Damage control surgery — MCQs

A 36-year-old woman is brought to the emergency department 20 minutes after being involved in a high-speed motor vehicle collision. On arrival, she is unconscious. Her pulse is 140/min, respirations are 12/min and shallow, and blood pressure is 76/55 mm Hg. 0.9% saline infusion is begun. A focused assessment with sonography shows blood in the left upper quadrant of the abdomen. Her hemoglobin concentration is 7.6 g/dL and hematocrit is 22%. The surgeon decided to move the patient to the operating room for an emergent explorative laparotomy. Packed red blood cell transfusion is ordered prior to surgery. However, a friend of the patient asks for the transfusion to be held as the patient is a Jehovah's Witness. The patient has no advance directive and there is no documentation showing her refusal of blood transfusions. The patient's husband and children cannot be contacted. Which of the following is the most appropriate next best step in management?
A 41-year-old man is admitted to the emergency room after being struck in the abdomen by a large cement plate while transporting it. On initial assessment by paramedics at the scene, his blood pressure was 110/80 mm Hg, heart rate 85/min, with no signs of respiratory distress. On admission, the patient is alert but in distress. He complains of severe, diffuse, abdominal pain and severe weakness. Vital signs are now: blood pressure 90/50 mm Hg, heart rate 96/min, respiratory rate 19/min, temperature 37.4℃ (99.3℉), and oxygen saturation of 95% on room air. His lungs are clear on auscultation. The cardiac exam is significant for a narrow pulse pressure. Abdominal examination reveals a large bruise over the epigastric and periumbilical regions. The abdomen is distended and there is diffuse tenderness to palpation with rebound and guarding, worst in the epigastric region. There is hyperresonance to percussion in the epigastric region and absence of hepatic dullness in the right upper quadrant. Aspiration of the nasogastric tube reveals bloody contents. Focused assessment with sonography for trauma (FAST) shows free fluid in the pelvic region. Evaluation of the perisplenic and perihepatic regions is impossible due to the presence of free air. Aggressive intravenous fluid resuscitation is administered but fails to improve upon the patient’s hemodynamics. Which of the following is the next best step in management?
A 30-year-old man is brought to the emergency room by ambulance after being found unconscious in his car parked in his garage with the engine running. His wife arrives and reveals that his past medical history is significant for severe depression treated with fluoxetine. He is now disoriented to person, place, and time. His temperature is 37.8 deg C (100.0 deg F), blood pressure is 100/50 mmHg, heart rate is 100/min, respiratory rate is 10/min, and SaO2 is 100%. On physical exam, there is no evidence of burn wounds. He has moist mucous membranes and no abnormalities on cardiac and pulmonary auscultation. His respirations are slow but spontaneous. His capillary refill time is 4 seconds. He is started on 100% supplemental oxygen by non-rebreather mask. His preliminary laboratory results are as follows: Arterial blood pH 7.20, PaO2 102 mm Hg, PaCO2 23 mm Hg, HCO3 10 mm Hg, WBC count 9.2/µL, Hb 14 mg/dL, platelets 200,000/µL, sodium 137 mEq/L, potassium 5.0 mEq/L, chloride 96 mEq/L, BUN 28 mg/dL, creatinine 1.0 mg/dL, and glucose 120 mg/dL. Which of the following is the cause of this patient's acid-base abnormality?
A 24-year-old woman is brought to the emergency department after being assaulted. The paramedics report that the patient was found conscious and reported being kicked many times in the torso. She is alert and able to respond to questions. She denies any head trauma. She has a past medical history of endometriosis and a tubo-ovarian abscess that was removed surgically two years ago. Her only home medication is oral contraceptive pills. Her temperature is 98.5°F (36.9°C), blood pressure is 82/51 mmHg, pulse is 136/min, respirations are 24/min, and SpO2 is 94%. She has superficial lacerations to the face and severe bruising over her chest and abdomen. Her lungs are clear to auscultation bilaterally and her abdomen is soft, distended, and diffusely tender to palpation. Her skin is cool and clammy. Her FAST exam reveals fluid in the perisplenic space. Which of the following is the next best step in management?
A 32-year-old man is brought to the emergency department after a skiing accident. The patient had been skiing down the mountain when he collided with another skier who had stopped suddenly in front of him. He is alert but complaining of pain in his chest and abdomen. He has a past medical history of intravenous drug use and peptic ulcer disease. He is a current smoker. His temperature is 97.4°F (36.3°C), blood pressure is 77/53 mmHg, pulse is 127/min, and respirations are 13/min. He has a GCS of 15 and bilateral shallow breath sounds. His abdomen is soft and distended with bruising over the epigastrium. He is moving all four extremities and has scattered lacerations on his face. His skin is cool and delayed capillary refill is present. Two large-bore IVs are placed in his antecubital fossa, and he is given 2L of normal saline. His FAST exam reveals fluid in Morison's pouch. Following the 2L normal saline, his temperature is 97.5°F (36.4°C), blood pressure is 97/62 mmHg, pulse is 115/min, and respirations are 12/min. Which of the following is the best next step in management?
A 27-year-old-man is brought to the emergency department 30 minutes after being involved in a motorcycle accident. He lost control at high speed and was thrown forward onto the handlebars. On arrival, he is alert and responsive. He has abdominal pain and superficial lacerations on his left arm. Vital signs are within normal limits. Examination shows a tender, erythematous area over his epigastrium. The abdomen is soft and non-distended. A CT scan of the abdomen shows no abnormalities. Treatment with analgesics is begun, the lacerations are cleaned and dressed, and the patient is discharged home after 2 hours of observation. Four days later, the patient returns to the emergency department with gradually worsening upper abdominal pain, fever, poor appetite, and vomiting. His pulse is 91/min and blood pressure is 135/82 mm Hg. Which of the following is the most likely diagnosis?
A 79-year-old man presents to the emergency department with abdominal pain. The patient describes the pain as severe, tearing, and radiating to the back. His history is significant for hypertension, hyperlipidemia, intermittent claudication, and a 60 pack-year history of smoking. He also has a previously diagnosed stable abdominal aortic aneurysm followed by ultrasound screening. On exam, the patient's temperature is 98°F (36.7°C), pulse is 113/min, blood pressure is 84/46 mmHg, respirations are 24/min, and oxygen saturation is 99% on room air. The patient is pale and diaphoretic, and becomes confused as you examine him. Which of the following is most appropriate in the evaluation and treatment of this patient?
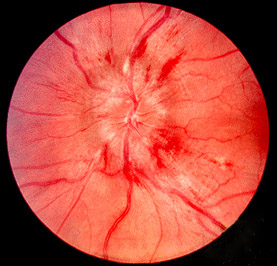
A 72-year-old woman comes to the emergency department 1 hour after the sudden onset of a diffuse, dull, throbbing headache. She also reports blurred vision, nausea, and one episode of vomiting. She has a history of poorly controlled hypertension. A photograph of her fundoscopic examination is shown. Which of the following is the most likely underlying cause of this patient's symptoms?
A 32-year-old woman comes to the physician because of a 2-week history of involuntary loss of urine. She loses small amounts of urine in the absence of an urge to urinate and for no apparent reason. She also reports that she has an intermittent urinary stream. Two years ago, she was diagnosed with multiple sclerosis. Current medications include glatiramer acetate and a multivitamin. She works as a librarian. She has 2 children who attend middle school. Vital signs are within normal limits. The abdomen is soft and nontender. Pelvic examination shows no abnormalities. Neurologic examination shows a slight hypesthesia in the lower left arm and absent abdominal reflex, but otherwise no abnormalities. Her post-void residual urine volume is 131 mL. Bladder size is normal. Which of the following is the most likely cause of the patient's urinary incontinence?
A 24-year-old woman comes to the emergency department because of abdominal pain, fever, nausea, and vomiting for 12 hours. Her abdominal pain was initially dull and diffuse but has progressed to a sharp pain on the lower right side. Two years ago she had to undergo right salpingo-oophorectomy after an ectopic pregnancy. Her temperature is 38.7°C (101.7°F). Physical examination shows severe right lower quadrant tenderness with rebound tenderness; bowel sounds are decreased. Laboratory studies show leukocytosis with left shift. An abdominal CT scan shows a distended, edematous appendix. The patient is taken to the operating room for an appendectomy. During the surgery, the adhesions from the patient's previous surgery make it difficult for the resident physician to identify the appendix. Her attending mentions that she should use a certain structure for guidance to locate the appendix. The attending is most likely referring to which of the following structures?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
