Respiratory — MCQs

On this page
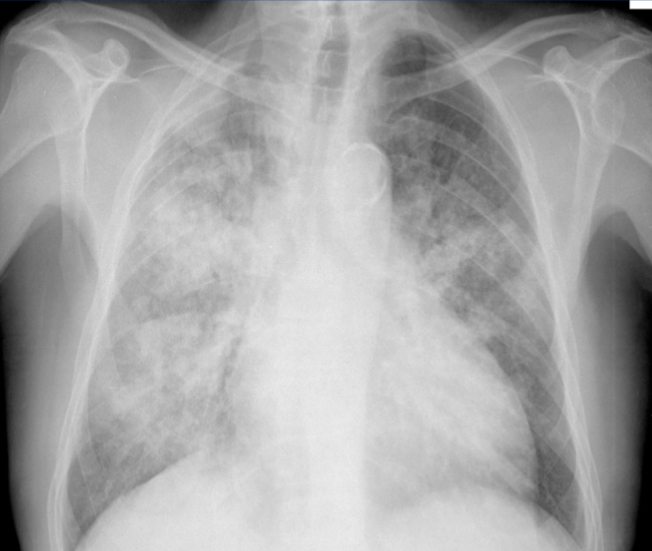
A 17-year-old boy presents to the emergency department of a hospital located in the town of Recuay (which is situated at 3,400 meters above mean sea level [MAMSL]) in the Ancash Region (Peru), 48 hours after returning from a 21-day stay in Lima (the capital city of Peru at 0 MAMSL). The patient has no previous medical history. His current complaints include cough, dyspnea at rest, hemoptysis, chest pain, and vomiting. His vital signs include: blood pressure 90/60 mm Hg; heart rate 149/min; respiratory rate 37/min; temperature 36.5°C (97.7°F); and O2 saturation 71%. Physical examination reveals polypnea, perioral cyanosis, intercostal retractions, and diffuse pulmonary crackles. His laboratory results are as follows: Hemoglobin 19.2 g/dL Hematocrit 60% Leukocytes 13,000 (Bands: 12%, Seg: 78%, Eos: 0%, Bas: 0%, Mon: 6%) Urea 25 mg/dL Creatinine 0.96 mg/dL A chest X-ray is shown. Which of the following statements is true and most likely regarding this patient’s condition?
Which of the following cells in the body depends on dynein for its unique functioning?
A 45-year-old man with a 15-pack-year smoking history is referred for pulmonary function testing. On physical exam, he appears barrel-chested and mildly overweight, but breathes normally. Which of the following tests will most accurately measure his total lung capacity?
A 62-year-old man presents to the emergency department for evaluation of a 2-year history of increasing shortness of breath. He also has an occasional nonproductive cough. The symptoms get worse with exertion. The medical history is significant for hypertension and he takes chlorthalidone. He is a smoker with a 40-pack-year smoking history. On physical examination, the patient is afebrile; the vital signs include: blood pressure 125/78 mm Hg, pulse 90/min, and respiratory rate 18/min. The body mass index (BMI) is 31 kg/m2. The oxygen saturation is 94% at rest on room air. A pulmonary examination reveals decreased breath sounds bilaterally, but is otherwise normal with no wheezes or crackles. The remainder of the examination is unremarkable. A chest radiograph shows hyperinflation of both lungs with mildly increased lung markings, but no focal findings. Based on this clinical presentation, which of the following is most likely?
A 29-year-old man presents for the evaluation of infertility. He has a history of recurrent lower respiratory tract infections, productive cough, abdominal pain, and diarrhea. Physical examination reveals clubbing and bilateral crackles on chest auscultation. Chest X-ray reveals increased pulmonary markings and peripheral bronchi with a ‘tram track’ appearance. Which of the following pathophysiologies is responsible for the patient’s condition?
A 56-year-old male comes to the physician because of a 2-month history of excessive sleepiness. He reports that he has been sleeping for an average of 10 to 12 hours at night and needs to take multiple naps during the day. Six months ago, he was diagnosed with small cell lung carcinoma and underwent prophylactic cranial irradiation. This patient's symptoms are most likely caused by damage to which of the following structures?
A group of investigators is studying thermoregulatory adaptations of the human body. A subject is seated in a thermally insulated isolation chamber with an internal temperature of 48°C (118°F), a pressure of 1 atmosphere, and a relative humidity of 10%. Which of the following is the primary mechanism of heat loss in this subject?
A 60-year-old woman with a history of emphysema has been referred by her pulmonologist for follow-up pulmonary function testing. During the test, the patient reaches a point where her airway pressure is equal to the atmospheric pressure. Which of the following is most likely to be found during this respiratory state?
A 10-year-old boy is brought to the physician by his mother because of a 2-day history of fever and productive cough. He has had similar episodes sporadically in the past with frequent episodes of thick, discolored nasal discharge. Physical examination shows diffuse crackles and rhonchi. The most likely cause of recurrent infections in this patient is a dysfunction of which of the following cell types?
An 18-year-old man presents to his primary care physician with a complaint of excessive daytime sleepiness. He denies any substance abuse or major changes in his sleep schedule. He reports frequently dozing off during his regular daily activities. On further review of systems, he endorses falling asleep frequently with the uncomfortable sensation that there is someone in the room, even though he is alone. He also describes that from time to time, he has transient episodes of slurred speech when experiencing heartfelt laughter. Vital signs are stable, and his physical exam is unremarkable. This patient is likely deficient in a neurotransmitter produced in which part of the brain?
Practice by Chapter
Respiratory mechanics and work of breathing
Practice Questions
Pulmonary volumes and capacities
Practice Questions
Spirometry interpretation
Practice Questions
Flow-volume loops
Practice Questions
Airway resistance determinants
Practice Questions
Control of breathing
Practice Questions
Central and peripheral chemoreceptors
Practice Questions
Respiratory centers in the brainstem
Practice Questions
Exercise respiratory physiology
Practice Questions
Sleep effects on respiration
Practice Questions
High altitude adaptation
Practice Questions
Dyspnea mechanisms
Practice Questions
Integrated respiratory responses
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
