Abdominal emergencies — MCQs

On this page
An 82-year-old woman visits her primary care provider complaining of a vague cramping pain on the right side of her abdomen for the past 6 hours. She is also nauseated and had an episode of vomiting earlier today and two episodes yesterday. Past medical history includes third-degree heart block, gastroesophageal reflux disease, hypertension, hypothyroidism and chronic cholecystitis with cholelithiasis. She is not a good candidate for cholecystectomy due to cardiac disease and is treated with analgesics and ursodeoxycholic acid. Her medications include chlorthalidone, omeprazole, levothyroxine, and occasional naproxen for pain. Vitals are normal. A supine abdominal X-ray reveals air in the gallbladder and biliary tree, small bowel obstruction, and a large radiolucent gallstone impacted in the small bowel. What is the most likely diagnosis?
A 29-year-old man presents to the emergency room with severe abdominal pain. He states that for the entire day, he has had pain in his lower right abdomen in addition to a loss of appetite accompanied by nausea and vomiting. His temperature is 101.3°F (38.5°C), blood pressure is 125/98 mmHg, pulse is 78/min, and respirations are 15/min. On physical examination, he exhibits increased abdominal pain in his right lower quadrant upon deep palpation of the left lower quadrant. What is the next step in the management of this patient?
A 72-year-old man is brought to the emergency department with increasing fever and abdominal pain over the past week. The pain is constant and limited to the lower right part of his abdomen. He has nausea but no vomiting or diarrhea. His past medical history is unremarkable for any serious illnesses. He takes acetaminophen for knee arthritis. He is fully alert and oriented. His temperature is 39.5°C (103.1°F), pulse is 89/min, respirations are 15/min, and blood pressure is 135/70 mm Hg. Abdominal examination shows a tender mass in the right lower quadrant. CT shows obstruction of the appendiceal neck with a fecalith and the appendiceal tip leading to an irregular walled-off fluid collection. Stranding of the surrounding fat planes is also noted. Intravenous hydration is initiated. Which of the following is the most appropriate next step in management?
A 66-year-old man comes to the physician because of yellowish discoloration of his eyes and skin, abdominal discomfort, and generalized fatigue for the past 2 weeks. He has had dark urine and pale stools during this period. He has had a 10-kg (22-lb) weight loss since his last visit 6 months ago. He has hypertension. He has smoked one pack of cigarettes daily for 34 years. He drinks three to four beers over the weekends. His only medication is amlodipine. His temperature is 37.3°C (99.1°F), pulse is 89/min, respirations are 14/min, and blood pressure is 114/74 mm Hg. Examination shows jaundice of the sclera and skin and excoriation marks on his trunk and extremities. The lungs are clear to auscultation. The abdomen is soft and nontender. The remainder of the examination shows no abnormalities. Laboratory studies show: Hemoglobin 12 g/dL Leukocyte count 5,000/mm3 Platelet count 400,000/mm3 Serum Urea nitrogen 28 mg/dL Creatinine 1.2 mg/dL Bilirubin Total 7.0 mg/dL Direct 5.5 mg/dL Alkaline phosphatase 615 U/L Aspartate aminotransferase (AST, GOT) 170 U/L Alanine aminotransferase (ALT, GPT) 310 U/L γ-Glutamyltransferase (GGT) 592 U/L (N = 5–50 U/L) An ultrasound shows extrahepatic biliary dilation. A CT scan of the abdomen shows a 2.5-cm (1-in) mass in the head of the pancreas with no abdominal lymphadenopathy. The patient undergoes biliary stenting. Which of the following is the most appropriate next step in the management of this patient?
A 59-year-old woman presents to the family medicine clinic with a lump in her breast for the past 6 months. She states that she has been doing breast self-examinations once a month. She has a medical history significant for generalized anxiety disorder and systemic lupus erythematosus. She takes sertraline and hydroxychloroquine for her medical conditions. The heart rate is 102/min, and the rest of the vital signs are stable. On physical examination, the patient appears anxious and tired. Her lungs are clear to auscultation bilaterally. Capillary refill is 2 seconds. There is no axillary lymphadenopathy present. Palpation of the left breast reveals a 2 x 2 cm mass. What is the most appropriate next step given the history of the patient?
A 68-year-old man presents for a screening ultrasound scan. He has been feeling well and is in his usual state of good health. His medical history is notable for mild hypertension and a 100-pack-year tobacco history. He has a blood pressure of 128/86 and heart rate of 62/min. Physical examination is clear lung sounds and regular heart sounds. On ultrasound, an infrarenal aortic aneurysm of 4 cm in diameter is identified. Which of the following is the best initial step for this patient?
A 40-year-old woman comes to the physician because of a 2-week history of anal pain that occurs during defecation and lasts for several hours. She reports that she often strains during defecation and sees bright red blood on toilet paper after wiping. She typically has 3 bowel movements per week. Physical examination shows a longitudinal, perianal tear. This patient's symptoms are most likely caused by tissue injury in which of the following locations?
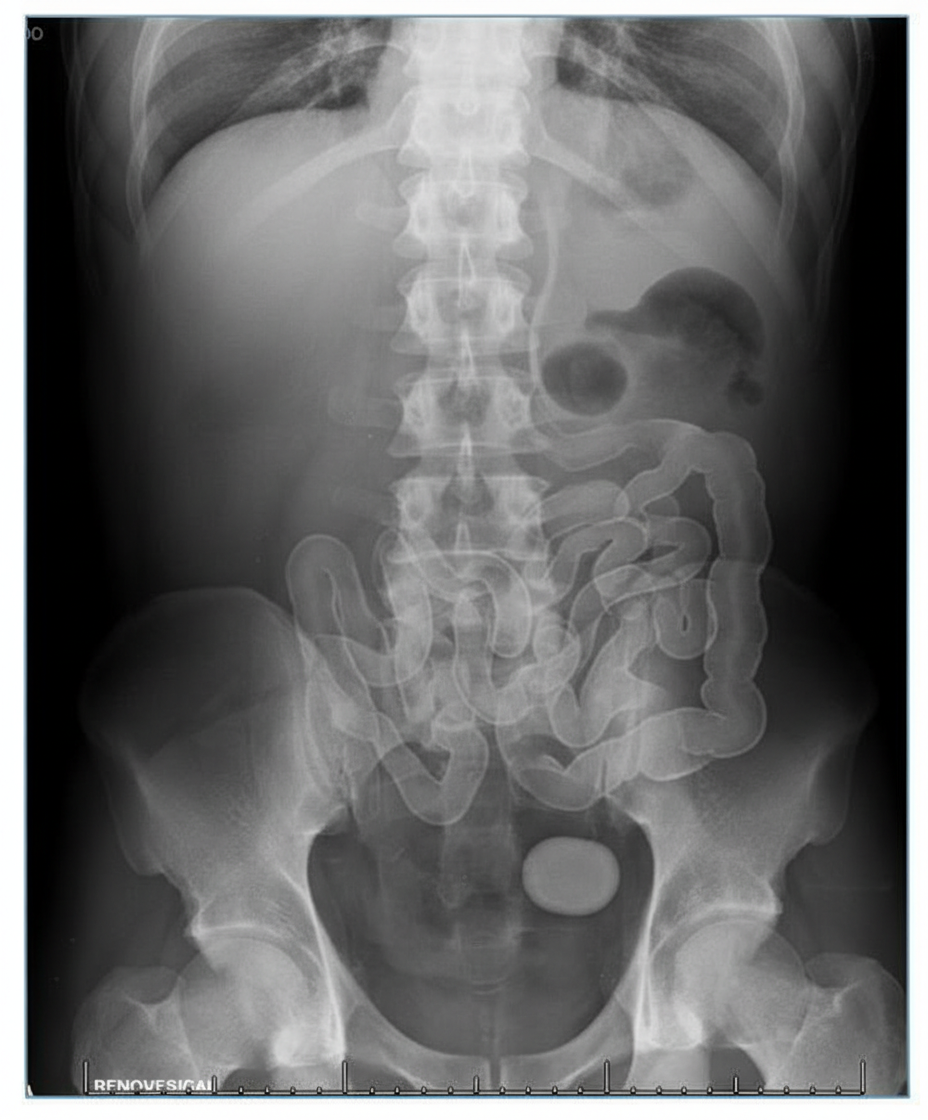
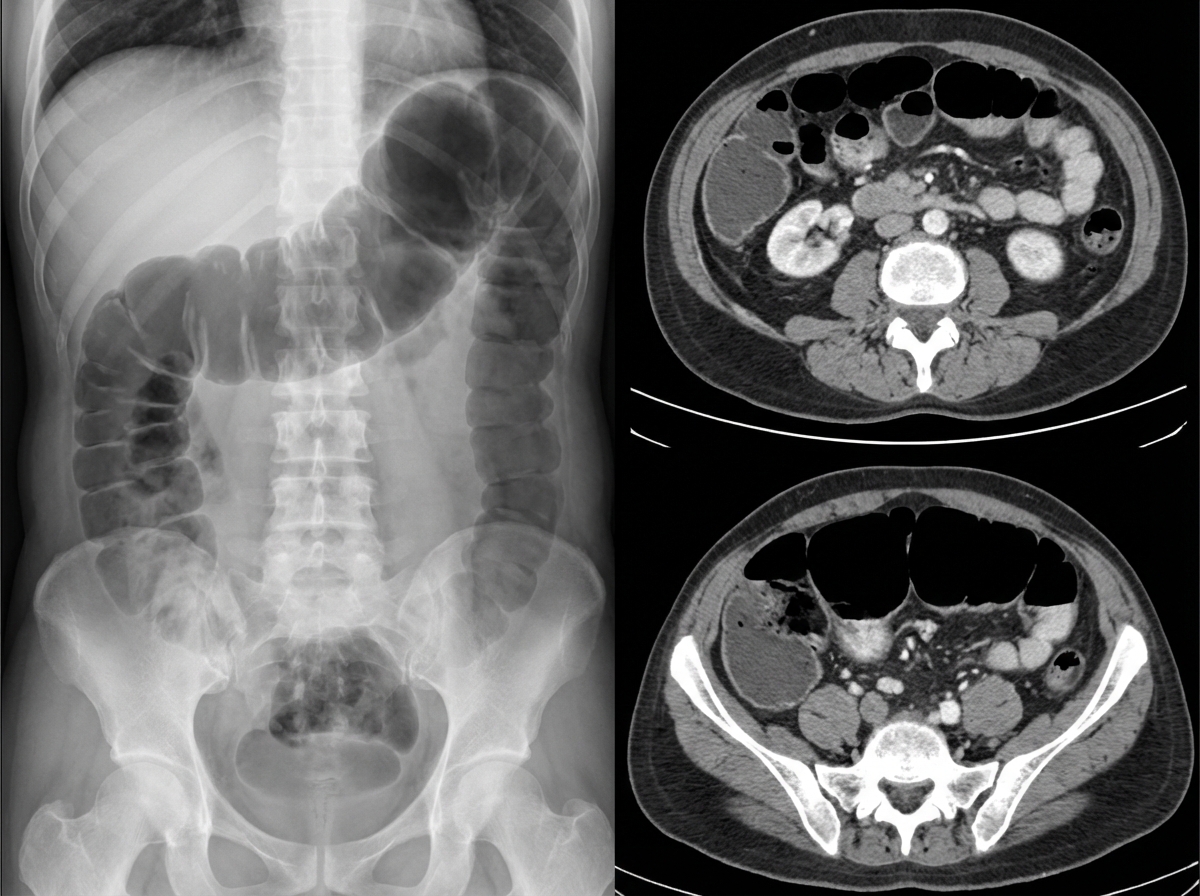
A 76-year-old female is brought to the emergency department after being found unresponsive in her room at her nursing facility. Past medical history is significant for Alzheimer's disease, hypertension, and diabetes. Surgical history is notable for an open cholecystectomy at age 38 and multiple cesarean sections. On arrival, she is non-responsive but breathing by herself, and her vital signs are T 102.9 F, HR 123 bpm, BP 95/64, RR 26/min, and SaO2 97% on 6L nasal cannula. On physical exam the patient has marked abdominal distension and is tympanic to percussion. Laboratory studies are notable for a lactic acidosis. An upright abdominal radiograph and CT abdomen/pelvis with contrast are shown in Figures A and B respectively. She is started on IV fluids and a nasogastric tube is placed to suction which returns green bilious fluid. Repeat vitals 1 hour later are T 101F, HR 140 bpm, BP 75/44, RR 30/min, and SaO2 is 100% on the ventilator after she is intubated for airway concerns. What is the next best step in management?
A 69-year-old man is brought to the emergency department because of severe abdominal pain radiating to his left flank for 30 minutes. He is weak and has been unable to stand since the onset of the pain. He vomited twice on the way to the hospital. He has not passed stools for 3 days. He has hypertension, coronary heart disease, and peptic ulcer disease. He has smoked half a pack of cigarettes daily for 46 years. Current medications include enalapril, metoprolol, aspirin, simvastatin, and pantoprazole. He appears ill. His temperature is 37°C (98.6°F), pulse is 131/min, respirations are 31/min, and blood pressure is 82/56 mm Hg. Pulse oximetry on room air shows an oxygen saturation of 92%. The lungs are clear to auscultation. Cardiac examination shows no abnormalities. Examination shows a painful pulsatile abdominal mass. Intravenous fluid resuscitation is begun. Which of the following is the most appropriate next step in management?
A 31-year-old man presents to an urgent care clinic with symptoms of lower abdominal pain, bloating, bloody diarrhea, and fullness, all of which have become more frequent over the last 3 months. His vital signs are as follows: blood pressure is 121/81 mm Hg, heart rate is 87/min, and respiratory rate is 15/min. Rectal examination reveals a small amount of bright red blood. Lower endoscopy is performed, showing extensive mucosal erythema, induration, and pseudopolyps extending from the rectum to the splenic flexure. Given the following options, what is the most appropriate initial treatment for this patient's underlying disease?
Practice by Chapter
Acute appendicitis
Practice Questions
Acute cholecystitis
Practice Questions
Small bowel obstruction
Practice Questions
Large bowel obstruction
Practice Questions
Mesenteric ischemia
Practice Questions
Gastrointestinal perforation
Practice Questions
Abdominal compartment syndrome
Practice Questions
Acute pancreatitis management
Practice Questions
Diverticulitis
Practice Questions
Incarcerated/strangulated hernias
Practice Questions
Non-operative management principles
Practice Questions
Diagnostic approach to acute abdomen
Practice Questions
Damage control surgery
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
