Breast Surgery — MCQs

On this page
A 24-year-old female patient presents with bilateral breast mass. On physical examination this breast mass is hyper mobile and soft. The mammogram is shown below. What is the most possible diagnosis?
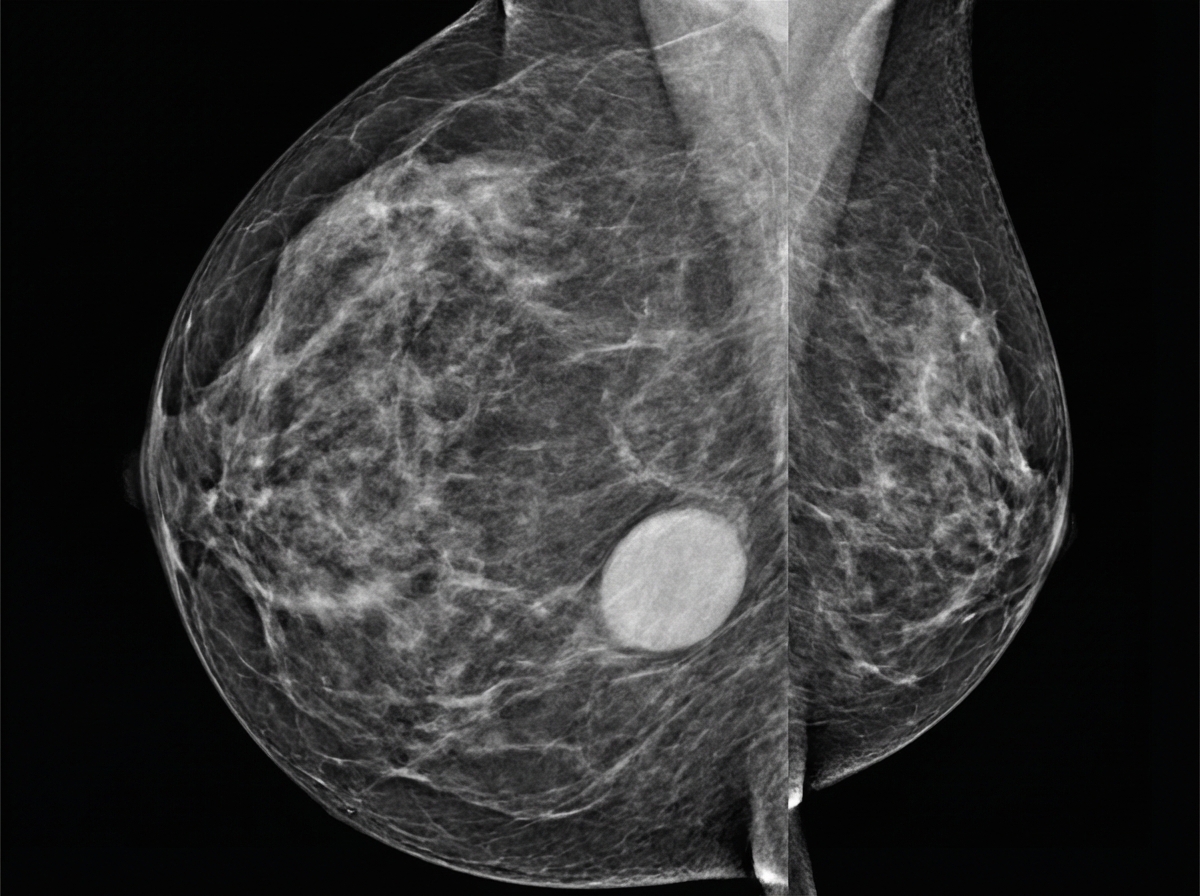
What is the diagnosis of the patient shown in the image? (Recent NEET Pattern 2016-17)
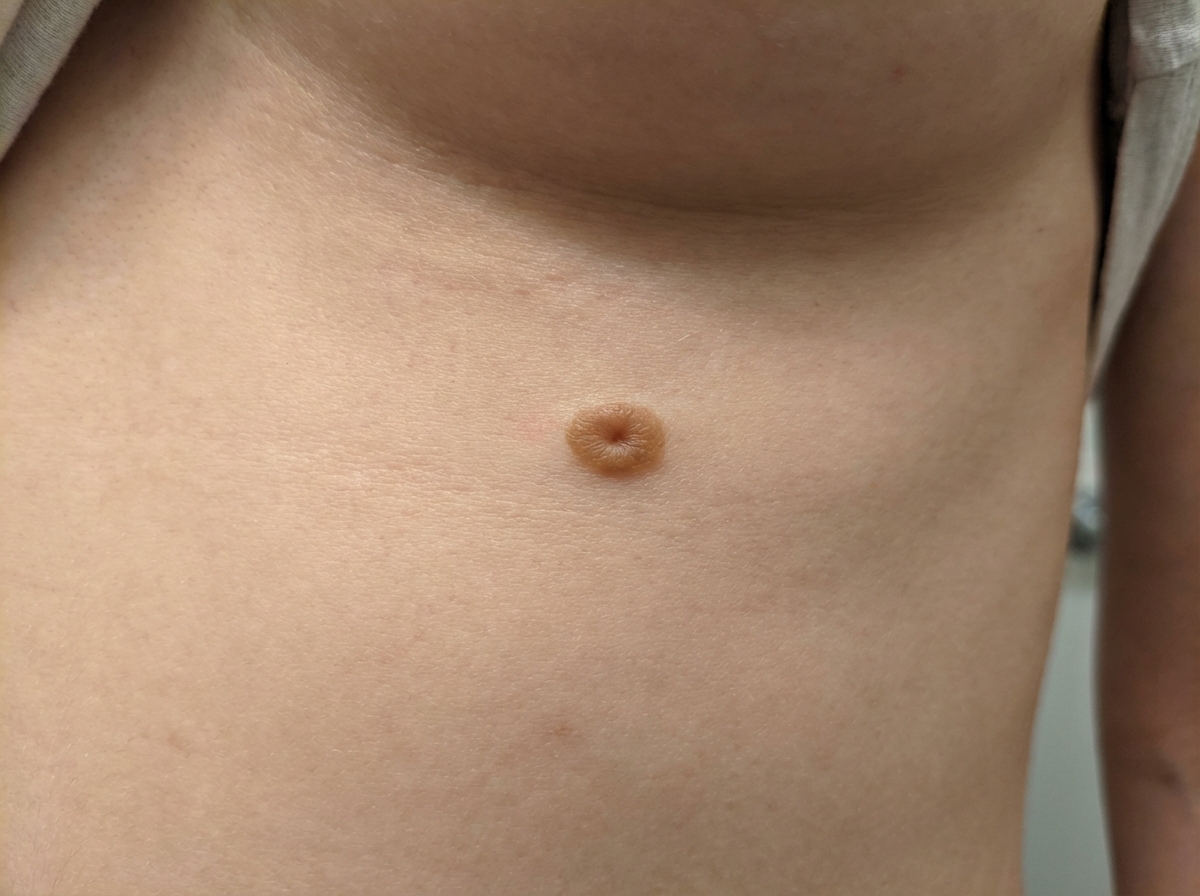
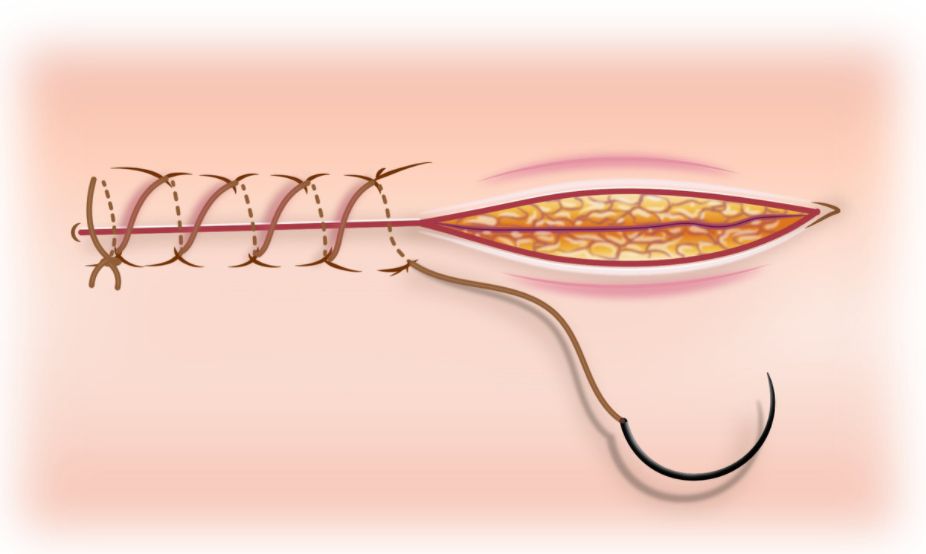
The surgeon attending has completed a modified radical mastectomy for a carcinoma breast patient. You have to suture the wound using subcuticular sutures. Which of the following sutures would you choose?
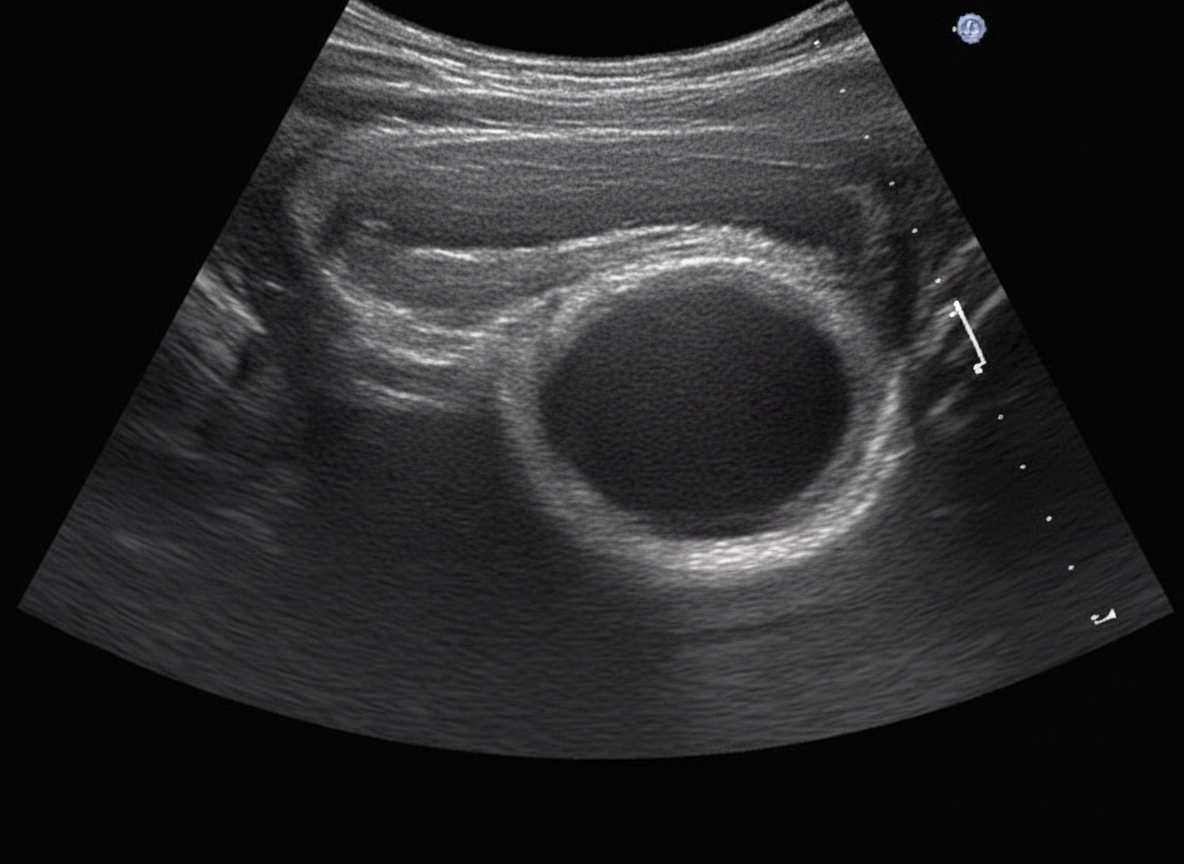
Which of the following is not an indication for surgery in the condition shown below?
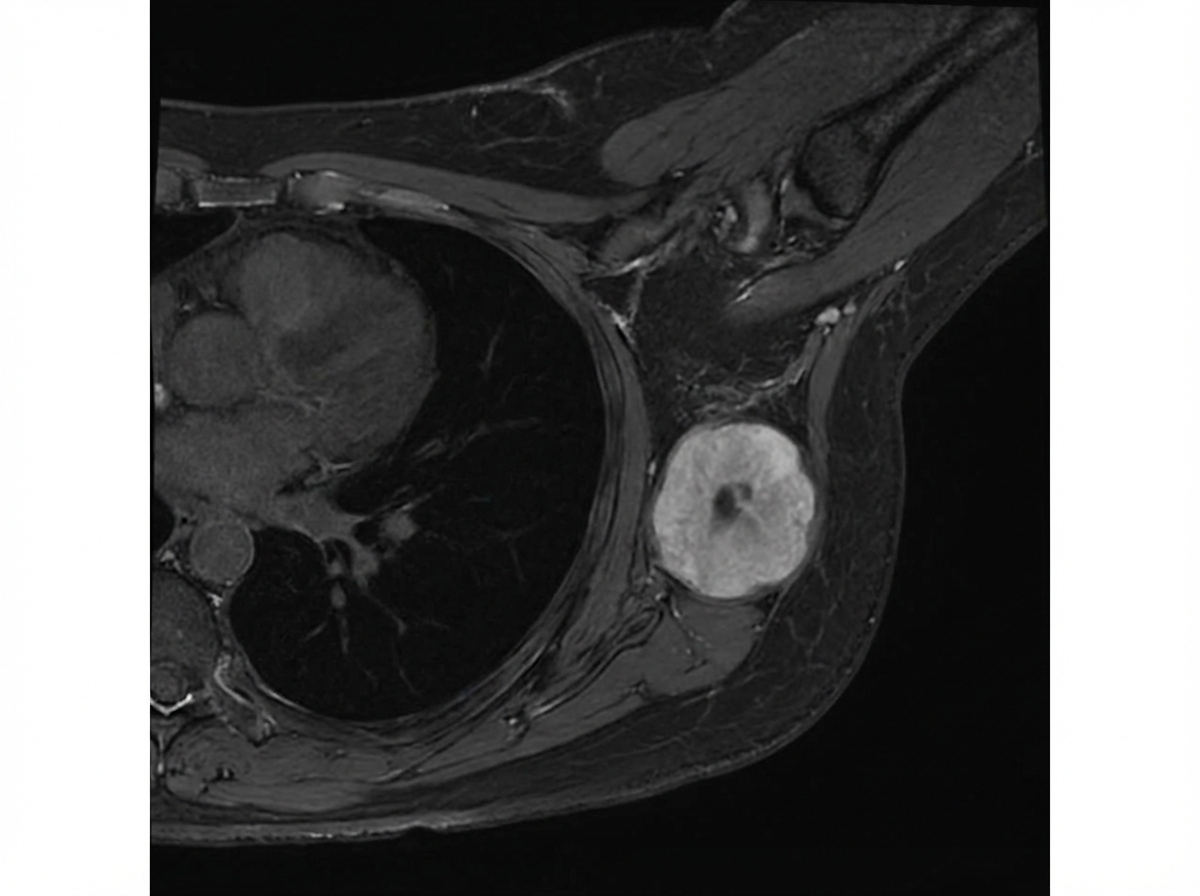
In the MRI breast shown below, 4 cm mass is present with no nodal metastasis. Which is the stage of breast cancer?
Practice by Chapter
Axillary lymph node dissection
Practice Questions
Benign breast disease management
Practice Questions
Breast biopsy techniques
Practice Questions
Breast cancer staging and surgical management
Practice Questions
Breast conservation therapy
Practice Questions
Breast reconstruction options
Practice Questions
Hereditary breast cancer syndromes
Practice Questions
Inflammatory breast cancer
Practice Questions
Male breast cancer
Practice Questions
Mastectomy techniques and indications
Practice Questions
Nipple discharge evaluation
Practice Questions
Post-mastectomy complications
Practice Questions
Sentinel lymph node biopsy
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
