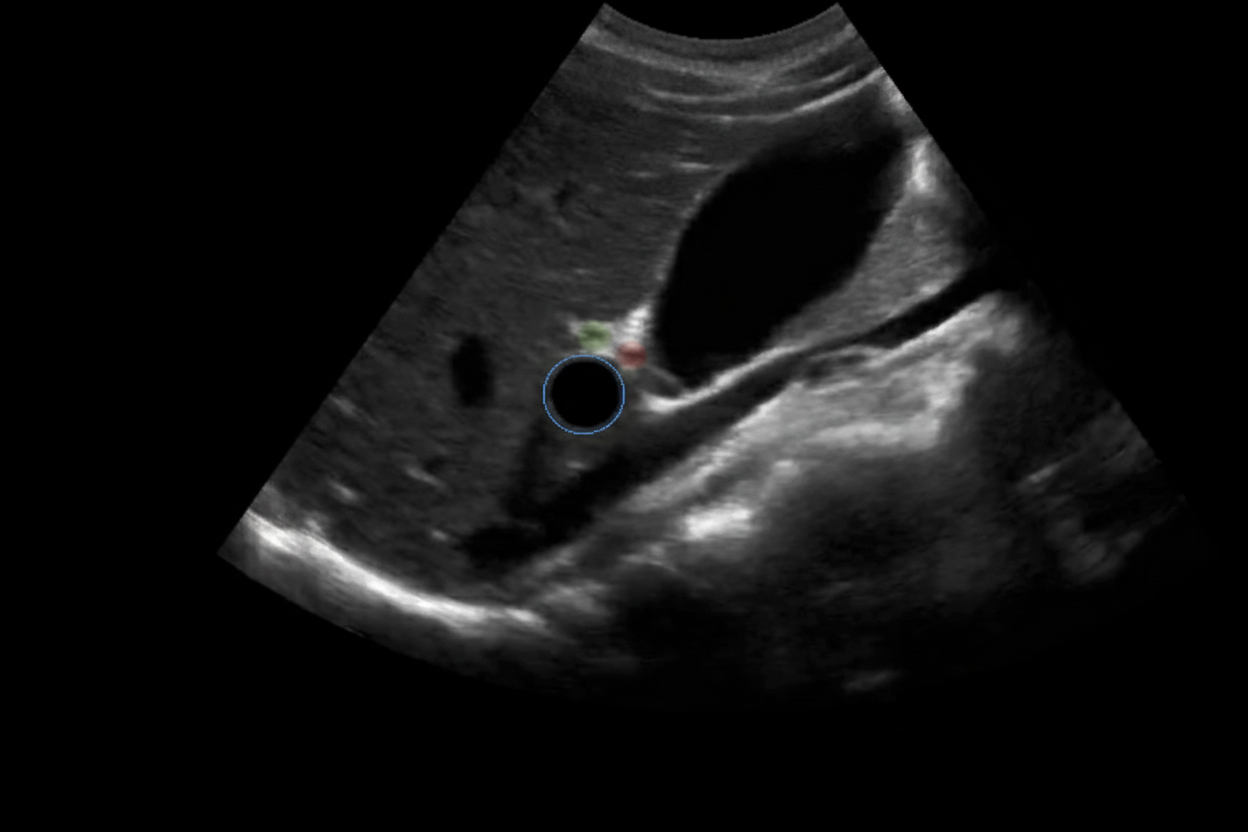
A 12-year-old patient with esophageal varices is managed by the procedure shown in the image. All of the following statements regarding this condition are true except:
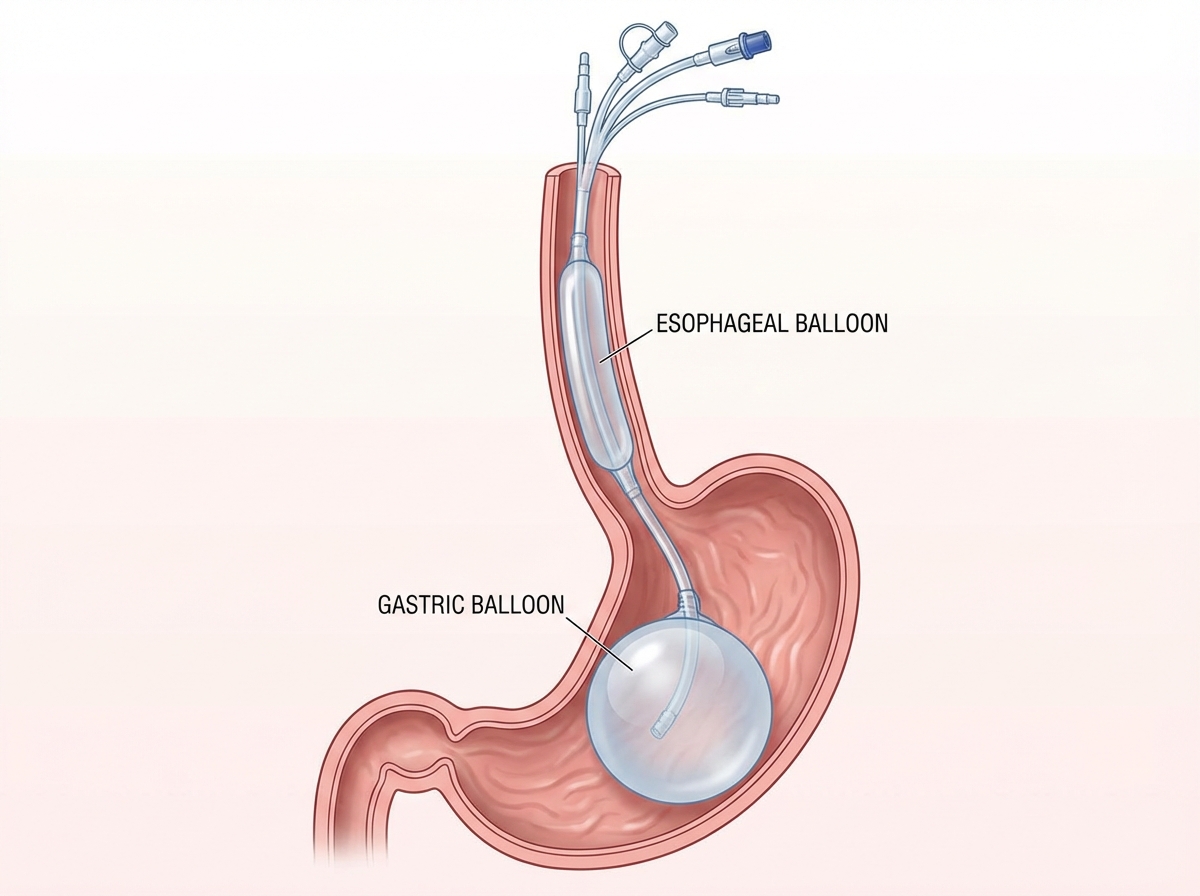
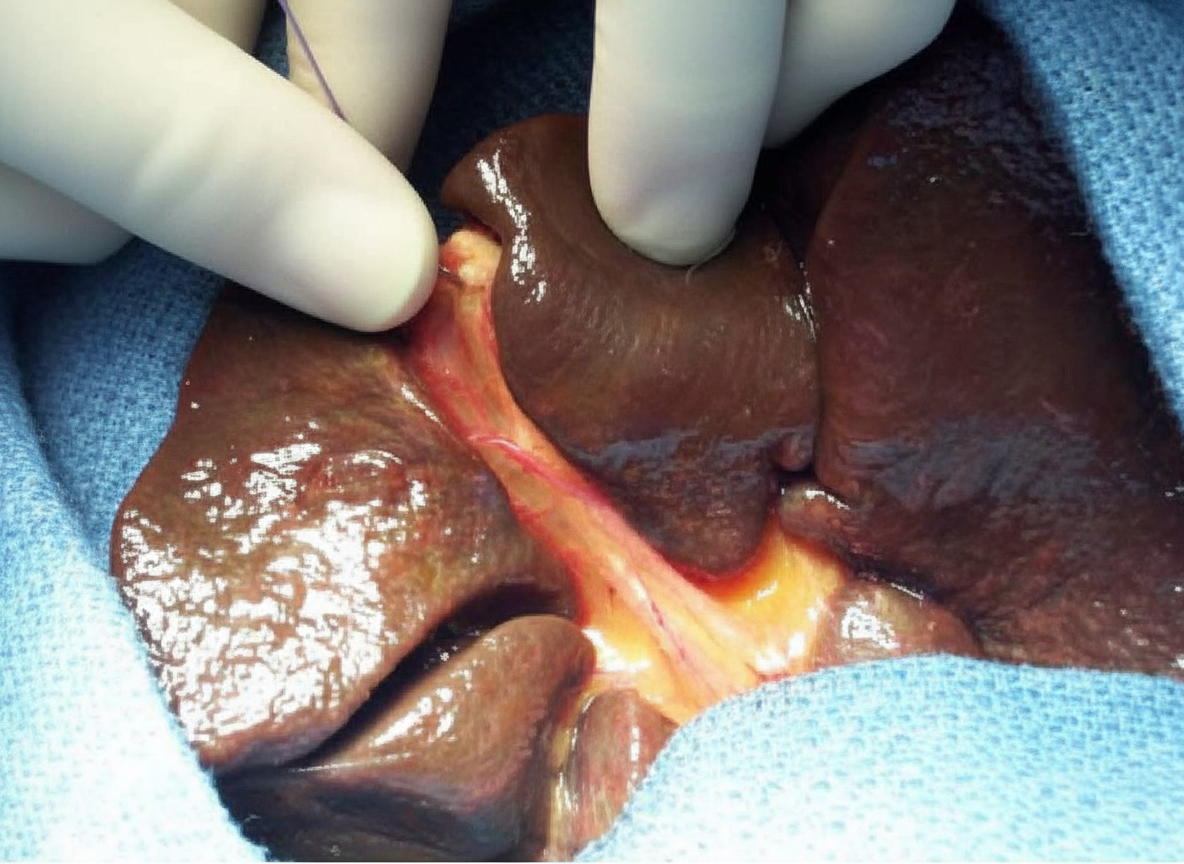
What does the intraoperative image shown below depict?
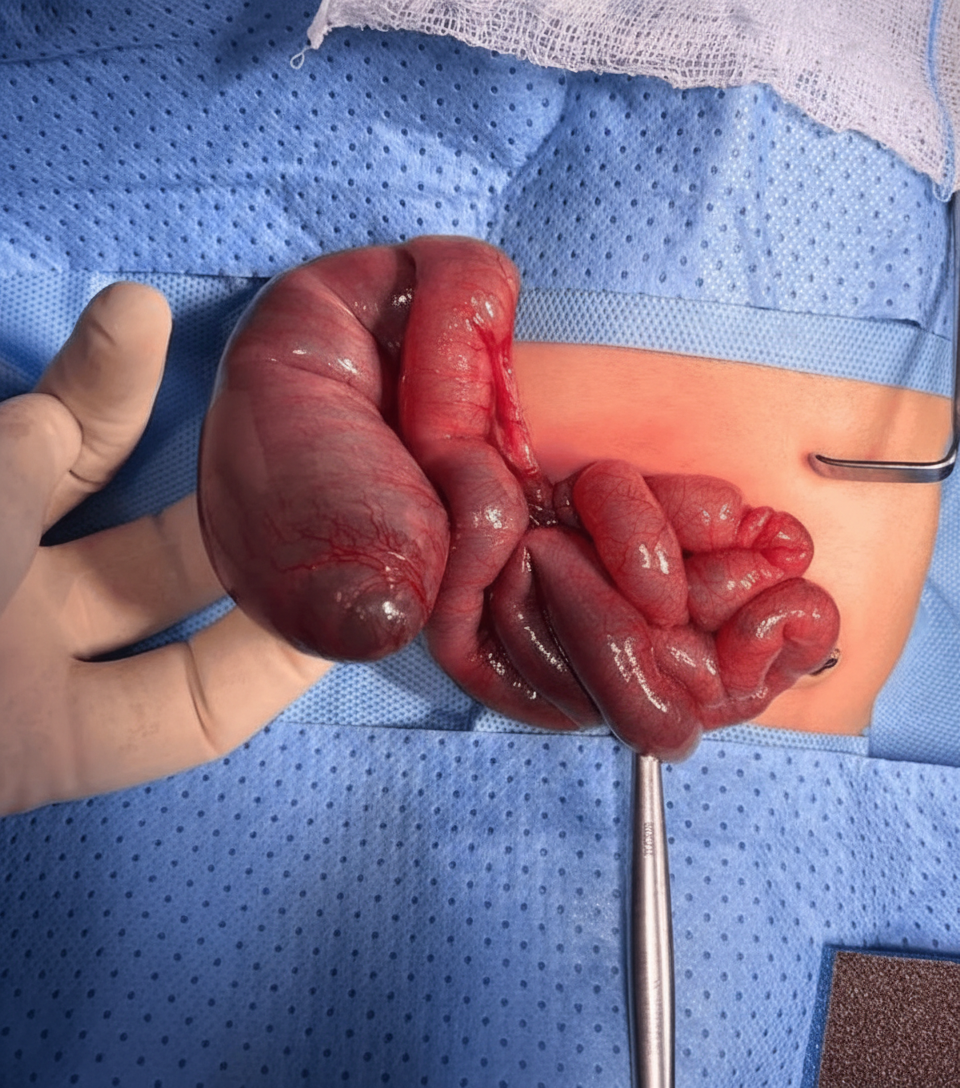
Which of the following is true regarding this condition?
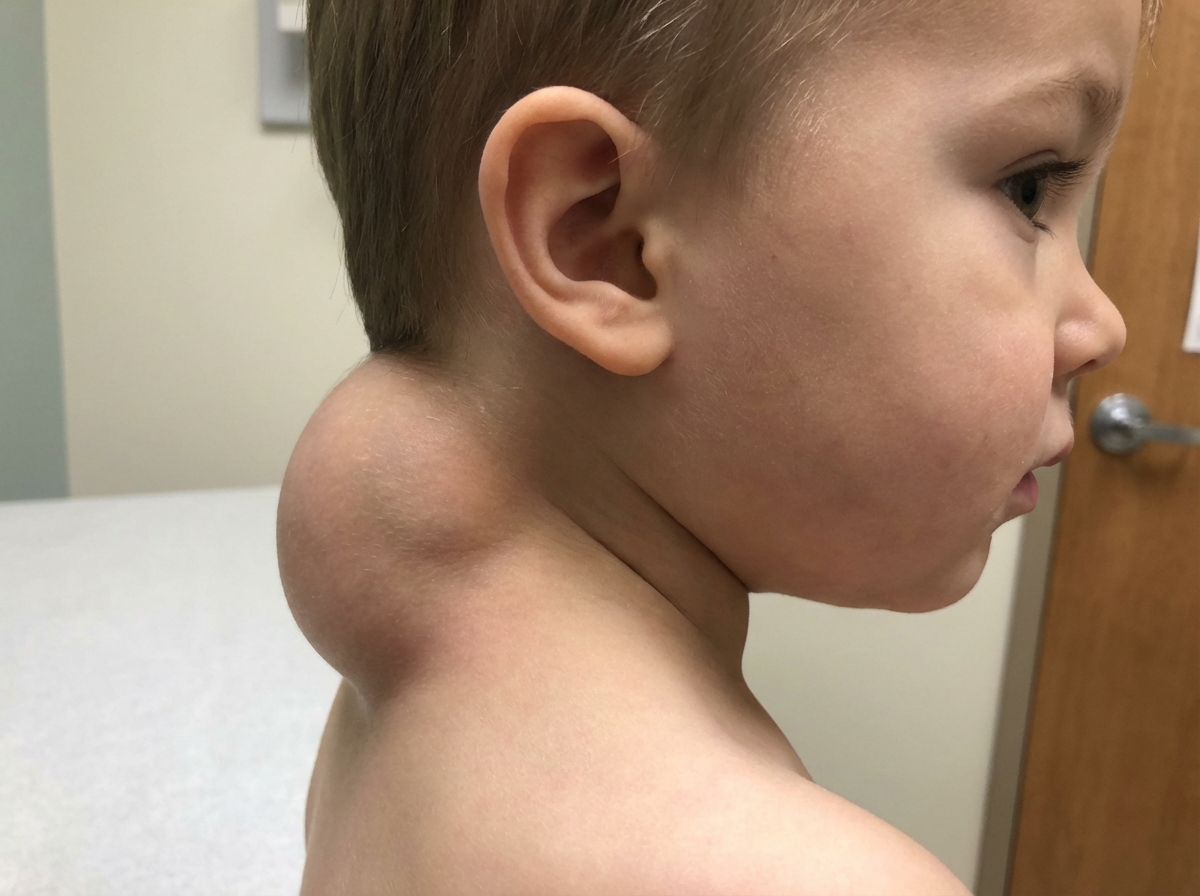
A 3-month-old child presents with umbilical discharge. The appearance is shown below. Which of the following is the next step in management of this patient? (AIIMS May 2018)
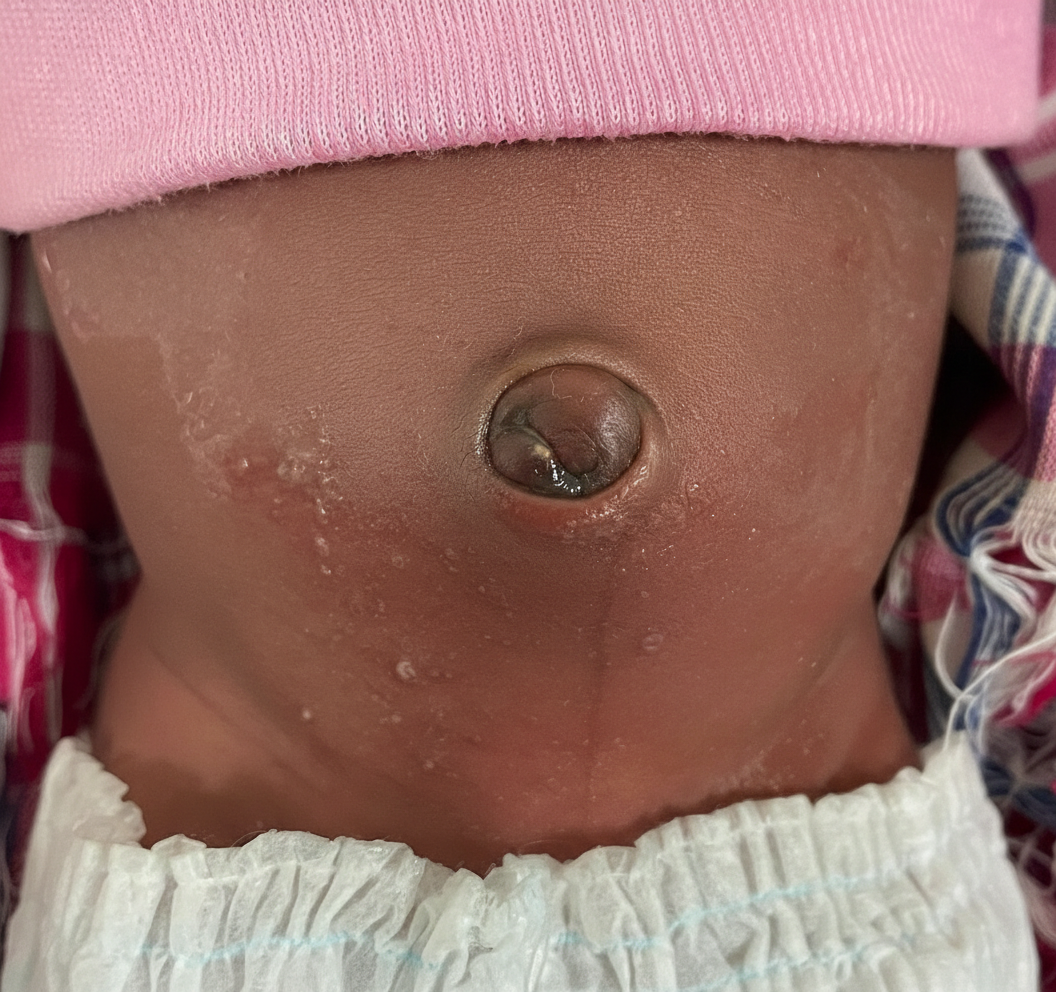
All of the following are usually associated findings in the given condition except? (AIIMS May 2018)
A 9-month-old child presents with excessive cry and presentation shown below. On examination right iliac fossa sausage shaped lump is felt. What is the best treatment?
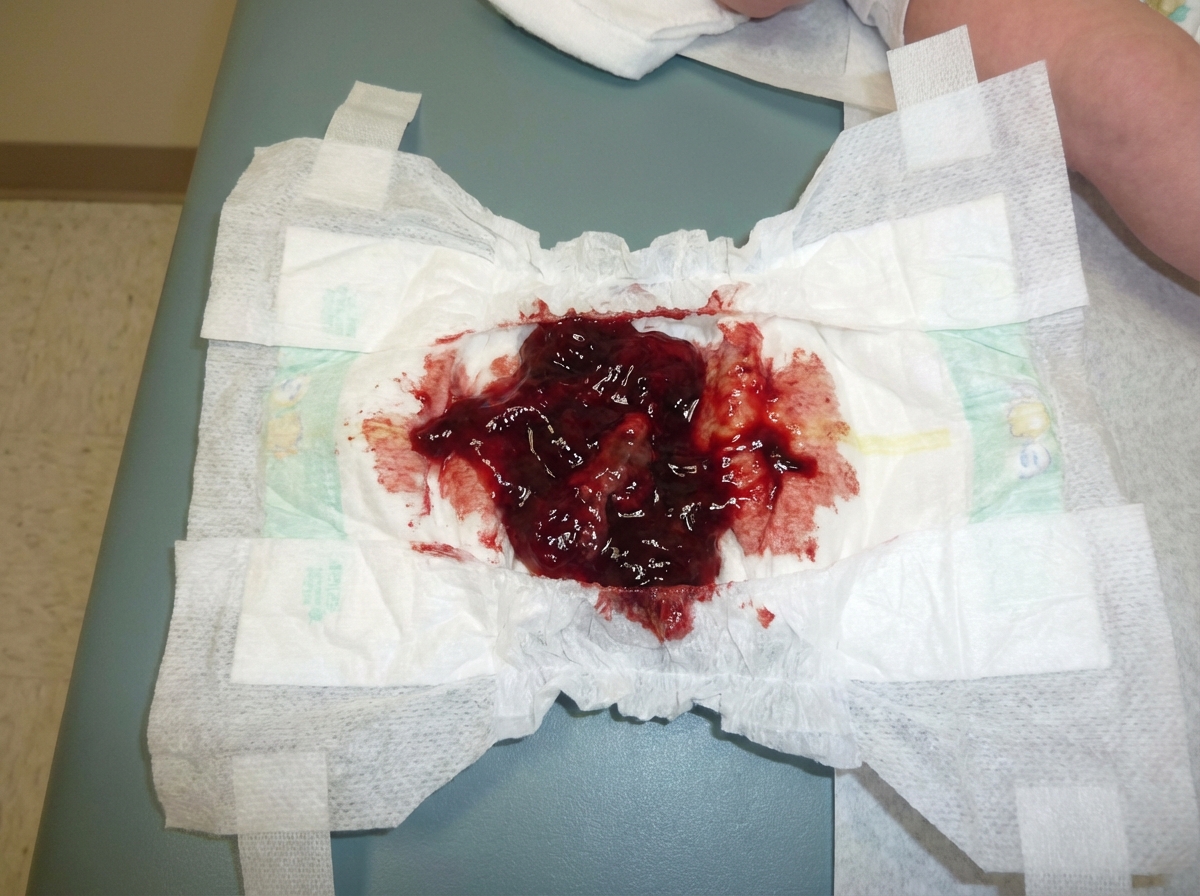
The structure shown in the image on the left represents which of the following?
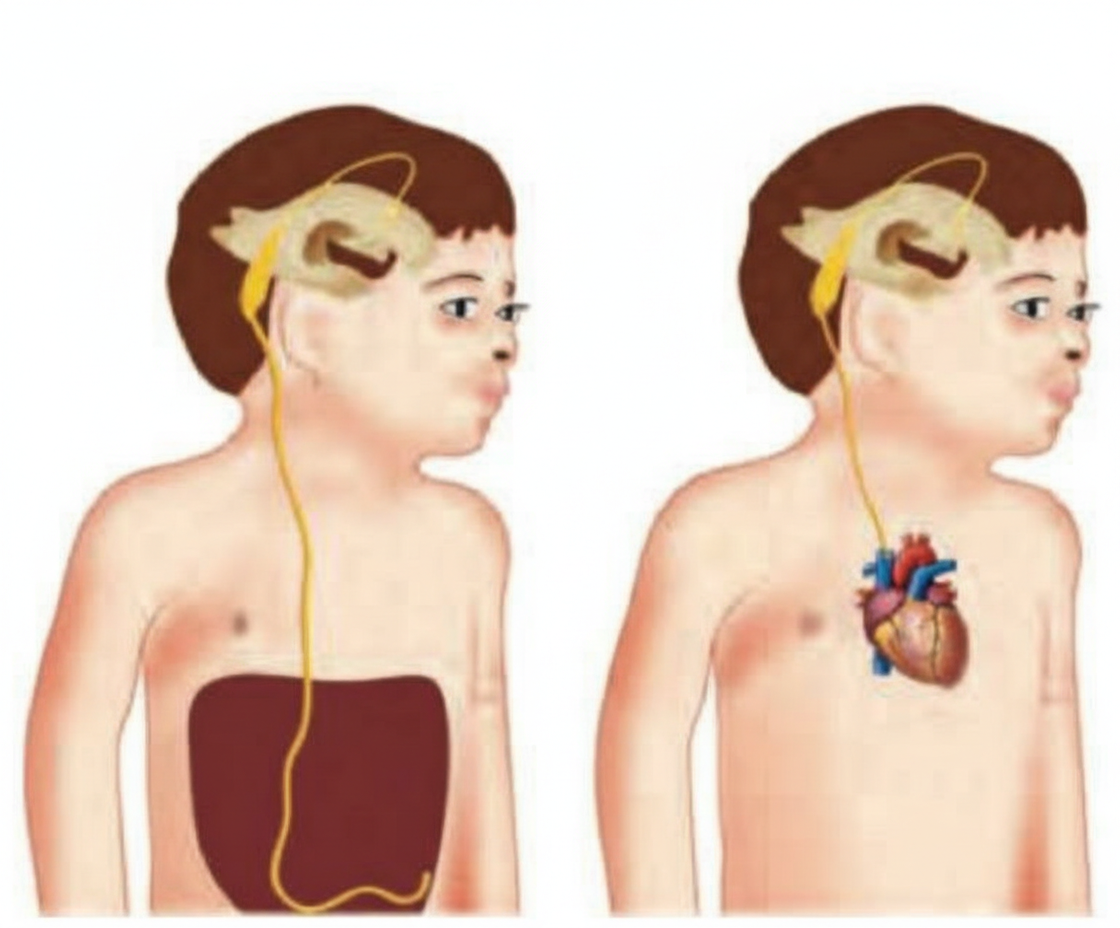
Practice by Chapter
Biliary atresia and Kasai procedure
Practice Questions
Congenital abdominal wall defects
Practice Questions
Congenital diaphragmatic hernia
Practice Questions
Congenital heart defects requiring surgery
Practice Questions
Hirschsprung disease management
Practice Questions
Intussusception reduction techniques
Practice Questions
Necrotizing enterocolitis surgical management
Practice Questions
Neonatal surgical emergencies
Practice Questions
Pediatric fluid and electrolyte management
Practice Questions
Pediatric trauma considerations
Practice Questions
Pyloric stenosis diagnosis and pyloromyotomy
Practice Questions
Tracheoesophageal fistula repair
Practice Questions
Undescended testis and orchiopexy
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
