Thoracotomy approaches and techniques — MCQs

A 79-year-old man is admitted to the intensive care unit for hospital acquired pneumonia, a COPD flare, and acute heart failure requiring intubation and mechanical ventilation. On his first night in the intensive care unit, his temperature is 99.7°F (37.6°C), blood pressure is 107/58 mm Hg, and pulse is 150/min which is a sudden change from his previous vitals. Physical exam is notable for jugular venous distension and a rapid heart rate. The ventilator is checked and is functioning normally. Which of the following is the best next step in management for the most likely diagnosis?
A 60-year-old man comes to the clinic complaining of a persistent cough for the last few months. His cough started gradually about a year ago, and it became more severe and persistent despite all his attempts to alleviate it. During the past year, he also noticed some weight loss and a decrease in his appetite. He also complains of progressive shortness of breath. He has a 40-pack-year smoking history but is a nonalcoholic. Physical examination findings are within normal limits. His chest X-ray shows a mass in the right lung. A chest CT shows a 5 cm mass with irregular borders near the lung hilum. A CT guided biopsy is planned. During the procedure, just after insertion of the needle, the patient starts to feel pain in his right shoulder. Which of the following nerves is responsible for his shoulder pain?
A 27-year-old man presents to the emergency department with severe dyspnea and sharp chest pain that suddenly started an hour ago after he finished exercising. He has a history of asthma as a child, and he achieves good control of his acute attacks with Ventolin. On examination, his right lung field is hyperresonant along with diminished lung sounds. Chest wall motion during respiration is asymmetrical. His blood pressure is 105/67 mm Hg, respirations are 22/min, pulse is 78/min, and temperature is 36.7°C (98.0°F). The patient is supported with oxygen, given corticosteroids, and has had analgesic medications via a nebulizer. Considering the likely condition affecting this patient, what is the best step in management?
A 24-year-old man is brought to the emergency department after being involved in a motor vehicle accident as an unrestrained driver. He was initially found unconscious at the scene but, after a few minutes, he regained consciousness. He says he is having difficulty breathing and has right-sided pleuritic chest pain. A primary trauma survey reveals multiple bruises and lacerations on the anterior chest wall. His temperature is 36.8°C (98.2°F), blood pressure is 100/60 mm Hg, pulse is 110/min, and respiratory rate is 28/min. Physical examination reveals a penetrating injury just below the right nipple. Cardiac examination is significant for jugular venous distention. There is also an absence of breath sounds on the right with hyperresonance to percussion. A bedside chest radiograph reveals evidence of a collapsed right lung with depression of the right hemidiaphragm and tracheal deviation to the left. Which of the following is the most appropriate next step in the management of this patient?
A 14-year-old boy is brought to the emergency department because of acute left-sided chest pain and dyspnea following a motor vehicle accident. His pulse is 122/min and blood pressure is 85/45 mm Hg. Physical examination shows distended neck veins and tracheal displacement to the right side. The left chest is hyperresonant to percussion and there are decreased breath sounds. This patient would most benefit from needle insertion at which of the following anatomical sites?
An 18-year-old man is brought to the emergency department 30 minutes after being stabbed in the chest during a fight. He has no other injuries. His pulse is 120/min, blood pressure is 90/60 mm Hg, and respirations are 22/min. Examination shows a 4-cm deep, straight stab wound in the 4th intercostal space 2 cm medial to the right midclavicular line. The knife most likely passed through which of the following structures?
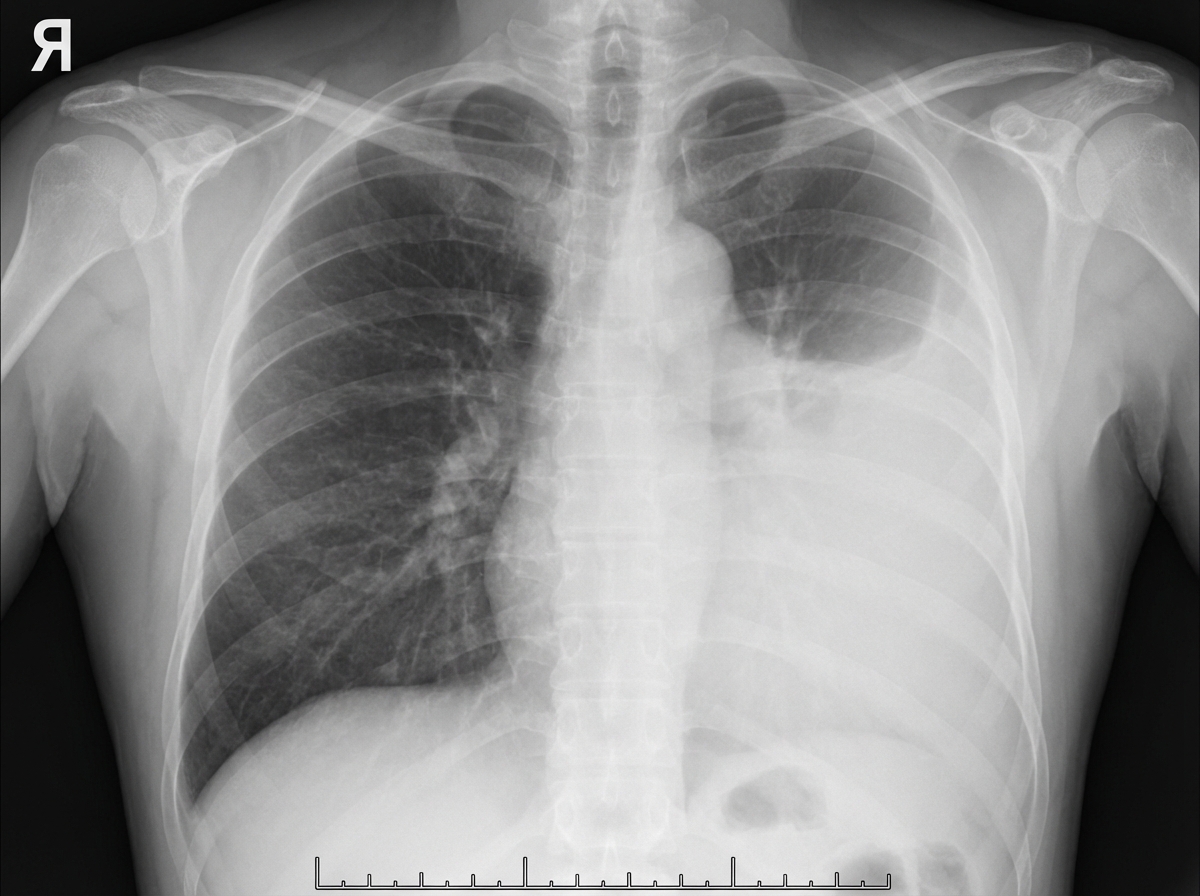
A 45-year-old man in respiratory distress presents to the emergency department. He sustained a stab to his left chest and was escorted to the nearest hospital. The patient appears pale and has moderate difficulty with breathing. His O2 saturation is 94%. The left lung is dull to percussion. CXRs are ordered and confirm the likely diagnosis. His blood pressure is 95/57 mm Hg, the respirations are 22/min, the pulse is 87/min, and the temperature is 36.7°C (98.0°F). His chest X-ray is shown. Which of the following is the next best step in management for this patient?
A 68-year-old man comes to the physician because of a 4-month history of difficulty swallowing. During this time, he has also had a 7-kg (15-lb) weight loss. Esophagogastroduodenoscopy shows an exophytic mass in the distal third of the esophagus. Histological examination of a biopsy specimen shows a well-differentiated adenocarcinoma. The patient is scheduled for surgical resection of the tumor. During the procedure, the surgeon damages a structure that passes through the diaphragm along with the esophagus at the level of the tenth thoracic vertebra (T10). Which of the following structures was most likely damaged?
A 45-year-old woman undergoes a modified radical mastectomy for breast cancer. Following the procedure, she experiences numbness in the medial aspect of her upper arm. Which of the following nerves was most likely injured during the surgery?
A 62-year-old man comes to the physician for a follow-up examination after having been diagnosed with stage II adenocarcinoma of the left lower lung lobe without evidence of distant metastases 1 week ago following an evaluation for a chronic cough. He has hypertension and type 2 diabetes mellitus. He has smoked one pack of cigarettes daily for the past 40 years. His current medications include metformin, sitagliptin, and enalapril. He is 177 cm (5 ft 10 in) tall and weighs 65 kg (143 lb); BMI is 20.7 kg/m2. He appears lethargic. Vital signs are within normal limits. Pulse oximetry shows an oxygen saturation of 98%. Examination shows inspiratory wheezing at the left lung base. The remainder of the examination shows no abnormalities. A complete blood count and serum concentrations of electrolytes, creatinine, glucose, and liver enzymes are within the reference range. Spirometry shows an FEV1 of 1.6 L. The diffusing lung capacity for carbon monoxide (DLCO) is 66% of predicted. Which of the following is the most appropriate next step in the management of this patient?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
