Benign breast disease management — MCQs

A 36-year-old woman comes to the physician because of progressively worsening painful swelling of both breasts for the past 24 hours. Three days ago, she vaginally delivered a healthy 2690-g (5-lb 15-oz) girl. The patient says that breastfeeding her newborn daughter is very painful. She reports exhaustion and moodiness. She has no history of serious illness. Medications include folic acid and a multivitamin. Her temperature is 37.4°C (99.3°F). Examination shows tenderness, firmness, and fullness of both breasts. The nipples appear cracked and the areolas are swollen bilaterally. Which of the following is the most appropriate next step in management?
A 42-year-old woman presents to the physician because of an abnormal breast biopsy report following suspicious findings on breast imaging. Other than being concerned about her report, she feels well. She has no history of any serious illnesses and takes no medications. She does not smoke. She consumes wine 1–2 times per week with dinner. There is no significant family history of breast or ovarian cancer. Vital signs are within normal limits. Physical examination shows no abnormal findings. The biopsy shows lobular carcinoma in situ (LCIS) in the left breast. Which of the following is the most appropriate next step in management?
A 32-year-old woman presents to her physician concerned about wet spots on the inside part of her dress shirts, which she thinks may be coming from one of her breasts. She states that it is painless and that the discharge is usually blood-tinged. She denies any history of malignancy in her family and states that she has been having regular periods since they first started at age 13. She does not have any children. The patient has normal vitals and denies any cough, fever. On exam, there are no palpable masses, and the patient does not have any erythema or induration. What is the most likely diagnosis?
A 51-year-old woman presents for her annual wellness visit. She says she feels healthy and has no specific concerns. Past medical history is significant for bipolar disorder, hypertension, and diabetes mellitus type 2, managed with lithium, lisinopril, and metformin, respectively. Her family history is significant for hypertension and diabetes mellitus type 2 in her father, who died from lung cancer at age 67. Her vital signs include: temperature 36.8°C (98.2°F), pulse 97/min, respiratory rate 16/min, blood pressure 120/75 mm Hg. Physical examination is unremarkable. Mammogram findings are labeled breast imaging reporting and data system-3 (BIRADS-3) (probably benign). Which of the following is the next best step in management in this patient?
A 32-year-old woman presented for her annual physical examination. She mentioned that her family history had changed since her last visit: her mother was recently diagnosed with breast cancer and her sister tested positive for the BRCA2 mutation. The patient, therefore, requested testing as well. If the patient tests positive for the BRCA1 or BRCA2 mutation, which of the following is the best screening approach?
A 26-year-old woman presents to her physician at the 3rd week postpartum with a fever and a swollen breast with redness and tenderness. She has been breastfeeding her infant since birth. The symptoms of the patient started 4 days ago. She has not taken any antibiotics for the past 12 months. She does not have any concurrent diseases. The vital signs include: blood pressure 110/80 mm Hg, heart rate 91/min, respiratory rate 15/min, and temperature 38.8℃ (101.8℉). Physical examination reveals redness and enlargement of the right breast. The breast is warm and is painful at palpation. There is purulent discharge from the nipple. No fluctuation is noted. Which of the following is a correct management strategy for this patient?
A 34-year-old woman visits an outpatient clinic with a complaint of pain in her left breast for the last few months. The pain worsens during her menstrual cycle and relieves once the cycle is over. She denies any nipple discharge, skins changes, warmth, erythema, or a palpable mass in the breast. Her family history is negative for breast, endometrial, and ovarian cancer. There is no palpable mass or any abnormality in the physical examination of her breast. A mammogram is ordered which shows a cluster of microcalcifications with a radiolucent center. A breast biopsy is also performed which reveals a lobulocentric proliferation of epithelium and myoepithelium. Which of the following is the most likely diagnosis?
A 32-year-old woman presents to her primary care physician for an annual checkup. She reports that she has been feeling well and has no medical concerns. Her past medical history is significant for childhood asthma but she has not experienced any symptoms since she was a teenager. Physical exam reveals a 1-centimeter hard mobile mass in the left upper outer quadrant of her breast. A mammogram was performed and demonstrated calcifications within the mass so a biopsy was obtained. The biopsy shows acinar proliferation with intralobular fibrosis. Which of the following conditions is most likely affecting this patient?
A 27-year-old woman presents for her routine annual examination. She has no complaints. She has a 3-year-old child who was born via normal vaginal delivery with no complications. She had a Pap smear during her last pregnancy and the findings were normal. Her remaining past medical history is not significant, and her family history is also not significant. Recently, one of her close friends was diagnosed with breast cancer at the age of 36, and, after reading some online research, she wants to be checked for all types of cancer. Which of the following statements would be the best advice regarding the most appropriate screening tests for this patient?
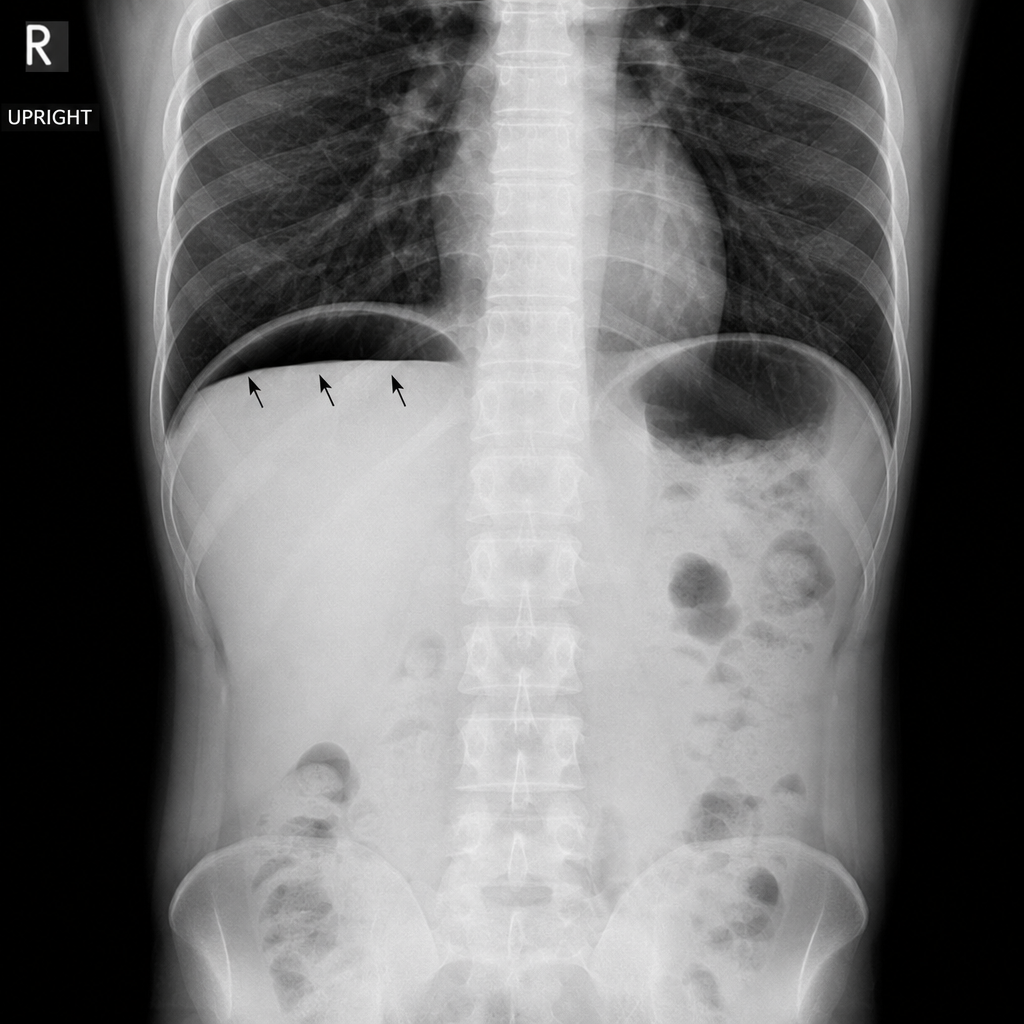
A 45-year-old man presents to the emergency department with a 12-hour history of severe periumbilical pain that has migrated to the right lower quadrant, fever of 38.4°C, and anorexia. On examination, there is point tenderness 2/3 of the way along a line from the umbilicus to the right anterior superior iliac spine. His WBC is 14,200/mm³ with a left shift. A plain abdominal radiograph is obtained. Which of the following findings on this image would most directly indicate perforation requiring urgent surgical intervention?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
