Dyspnea mechanisms — MCQs

A 21-year-old man presents to his physician because he has been feeling increasingly tired and short of breath at work. He has previously had these symptoms but cannot recall the diagnosis he was given. Chart review reveals the following results: Oxygen tension in inspired air = 150 mmHg Alveolar carbon dioxide tension = 50 mmHg Arterial oxygen tension = 71 mmHg Respiratory exchange ratio = 0.80 Diffusion studies reveal normal diffusion distance. The patient is administered 100% oxygen but the patient's blood oxygen concentration does not improve. Which of the following conditions would best explain this patient's findings?
A 60-year-old woman is brought to the emergency department by her husband because of worsening shortness of breath over the past 2 days. Last week, she had a sore throat and a low-grade fever. She has coughed up white sputum each morning for the past 2 years. She has hypertension and type 2 diabetes mellitus. She has smoked 2 packs of cigarettes daily for 35 years. Current medications include metformin and lisinopril. On examination, she occasionally has to catch her breath between sentences. Her temperature is 38.1°C (100.6°F), pulse is 85/min, respirations are 16/min, and blood pressure is 140/70 mm Hg. Expiratory wheezes with a prolonged expiratory phase are heard over both lung fields. Arterial blood gas analysis on room air shows: pH 7.33 PCO2 53 mm Hg PO2 68 mm Hg An x-ray of the chest shows hyperinflation of bilateral lung fields and flattening of the diaphragm. Which of the following additional findings is most likely in this patient?
A 27-year-old woman is admitted to the emergency room with dyspnea which began after swimming and progressed gradually over the last 3 days. She denies cough, chest pain, or other respiratory symptoms. She reports that for the past 4 months, she has had several dyspneic episodes that occurred after the exercising and progressed at rest, but none of these were as long as the current one. Also, she notes that her tongue becomes ‘wadded’ when she speaks and she tires very quickly during the day. The patient’s vital signs are as follows: blood pressure 125/60 mm Hg, heart rate 92/min, respiratory rate 34/min, and body temperature 36.2℃ (97.2℉). Blood saturation on room air is initially 92% but falls to 90% as she speaks up. On physical examination, the patient is slightly lethargic. Her breathing is rapid and shallow. Lung auscultation, as well as cardiac, and abdominal examinations show no remarkable findings. Neurological examination reveals slight bilateral ptosis increased by repetitive blinking, and easy fatigability of muscles on repeated movement worse on the face and distal muscles of the upper and lower extremities. Which arterial blood gas parameters would you expect to see in this patient?
A 57-year-old man presents to the clinic for a chronic cough over the past 4 months. The patient reports a productive yellow/green cough that is worse at night. He denies any significant precipitating event prior to his symptoms. He denies fever, chest pain, palpitations, weight changes, or abdominal pain, but endorses some difficulty breathing that waxes and wanes. He denies alcohol usage but endorses a 35 pack-year smoking history. A physical examination demonstrates mild wheezes, bibasilar crackles, and mild clubbing of his fingertips. A pulmonary function test is subsequently ordered, and partial results are shown below: Tidal volume: 500 mL Residual volume: 1700 mL Expiratory reserve volume: 1500 mL Inspiratory reserve volume: 3000 mL What is the functional residual capacity of this patient?
During heavy exercise, what is the primary mechanism for maintaining arterial pH despite increased lactic acid production?
A 58-year-old man comes to the physician because of a 5-day history of progressively worsening shortness of breath and fatigue. He has smoked 1 pack of cigarettes daily for 30 years. His pulse is 96/min, respirations are 26/min, and blood pressure is 100/60 mm Hg. An x-ray of the chest is shown. Which of the following is the most likely cause of this patient's findings?
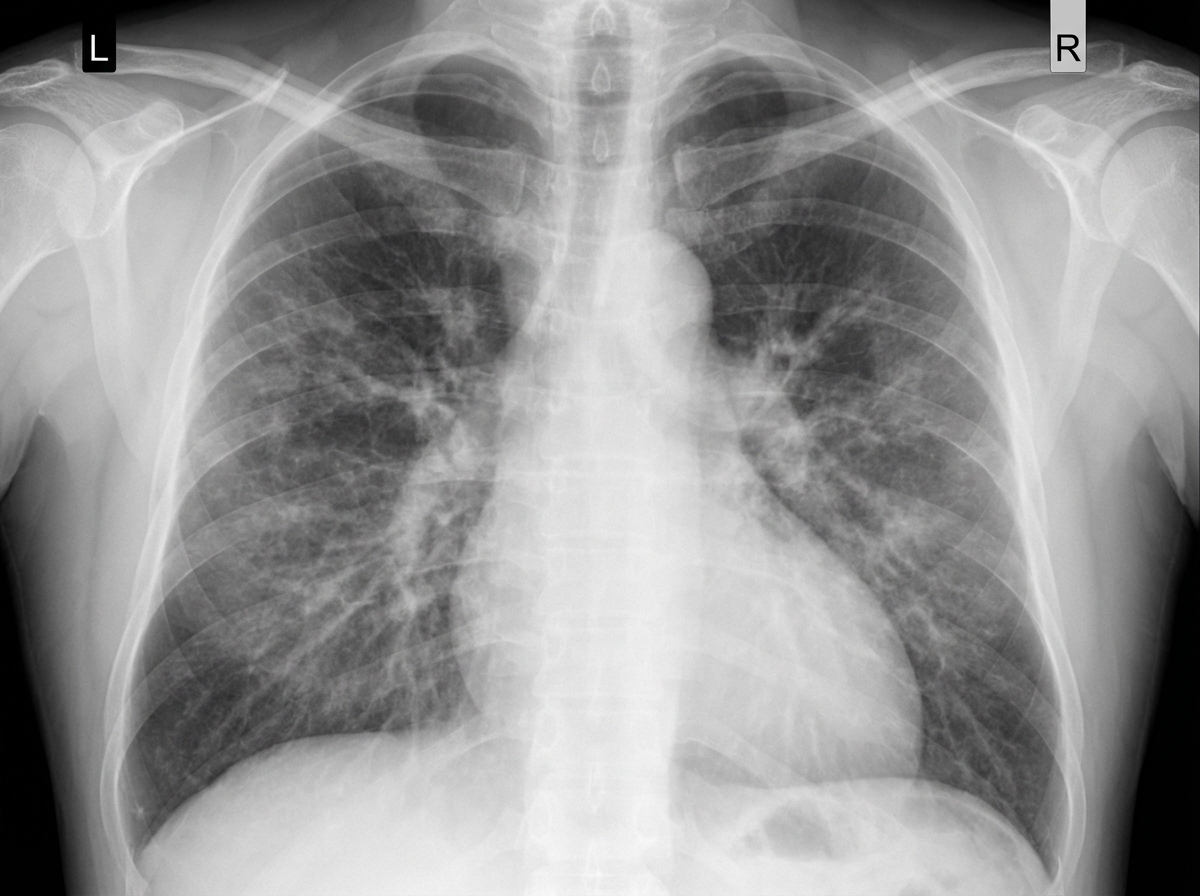
A 55-year-old man presents with an unremitting cough and swelling of the lower limbs for the past 2 weeks. He says he has had a chronic cough for years, however, he feels it is getting worse. He reports a 30-pack-year smoking history. Physical examination reveals mild central cyanosis and expiratory wheezes throughout the chest. Oxygen therapy is ordered immediately but, soon after administering it, his respiratory rate starts to slow down and he becomes drowsy. Dysfunction of which of the following receptors most likely led to this patient’s current condition?
A 63-year-old man undergoes workup for nocturnal dyspnea and what he describes as a "choking" sensation while sleeping. He also endorses fatigue and dyspnea on exertion. Physical exam reveals a normal S1, loud P2, and a neck circumference of 17 inches (43 cm) (normal < 14 inches (< 35 cm)). His temperature is 98.8°F (37°C), blood pressure is 128/82 mmHg, pulse is 86/min, and respirations are 19/min. He undergoes spirometry, which is unrevealing, and polysomnography, which shows 16 hypopneic and apneic events per hour. Mean pulmonary arterial pressure is 30 mmHg. Which of the following complications is this patient most at risk for?
A 22-year-old woman presents to the emergency department with a chief concern of shortness of breath. She was hiking when she suddenly felt unable to breathe and had to take slow deep breaths to improve her symptoms. The patient is a Swedish foreign exchange student and does not speak any English. Her past medical history and current medications are unknown. Her temperature is 99.5°F (37.5°C), blood pressure is 127/68 mmHg, pulse is 120/min, respirations are 22/min, and oxygen saturation is 90% on room air. Physical exam is notable for poor air movement bilaterally and tachycardia. The patient is started on treatment. Which of the following best describes this patient's underlying pathology? FEV1 = Forced expiratory volume in 1 second FVC = Forced vital capacity DLCO = Diffusing capacity of carbon monoxide
A 21-year-old man is admitted to the intensive care unit for respiratory failure requiring mechanical ventilation. His minute ventilation is calculated to be 7.0 L/min, and his alveolar ventilation is calculated to be 5.1 L/min. Which of the following is most likely to decrease the difference between minute ventilation and alveolar ventilation?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
