Oxygen transport in blood — MCQs

A research scientist attempts to understand the influence of carbon dioxide content in blood on its oxygen binding. The scientist adds carbon dioxide to dog blood and measures the uptake of oxygen in the blood versus oxygen pressure in the peripheral tissue. He notes in one dog that with the addition of carbon dioxide with a pressure of 90 mmHg, the oxygen pressure in the peripheral tissue rose from 26 to 33 mmHg. How can this phenomenon be explained?
A 44-year-old male immigrant presents to his primary care physician for a new patient visit. The patient reports chronic fatigue but states that he otherwise feels well. His past medical history is not known, and he is not currently taking any medications. The patient admits to drinking 7 alcoholic beverages per day and smoking 1 pack of cigarettes per day. His temperature is 99.4°F (37.4°C), blood pressure is 157/98 mmHg, pulse is 99/min, respirations are 18/min, and oxygen saturation is 100% on room air. Physical exam demonstrates mild pallor but is otherwise not remarkable. Laboratory studies are ordered as seen below. Hemoglobin: 9 g/dL Hematocrit: 33% Leukocyte count: 6,500/mm^3 with normal differential Platelet count: 190,000/mm^3 Mean corpuscular volume (MCV): 60 femtoliters Free iron: 272 mcg/dL Total iron binding capacity (TIBC): 175 mcg/dL Ferritin: 526 ng/mL Reticulocyte count: 2.8% Which of the following is the most likely diagnosis?
A 40-year-old female volunteers for an invasive study to measure her cardiac function. She has no previous cardiovascular history and takes no medications. With the test subject at rest, the following data is collected using blood tests, intravascular probes, and a closed rebreathing circuit: Blood hemoglobin concentration 14 g/dL Arterial oxygen content 0.22 mL O2/mL Arterial oxygen saturation 98% Venous oxygen content 0.17 mL O2/mL Venous oxygen saturation 78% Oxygen consumption 250 mL/min The patient's pulse is 75/min, respiratory rate is 14/ min, and blood pressure is 125/70 mm Hg. What is the cardiac output of this volunteer?
A 19-year-old male college student is brought to the emergency department by his girlfriend complaining of intense pain. They had been playing outside in the snow when the patient started to have severe hand and feet pain. He says the pain is 9 out of 10 and causing him to have trouble moving his fingers and toes. He also reports some difficulty “catching his breath.” He notes that he has been tiring easily for the past month but thought it was because he was studying and going out late. On physical examination, the patient appears uncomfortable. Bilateral conjunctivae are pale. His hands are swollen and tender to palpation. Cardiopulmonary examination is normal. Hemoglobin is 9.0 g/dL. An electrocardiogram shows mild sinus tachycardia. Hemoglobin electrophoresis is performed, which confirms sickle cell disease. The patient’s pain is managed, and he is discharged on hydroxyurea. Which of the following is the most likely to occur as a result of the new medication?
A 48-year-old man is brought to the emergency department 20 minutes after being rescued from a house fire. He reports headache, metallic taste, abdominal pain, and nausea. He appears confused and agitated. His pulse is 125/min, respirations are 33/min, and blood pressure is 100/65 mm Hg. Pulse oximetry on room air shows an oxygen saturation of 98%. Physical examination shows a bright red color of the skin. His breath smells of bitter almonds. Hyperbaric oxygen therapy and appropriate pharmacotherapy are initiated. The expected beneficial effect of this drug is most likely due to which of the following mechanisms?
Which factor most strongly influences coronary blood flow during exercise?
A 63-year-old man presents to the clinic with fever accompanied by shortness of breath. The symptoms developed a week ago and have been progressively worsening over the last 2 days. He reports his cough is productive of thick, yellow sputum. He was diagnosed with chronic obstructive pulmonary disease 3 years ago and has been on treatment ever since. He quit smoking 10 years ago but occasionally experiences shortness of breath along with chest tightness that improves with the use of an inhaler. However, this time the symptoms seem to be more severe and unrelenting. His temperature is 38.6°C (101.4°F), the respirations are 21/min, the blood pressure is 100/60 mm Hg, and the pulse is 105/min. Auscultation reveals bilateral crackles and expiratory wheezes. His oxygen saturation is 95% on room air. According to this patient’s history, which of the following should be the next step in the management of this patient?
A 50-year-old man presents to the urgent care clinic for 3 hours of worsening cough, shortness of breath, and dyspnea. He works as a long-haul truck driver, and he informs you that he recently returned to the west coast from a trip to Arkansas. His medical history is significant for gout, hypertension, hypercholesterolemia, diabetes mellitus type 2, chronic obstructive pulmonary disease (COPD), and mild intellectual disability. He currently smokes 1 pack of cigarettes/day, drinks a 6-pack of beer/day, and he endorses a past history of injection drug use but currently denies any illicit drug use. The vital signs include: temperature 36.7°C (98.0°F), blood pressure 126/74 mm Hg, heart rate 87/min, and respiratory rate 23/min. His physical examination shows mild, bilateral, coarse rhonchi, but otherwise clear lungs on auscultation, grade 2/6 holosystolic murmur, and a benign abdominal physical examination. He states that he ran out of his albuterol inhaler 6 days ago and has been meaning to follow-up with his primary care physician (PCP) for a refill. Complete blood count (CBC) and complete metabolic panel are within normal limits. He also has a D-dimer result within normal limits. Which of the following is the most appropriate next step in evaluation?
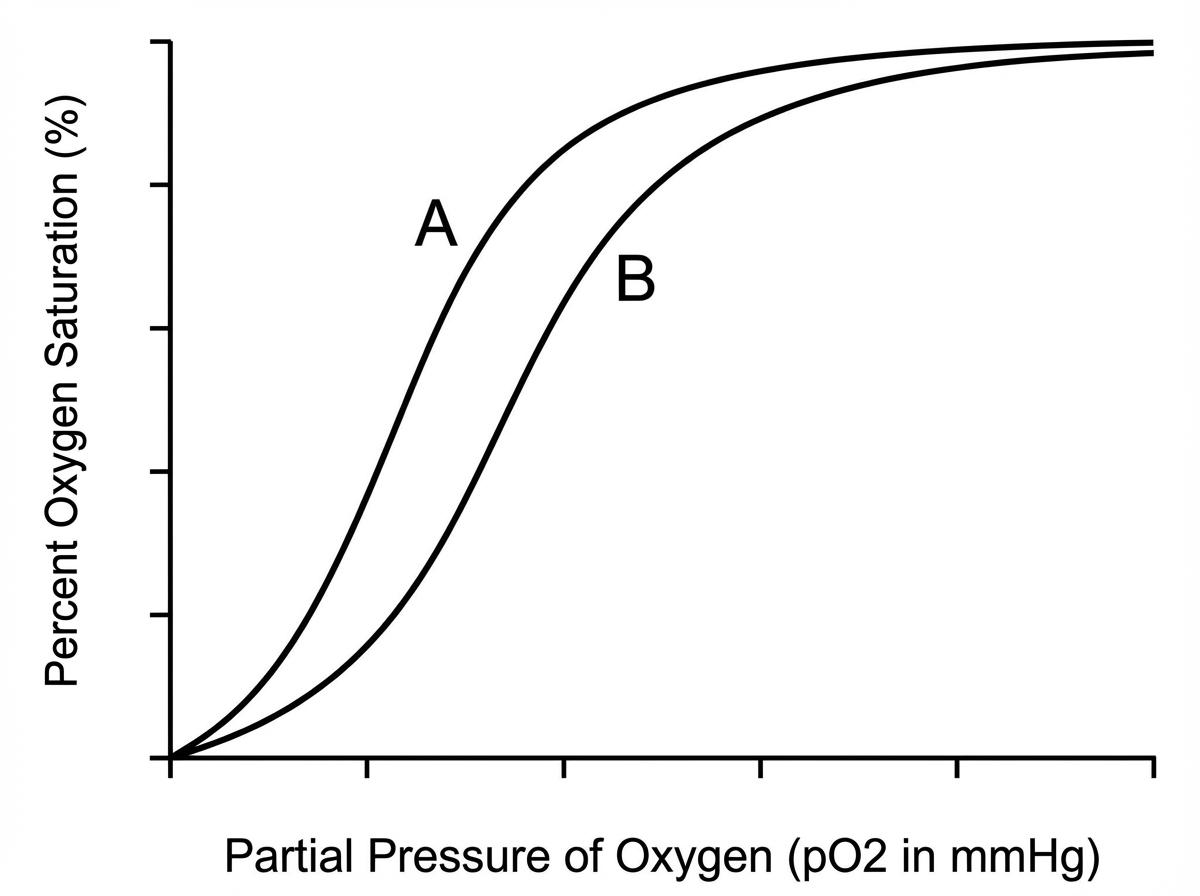
An investigator is conducting a study on hematological factors that affect the affinity of hemoglobin for oxygen. An illustration of two graphs (A and B) that represent the affinity of hemoglobin for oxygen is shown. Which of the following best explains a shift from A to B?
A 32-year-old female with Crohn's disease diagnosed in her early 20s comes to your office for a follow-up appointment. She is complaining of headaches and fatigue. Which of the following arterial blood gas findings might you expect?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
