Renal — MCQs

On this page
An investigator studying hormone synthesis and transport uses immunocytochemical techniques to localize a carrier protein in the central nervous system of an experimental animal. The investigator finds that this protein is synthesized together with a specific hormone from a composite precursor. The protein is involved in the transport of the hormone from the supraoptic and paraventricular nuclei to its destination. The hormone transported by these carrier proteins is most likely responsible for which of the following functions?
A 3-year-old boy is brought to the emergency department with a history of unintentional ingestion of seawater while swimming in the sea. The amount of seawater ingested is not known. There is no history of vomiting. On physical examination, the boy appears confused and is asking for more water to drink. His serum sodium is 152 mmol/L (152 mEq/L). Which of the following changes in volumes and osmolality of body fluids are most likely to be present in this boy?
An investigator is studying the effect of antihypertensive drugs on cardiac output and renal blood flow. For comparison, a healthy volunteer is given a placebo and a continuous infusion of para-aminohippuric acid (PAH) to achieve a plasma concentration of 0.02 mg/ml. His urinary flow rate is 1.5 ml/min and the urinary concentration of PAH is measured to be 8 mg/ml. His hematocrit is 50%. Which of the following values best estimates cardiac output in this volunteer?
A 45-year-old woman is brought to the Emergency Department by her husband due to increasing confusion. He reports that she has been urinating a lot for the past month or so, especially at night, and has also been constantly drinking water and tea. Lately, she has been more tired than usual as well. Her past medical history is significant for bipolar disorder. She takes lithium and a multivitamin. She has a levonorgestrel IUD. Her blood pressure is 140/90 mmHg, pulse rate is 95/min, respiratory rate is 16/min, and temperature is 36°C (96.8°F). At physical examination, she is drowsy and disoriented. Her capillary refill is delayed and her mucous membranes appear dry. The rest of the exam is nondiagnostic. Laboratory studies show: Na+: 148 mEq/L K+: 4.2 mEq/L Serum calcium: 11.0 mg/dL Creatinine: 1.0 mg/dL Urine osmolality: 190 mOsm/kg Serum osmolality: 280 mOsm/kg Finger-stick glucose: 120 mg/dL Fluid resuscitation is initiated. Which of the following is the most likely diagnosis?
A 29-year-old woman presents to the emergency department with a broken arm after she tripped and fell at work. She says that she has no history of broken bones but that she has been having bone pain in her back and hips for several months. In addition, she says that she has been waking up several times in the middle of the night to use the restroom and has been drinking a lot more water. Her symptoms started after she fell ill during an international mission trip with her church and was treated by a local doctor with unknown antibiotics. Since then she has been experiencing weight loss and muscle pain in addition to the symptoms listed above. Urine studies are obtained showing amino acids in her urine. The pH of her urine is also found to be < 5.5. Which of the following would most likely also be seen in this patient?
An investigator is studying the effects of hyperphosphatemia on calcium homeostasis. A high-dose phosphate infusion is administered intravenously to a healthy subject over the course of 3 hours. Which of the following sets of changes is most likely to occur in response to the infusion? $$$ Serum parathyroid hormone %%% Serum total calcium %%% Serum calcitriol %%% Urine phosphate $$$
A 73-year-old male presents to the clinic with lumbar pain and symmetrical bone pain in his legs and arms. He has trouble going up to his bedroom on the second floor and getting up from a chair. Past medical history reveals that he has had acid reflux for the past 5 years that is refractory to medications (PPIs & H2 antagonists); thus, he had decided to stay away from foods which have previously given him heartburn - red meats, whole milk, salmon - and has eaten a mainly vegetarian diet. Which of the following processes is most likely decreased in this male?
A 56-year-old man is seen in the hospital for a chief complaint of intense thirst and polyuria. His history is significant for recent transsphenoidal resection of a pituitary adenoma. With regard to the man's fluid balance, which of the following would be expected?
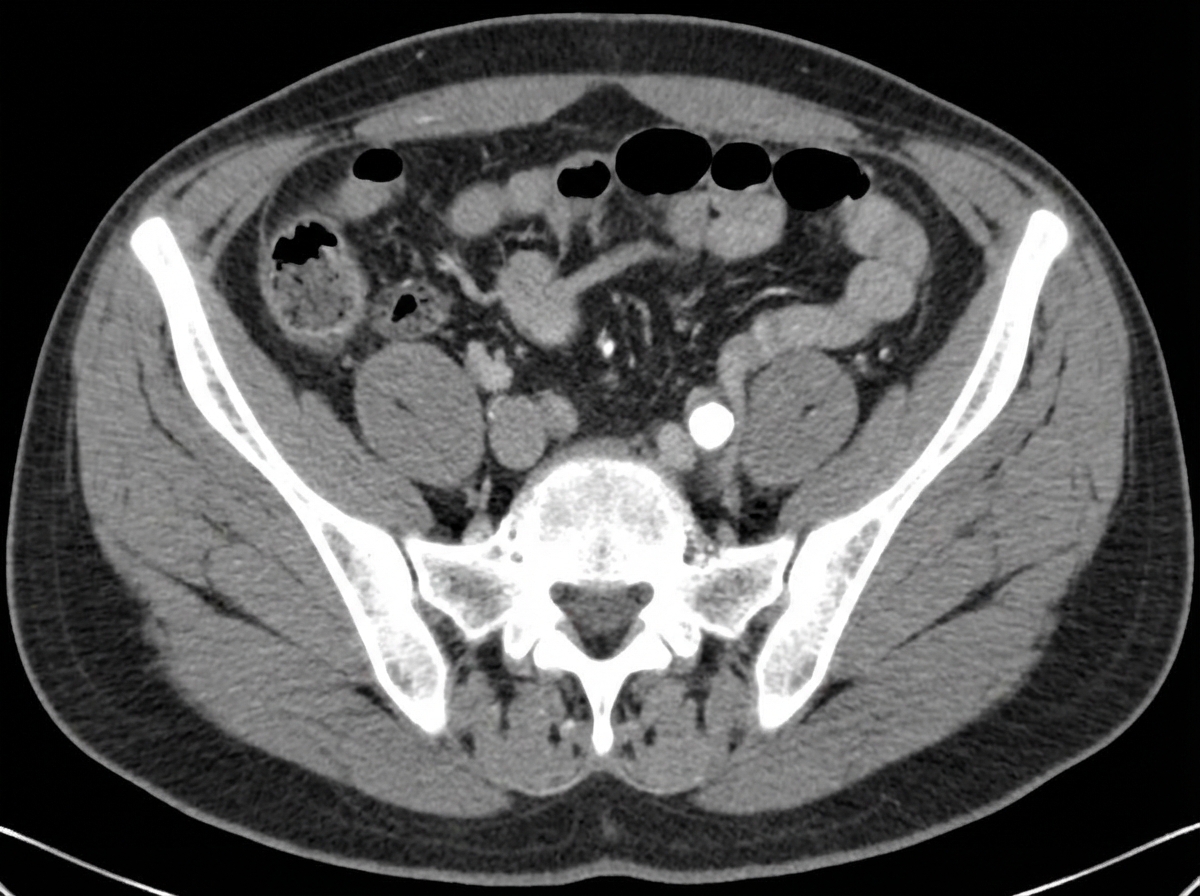
A 55-year-old woman presents to the emergency room with severe abdominal pain for the past 24 hours. She has also noticed blood in her urine. She does not have any significant past medical history. Family history is significant for her mother having cholecystitis status post cholecystectomy at age 45. Her vital signs include: temperature 36.8°C (98.2°F), pulse 103/min, respiratory rate 15/min, blood pressure 105/85 mm Hg. Physical examination is significant for a woman continuously moving on the exam table in an attempt to get comfortable. Laboratory findings are significant for the following: Serum electrolytes Na 138 mEq/L N: 135–145 mEq/L K 4.0 mEq/L N: 3.5–5.0 mEq/L Cl 102 mEq/L N: 98–108 mEq/L CO2 27 mEq/L N: 22–32 mEq/L Ca 9.2 mEq/dL N: 8.4–10.2 mEq/dL PO4 3.5 mg/dL N: 3.0–4.5 mg/dL A 24-hour urine collection is performed and reveals a urinary calcium of 345 mg/day (ref: < 300 mg/day in men; < 250 mg/day in women). A non-contrast CT of the abdomen is performed and is shown in the exhibit. The patient’s symptoms pass within the next 12 hours with hydration and acetaminophen for pain management. She is prescribed a medication to prevent subsequent episodes. At which of the following parts of the nephron does this medication most likely work?
A 28-year-old woman presents to her primary care physician complaining of intense thirst and frequent urination for the past 2 weeks. She says that she constantly feels the urge to drink water and is also going to the bathroom to urinate frequently throughout the day and multiple times at night. She was most recently hospitalized 1 month prior to presentation following a motor vehicle accident in which she suffered severe impact to her head. The physician obtains laboratory tests, with the results shown below: Serum: Na+: 149 mEq/L Cl-: 103 mEq/L K+: 3.5 mEq/L HCO3-: 24 mEq/L BUN: 20 mg/dL Glucose: 105 mg/dL Urine Osm: 250 mOsm/kg The patient’s condition is most likely caused by inadequate hormone secretion from which of the following locations?
Practice by Chapter
Renal blood flow distribution
Practice Questions
Proximal tubule reabsorption
Practice Questions
Loop of Henle function
Practice Questions
Distal tubule and collecting duct function
Practice Questions
Concentration and dilution of urine
Practice Questions
Countercurrent multiplication system
Practice Questions
Sodium handling along the nephron
Practice Questions
Potassium balance and regulation
Practice Questions
Calcium and phosphate handling
Practice Questions
Magnesium handling
Practice Questions
Water balance and osmoregulation
Practice Questions
Diuretic mechanisms of action
Practice Questions
Integrated nephron function
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
