Abdominal emergencies — MCQs

On this page
A 46-year-old man comes to the physician with chronic abdominal pain. He has a 3-year history of severe peptic ulcer disease and esophagitis. Two months ago, he took omeprazole, clarithromycin, and amoxicillin for 14 days. His medical history is otherwise unremarkable. Currently, he takes omeprazole 60 mg/day. He is a 10 pack-year smoker and consumes alcohol regularly. Vital signs are within normal limits. Mild epigastric tenderness is noted on deep palpation of the epigastrium. Laboratory studies show: Serum Calcium 9.5 mg/dL Phosphorus 4 mg/dL An upper endoscopy shows several large ulcers in the antrum and 2nd and 3rd parts of the duodenum. The rapid urease test is negative. Fasting gastrin levels are elevated. PET-CT with Ga-Dotatate shows a single mass in the wall of the duodenum. No other mass is detected. Pituitary MRI shows no abnormality. Which of the following is the most appropriate next step in management?
A 24-year-old man comes to the emergency department because of left shoulder pain hours after suffering a fall from a height of approximately 10 feet while rock climbing about 5 hours ago. He initially thought the pain would resolve with rest but it became more severe over the last 2 hours. Last year while rock climbing he fell onto his right shoulder and “needed a sling to fix it”. He has psoriasis. His only medication is topical clobetasol. His pulse is 95/min, respiratory rate is 16/minute, and blood pressure is 114/70 mm Hg. Examination shows full passive and active range of motion at the left shoulder. There is no tenderness to palpation at the acromioclavicular joint. There are silvery plaques over both knees and elbows. Abdominal exam shows 7/10 left upper quadrant tenderness with voluntary guarding. A complete blood count and serum concentrations of electrolytes are within the reference range. Which of the following is the most appropriate next step in management?
A 45-year-old woman comes to the physician because of a 3-month history of mild right upper abdominal pain. She has not had any fevers, chills, or weight loss. There is no personal or family history of serious illness. Medications include transdermal estrogen, which she recently started taking for symptoms related to menopause. Abdominal examination shows no abnormalities. Ultrasonography of the liver shows a well-demarcated, homogeneous, hyperechoic mass surrounded by normal liver tissue. A biopsy of the lesion would put this patient at greatest risk for which of the following complications?
A 73-year-old man presents to the emergency department complaining of abdominal pain with nausea and vomiting, stating that he “can’t keep anything down”. He states that the pain has been gradually getting worse over the past 2 months, saying that, at first, it was present only an hour after he ate but now is constant. He also says that he has been constipated for the last 2 weeks, which has also been getting progressively worse. His last bowel movement was 4 days ago which was normal. He states that he cannot pass flatus. The patient’s past medical history is significant for hypertension and an episode of pneumonia last year. The patient is afebrile and his pulse is 105/min. On physical examination, the patient is uncomfortable. His lungs are clear to auscultation bilaterally. His abdomen is visibly distended and diffusely tender with tympany on percussion. A contrast CT scan of the abdomen shows dilated loops of small bowel with collapsed large bowel. Which of the following is the most likely cause of this patient’s condition?
A 74-year-old man presents to the emergency department with sudden-onset abdominal pain that is most painful around the umbilicus. The pain began 16 hours ago and has no association with meals. He has not been vomiting, but he has had several episodes of bloody loose bowel movements. He was hospitalized 1 week ago for an acute myocardial infarction. He has had diabetes mellitus for 35 years and hypertension for 20 years. He has smoked 15–20 cigarettes per day for the past 40 years. His temperature is 36.9°C (98.42°F), blood pressure is 95/65 mm Hg, and pulse is 95/min. On physical examination, the patient is in severe pain, there is mild periumbilical tenderness, and a bruit is heard over the epigastric area. Which of the following is the definitive test to assess the patient condition?
A 30-year-old woman, gravida 1, para 0, at 30 weeks' gestation is brought to the emergency department because of progressive upper abdominal pain for the past hour. The patient vomited once on her way to the hospital. She states that she initially had dull stomach pain about 6 hours ago, but now the pain is located in the upper abdomen and is more severe. There is no personal or family history of serious illness. She is sexually active with her husband. She does not smoke or drink alcohol. Medications include folic acid and a multivitamin. Her temperature is 38.5°C (101.3°F), pulse is 100/min, and blood pressure is 130/80 mm Hg. Physical examination shows right upper quadrant tenderness. The remainder of the examination shows no abnormalities. Laboratory studies show a leukocyte count of 12,000/mm3. Urinalysis shows mild pyuria. Which of the following is the most likely diagnosis?
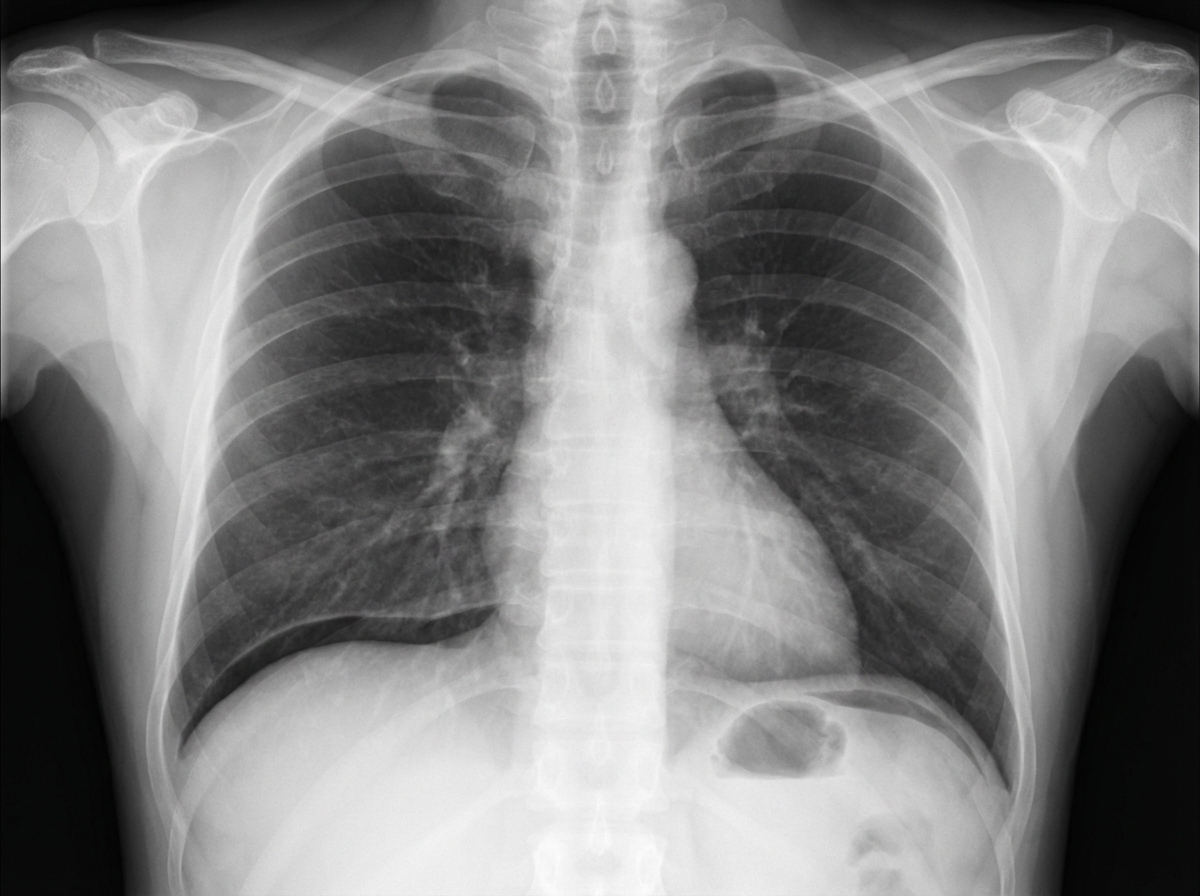
A 54-year-old woman comes to the emergency department because of a 5-hour history of diffuse, severe abdominal pain, nausea, and vomiting. She reports that there is no blood or bile in the vomitus. Two weeks ago, she started having mild aching epigastric pain, which improved with eating. Since then, she has gained 1.4 kg (3 lb). She has a 2-year history of osteoarthritis of both knees, for which she takes ibuprofen. She drinks 1–2 glasses of wine daily. She is lying supine with her knees drawn up and avoids any movement. Her temperature is 38.5°C (101.3°F), pulse is 112/min, respirations are 20/min, and blood pressure is 115/70 mm Hg. Physical examination shows abdominal tenderness and guarding; bowel sounds are decreased. An x-ray of the chest is shown. Which of the following is the most likely cause of this patient's current symptoms?
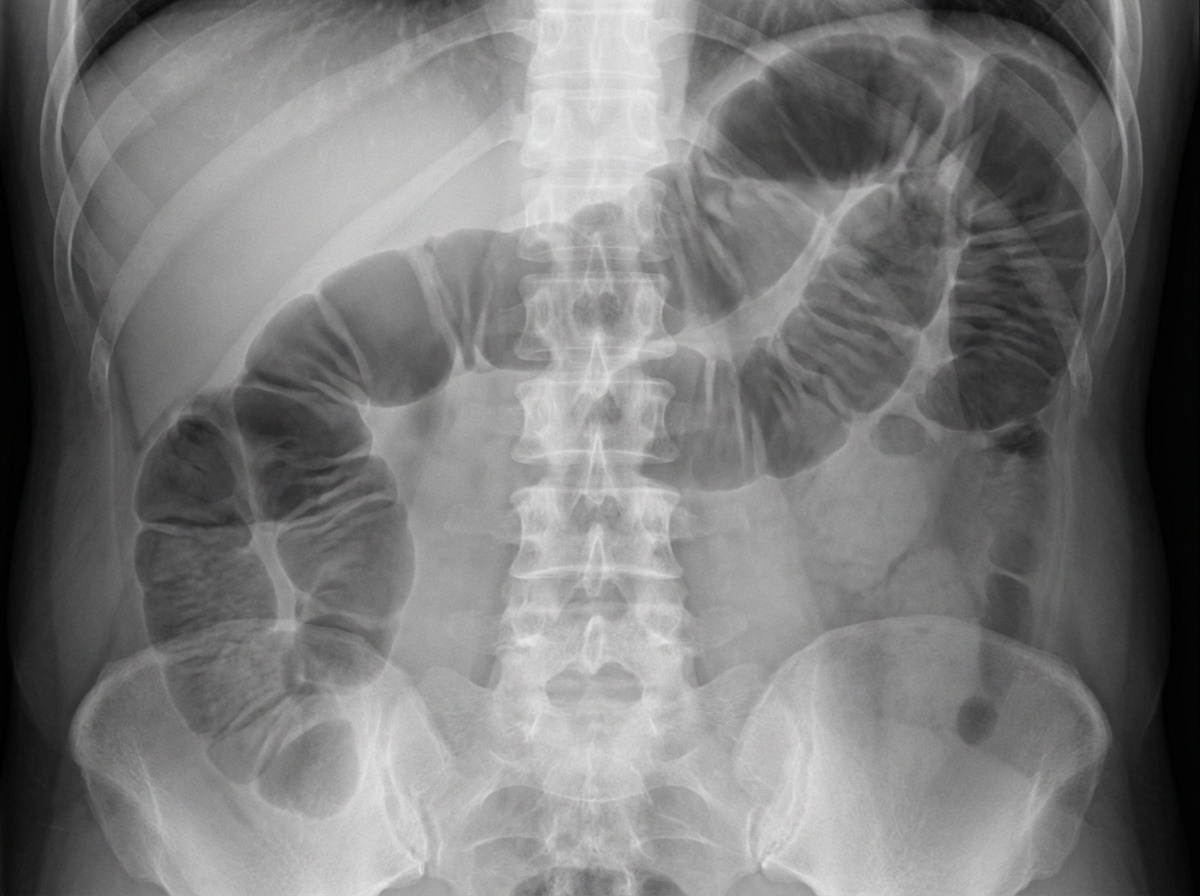
A 63-year-old man is brought to the emergency department for evaluation of abdominal pain. The pain started four days ago and is now a diffuse crampy pain with an intensity of 6/10. The patient has nausea and has vomited twice today. His last bowel movement was three days ago. He has a history of hypertension and recurrent constipation. Five years ago, he underwent emergency laparotomy for a perforated duodenal ulcer. His father died of colorectal cancer at the age of 65 years. The patient has been smoking one pack of cigarettes daily for the past 40 years. Current medications include lisinopril and lactulose. His temperature is 37.6°C (99.7°F), pulse is 89/min, and blood pressure is 120/80 mm Hg. Abdominal examination shows distention and mild tenderness to palpation. There is no guarding or rebound tenderness. The bowel sounds are high-pitched. Digital rectal examination shows no abnormalities. An x-ray of the abdomen is shown. In addition to fluid resuscitation, which of the following is the most appropriate next step in the management of this patient?
A 67-year-old man presents to the emergency department with abdominal pain that started 1 hour ago. The patient has a past medical history of diabetes and hypertension as well as a 40 pack-year smoking history. His blood pressure is 107/58 mmHg, pulse is 130/min, respirations are 23/min, and oxygen saturation is 98% on room air. An abdominal ultrasound demonstrates focal dilation of the aorta with peri-aortic fluid. Which of the following is the best next step in management?
A 61-year-old man comes to the physician because of several episodes of dark urine over the past 2 weeks. He does not have dysuria or flank pain. He works in a factory that produces dyes. Since an accident at work 5 years ago, he has had moderate hearing loss bilaterally. He takes no medications. He has smoked a pack of cigarettes daily for 29 years and drinks one alcoholic beverage daily. Vital signs are within normal limits. Physical examination shows no abnormalities. His urine is pink; urinalysis shows 80 RBC/hpf but no WBCs. Cystoscopy shows a 3-cm mass in the bladder mucosa. The mass is resected. Pathologic examination shows an urothelial carcinoma with penetration into the muscular layer. An x-ray of the chest and a CT scan of the abdomen and pelvis with contrast show a normal upper urinary tract and normal lymph nodes. Which of the following is the most appropriate next step in management?
Practice by Chapter
Acute appendicitis
Practice Questions
Acute cholecystitis
Practice Questions
Small bowel obstruction
Practice Questions
Large bowel obstruction
Practice Questions
Mesenteric ischemia
Practice Questions
Gastrointestinal perforation
Practice Questions
Abdominal compartment syndrome
Practice Questions
Acute pancreatitis management
Practice Questions
Diverticulitis
Practice Questions
Incarcerated/strangulated hernias
Practice Questions
Non-operative management principles
Practice Questions
Diagnostic approach to acute abdomen
Practice Questions
Damage control surgery
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
