General anesthesia principles — MCQs

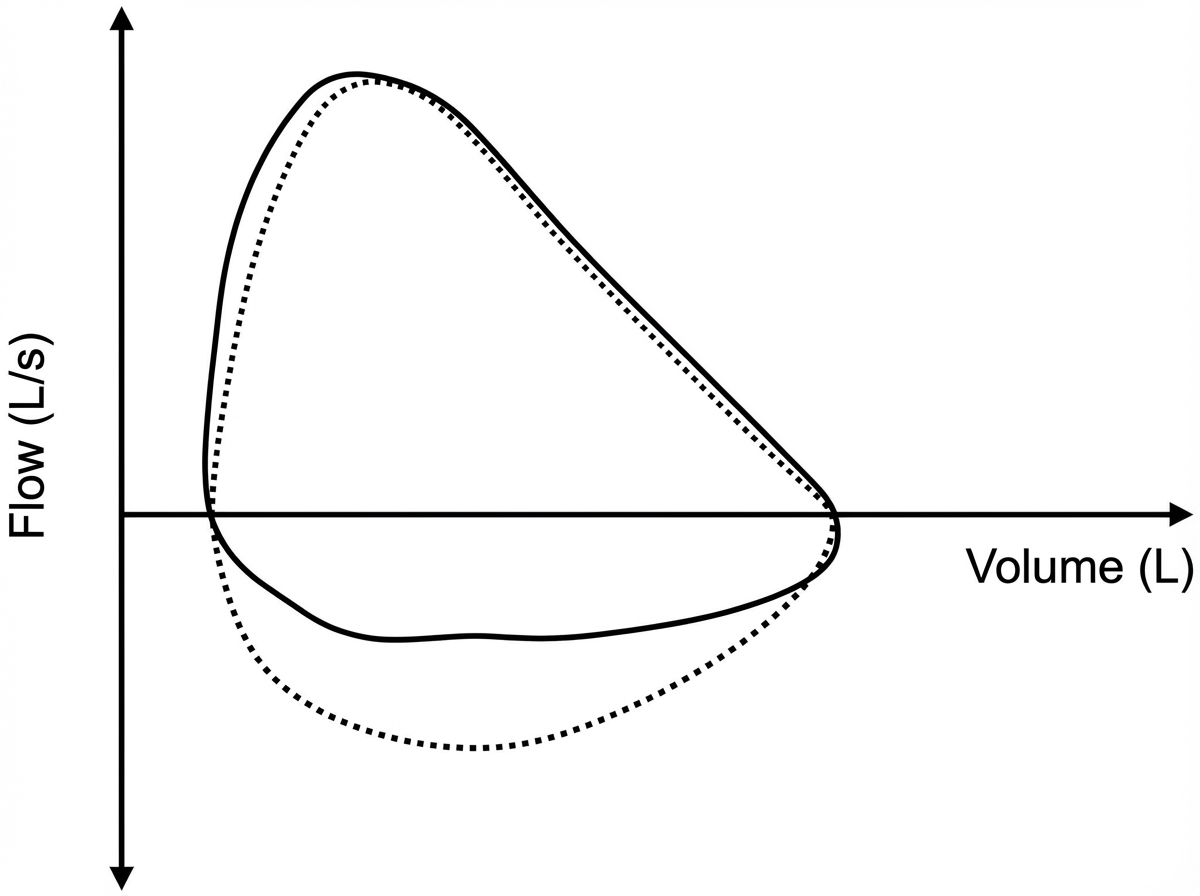
Five minutes after arriving in the postoperative care unit following total knee replacement under general anesthesia, a 55-year-old woman is acutely short of breath. The procedure was uncomplicated. Postoperatively, prophylactic treatment with cefazolin was begun and the patient received morphine and ketorolac for pain management. She has generalized anxiety disorder. Her only other medication is escitalopram. She has smoked one pack of cigarettes daily for 25 years. Her temperature is 37°C (98.6°F), pulse is 108/min, respirations are 26/min, and blood pressure is 95/52 mm Hg. A flow-volume loop obtained via pulmonary function testing is shown. Which of the following is the most likely underlying cause of this patient's symptoms?
A 59-year-old woman is scheduled to undergo a right hip total arthroplasty for severe hip osteoarthritis that has failed conservative management. She has never had surgery before. She has a history of major depressive disorder and takes sertraline daily and ibuprofen occasionally for pain. Her mother died of breast cancer and her father died from a myocardial infarction. She has a brother who had an adverse reaction following anesthesia, but she does not know details of the event. In the operating room, the anesthesiologist administers isoflurane and succinylcholine. Two minutes later, the patient develops hypercarbia and hypertonicity of her bilateral upper and lower extremities. Her temperature is 103.7°F (39.8°C), blood pressure is 155/95 mmHg, pulse is 115/min, and respirations are 20/min. A medication with which of the following mechanisms of action is most strongly indicated for this patient?
Two hours after undergoing elective cholecystectomy with general anesthesia, a 41-year-old woman is evaluated for decreased mental status. BMI is 36.6 kg/m2. Respirations are 18/min and blood pressure is 126/73 mm Hg. Physical examination shows the endotracheal tube in normal position. She does not respond to sternal rub and gag reflex is absent. Arterial blood gas analysis on room air shows normal PO2 and PCO2 levels. Which of the following anesthetic properties is the most likely cause of these findings?
A 29-year-old man is being monitored at the hospital after cutting open his left wrist. He has a long-standing history of unipolar depressive disorder and multiple trials of antidepressants. The patient expresses thoughts of self-harm and does not deny suicidal intent. A course of electroconvulsive therapy is suggested. His medical history is not significant for other organic illness. Which of the following complications of this therapy is this patient at greatest risk for?
A 28-year-old man comes to the emergency department for an injury sustained while doing construction. Physical examination shows a long, deep, irregular laceration on the lateral aspect of the left forearm with exposed fascia. Prior to surgical repair of the injury, a brachial plexus block is performed using a local anesthetic. Shortly after the nerve block is performed, he complains of dizziness and then loses consciousness. His radial pulse is faint and a continuous cardiac monitor shows a heart rate of 24/min. Which of the following is the most likely mechanism of action of the anesthetic that was administered?
A 23-year-old man is brought to the emergency department by ambulance following a motor vehicle accident. He was pinned between 2 cars for several hours. The patient has a history of asthma. He uses an albuterol inhaler intermittently. The patient was not the driver, and admits to having a few beers at a party prior to the accident. His vitals in the ambulance are stable. Upon presentation to the emergency department, the patient is immediately brought to the operating room for evaluation and surgical intervention. It is determined that the patient’s right leg has a Gustilo IIIC injury in the mid-shaft of the tibia with a severely comminuted fracture. The patient’s left leg suffered a similar injury but with damage to the peroneal nerve. The anesthesiologist begins to induce anesthesia. Which of the following agents would be contraindicated in this patient?
A 17-year-old boy is brought to the emergency department by his brother after losing consciousness 1 hour ago. The brother reports that the patient was skateboarding outside when he fell on the ground and started to have generalized contractions. There was also some blood coming from his mouth. The contractions stopped after about 1 minute, but he remained unconscious for a few minutes afterward. He has never had a similar episode before. There is no personal or family history of serious illness. He does not smoke or drink alcohol. He does not use illicit drugs. He takes no medications. On arrival, he is confused and oriented only to person and place. He cannot recall what happened and reports diffuse muscle ache, headache, and fatigue. He appears pale. His temperature is 37°C (98.6°F), pulse is 80/min, and blood pressure is 130/80 mm Hg. There is a small wound on the left side of the tongue. A complete blood count and serum concentrations of electrolytes, urea nitrogen, and creatinine are within the reference ranges. Toxicology screening is negative. An ECG shows no abnormalities. Which of the following is the most appropriate next step in management?
A 55-year-old man with chronic pain on high-dose opioids (120 mg oral morphine equivalents daily) requires major spine surgery. Intraoperatively, he requires escalating doses of fentanyl with poor pain control. Postoperatively, his pain remains severe (10/10) despite maximum conventional multimodal analgesia including IV hydromorphone PCA, acetaminophen, and ketorolac. He becomes increasingly agitated and tachycardic. Evaluate the most comprehensive pain management strategy addressing the underlying pathophysiology.
A 70-year-old man with severe aortic stenosis (valve area 0.6 cm², mean gradient 55 mmHg) develops acute cholecystitis requiring surgery. He is symptomatic with exertional angina and dyspnea. Cardiology recommends TAVR before surgery, but the patient has signs of gallbladder perforation. The surgical team debates timing of interventions. Evaluate the optimal management strategy weighing cardiac and surgical risks.
A 42-year-old woman with a history of multiple anesthetic complications presents for elective surgery. Previous records indicate awareness during general anesthesia twice, prolonged paralysis after succinylcholine requiring 6 hours of ventilation, and a sibling with fatal anesthetic complication involving hyperthermia and rhabdomyolysis. Evaluate the comprehensive anesthetic plan that addresses all potential complications.
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
