Abdominal emergencies — MCQs

On this page
A 63-year-old man is brought to the emergency department for the evaluation of severe abdominal pain that started suddenly 1 hour ago while he was having a barbecue with his family. The pain is located in the middle of his abdomen and he describes it as 9 out of 10 in intensity. The patient feels nauseated and has vomited twice. He has also had a loose bowel movement. He was diagnosed with hypertension 2 years ago and was started on hydrochlorothiazide. He stopped taking his pills 1 week ago because of several episodes of heart racing and dizziness that he attributes to his medication. The patient has smoked one pack of cigarettes daily for the last 40 years. He is in severe distress. His temperature is 37.6°C (99.7°F), pulse is 120/min, respirations are 16/min, and blood pressure is 130/90 mm Hg. Cardiac examination shows an irregularly irregular rhythm. Bowel sounds are normal. The abdomen is soft and nontender. The remainder of the physical examination shows no abnormalities. Laboratory studies show: Hemoglobin 16.8 g/dL Leukocyte count 13,000/mm3 Platelet count 340,000/mm3 Prothrombin time 13 seconds Partial thromboplastin time 38 seconds Lactate (venous) 2.4 mEq/L (N=0.5 - 2.2 mEq/L) Serum Urea Nitrogen 15 mg/dL Creatinine 1.2 mg/dL Lactate dehydrogenase 105 U/L CT angiography is performed and the diagnosis is confirmed. Which of the following is the most appropriate definitive management of this patient?
A 65-year-old African American man presents for follow-up examination with a 6-month history of urinary hesitancy, weak stream, and terminal dribbling, which is refractory to a combination therapy of finasteride and tamsulosin. The patient’s past medical history is otherwise unremarkable. His father and brother were diagnosed with prostate cancer at the age of 55 years. His vital signs are within normal limits. The patient has a normal anal sphincter tone and a bulbocavernosus muscle reflex. Digital rectal exam (DRE) reveals a prostate size equivalent to 2 finger pads with a hard nodule and without fluctuance or tenderness. Serum prostate-specific antigen (PSA) level is 5 ng/mL. Which of the following investigations is most likely to establish a definitive diagnosis?
A 42-year-old woman is brought to the emergency department because of a 5-day history of epigastric pain, fever, nausea, and malaise. Five weeks ago she had acute biliary pancreatitis and was treated with endoscopic retrograde cholangiopancreatography and subsequent cholecystectomy. Her maternal grandfather died of pancreatic cancer. She does not smoke. She drinks 1–2 beers daily. Her temperature is 38.7°C (101.7°F), respirations are 18/min, pulse is 120/min, and blood pressure is 100/70 mm Hg. Abdominal examination shows epigastric tenderness and three well-healed laparoscopy scars. The remainder of the examination shows no abnormalities. Laboratory studies show: Hemoglobin 10 g/dL Leukocyte count 15,800/mm3 Serum Na+ 140 mEq/L Cl− 103 mEq/L K+ 4.5 mEq/L HCO3- 25 mEq/L Urea nitrogen 18 mg/dL Creatinine 1.0 mg/dL Alkaline phosphatase 70 U/L Aspartate aminotransferase (AST, GOT) 22 U/L Alanine aminotransferase (ALT, GPT) 19 U/L γ-Glutamyltransferase (GGT) 55 U/L (N = 5–50) Bilirubin 1 mg/dl Glucose 105 mg/dL Amylase 220 U/L Lipase 365 U/L (N = 14–280) Abdominal ultrasound shows a complex cystic fluid collection with irregular walls and septations in the pancreas. Which of the following is the most likely diagnosis?
A 62-year-old man presents to the emergency department with acute pain in the left lower abdomen and profuse rectal bleeding. These symptoms started 3 hours ago. The patient has chronic constipation and bloating, for which he takes lactulose. His family history is negative for gastrointestinal disorders. His temperature is 38.2°C (100.8°F), blood pressure is 90/60 mm Hg, and pulse is 110/min. On physical examination, the patient appears drowsy, and there is tenderness with guarding in the left lower abdominal quadrant. Flexible sigmoidoscopy shows multiple, scattered diverticula with acute mucosal inflammation in the sigmoid colon. Which of the following is the best initial treatment for this patient?
A 47-year-old woman presents to the emergency department with abdominal pain. The patient states that she felt this pain come on during dinner last night. Since then, she has felt bloated, constipated, and has been vomiting. Her current medications include metformin, insulin, levothyroxine, and ibuprofen. Her temperature is 99.0°F (37.2°C), blood pressure is 139/79 mmHg, pulse is 95/min, respirations are 12/min, and oxygen saturation is 98% on room air. On physical exam, the patient appears uncomfortable. Abdominal exam is notable for hypoactive bowel sounds, abdominal distension, and diffuse tenderness in all four quadrants. Cardiac and pulmonary exams are within normal limits. Which of the following is the best next step in management?
A 45-year-old man is brought to the emergency department because of severe abdominal pain for the past 2 hours. He has a 2-year history of burning epigastric pain that gets worse with meals. His pulse is 120/min, respirations are 22/min, and blood pressure is 60/40 mm Hg. Despite appropriate lifesaving measures, he dies. At autopsy, examination shows erosion of the right gastric artery. Perforation of an ulcer in which of the following locations most likely caused this patient's findings?
A 47-year-old man visits the outpatient clinic with complaints of heartburn and chest pain for the past 6 months. His pain is retrosternal and was initially only associated with intake of solid foods, but it now occurs with liquids as well. Antacids do not relieve his pain anymore. He is worried about the pain as it is getting worse with time. He also had an unintentional weight loss of 2.7 kg (6 lb) during this period. Physical examination including the abdominal examination is normal. Laboratory investigations reveal: Hgb 10 mg/dL White blood cell total count 5 x 109/L Platelet count 168 x 109/ L Hematocrit 38% Red blood cell count 4.2 x 1012/ L Esophagogastroduodenoscopy reveals an exophytic mass in the lower third of the esophagus with ulcerations and mucous plugs. Which of the following is the most likely diagnosis in this patient?
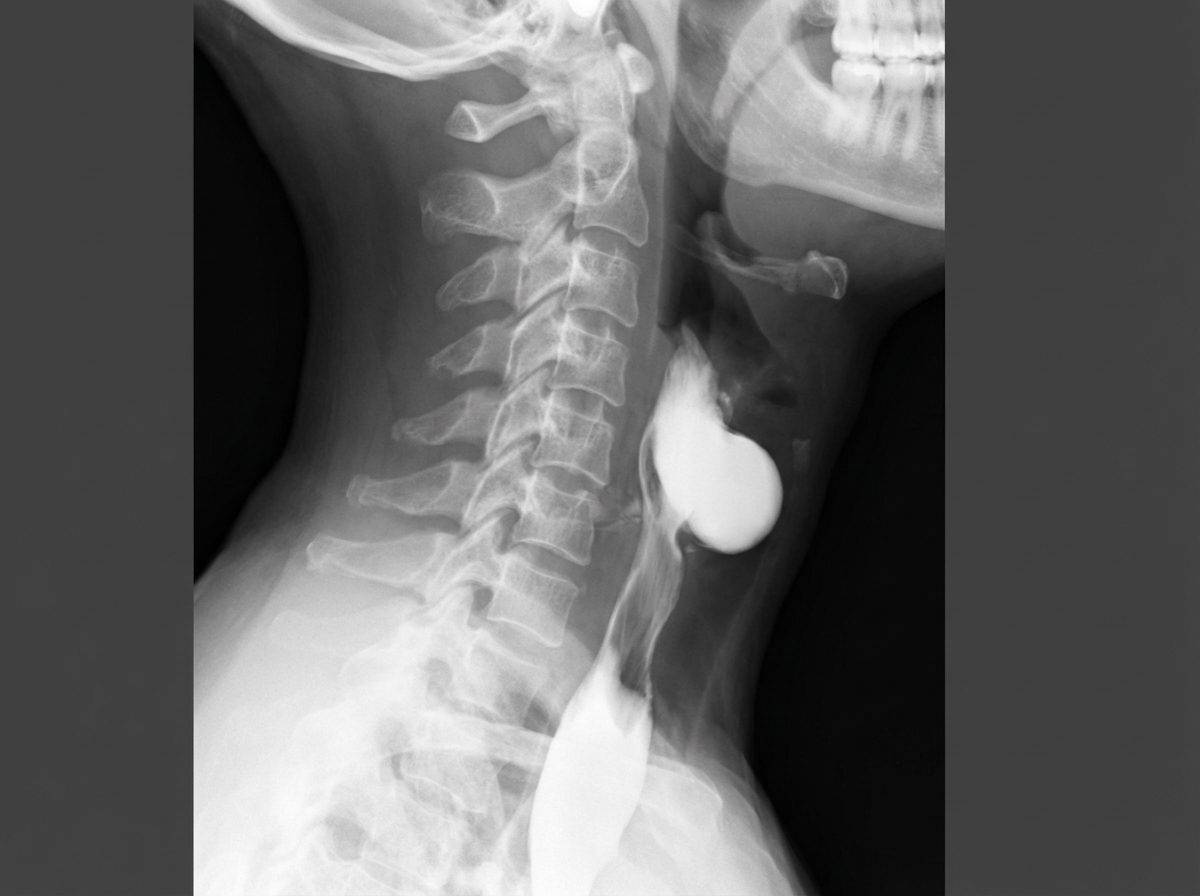
A 68-year-old man presents to the office with his wife complaining of difficulty in swallowing, which progressively worsened over the past month. He has difficulty in initiating swallowing and often has to drink water with solid foods. He has no problems swallowing liquids. His wife is concerned about her husband's bad breath. Adding to his wife, the patient mentions a recent episode of vomiting where the vomit smelled 'really bad' and contained the food that he ate 2 days before. On examination, the patient's blood pressure is 110/70 mm Hg, pulse rate is 72/min, with normal bowel sounds, and no abdominal tenderness to palpation. A barium swallow radiograph is performed (shown below), which reveals a localized collection of contrast material in the cervical region suggestive of an outpouching. Which of the following statements best describes the lesion seen on the radiograph?
A 67-year-old man presents to his primary care physician with constant and gnawing lower abdominal pain for 2 days. The pain has been steadily worsening in intensity. He says the pain occasionally radiates to his lower back and groin bilaterally. While he cannot identify any aggravating factors, he feels that the pain improves with his knees flexed. His medical history is notable for hypertension which is well controlled with medications. He has smoked 40–50 cigarettes daily for 35 years. On examination, there is a palpable pulsatile mass just left of midline below the umbilicus. He is immediately referred for definitive management but during transfer, he becomes hypotensive and unresponsive. Which of the following is the most likely diagnosis?
A 16-year-old boy comes to the physician because of painless enlargement of his left testis for the past 2 weeks. The patient reports that the enlargement is worse in the evenings, especially after playing soccer. He has not had any trauma to the testes. There is no personal or family history of serious illness. Vital signs are within normal limits. Examination shows multiple cord-like structures above the left testes. The findings are more prominent while standing. The cord-like structures disappear in the supine position. The testes are normal on palpation. The patient is at greatest risk of developing which of the following complications?
Practice by Chapter
Acute appendicitis
Practice Questions
Acute cholecystitis
Practice Questions
Small bowel obstruction
Practice Questions
Large bowel obstruction
Practice Questions
Mesenteric ischemia
Practice Questions
Gastrointestinal perforation
Practice Questions
Abdominal compartment syndrome
Practice Questions
Acute pancreatitis management
Practice Questions
Diverticulitis
Practice Questions
Incarcerated/strangulated hernias
Practice Questions
Non-operative management principles
Practice Questions
Diagnostic approach to acute abdomen
Practice Questions
Damage control surgery
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
